Abstract
Purpose
The objective of this meta-analysis is to determine how sacubitril/valsartan (SV) compares to equivalent and sub-equivalent angiotensin receptor blockers (ARB) or angiotensin-converting enzyme inhibitors (ACEI) in patients with heart failure with reduced ejection fraction (HFrEF).
Methods
The databases of PubMed and EMBASE were used to identify those randomized controlled trials which compared SV to ARB/ACEI in patients with HFrEF. Only those trials that reported outcomes regarding total mortality, cardiovascular mortality, and worsening heart failure were considered. Meta-analysis was performed separately in those patients receiving equivalent doses of ARB/ACEI and those receiving sub-equivalent doses. Equivalent doses were SV 97/103 = valsartan 160 mg twice daily = enalapril 20 mg twice daily = ramipril 5 mg twice daily. Meta-analyses were performed using Review Manager 5.4.
Results
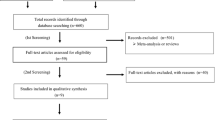
Twelve randomized trials were identified involving 17,484 patients: 11,291 in the sub-equivalent group (8 trials) and 6193 in the equivalent group (4 trials). Meta-analyses showed there were no statistical differences regarding the outcomes of total mortality, cardiovascular mortality, and worsening heart failure in the equivalent dosing group. However, SV reduced total mortality (risk ratio (RR) = 0.85, 95% confidence interval (CI) = 0.78–0.93, p < 0.001), cardiovascular mortality (RR = 0.81, 95% CI = 0.73–0.90, p ≤ 0.001) and worsening heart failure (RR = 0.77, 95% CI = 0.64–0.92, p = 0.005) in the sub-equivalent group.
Conclusion
When compared to equivalent doses of ARB/ACEI, SV is not superior in reducing mortality and worsening heart failure. SV is superior when compared to sub-equivalent doses of ACEI.



Similar content being viewed by others
Data availability
Clinical trial data were extracted from published studies in the PubMed and EMBASE databases. Data from the statistical analyses are included in the manuscript text and figures.
References
Heidenreich PA, Bozkurt B (2022) 2022 AHA/ACC/HFSA guideline for the management of heart failure. J Am Coll Cardiol. https://doi.org/10.1016/j.jacc2021.12.012
McMurray JJV, Packer M, Desai AS et al (2014) Angiotensin-neprilysin inhibition versus enalapril in heart failure. N Engl J Med 371:993–1004
Ahn R, Prasad V (2018) Do limitations in the design of Paradigm-HF justify the slow real world uptake of sacubitril/valsartan (Entresto)? Cardiovasc Drugs Ther 32:633–635
Yandrapalli S, Aronow WS, Mondal P et al (2017) Limitations of sacubitril/valsartan in the management of heart failure. Am J Therap 24:e234–e239
Bernardez-Pereira S, Alvares-Ramires FJ, Tavares de Melo RF et al (2018) Was the enalapril dose too low in the PARADIGM-HF trial? Cardiol Rev 26:196–200
Mandrola J (2021) PARADISE-MI makes me question the benefits of sacubitril/valsartan. Medscape. Available on: https://www.medscape.com/viewarticle/951239
Pfeffer MA, Claggett B, Lewis EF et al (2021) Angiotensin receptor-neprilysin inhibition in acute myocardial infarction. N Engl J Med 385:1845–1855
Mann DL, Givertz MM, Vadere JM et al (2022) Effect of treatment with sacubitril/valsartan in patients with advanced heart failure and reduced ejection fraction: a randomized clinical trial. JAMA Cardiol 7:17–25
Solomon SD, McMurray JJV, Anand IS et al (2019) Angiotensin-neprilysin inhibition in heart failure with preserved ejection fraction. N Engl J Med 381:1609–1620
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
(2015) Sacubitril/Valsartan (Entresto) for Heart Failure. JAMA. 314:722–723. https://doi.org/10.1001/jama.2015.9398
Clinical Resource (2016) ACE Inhibitor antihypertensive dose comparison. Pharmacist's letter/prescriber's letter, Resource #321151
Begic E, Mandzuka M, Begic Z et al (2017) Antihypertensive therapy dose calculator AFMBE Proceedings 62:660–665
Downs SH, Black N (1998) The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. J Epidemiol Community Health 52:377–384
Velazquez EJ, Morrow DA, DeVore AD et al (2019) Angiotensin-neprilysin inhibition in acute decompensated heart failure. N Engl J Med 380:539–548
Piepoli MF, Hussain RI, Comin-Colet J et al (2021) OUTSTEP-HF: randomized controlled trial comparing short-term effects of sacubitril/valsartan versus enalapril on daily physical activity in patients with chronic heart failure with reduced ejection fraction. Eur J Heart Fail 23:127–135
Desai AS, Solomon SD, Shah AM et al (2019) Effect of sacubitril-valsartan vs enalapril on aortic stiffness in patients with heart failure and reduced ejection fraction: a randomized clinical trial. JAMA 322:1077–1084
Bano S, Bai P, Kumar S et al (2021) Comparison of sacubitril/valsartan versus enalapril in the management of heart failure. Cureus 13:e16332
Tsutsui H, Momomura S, Saito Y et al (2021) Efficacy and safety of sacubitril/valsartan in Japanese patients with chronic heart failure and reduced ejection fraction. Results from the PARALLEL-HF study. Circ J 85:584–594
Halle M, Schobel C, Winzer EB et al (2021) A randomized clinical trial on the short-term effects of 12 week sacubitril/valsartan vs. enalapril on peak oxygen consumption in patients with heart failure with reduced ejection fraction: results from the ACTIVITY-HF study. Eur J Heart Fail 23:2073–2082
Khandwalla RM, Grant D, Birkeland K et al (2021) The AWAKE-HF study: sacubitril/valsartan impact on daily physical activity and sleep in heart failure. Am J Cardiovasc Drugs 21:241–254
Ghafur S, Zahid A, Sarkar H et al (2020) Effect of angiotensin receptor-neprilysin inhibit versus valsartan on cardiac status in patients with chronic heart failure with reduced ejection fraction: a randomized clinical trial in Rangpur Medical College Hospital. Bangladesh Open J Intern Med 10:21–34
Zhao Y, Tian LG, Zhang LX et al (2022) The comparative effects of sacubitril/valsartan versus enalapril on pulmonary hypertension due to heart failure with a reduced ejection fraction. Pulm Circ 12:1–8
Packer M, Poole-Wilson PA, Armstrong PW et al (1999) Comparative effects of low and high doses of angiotensin-converting enzyme inhibitor, lisinopril, on morbidity and mortality in chronic heart failure. Circulation 100:2312–2318
Shahzeb Khan M, Fonarow GC, Ahmed A et al (2017) Dose of angiotensin-converting enzyme inhibitors and angiotensin receptor blockers and outcomes in heart failure. A meta-analysis Circ Heart Fail 10:1–8
Konstam MA, Neaton JD, Dickstein K et al (2009) Effects of high-dose versus low-dose losartan on clinical outcomes in patients with heart failure (HEAAL study): a randomised, double-blind trial. Lancet 374:1840–1848
Yasky J, Verho M, Erasmus TP et al (1996) Efficacy of ramipril versus enalapril in patients with mild to moderate essential hypertension. Br J Clin Pract 50:302–310
McAuley D (2017) DRUG COMPARISONS -ACE INHIBITORS – MED EQUIVALENTS. Global RPH. https://globalrph.com/medcalcs/drug-comparisons-ace-inhibitors-medication-equivalents/. Accessed 7 October 2023
Zabludowski J, Rosenfeld J, Akbary MA, Rangoonwala B, Schinzel S (1988) A multi-centre comparative study between ramipril and enalapril in patients with mild to moderate essential hypertension. Curr Med Res Opin 11:93–106
Ruddy MC, Morczek WJ (1993) Comparison of enalapril and ramipril in patients with essential hypertension. Pharmacotherapy 13:224–228
(2023) Heart failure. Centers for Disease Control and Prevention. https://www.cdc.gov/heartdisease/heart_failure.htm. Accessed 7 October 2023
Mukhopadhyay A, Adhikari S, Li X et al (2022) Association between copayment amount and filling of medications for angiotensin receptor neprilysin inhibitors in patients with heart failure. J Am Heart Assoc 11:e027662. https://doi.org/10.1161/JAHA.122.027662
Author information
Authors and Affiliations
Contributions
JPR was involved in the conception, research, and writing of this manuscript. CKM was involved in the research and review of this manuscript.
Corresponding author
Ethics declarations
Ethical approval
Since this was a meta-analysis and individual human subjects were not involved, this study was exempted from needing approval by our local IRB or R&D committee.
Consent to participate
This study is a meta-analysis, and individual human subjects were not included, so consent was not needed.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rindone, J.P., Mellen, C.K. Sacubitril/valsartan compared to equivalent/sub-equivalent dose angiotensin receptor blocker or angiotensin-converting enzyme inhibitor in heart failure with reduced ejection fraction: a meta-analysis of randomized trials. Eur J Clin Pharmacol (2024). https://doi.org/10.1007/s00228-024-03686-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00228-024-03686-6