Abstract
Objective
Effective treatment of hypertension requires continued prescribing of antihypertensive medications for many years. Persistence in prescribing habits, however, has been reported to be low. The study described herein – which is completely independent of pharmaceutical sponsors – was undertaken to evaluate persistence with antihypertensive treatment in Germany.
Methods
A total of 13,763 newly diagnosed hypertensive patients were identified in the IMS Disease Analyzer database and observed for 3 years after their first antihypertensive prescription.
Results
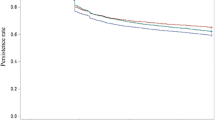
The median age of the study cohort was 65 years, and 56% were female. One in four patient received no more than three prescriptions within 3 years. Persistence was longest for patients whose initial prescription was for a free combination based on angiotensin converting enzyme inhibitors (median: 392.5 days), followed patients initially receiving a fixed combination, including angiotensin II receptor antagonists (208.5 days) and AIIRA monotherapy (168 days). Persistence was shortest with diuretics (57 days). Across all treatment groups, persistence after 3 years was 15.2%. Insurance status, sex and comorbidities were not found to impact persistence.
Conclusion
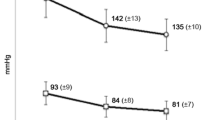
Our data indicate that persistence differs markedly among the drug classes (p ≤ 0.001) but that even persistence of the best drug class is not sufficient to provide for an adequate blood pressure control in the population. The largest decline in persistence occurred in the first 3 months of treatment. More research is needed to elucidate the causes of this early drop in persistence and to develop effective means of improving the currently unsatisfactory situation.
Similar content being viewed by others
References
Cooper RS, Wolf-Maier K, Luke A, Adeyemo A, Banegas JR, Forrester T et al. (2005) An international comparative study of blood pressure in populations of European vs. African descent. BMC Med 3:2
Wolf-Maier K, Cooper RS, Banegas JR, Giampaoli S, Hense HW, Joffres M et al. (2003) Hypertension prevalence and blood pressure levels in 6 European countries, Canada and the United States. JAMA 289:2363–2369
Pittrow D, Kirch W, Bramlage P, Lehnert H, Hofler M, Unger T et al. (2004) Patterns of antihypertensive drug utilization in primary care. Eur J Clin Pharmacol 60:135–142
Neutel JM, Smith DH (2003) Improving patient compliance: a major goal in the management of hypertension. J Clin Hypertens 5:127–132
Elliott WJ (2003) Compliance – and improving it – in hypertension. Manag Care [8 Suppl Hypertension]:56–61
Werlemann BC, Offers E, Kolloch R (2004) Compliance problems in therapy resistant hypertension. Herz 29:271–275
Wetzels GE, Nelemans P, Schouten JS, Prins MH (2004) Facts and fiction of poor compliance as a cause of inadequate blood pressure control: a systematic review. J Hypertens 22:1849–1855
Osterberg L, Blaschke T (2005) Adherence to medication. N Engl J Med 353:487–497
Dezii CM (2001) Persistence with drug therapy: a practical approach using administrative claims data. Manage Care 10:42–45
Jones JK, Gorkin L, Lian JF, Staffa JA, Fletcher AP (1995) Discontinuation of and changes in treatment after start of new course of antihypertensive drugs: a study of a United Kingdom population. Br Med J 311:293–295
Hasford J, Mimran A, Simons WR (2002) A population-based European cohort study of persistence in newly diagnosed hypertensive patients. J Hum Hypertens 16:569–575
Dietlein G, Schröder-Bernhardi D (2002) Use of the Mediplus patient database in healthcare research. Int J Clin Pharmacol Ther 40:30–33
www.ephmra.org/pdf/ATCGuidelines2006%20revised.pdf (last access: June 4, 2007)
Poluzzi E, Strahinja P, Vargiu A, Chiabrando G, Silvani MC, Motola D et al. (2005) Initial treatment of hypertension and adherence to therapy in general practice in Italy. Eur J Clin Pharmacol 61:603–609
Dezii CM (2000) A retrospective study of persistence with single-pill combination therapy vs concurrent two-pill therapy in patients with hypertension. Manag Care 9[Suppl]:2–6
Erkens JA, Panneman MM, Klungel OH, van den Boom G, Prescott MF, Herings RM (2005) Differences in antihypertensive drug persistence associated with drug class and gender: a PHARMO study. Pharmacoepidemiol Drug Safe 14:745–803
Caro JJ, Speckman JL, Salas M, Raggio G, Jackson JD (1999) Effect of initial drug choice on persistence with antihypertensive therapy: the importance of actual practice data. Can Med Assoc J 160:41–46
Morgan SG, Yan L (2004) Persistence with hypertension treatment among community-dwelling BC seniors. Can J Clin Pharmacol 11:e267–e273
Mazzaglia G, Mantovani LG, Sturkenboom MC, Filippi A, Trifiro G, Cricelli C et al. (2005) Patterns of persistence with antihypertensive medications in newly diagnosed hypertensive patients in Italy: a retrospective cohort study in primary care. J Hypertens 11:2093–2100
Perreault S, Lamarre D, Blais L, Dragomir A, Berbiche D, Lalonde L et al. (2005) Persistence with treatment in newly treated middle-aged patients with essential hypertension. Ann Pharmacother 39:1401–1408
Anonymous (2005) After the diagnosis: adherence and persistence with hypertension treatment. Am J Manage Care 11:S395–S399
Wallenius SH, Vainio KK, Korhonen MJ, Hartzema AG, Enlund HK (1995) Self-initiated modification of hypertension treatment in response to perceived problems. Ann Pharmacother 29:1213–1217
The ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group (2002) Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs. diuretics. The Antihypertensive and Lipid-Lowering Treatment to prevent Heart Attack Trial (ALLHAT). JAMA 288:2981–2997
Van Wijk BL, Klungel OH, Heerdink ER, de Boer A (2006) Refill persistence with chronic medication assessed from a pharmacy database was influenced by method of calculation. J Clin Epidemiol 59:11–17
Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (1997) The sixth report of the Joint National Committee on prevention, detection, evaluation, and treatment of high blood pressure. Arch Intern Med 157:2413–2446
Krousel-Wood M, Hyre A, Muntner P, Morisky D (2005) Methods to improve medication adherence in patients with hypertension: current status and future directions. Curr Opin Cardiol 20:296–300
Schroeder K, Fahey T, Ebrahim S (2004) Interventions for improving adherence to treatment in patients with high blood pressure in ambulatory settings. Cochrane Database Syst Rev 2:CD004804
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hasford, J., Schröder-Bernhardi, D., Rottenkolber, M. et al. Persistence with antihypertensive treatments: results of a 3-year follow-up cohort study. Eur J Clin Pharmacol 63, 1055–1061 (2007). https://doi.org/10.1007/s00228-007-0340-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-007-0340-2