Abstract
Purpose
A standardized medication plan for patients has been developed and recently enacted into German law depicting all medicines taken. It can only increase medication safety if patients use and understand it. We evaluated patients’ comprehensibility of the medication plan and analyzed potential variables influencing patients’ understanding.
Methods
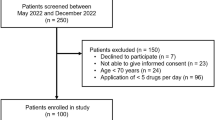
The medication plan template v2.0 was first tested in N = 40 patients, and the “Evaluation Tool to test the handling of the Medication Plan” (ET-MP) was developed, rating patients’ understanding from 0 to 100 %. The cut-off, distinguishing if patients understand the medication plan, was set at 90 %. The ET-MP was then applied to an amended medication plan questioning N = 40 general internal medicine (GIM) and N = 50 patients with chronic heart failure (CHF).
Results
The mean (± standard deviation (SD)) age of the study cohort was 69 ± 13 years, 47 % female. Patients took 8 ± 3 drugs chronically. The CHF patients had a lower level of education compared to the GIM group (p = 0.004). The overall ET-MP score was 82 ± 21 % (GIM 86 ± 19 %, CHF 78 ± 23 %; p = 0.16). Forty-three percent achieved a score >90 %. A moderate correlation was found between the ET-MP score and the level of education (r = 0.45) and age (r = −0.46), respectively (both p < 0.001). Cognitively impaired CHF patients (p = 0.03) and patients with advanced CHF (p = 0.006) achieved a lower ET-MP score. In the CHF cohort, signs of depression or a lower level of self-care behaviour were not associated with a lower ET-MP score.
Conclusion
The ET-MP is suitable to explore patients’ understanding of a medication plan. Less than 50 % of the patients reached a score above 90 %. Higher age and lower level of education but not the diagnosis of CHF seem to correlate with impaired understanding of the standardized medication plan. In addition to a medication plan, a significant number of patients are in need of further and continuous care to improve medication safety.


Similar content being viewed by others
References
Ewen S, Baumgarten T, Rettig-Ewen V et al (2015) Analyses of drugs stored at home by elderly patients with chronic heart failure. Clin Res Cardiol 104(4):320–327. doi:10.1007/s00392-014-0783-2
Bedell SE, Jabbour S, Goldberg R et al (2000) Discrepancies in the use of medications: their extent and predictors in an outpatient practice. Arch Intern Med 160(14):2129–2134. doi:10.1001/archinte.160.14.2129
Carow F, Rieger K, Walter-Sack I et al (2012) Objective assessment of nonadherence and unknown co-medication in hospitalized patients. Eur J Clin Pharmacol 68(8):1191–1199. doi:10.1007/s00228-012-1229-2
McGuire LC (1996) Remembering what the doctor said: organization and adults’ memory for medical information. Exp Aging Res 22(4):403–428. doi:10.1080/03610739608254020
Tarn DM, Heritage J, Paterniti DA et al (2006) Physician communication when prescribing new medications. Arch Intern Med 166(17):1855–1862. doi:10.1001/archinte.166.17.1855
Send AF, Schwab M, Gauss A et al (2014) Pilot study to assess the influence of an enhanced medication plan on patient knowledge at hospital discharge. Eur J Clin Pharmacol 70(10):1243–1250. doi:10.1007/s00228-014-1723-9
Botermann L, Schulz M (2014) Grundlegende Voraussetzungen für die elektronische Abbildung von Arzneimitteldaten im Hinblick auf den Medikationsplan. Aktionsplan Arzneimitteltherapiesicherheit (AMTS) des Bundesministeriums für Gesundheit (BMG). Abschlussbericht. https://www.bundesgesundheitsministerium.de/service/publikationen/einzelansicht.html?tx_rsmpublications_pi1[publication]=2590&tx_rsmpublications_pi1[action]=show&tx_rsmpublications_pi1[controller]=Publication&cHash=202aa6380f3ec6c375c5479cebe026cc. Accessed 19 Feb 2016
Koordinierungsgruppe zur Umsetzung und Fortschreibung des Aktionsplanes zur Verbesserung der Arzneimitteltherapiesicherheit in Deutschland (2013) Spezifikation für einen patientenbezogenen Medikationsplan. Version 2.0-für Modellvorhaben. http://www.akdae.de/AMTS/Medikationsplan/index.html. Accessed 19 Feb 2016
Send AF, Al-Ayyash A, Schecher S et al (2013) Development of a standardized knowledge base to generate individualized medication plans automatically with drug administration recommendations. Br J Clin Pharmacol 76(Suppl 1):37–46
Bailey SC, Pandit AU, Yin S et al (2009) Predictors of misunderstanding pediatric liquid medication instructions. Fam Med 41(10):715–721
Davis TC, Wolf MS, Bass PF 3rd et al (2006) Literacy and misunderstanding prescription drug labels. Ann Intern Med 145(12):887–894. doi:10.7326/0003-4819-145-12-200612190-00144
Gazmararian JA, Baker DW, Williams MV et al (1999) Health literacy among Medicare enrollees in a managed care organization. JAMA 281(6):545–551. doi:10.1001/jama.281.6.545
King SR, McCaffrey DJ, Bouldin AS (2011) Health literacy in the pharmacy setting: defining pharmacotherapy literacy. Pharm Pract (Granada) 9(4):213–220
Coughlan D, Sahm L, Byrne S (2012) The importance of health literacy in the development of ‘Self Care’ cards for community pharmacies in Ireland. Pharm Pract (Granada) 10(3):143–150
McNaughton CD, Cawthon C, Kripalani S et al (2015) Health literacy and mortality: a cohort study of patients hospitalized for acute heart failure. J Am Heart Assoc 4(5):1–9. doi:10.1161/JAHA.115.001799
Raynor DK (2008) Testing, testing: the benefits of user-testing package leaflets. Regulatory Focus April, pp 16–19. http://www.raps.org/WorkArea/DownloadAsset.aspx?id=4041. Accessed 14 Jun 2016
European Commission (2009) Guideline on the readability of the labelling and package leaflet of medicinal products for human use. http://ec.europa.eu/health/files/eudralex/vol-2/c/2009_01_12_readability_guideline_final_en.pdf. Accessed 19 Feb 2016
Brockmeyer R, Steindl L, Behrens L et al (2001) Testing of the readability of package inserts at a community pharmacy. Pharm Ind 63(2):114–119
Kuske S, Lessing C, Lux R et al (2012) Patientensicherheitsindikatoren zur Arzneimitteltherapiesicherheit (AMTS-PSI): Internationaler Status, Übertragbarkeit und Validierung (Patient safety indicators for medication safety (AMTS-PSI): international status, transferability and validation). Gesundheitswesen 74(2):79–86. doi:10.1055/s-0030-1269838
Wenger NS, Young RT (2007) Quality indicators for continuity and coordination of care in vulnerable elders. J Am Geriatr Soc 55(Suppl 2):S285–S292. doi:10.1111/j.1532-5415.2007.01334.x
Committee on Identifying and Preventing Medication Errors (2006) What can you do to avoid medication errors. fact sheet. http://iom.nationalacademies.org/~/media/Files/Report%20Files/2006/Preventing-Medication-Errors-Quality-Chasm-Series/medicationerrorsfactsheet.pdf. Accessed 19 Feb 2016
Bundesministerium für Gesundheit (2010) Aktionsplan 2010–2012 des Bundesministeriums für Gesundheit zur Verbesserung der Arzneimitteltherapiesicherheit in Deutschland. Aktionsplan AMTS 2010–2012. http://www.akdae.de/AMTS/Aktionsplan/index.html. Accessed 19 Feb 2016
Deutscher Bundestag (2015) Gesetz für sichere digitale Kommunikation und Anwendungen im Gesundheitswesen. E-Health-Gesetz. http://www.bgbl.de/xaver/bgbl/start.xav?startbk=Bundesanzeiger_BGBl&jumpTo=bgbl115s2408.pdf. Accessed 19 Feb 2016
Botermann L, Krueger K, Eickhoff C et al (2016) Patients’ handling of a standardized medication plan: a pilot study and method development. Patient Prefer and Adherence 10:621–630. doi:10.2147/PPA.S96431
Viktil KK, Blix HS, Moger TA et al (2007) Polypharmacy as commonly defined is an indicator of limited value in the assessment of drug-related problems. Br J Clin Pharmacol 63(2):187–195. doi:10.1111/j.1365-2125.2006.02744.x
Thürmann PA, Selke GW (2014) Arzneimittelversorgung älterer Patienten. In: Klauber J, Günster C, Gerste B et al (eds) Versorgungs-Report 2013/2014. Schattauer, Stuttgart, pp 185–204
Hilmer SN (2008) The dilemma of polypharmacy. Aust Prescr 31(1):2–3
Charlson ME, Pompei P, Ales KL et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383. doi:10.1016/0021-9681(87)90171-8
Gräfe K, Zipfel S, Herzog W et al (2004) Screening psychischer Störungen mit dem “Gesundheitsfragebogen für Patienten (PHQ-D)”. Diagnostica 50(4):171–181. doi:10.1026/0012-1924.50.4.171
Kroenke K, Spitzer RL, Williams JB (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16(9):606–613. doi:10.1046/j.1525-1497.2001.016009606.x
Köberich S, Glattacker M, Jaarsma T et al (2013) Validity and reliability of the German version of the 9-item European Heart Failure Self-care Behaviour Scale. Eur J Cardiovasc Nurs 12(2):150–158. doi:10.1177/1474515112438639
Jaarsma T, Arestedt KF, Mårtensson J et al (2009) The European Heart Failure Self-care Behaviour scale revised into a nine-item scale (EHFScB-9): a reliable and valid international instrument. Eur J Heart Fail 11(1):99–105. doi:10.1093/eurjhf/hfn007
Borson S, Scanlan J, Brush M et al (2000) The Mini-Cog: a cognitive ‘vital signs’ measure for dementia screening in multi-lingual elderly. Int J Geriatr Psychiatry 15(11):1021–1027. doi:10.1002/1099-1166(200011)15:11<1021
Kroenke K, Spitzer RL (2002) The PHQ-9: a new depression diagnostic and severity measure. Psychiatr Ann 32(9):509–515. doi:10.3928/0048-5713-20020901-06
Azodi K, Himstedt S, Hinrichs A et al (2002) Testing of the readability of package leaflets as an initial step under the pharmaceutical care initiative towards increasing the safety of medicinal products. Pharm Ind 64(11):1119–1125
Koordinierungsgruppe zur Umsetzung und Fortschreibung des Aktionsplanes zur Verbesserung der Arzneimitteltherapiesicherheit in Deutschland (2015) Medikationsplan V2.0. Erste Ergebnisse des Lesbarkeitstests zum einheitlichen patientenbezogenen Medikationsplan. http://www.akdae.de/AMTS/Medikationsplan/. Accessed 19 Feb 2016
Arzneimittel Initiative Sachsen Thüringen (ARMIN)-Projektgruppe (2015) Umsetzung einer Zusatzanforderung zur Spezifikation 2.0 (korr.) des patientenorientierten Medikationsplans im Rahmen des Modellprojekts ARMIN. Änderung der Tabellenüberschrift der Spalte Dosierungsschema. http://www.akdae.de/AMTS/Medikationsplan/docs/Prima.pdf. Accessed 19 Feb 2016
Waltering I, Schwalbe O, Hempel G (2015) Discrepancies on medication plans detected in German community pharmacies. J Eval Clin Pract 21(5):886–892. doi:10.1111/jep.12395
Krüger-Brand H (2015) Arzneimitteltherapie. Medikationsplan für mehr Sicherheit. Dtsch Ärztebl 112(35–36):A1410–A1413
Koster ES, Philbert D, Bouvy ML (2015) Health literacy among pharmacy visitors in the Netherlands. Pharmacoepidemiol Drug Saf 24(7):716–721. doi:10.1002/pds.3803
Raynor DK (2009) Addressing medication literacy: a pharmacy practice priority. Int J Pharm Pract 17(5):257–259
Dunlay SM, Redfield MM, Weston SA et al (2009) Hospitalizations after heart failure diagnosis: a community perspective. J Am Coll Cardiol 54(18):1695–1702. doi:10.1016/j.jacc.2009.08.019
McMurray JJV, Adamopoulos S, Anker SD et al (2012) ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure 2012: the Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2012 of the European Society of Cardiology. Developed in collaboration with the Heart Failure Association (HFA) of the ESC. Eur Heart J 33(14):1787–1847. doi:10.1093/eurheartj/ehs104
Sokol MC, McGuigan KA, Verbrugge RR et al (2005) Impact of medication adherence on hospitalization risk and healthcare cost. Med Care 43(6):521–530
Krueger K, Botermann L, Schorr SG et al (2015) Age-related medication adherence in patients with chronic heart failure: a systematic literature review. Int J Cardiol 184:728–735. doi:10.1016/j.ijcard.2015.03.042
Rutledge T, Reis VA, Linke SE et al (2006) Depression in heart failure: a meta-analytic review of prevalence, intervention effects, and associations with clinical outcomes. J Am Coll Cardiol 48(8):1527–1537. doi:10.1016/j.jacc.2006.06.055
Ladwig K, Lederbogen F, Albus C, et al. (2014) Position paper on the importance of psychosocial factors in cardiology: update 2013. Ger Med Sci 12: Doc09. doi: 10.3205/000194
Kindermann I, Fischer D, Karbach J et al (2012) Cognitive function in patients with decompensated heart failure: the Cognitive Impairment in Heart Failure (CogImpair-HF) study. Eur J Heart Fail 14(4):404–413. doi:10.1093/eurjhf/hfs015
Fikenzer K, Knoll A, Lenski D et al (2014) Chronische Herzinsuffizienz: Teufelskreis aus geringer Einnahmetreue von Medikamenten und kardialer Dekompensation (Poor medication adherence and worsening of heart failure—a vicious circle). Dtsch Med Wochenschr 139(47):2390–2394. doi:10.1055/s-0034-1387391
Acknowledgments
We thank the participating community pharmacies for their support in recruiting study participants. We acknowledge the contributions of Maike Petersen, Sophie Bronkow and Saskia Koslowski, pharmacy students at the Freie Universitaet Berlin, for conducting interviews in the main investigation.
Contribution of the authors
Contributors: LB substantially contributed to the conception and design of the study, recruitment and data collection of the pilot and GIM patients, overall data analyses and writing of the manuscript. KM substantially contributed in the recruitment, data collection and analyses of the CHF patients. KK, CE and MS contributed to the conception and design of the study as well as writing the manuscript. AW and UL contributed in the recruitment and data collection of CHF patients. CK and UL contributed to the conception and design of the study. All authors contributed in critically revising the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Funding
The pilot study was funded by the German Federal Ministry of Health as part of the PRIMA project (Primärsystem-Integration des Medikationsplans mit Akzeptanzuntersuchung, ref. no. 2514ATS001).
Rights and permissions
About this article
Cite this article
Botermann, L., Monzel, K., Krueger, K. et al. Evaluating patients’ comprehensibility of a standardized medication plan. Eur J Clin Pharmacol 72, 1229–1237 (2016). https://doi.org/10.1007/s00228-016-2082-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-016-2082-5