Abstract
Introduction
The objective of this study was to explore the volumetric alterations of dural sinuses in patients with idiopathic intracranial hypertension (IIH).
Methods
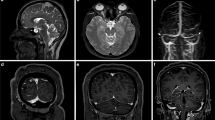
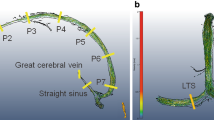
Standardized cranial magnetic resonance imaging (MRI) was used in 17 patients prior to and following treatment of IIH and in seven controls. Magnetic resonance venographies (MRV) were employed for (a) judgement of circumscript dural sinus stenoses and (b) computation of sinus volumes. Cross-sectional areas (CSA) of the superior sagittal sinuses (SSS) were measured on T2-weighted images. Results of the initial MRIs were compared to those on follow-up MRIs and to results of controls.
Results
Stenoses of the transverse sinuses (TS) resulting in cranial venous outflow obstruction (CVOO) were present in 15/17 (88%) patients, normalizing in 7/15 cases (47%) after treatment of IIH. CVOO was not detected in the control group. Segmentation of MRV revealed decreased dural sinus volumes in patients with IIH as compared to controls (P = 0.018). Sinus volumes increased significantly with normalization of intracranial pressure independent from disappearing of TS stenoses (P = 0.007). The CSA of the SSS were normal on the initial MRIs of patients with IIH and increased on follow-up after treatment (P < 0.001). However, volumetries displayed overlap in patients and controls.
Conclusions
Patients with IIH not only exhibit bilateral stenoses of the TS as has been reported, but volume changes of their entire dural sinus system also occur. The potential etiopathological and diagnostic roles of these changes are discussed.



Similar content being viewed by others
References
Monro A (1823) Observations on the structure and function of the nervous system. Creech & Johnson, Edinburgh
Kellie G (1824) Appearances observed in the dissection of two individuals; death from cold and congestion of the brain. Trans Med Chir Soc Edinb 1:84–169
Ball AK, Clarke CE (2006) Idiopathic intracranial hypertension. Lancet Neurol 5:433–442
Bershad EM, Humphreis WE, Suarez JI (2008) Intracranial hypertension. Semin Neurol 28:690–702
Binder DK, Horton JC, Lawton MT et al (2004) Idiopathic intracranial hypertension. Neurosurgery 54:538–551, discussion 551–532
Skau M, Brennum J, Gjerris F et al (2006) What is new about idiopathic intracranial hypertension? An updated review of mechanism and treatment. Cephalalgia 26:384–399
Karahalios DG, Rekate HL, Khayata MH et al (1996) Elevated intracranial venous pressure as a universal mechanism in pseudotumor cerebri of varying etiologies. Neurology 46:198–202
King JO, Mitchell PJ, Thomson KR et al (2002) Manometry combined with cervical puncture in idiopathic intracranial hypertension. Neurology 58:26–30
Farb RI, Vanek I, Scott JN et al (2003) Idiopathic intracranial hypertension: the prevalence and morphology of sinovenous stenosis. Neurology 60:1418–1424
Baryshnik DB, Farb RI (2004) Changes in the appearance of venous sinuses after treatment of disordered intracranial pressure. Neurology 62:1445–1446
Higgins JN, Pickard JD (2004) Lateral sinus stenoses in idiopathic intracranial hypertension resolving after CSF diversion. Neurology 62:1907–1908
McGonigal A, Bone I, Teasdale E (2004) Resolution of transverse sinus stenosis in idiopathic intracranial hypertension after L-P shunt. Neurology 62:514–515
Rohr A, Dorner L, Stingele R et al (2007) Reversibility of venous sinus obstruction in idiopathic intracranial hypertension. AJNR Am J Neuroradiol 28:656–659
Owler BK, Parker G, Halmagyi GM et al (2003) Pseudotumor cerebri syndrome: venous sinus obstruction and its treatment with stent placement. J Neurosurg 98:1045–1055
Higgins JN, Cousins C, Owler BK et al (2003) Idiopathic intracranial hypertension: 12 cases treated by venous sinus stenting. J Neurol Neurosurg Psychiatry 74:1662–1666
Donnet A, Metellus P, Levrier O et al (2008) Endovascular treatment of idiopathic intracranial hypertension: clinical and radiologic outcome of 10 consecutive patients. Neurology 70:641–647
De Simone E, Marano C, Fiorillo F et al (2005) Sudden re-opening of collapsed transverse sinuses and longstanding clinical remission after a single lumbar puncture in a case of idiopathic intracranial hypertension pathogenetic implications. Neurol Sci 25:342–344
Bateman GA, Stevens SA, Stimpson J (2009) A mathematical model of idiopathic intracranial hypertension incorporating increased arterial inflow and variable venous outflow collapsibility. J Neurosurg 110:446–456
Batemen GA (2008) Stenoses in idiopathic intracranial hypertension: to stent or not to stent? AJNR Am J Neuroradiol 29(2):215; author reply 215–6. Comment on Rohr A, Dorner L, Stingele R et al (2007) Reversibility of venous sinus obstruction in idiopathic intracranial hypertension. AJNR Am J Neuroradiol 28:656–659
De Simone R, Ranieri A, Bonavita V (2010) Advancement in idiopathic intracranial hypertension pathogenesis: focus on sinus venous stenosis. Neurol Sci 31(Suppl 1):S33–9
Connor SAJ, Siddiqui MA, Stewart VR, O’Flynn EAM (2008) The relationship of transverse sinus stenosis to bony groove dimensions provides an insight into the aetiology of idiopathic intracranial hypertension. Neuroradiology 50:999–1004
Bono F, Giliberto C, Mastrandrea C et al (2005) Transverse sinus stenoses persist after normalization of the CSF pressure in IIH. Neurology 65:1090–1093
Farb RI, Forghani R, Lee SK et al (2007) The venous distension sign: a diagnostic sign of intracranial hypotension at MR imaging of the brain. AJNR Am J Neuroradiol 28:1489–93
Rohr A, Jensen U, Riedel C et al (2010) MR imaging of the optic nerve sheath in patients with craniospinal hypotension. AJNR Am J Neuroradiol 31:1752–7
Conflict of interest
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rohr, A., Bindeballe, J., Riedel, C. et al. The entire dural sinus tree is compressed in patients with idiopathic intracranial hypertension: a longitudinal, volumetric magnetic resonance imaging study. Neuroradiology 54, 25–33 (2012). https://doi.org/10.1007/s00234-011-0850-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-011-0850-6