Abstract
Purpose
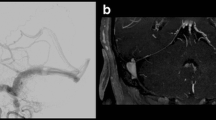
Computed tomography angiography (CTA) and magnetic resonance imaging/angiography (MRI/MRA) are used for the diagnosis of intracranial dural arteriovenous fistulas (DAVFs). The purpose of this study was to compare the diagnostic accuracy of CTA and magnetic resonance imaging/angiography (MRI/MRA) for detection of cortical venous reflux (CVR) in intracranial DAVFs.
Methods
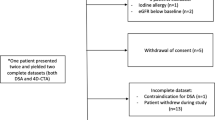
The records of patients with angiography-confirmed intracranial DAVFs who also received CTA and MRI/MRA from January 2008 to July 2016 were reviewed. CTA and MRI/MRA were reviewed for signs of CVR, and the diagnostic accuracy of individual signs was evaluated by receiver operating curve (ROC) analysis.
Results
A total 108 patients were included in this study. CTA signs of CVR included abnormal dilatation, early enhancement, and the presence of a medullary or pial vein. MRI/MRA signs of CVR included abnormal dilatation, early enhancement, flow-related enhancement, flow void, and medullary or pial venous collaterals. The sensitivity of individual CTA signs ranged from 62 to 96%, and specificities from 79 to 94%. The sensitivities of individual MRI/MRA signs ranged from 58 to 83%, and specificities from 77 to 93%. The area under ROC curve (AUC) of CTA and MRI/MRA were 0.91 and 0.87, respectively (P = 0.04 in direct comparison). In subgroup analysis, CTA had better diagnostic accuracy for higher grade disease (P = 0.05) and non-aggressive manifestation (P = 0.04).
Conclusions
Both CTA and MRI/MRA have good diagnostic accuracy for detection of CVR in patients with intracranial DAVFs. There is modest evidence that CTA is better than MRI/MRA.



Similar content being viewed by others
References
Cognard C, Gobin YP, Pierot L, Bailly AL, Houdart E, Casasco A, Chiras J, Merland JJ (1995) Cerebral dural arteriovenous fistulas: clinical and angiographic correlation with a revised classification of venous drainage. Radiology 194(3):671–680. https://doi.org/10.1148/radiology.194.3.7862961
Borden JA, Wu JK, Shucart WA (1995) A proposed classification for spinal and cranial dural arteriovenous fistulous malformations and implications for treatment. J Neurosurg 82(2):166–179. https://doi.org/10.3171/jns.1995.82.2.0166
Kobayashi A, Al-Shahi Salman R (2014) Prognosis and treatment of intracranial dural arteriovenous fistulae: a systematic review and meta-analysis. International journal of stroke : official journal of the International Stroke Society 9(6):670–677. https://doi.org/10.1111/ijs.12337
van Dijk JMC, terBrugge KG, Willinsky RA, Wallace MC (2002) Clinical course of cranial dural arteriovenous fistulas with long-term persistent cortical venous reflux. Stroke 33(5):1233–1236. https://doi.org/10.1161/01.str.0000014772.02908.44
van Rooij WJ, Sluzewski M, Beute GN (2007) Dural arteriovenous fistulas with cortical venous drainage: incidence, clinical presentation, and treatment. AJNR Am J Neuroradiol 28(4):651–655
Lee CW, Huang A, Wang YH, Yang CY, Chen YF, Liu HM (2010) Intracranial dural arteriovenous fistulas: diagnosis and evaluation with 64-detector row CT angiography. Radiology 256(1):219–228. https://doi.org/10.1148/radiol.10091835
Shweel M, Hamdy B (2013) Diagnostic utility of magnetic resonance imaging and magnetic resonance angiography in the radiological evaluation of pulsatile tinnitus. Am J Otolaryngol 34(6):710–717. https://doi.org/10.1016/j.amjoto.2013.08.001
Lin YH, Lin HH, Liu HM, Lee CW, Chen YF (2016) Diagnostic performance of CT and MRI on the detection of symptomatic intracranial dural arteriovenous fistula: a meta-analysis with indirect comparison. Neuroradiology 58(8):753–763. https://doi.org/10.1007/s00234-016-1696-8
Bulters DO, Mathad N, Culliford D, Millar J, Sparrow OC (2012) The natural history of cranial dural arteriovenous fistulae with cortical venous reflux--the significance of venous ectasia. Neurosurgery 70(2):312–318; discussion 318-319. https://doi.org/10.1227/NEU.0b013e318230966f
Kitajima M, Hirai T, Korogi Y, Yamura M, Kawanaka K, Ikushima I, Hayashida Y, Yamashita Y, Kuratsu J (2005) Retrograde cortical and deep venous drainage in patients with intracranial dural arteriovenous fistulas: comparison of MR imaging and angiographic findings. Am J Neuroradiol 26(6):1532–1538
Willinsky R, Terbrugge K, Montanera W, Mikulis D, Wallace MC (1994) Venous congestion: an MR finding in dural arteriovenous malformations with cortical venous drainage. Am J Neuroradiol 15(8):1501–1507
Willinsky R, Goyal M, terBrugge K, Montanera W (1999) Tortuous, engorged pial veins in intracranial dural arteriovenous fistulas: correlations with presentation, location, and MR findings in 122 patients. AJNR Am J Neuroradiol 20(6):1031–1036
Kwon BJ, Han MH, Kang HS, Chang KH (2005) MR imaging findings of intracranial dural arteriovenous fistulas: relations with venous drainage patterns. AJNR Am J Neuroradiol 26(10):2500–2507
Letourneau-Guillon L, Cruz JP, Krings T (2015) CT and MR imaging of non-cavernous cranial dural arteriovenous fistulas: findings associated with cortical venous reflux. Eur J Radiol 84(8):1555–1563. https://doi.org/10.1016/j.ejrad.2015.04.019
Miller TR, Gandhi D (2015) Intracranial dural arteriovenous fistulae: clinical presentation and management strategies. Stroke 46(7):2017–2025. https://doi.org/10.1161/strokeaha.115.008228
Farb RI, Agid R, Willinsky RA, Johnstone DM, Terbrugge KG (2009) Cranial dural arteriovenous fistula: diagnosis and classification with time-resolved MR angiography at 3T. AJNR Am J Neuroradiol 30(8):1546–1551. https://doi.org/10.3174/ajnr.A1646
Noguchi K, Melhem ER, Kanazawa T, Kubo M, Kuwayama N, Seto H (2004) Intracranial dural arteriovenous fistulas: evaluation with combined 3D time-of-flight MR angiography and MR digital subtraction angiography. AJR Am J Roentgenol 182(1):183–190. https://doi.org/10.2214/ajr.182.1.1820183
Noguchi K, Kubo M, Kuwayama N, Kamisaki Y, Tomizawa G, Kameda K, Kawabe H, Ogawa S, Watanabe N, Endo S, Seto H (2006) Intracranial dural arteriovenous fistulas with retrograde cortical venous drainage: assessment with cerebral blood volume by dynamic susceptibility contrast magnetic resonance imaging. AJNR Am J Neuroradiol 27(6):1252–1256
Amukotuwa SA, Heit JJ, Marks MP, Fischbein N, Bammer R (2016) Detection of cortical venous drainage and determination of the Borden type of dural arteriovenous fistula by means of 3D pseudocontinuous arterial spin-labeling MRI. Am J Roentgenol 207(1):163–169. https://doi.org/10.2214/AJR.15.15171
Nakagawa I, Taoka T, Wada T, Nakagawa H, Sakamoto M, Kichikawa K, Hironaka Y, Motoyama Y, Park YS, Nakase H (2013) The use of susceptibility-weighted imaging as an indicator of retrograde leptomeningeal venous drainage and venous congestion with dural arteriovenous fistula: diagnosis and follow-up after treatment. Neurosurgery 72(1):47–54; discussion 55. https://doi.org/10.1227/NEU.0b013e318276f7cc
Letourneau-Guillon L, Krings T (2012) Simultaneous arteriovenous shunting and venous congestion identification in dural arteriovenous fistulas using susceptibility-weighted imaging: initial experience. AJNR Am J Neuroradiol 33(2):301–307. https://doi.org/10.3174/ajnr.A2777
Lagares A, Millan JM, Ramos A, Alen JA, Gallego JH (2010) Perfusion computed tomography in a dural arteriovenous fistula presenting with focal signs: vascular congestion as a cause of reversible neurologic dysfunction. Neurosurgery 66(1):E226–E227; discussion E227. https://doi.org/10.1227/01.neu.0000361996.27921.6c
Willems PW, Brouwer PA, Barfett JJ, terBrugge KG, Krings T (2011) Detection and classification of cranial dural arteriovenous fistulas using 4D-CT angiography: initial experience. AJNR Am J Neuroradiol 32(1):49–53. https://doi.org/10.3174/ajnr.A2248
Kim MS, Han DH, Kwon OK, Oh CW, Han MH (2002) Clinical characteristics of dural arteriovenous fistula. Journal of clinical neuroscience : official journal of the Neurosurgical Society of Australasia 9(2):147–155. https://doi.org/10.1054/jocn.2001.1029
McDougall CG, Halbach VV, Higashida RT, Larsen DW, Dowd CF, Hieshima GB, Wilson CB (1997) Treatment of dural arteriovenous fistulas. Neurosurg Q 7(2):110–134
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this study.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in the studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. For this type of study formal consent is not required.
Informed consent
For this type of retrospective study formal consent is not required.
Rights and permissions
About this article
Cite this article
Lin, YH., Wang, YF., Liu, HM. et al. Diagnostic accuracy of CTA and MRI/MRA in the evaluation of the cortical venous reflux in the intracranial dural arteriovenous fistula DAVF. Neuroradiology 60, 7–15 (2018). https://doi.org/10.1007/s00234-017-1948-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-017-1948-2