Abstract
Purpose
To determine factors associated with low persistence in patients initiated on drug treatment for hypertension.
Methods
Cohort study using medical records for patients with hypertension in 48 Swedish primary healthcare centres. Data were linked to national registers on dispensed drugs, hospitalizations, outpatient hospital consultations, deaths, migration, and socioeconomy. We identified 5225 patients (55 % women, mean age 61 years) initiated on antihypertensive drug treatment during 2006–2007. Persistence was measured for two years by the dispensed drugs. Patients with a gap of >30 days between end of dispensed supply and the next dispensed prescription were classified as non-persistent. This was calculated by Kaplan–Meier analysis. Cox proportional hazard regression was used to estimate hazard ratios for discontinuation. Potential predictors included age, gender, blood pressure before initiation of therapy, cardiovascular comorbidity, educational level, country of birth, and income.
Results
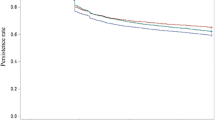
Among patients with a dispensed first prescription, 26 % discontinued treatment during the first year, and a further 9 % discontinued during the second year. Discontinuation (all adjusted) was more common in men (P = 0.002) and in younger patients (30–49 years, P < 0.001). Systolic (P < 0.001) but not diastolic blood pressure was positively associated with persistence. Native-born Swedish citizens and patients born in the other Nordic countries had lower discontinuation rates than those born outside the Nordic countries (P < 0.001).
Conclusion
Major determinants of discontinuation of antihypertensive drug treatment are male sex, young age, mild-to-moderate systolic blood pressure elevation, and birth outside of Sweden.





Similar content being viewed by others
References
Kearney PM, Whelton M, Reynolds K, Muntner P, Whelton PK, He J (2005) Global burden of hypertension: analysis of worldwide data. Lancet 365(9455):217–223. doi:10.1016/S0140-6736(05)17741-1
Lim SS, Vos T, Flaxman AD, Danaei G, Shibuya K, Adair-Rohani H, Amann M, Anderson HR, Andrews KG, Aryee M, Atkinson C, Bacchus LJ, Bahalim AN, Balakrishnan K, Balmes J, Barker-Collo S, Baxter A, Bell ML, Blore JD, Blyth F, Bonner C, Borges G, Bourne R, Boussinesq M, Brauer M, Brooks P, Bruce NG, Brunekreef B, Bryan-Hancock C, Bucello C, Buchbinder R, Bull F, Burnett RT, Byers TE, Calabria B, Carapetis J, Carnahan E, Chafe Z, Charlson F, Chen H, Chen JS, Cheng AT, Child JC, Cohen A, Colson KE, Cowie BC, Darby S, Darling S, Davis A, Degenhardt L, Dentener F, Des Jarlais DC, Devries K, Dherani M, Ding EL, Dorsey ER, Driscoll T, Edmond K, Ali SE, Engell RE, Erwin PJ, Fahimi S, Falder G, Farzadfar F, Ferrari A, Finucane MM, Flaxman S, Fowkes FG, Freedman G, Freeman MK, Gakidou E, Ghosh S, Giovannucci E, Gmel G, Graham K, Grainger R, Grant B, Gunnell D, Gutierrez HR, Hall W, Hoek HW, Hogan A, Hosgood HD 3rd, Hoy D, Hu H, Hubbell BJ, Hutchings SJ, Ibeanusi SE, Jacklyn GL, Jasrasaria R, Jonas JB, Kan H, Kanis JA, Kassebaum N, Kawakami N, Khang YH, Khatibzadeh S, Khoo JP, Kok C, Laden F, Lalloo R, Lan Q, Lathlean T, Leasher JL, Leigh J, Li Y, Lin JK, Lipshultz SE, London S, Lozano R, Lu Y, Mak J, Malekzadeh R, Mallinger L, Marcenes W, March L, Marks R, Martin R, McGale P, McGrath J, Mehta S, Mensah GA, Merriman TR, Micha R, Michaud C, Mishra V, Hanafiah KM, Mokdad AA, Morawska L, Mozaffarian D, Murphy T, Naghavi M, Neal B, Nelson PK, Nolla JM, Norman R, Olives C, Omer SB, Orchard J, Osborne R, Ostro B, Page A, Pandey KD, Parry CD, Passmore E, Patra J, Pearce N, Pelizzari PM, Petzold M, Phillips MR, Pope D, Pope CA 3rd, Powles J, Rao M, Razavi H, Rehfuess EA, Rehm JT, Ritz B, Rivara FP, Roberts T, Robinson C, Rodriguez-Portales JA, Romieu I, Room R, Rosenfeld LC, Roy A, Rushton L, Salomon JA, Sampson U, Sanchez-Riera L, Sanman E, Sapkota A, Seedat S, Shi P, Shield K, Shivakoti R, Singh GM, Sleet DA, Smith E, Smith KR, Stapelberg NJ, Steenland K, Stockl H, Stovner LJ, Straif K, Straney L, Thurston GD, Tran JH, Van Dingenen R, van Donkelaar A, Veerman JL, Vijayakumar L, Weintraub R, Weissman MM, White RA, Whiteford H, Wiersma ST, Wilkinson JD, Williams HC, Williams W, Wilson N, Woolf AD, Yip P, Zielinski JM, Lopez AD, Murray CJ, Ezzati M (2013) A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380(9859):2224–2260. doi:10.1016/S0140-6736(12)61766-8
Staessen JA, Li Y, Thijs L, Wang JG (2005) Blood pressure reduction and cardiovascular prevention: an update including the 2003–2004 secondary prevention trials. Hypertens Res 28(5):385–407. doi:10.1291/hypres.28.385
Law MR, Morris JK, Wald NJ (2009) Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies. BMJ 338:b1665
Wolf-Maier K, Cooper RS, Kramer H, Banegas JR, Giampaoli S, Joffres MR, Poulter N, Primatesta P, Stegmayr B, Thamm M (2004) Hypertension treatment and control in five European countries, Canada, and the United States. Hypertension 43(1):10–17. doi:10.1161/01.HYP.0000103630.72812.10
Qvarnström M, Wettermark B, Ljungman C, Zarrinkoub R, Hasselström J, Manhem K, Sundström A, Kahan T (2011) Antihypertensive treatment and control in a large primary care population of 21 167 patients. J Hum Hypertens 25(8):484–491. doi:10.1038/jhh.2010.86
Bramley TJ, Gerbino PP, Nightengale BS, Frech-Tamas F (2006) Relationship of blood pressure control to adherence with antihypertensive monotherapy in 13 managed care organizations. J Manag Care Pharm 12(3):239–245
Breekveldt-Postma NS, Penning-van Beest FJ, Siiskonen SJ, Koerselman J, Klungel OH, Falvey H, Vincze G, Herings RM (2008) Effect of persistent use of antihypertensives on blood pressure goal attainment. Curr Med Res Opin 24(4):1025–1031. doi:10.1185/030079908X280554
DiMatteo MR, Giordani PJ, Lepper HS, Croghan TW (2002) Patient adherence and medical treatment outcomes: A meta-analysis. Med Care 40(9):794–811. doi:10.1097/01.MLR.0000024612.61915.2D
Krousel-Wood M, Thomas S, Muntner P, Morisky D (2004) Medication adherence: a key factor in achieving blood pressure control and good clinical outcomes in hypertensive patients. Curr Opin Cardiol 19(4):357–362
Cramer JA, Roy A, Burrell A, Fairchild CJ, Fuldeore MJ, Ollendorf DA, Wong PK (2008) Medication compliance and persistence: terminology and definitions. Value Health 11(1):44–47. doi:10.1111/j.1524-4733.2007.00213.x
Cramer JA, Benedict A, Muszbek N, Keskinaslan A, Khan ZM (2008) The significance of compliance and persistence in the treatment of diabetes, hypertension and dyslipidaemia: a review. Int J Clin Pract 62(1):76–87. doi:10.1111/j.1742-1241.2007.01630.x
Friedman O, McAlister FA, Yun L, Campbell NR, Tu K (2010) Antihypertensive drug persistence and compliance among newly treated elderly hypertensives in ontario. Am J Med 123(2):173–181. doi:10.1016/j.amjmed.2009.08.008
Hasford J, Schroder-Bernhardi D, Rottenkolber M, Kostev K, Dietlein G (2007) Persistence with antihypertensive treatments: results of a 3-year follow-up cohort study. Eur J Clin Pharmacol 63(11):1055–1061. doi:10.1007/s00228-007-0340-2
Nicotra F, Wettermark B, Sturkenboom MC, Parodi A, Bellocco R, Ekbom A, Merlino L, Leimanis A, Mancia G, Fored M, Corrao G (2009) Management of antihypertensive drugs in three European countries. J Hypertens 27(9):1917–1922. doi:10.1097/HJH.0b013e32832d4692
Selmer R, Blix HS, Landmark K, Reikvam A (2012) Choice of initial antihypertensive drugs and persistence of drug use–a 4-year follow-up of 78,453 incident users. Eur J Clin Pharmacol 68(10):1435–1442. doi:10.1007/s00228-012-1261-2
Simons LA, Ortiz M, Calcino G (2008) Persistence with antihypertensive medication: Australia-wide experience, 2004–2006. Med J Aust 188(4):224–227
van Wijk BL, Shrank WH, Klungel OH, Schneeweiss S, Brookhart MA, Avorn J (2008) A cross-national study of the persistence of antihypertensive medication use in the elderly. J Hypertens 26(1):145–153. doi:10.1097/HJH.0b013e32826308b4
Wong MC (2008) Short- and long-term discontinuation patterns of commonly prescribed antihypertensive drugs among a Chinese population: cohort study. J Hum Hypertens 22(6):435–437. doi:10.1038/jhh.2008.13
Andrade SE, Kahler KH, Frech F, Chan KA (2006) Methods for evaluation of medication adherence and persistence using automated databases. Pharmacoepidemiol Drug Saf 15(8):565–574. doi:10.1002/pds.1230, discussion 575–567
Bautista LE (2008) Predictors of persistence with antihypertensive therapy: results from the NHANES. Am J Hypertens 21(2):183–188. doi:10.1038/ajh.2007.33
Tamblyn R, Abrahamowicz M, Dauphinee D, Wenghofer E, Jacques A, Klass D, Smee S, Eguale T, Winslade N, Girard N, Bartman I, Buckeridge DL, Hanley JA (2010) Influence of physicians’ management and communication ability on patients’ persistence with antihypertensive medication. Arch Intern Med 170(12):1064–1072. doi:10.1001/archinternmed.2010.167
Hasselström J, Zarrinkoub R, Holmquist C, Hjerpe P, Ljungman C, Qvarnström M, Wettermark B, Manhem K, Kahan T, Bengtsson Boström K (2013) The Swedish Primary Care Cardiovascular Database (SPCCD): 74 751 hypertensive primary care patients. Blood Pressure. In press
Kristianson KJ, Ljunggren H, Gustafsson LL (2009) Data extraction from a semi-structured electronic medical record system for outpatients: a model to facilitate the access and use of data for quality control and research. Health Informatics J 15(4):305–319. doi:10.1177/1460458209345889
Hjerpe P, Merlo J, Ohlsson H, Bengtsson Boström K, Lindblad U (2010) Validity of registration of ICD codes and prescriptions in a research database in Swedish primary care: a cross-sectional study in Skaraborg primary care database. BMC Med Inform Decis Mak 10:23. doi:10.1186/1472-6947-10-23
Ludvigsson JF, Otterblad-Olausson P, Pettersson BU, Ekbom A (2009) The Swedish personal identity number: possibilities and pitfalls in healthcare and medical research. Eur J Epidemiol 24(11):659–667. doi:10.1007/s10654-009-9350-y
Wettermark B, Hammar N, Fored CM, Leimanis A, Otterblad Olausson P, Bergman U, Persson I, Sundström A, Westerholm B, Rosén M (2007) The new Swedish Prescribed Drug Register–opportunities for pharmacoepidemiological research and experience from the first six months. Pharmacoepidemiol Drug Saf 16(7):726–735. doi:10.1002/pds.1294
Ludvigsson JF, Andersson E, Ekbom A, Feychting M, Kim JL, Reuterwall C, Heurgren M, Olausson PO (2011) External review and validation of the Swedish national inpatient register. BMC Publ Health 11:450. doi:10.1186/1471-2458-11-450
Johansson LA, Westerling R (2000) Comparing Swedish hospital discharge records with death certificates: implications for mortality statistics. Int J Epidemiol 29(3):495–502
Caetano PA, Lam JM, Morgan SG (2006) Toward a standard definition and measurement of persistence with drug therapy: Examples from research on statin and antihypertensive utilization. Clin Ther 28(9):1411–1424. doi:10.1016/j.clinthera.2006.09.021, discussion 1410
Saleh SS, Szebenyi S, Carter JA, Zacher C, Belletti D (2008) Patterns and associated health services costs of antihypertensive drug modifications. J Clin Hypertens (Greenwich) 10(1):43–50
Erkens JA, Panneman MM, Klungel OH, van den Boom G, Prescott MF, Herings RM (2005) Differences in antihypertensive drug persistence associated with drug class and gender: a PHARMO study. Pharmacoepidemiol Drug Saf 14(11):795–803. doi:10.1002/pds.1156
Sagie A, Larson MG, Levy D (1993) The natural history of borderline isolated systolic hypertension. N Engl J Med 329(26):1912–1917. doi:10.1056/NEJM199312233292602
Soldin OP, Mattison DR (2009) Sex differences in pharmacokinetics and pharmacodynamics. Clin Pharmacokinet 48(3):143–157. doi:10.2165/00003088-200948030-00001
Vinker S, Alkalay A, Hoffman RD, Elhayany A, Kaiserman I, Kitai E (2008) Long-term adherence to antihypertensive therapy: a survey in four primary care clinics. Expert Opin Pharmacother 9(8):1271–1277. doi:10.1517/14656566.9.8.1271
Hoer A, Gothe H, Khan ZM, Schiffhorst G, Vincze G, Haussler B (2007) Persistence and adherence with antihypertensive drug therapy in a German sickness fund population. J Hum Hypertens 21(9):744–746. doi:10.1038/sj.jhh.1002223
Lewington S, Clarke R, Qizilbash N, Peto R, Collins R (9349) Age-specific relevance of usual blood pressure to vascular mortality: a meta-analysis of individual data for one million adults in 61 prospective studies. Lancet 360:1903–1913
Briesacher BA, Limcangco MR, Frech-Tamas F (2007) New-user persistence with antihypertensives and prescription drug cost-sharing. J Clin Hypertens (Greenwich) 9(11):831–836
Wettermark B, Godman B, Neovius M, Hedberg N, Mellgren TO, Kahan T (2010) Initial effects of a reimbursement restriction to improve the cost-effectiveness of antihypertensive treatment. Health Policy 94(3):221–229. doi:10.1016/j.healthpol.2009.09.014
Krueger KP, Berger BA, Felkey B (2005) Medication adherence and persistence: a comprehensive review. Adv Ther 22(4):313–356
Helman CG (2000) Culture, health and illness. Butterworth Heineman, Oxford
Carlsson AC, Wändell PE, de Faire U, Hellenius ML (2008) Prevalence of hypertension in immigrants and Swedish-born individuals, a cross-sectional study of 60-year-old men and women in Sweden. J Hypertens 26(12):2295–2302. doi:10.1097/HJH.0b013e32831391c3
Melloni C, Alexander KP, Ou FS, LaPointe NM, Roe MT, Newby LK, Baloch K, Ho PM, Rumsfeld JS, Peterson ED (2009) Predictors of early discontinuation of evidence-based medicine after acute coronary syndrome. Am J Cardiol 104(2):175–181. doi:10.1016/j.amjcard.2009.03.013
Ekedahl A, Månsson N (2004) Unclaimed prescriptions after automated prescription transmittals to pharmacies. Pharm World Sci 26(1):26–31
Ax F, Ekedahl A (2010) Electronically transmitted prescriptions not picked up at pharmacies in Sweden. Res Social Adm Pharm 6(1):70–77. doi:10.1016/j.sapharm.2009.06.003
Fischer MA, Stedman MR, Lii J, Vogeli C, Shrank WH, Brookhart MA, Weissman JS (2010) Primary medication non-adherence: analysis of 195,930 electronic prescriptions. J Gen Intern Med 25(4):284–290. doi:10.1007/s11606-010-1253-9
Fischer MA, Choudhry NK, Brill G, Avorn J, Schneeweiss S, Hutchins D, Liberman JN, Brennan TA, Shrank WH (2011) Trouble getting started: predictors of primary medication nonadherence. Am J Med 124(11):1081. doi:10.1016/j.amjmed.2011.05.028, e1089-1022
Sörensen HT, Sabroe S, Olsen J (1996) A framework for evaluation of secondary data sources for epidemiological research. Int J Epidemiol 25(2):435–442
Van Wijk BL, Klungel OH, Heerdink ER, de Boer A (2006) Refill persistence with chronic medication assessed from a pharmacy database was influenced by method of calculation. J Clin Epidemiol 59(1):11–17. doi:10.1016/j.jclinepi.2005.05.005
Acknowledgments
This study was funded by the Swedish Heart Lung Foundation, the Drug and Therapeutics Committee of Stockholm County Council, Karolinska Institutet, the Health & Medical Care Committee of the Regional Executive Board of the Region Västra Götaland, and the Skaraborg Research and Development Council. The SPCCD is endorsed by the Swedish Society of Hypertension, Stroke, and Vascular Medicine.
Declaration of interest
All authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Qvarnström, M., Kahan, T., Kieler, H. et al. Persistence to antihypertensive drug treatment in Swedish primary healthcare. Eur J Clin Pharmacol 69, 1955–1964 (2013). https://doi.org/10.1007/s00228-013-1555-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-013-1555-z