Abstract
Aim
Drug-drug interactions are sometimes neglected in oncology practice. Due to drug pharmacokinetic and pharmacodynamic interactions, clinically increased or decreased drug effects and increased or decreased adverse effects may occur. Considering that the concomitant use of these two drugs that affect vascular endothelial growth factor receptor (VEGFR) may cause pharmacological potentiation or additive interaction, we aimed to evaluate the survival outcomes of concomitant use of bevacizumab and beta blockers in patients with metastatic colorectal cancer (mCRC).
Methods
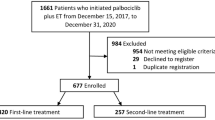
In total, 181 patients with mCRC administered with bevacizumab plus cytotoxic chemotherapy regimen in a first-line setting were divided into two groups: concomitant beta-blocker user and nonuser.
Results
The median overall survival (mOS) was 35.9 (95% CI: 27.9–43.9) months in the beta-blocker-using group and 29.6 (95% CI: 27.9–43.9) months in the beta-blocker-non-using group (p = 0.054). The median progression-free survival (mPFS) was 16.1 (95% CI: 12.4–19.9) months in the beta-blocker-using group and 12.8 (95% CI: 10.6–15.0) months in the beta-blocker-non-using group (p = 0.006). The multivariate analysis revealed that beta-blocker use was an independent predictor of mPFS (HR: 0.66, 95% CI: 0.46–0.93, p = 0.018) and mOS (HR: 0.57, 95% CI: 0.36–0.91, p = 0.02).
Conclusion
This study demonstrated that concomitant usage of beta blockers improved both survival outcomes, irrespective of the kind of beta blocker.

Similar content being viewed by others
Data availability
Data can be accessed from the corresponding author.
References
Cancer IAfRo (2020) Cancer IAfRo: GLOBOCAN 2020: estimated cancer incidence, mortality, and prevalence worldwide in 2020. In Website
Kasi PM, Hubbard JM, Grothey A (2015) Selection of biologics for patients with metastatic colorectal cancer: the role of predictive markers. Expert Rev Gastroenterol Hepatol 9:273–276
Roche Registration Limited (2009) Avastin (bevacizumab) summary of product characteristics (last update 10/19/2016). https://www.ema.europa.eu/en/documents/product-information/avastin-epar-product-information_en.pdf Accessed 12 Dec 2022.
Hurwitz H, Fehrenbacher L, Novotny W, Cartwright T, Hainsworth J, Heim W, Berlin J, Baron A, Griffing S, Holmgren E (2004) Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 350:2335–2342
Giantonio BJ, Catalano PJ, Meropol NJ, O’Dwyer PJ, Mitchell EP, Alberts SR, Schwartz MA, Benson AB III (2007) Bevacizumab in combination with oxaliplatin, fluorouracil, and leucovorin (FOLFOX4) for previously treated metastatic colorectal cancer: results from the Eastern Cooperative Oncology Group Study E3200. J Clin Oncol 25:1539–1544
Strickler JH, Hurwitz HI (2012) Bevacizumab-based therapies in the first-line treatment of metastatic colorectal cancer. Oncologist 17:513–524
Melhem-Bertrandt A, Chavez-MacGregor M, Lei X, Brown EN, Lee RT, Meric-Bernstam F, Sood AK, Conzen SD, Hortobagyi GN, Gonzalez-Angulo A-M (2011) Beta-blocker use is associated with improved relapse-free survival in patients with triple-negative breast cancer. J Clin Oncol 29:2645
Heitz F, du Bois A, Harter P, Kurzeder C, Lubbe D, Vergote I, Plante M, Pfisterer J (2012) Impact of beta-blocker medication in patients with platinum sensitive recurrent ovarian cancer–a combined analysis of 2 prospective multicenter trials by the AGO study group, NCIC-CTG and EORTC-CTG. Eur J Cancer 48:186–187
Armaiz-Pena GN, Allen JK, Cruz A, Stone RL, Nick AM, Lin YG, Han LY, Mangala LS, Villares GJ, Vivas-Mejia P (2013) Src activation by β-adrenoreceptors is a key switch for tumour metastasis. Nat Commun 4:1–12
Thaker PH, Han LY, Kamat AA, Arevalo JM, Takahashi R, Lu C, Jennings NB, Armaiz-Pena G, Bankson JA, Ravoori M (2006) Chronic stress promotes tumor growth and angiogenesis in a mouse model of ovarian carcinoma. Nat Med 12:939–944
Stewart CL, Warner S, Ito K, Raoof M, Wu GX, Lu W-P, Kessler J, Kim JY, Fong Y (2018) Cytoreduction for colorectal metastases: liver, lung, peritoneum, lymph nodes, bone, brain. When does it palliate, prolong survival, and potentially cure? Curr Probl Surg 55:330
Hashizume R, Kawahara H, Ogawa M, Suwa K, Eto K, Yanaga K (2019) CA19-9 concentration after first-line chemotherapy is prognostic predictor of metastatic colon cancer. In Vivo 33:2087–2093
Neugut AI, Lin A, Raab GT, Hillyer GC, Keller D, O’Neil DS, Accordino MK, Kiran RP, Wright J, Hershman DL (2019) FOLFOX and FOLFIRI use in stage IV colon cancer: analysis of SEER-medicare data. Clin Colorectal Cancer 18:133–140
Schuller HM (2010) Beta-adrenergic signaling, a novel target for cancer therapy? Oncotarget 1:466–469
Yang EV, Sood AK, Chen M, Li Y, Eubank TD, Marsh CB, Jewell S, Flavahan NA, Morrison C, Yeh P-E (2006) Norepinephrine up-regulates the expression of vascular endothelial growth factor, matrix metalloproteinase (MMP)-2, and MMP-9 in nasopharyngeal carcinoma tumor cells. Cancer Res 66:10357–10364
Shahzad MM, Arevalo JM, Armaiz-Pena GN, Lu C, Stone RL, Moreno-Smith M, Nishimura M, Lee J-W, Jennings NB, Bottsford-Miller J (2010) Stress effects on FosB-and interleukin-8 (IL8)-driven ovarian cancer growth and metastasis. J Biol Chem 285:35462–35470
Nilsson MB, Armaiz-Pena G, Takahashi R, Lin YG, Trevino J, Li Y, Jennings N, Arevalo J, Lutgendorf SK, Gallick GE (2007) Stress hormones regulate interleukin-6 expression by human ovarian carcinoma cells through a Src-dependent mechanism. J Biol Chem 282:29919–29926
Sood AK, Armaiz-Pena GN, Halder J, Nick AM, Stone RL, Hu W, Carroll AR, Spannuth WA, Deavers MT, Allen JK (2010) Adrenergic modulation of focal adhesion kinase protects human ovarian cancer cells from anoikis. J Clin Invest 120:1515–1523
Masur K, Niggemann B, Zanker KS, Entschladen F (2001) Norepinephrine-induced migration of SW 480 colon carcinoma cells is inhibited by β-blockers. Cancer Res 61:2866–2869
Stiles JM, Amaya C, Rains S, Diaz D, Pham R, Battiste J, Modiano JF, Kokta V, Boucheron LE, Mitchell DC (2013) Targeting of beta adrenergic receptors results in therapeutic efficacy against models of hemangioendothelioma and angiosarcoma. PLoS One 8:e60021
Olgun Y, Aktas S, Sutay S, Ecevit MC (2022) The effect of bevacizumab and propranolol on nasal polyposis. Int J Clin Prac 2022:6174664
Zhong S, Yu D, Zhang X, Chen X, Yang S, Tang J, Zhao J, Wang S (2016) β-blocker use and mortality in cancer patients: systematic review and meta-analysis of observational studies. Eur J Cancer Prev 25:440–448
Na Z, Qiao X, Hao X, Fan L, Xiao Y, Shao Y, Sun M, Feng Z, Guo W, Li J (2018) The effects of beta-blocker use on cancer prognosis: a meta-analysis based on 319,006 patients. Onco Targets Ther 11:4913
Musselman R, Li W, Gomes T, Mamdani M, Haggar F, Moloo H, Boushey R, Al-Omran M, Al-Obeed O, VanWalraven C (2014) Association between beta blocker usage and cancer survival in a large, matched population study among hypertensive patients. J Surg Res 186:639–640
Grytli HH, Fagerland MW, Fosså SD, Taskén KA (2014) Association between use of β-blockers and prostate cancer–specific survival: a cohort study of 3561 prostate cancer patients with high-risk or metastatic disease. Eur Urol 65:635–641
Giampieri R, Scartozzi M, Del Prete M, Faloppi L, Bianconi M, Ridolfi F, Cascinu S (2015) Prognostic value for incidental antihypertensive therapy with β-blockers in metastatic colorectal cancer. Medicine 94(24)
Fiala O, Ostasov P, Sorejs O, Liska V, Buchler T, Poprach A, Finek J (2019) Incidental use of beta-blockers is associated with outcome of metastatic colorectal cancer patients treated with bevacizumab-based therapy: a single-institution retrospective analysis of 514 patients. Cancers 11:1856
Author information
Authors and Affiliations
Contributions
Concept—EH, ME, and MA. Design—MU, EH, and MA. Data collection and/or processing—all authors. Analysis and/or interpretation—MZK, MKE, and MA. Literature search—MA, MKE, MA, and MU. Writing—MU, MZK, and MA. Critical reviews—all authors.
Corresponding author
Ethics declarations
Ethics approval
Ethics approval was obtained from the Ethics Committee of Necmettin Erbakan University (approval no: 2022/3779).
Informed consent
Written informed consent was not obtained as the study was a retrospective study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kocak, M.Z., Er, M., Ugrakli, M. et al. Could the concomitant use of beta blockers with bevacizumab improve survival in metastatic colon cancer?. Eur J Clin Pharmacol 79, 485–491 (2023). https://doi.org/10.1007/s00228-023-03464-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-023-03464-w