Abstract
An analytical method using 2D high-performance liquid chromatography followed by tandem mass spectrometry for the quantification of the beta-lactam antibiotics amoxicillin, flucloxacillin, piperacillin, benzylpenicillin, the beta-lactamase inhibitors clavulanic acid, and tazobactam, as well as the macrolide antibiotic clindamycin, is presented. All analytes were measured in human plasma, while amoxicillin, clavulanic acid, flucloxacillin, and clindamycin were also analyzed in human tissue samples. Because of its high-protein binding, additionally, the free fraction of flucloxacillin was measured after ultrafiltration. As internal standards, deuterated forms of the beta-lactams were used. Sample preparation for all matrices was protein precipitation followed by online extraction on a TurboFlow MAX column, while sample separation was performed on an Accucore XL C18 column. Calibration curves were linear over 0.2–25 mg/kg for the tissue samples and 0.05–20 mg/l for the free fraction of flucloxacillin. In plasma, the calibration curves for amoxicillin and piperacillin were linear over 3.125–125 mg/l, for clavulanic acid and tazobactam over 1–40 mg/l, for benzylpenicillin 0.25–40 mg/l, and for flucloxacillin and clindamycin over 1.5–60 mg/l and 0.05–8 mg/l respectively. In plasma and plasma ultrafiltrate, inaccuracy and imprecision for any analyte were always less than 15%. In tissue, the accuracy and precision varied up to 16%, respectively, 20%, when various tissues were analyzed using a calibration in water.

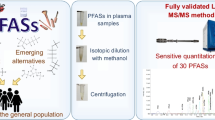
Graphical abstract





Similar content being viewed by others
References
Muller AE, Huttner B, Huttner A. Therapeutic drug monitoring of beta-lactams and other antibiotics in the intensive care unit: which agents, which patients and which infections? Drugs. 2018;78(4):439–51. https://doi.org/10.1007/s40265-018-0880-z .
Huttner A, Harbarth S, Hope WW, Lipman J, Roberts JA. Therapeutic drug monitoring of the β-lactam antibiotics: what is the evidence and which patients should we be using it for? J Antimicrob Chemother. 2015;70(12):3178–83. https://doi.org/10.1093/jac/dkv201 .
Dalhoff A. Seventy-five years of research on protein binding. Antimicrob Agents Chemother. 2018;62(2):1663–17. https://doi.org/10.1128/AAC.01663-17 .
Sutherland R, Croydon EA, Rolinson GN. Flucloxacillin, a new isoxazolyl penicillin, compared with oxacillin, cloxacillin, and dicloxacillin. Br Med J. 1970;4(5733):455–60. https://doi.org/10.1136/bmj.4.5733.455 .
Røder BL, Frimodt-Møller N, Espersen F, Rasmussen SN. Dicloxacillin and flucloxacillin: pharmacokinetics, protein binding and serum bactericidal titers in healthy subjects after oral administration. Infection. 1995;23(2):107–12. https://doi.org/10.1007/BF01833876 .
Gordon RC, Regamey C, Kirby WM. Serum protein binding of erythromycin, lincomycin, and clindamycin. J Pharm Sci. 1973;62(7):1074–7. https://doi.org/10.1002/jps.2600620704 .
Ulldemolins M, Roberts JA, Wallis SC, Rello J, Lipman J. Flucloxacillin dosing in critically ill patients with hypoalbuminaemia: special emphasis on unbound pharmacokinetics. J Antimicrob Chemother. 2010;65(8):1771–8. https://doi.org/10.1093/jac/dkq184 .
Theuretzbacher U. Tissue penetration of antibacterial agents: how should this be incorporated into pharmacodynamic analyses? Curr Opin Pharmacol. 2007;7(5):498–504. https://doi.org/10.1016/j.coph.2007.05.003 .
Pardridge WM. Drug transport across the blood-brain barrier. J Cereb Blood Flow Metab. 2012;32(11):1959–72. https://doi.org/10.1038/jcbfm.2012.126 .
Li X, Zhang Z, Chang X, Wang X, Hu J, Lin Q, et al. Disruption of blood-brain barrier by an Escherichia coli isolated from canine septicemia and meningoencephalitis. Comp Immunol Microbiol Infect Dis. 2019;63:44–50. https://doi.org/10.1016/j.cimid.2019.01.002 .
Varatharaj A, Galea I. The blood-brain barrier in systemic inflammation. Brain Behav Immun. 2017;60:1–12. https://doi.org/10.1016/j.bbi.2016.03.010 .
Dando SJ, Mackay-Sim A, Norton R, Currie BJ, St John JA, Ekberg JAK, et al. Pathogens penetrating the central nervous system: infection pathways and the cellular and molecular mechanisms of invasion. Clin Microbiol Rev. 2014;27(4):691–726. https://doi.org/10.1128/CMR.00118-13 .
Dong X, Ding L, Cao X, Jiang L, Zhong S. A sensitive LC-MS/MS method for the simultaneous determination of amoxicillin and ambroxol in human plasma with segmental monitoring. Biomed Chromatogr. 2013;27(4):520–6. https://doi.org/10.1002/bmc.2824 .
Abdulla A, Bahmany S, Wijma RA, van der Nagel BCH, Koch BCP. Simultaneous determination of nine β-lactam antibiotics in human plasma by an ultrafast hydrophilic-interaction chromatography-tandem mass spectrometry. J Chromatogr B. 2017;1060:138–43. https://doi.org/10.1016/j.jchromb.2017.06.014 .
Carlier M, Stove V, de Waele JJ, Verstraete AG. Ultrafast quantification of β-lactam antibiotics in human plasma using UPLC–MS/MS. J Chromatogr B. 2015;978-979:89–94. https://doi.org/10.1016/j.jchromb.2014.11.034 .
Zander J, Döbbeler G, Nagel D, Maier B, Scharf C, Huseyn-Zada M, et al. Piperacillin concentration in relation to therapeutic range in critically ill patients - a prospective observational study. Crit Care. 2016;20(1):79. https://doi.org/10.1186/s13054-016-1255-z .
Di Rocco M, Moloney M, O'Beirne T, Earley S, Berendsen B, Furey A, et al. Development and validation of a quantitative confirmatory method for 30 β-lactam antibiotics in bovine muscle using liquid chromatography coupled to tandem mass spectrometry. J Chromatogr A. 2017;1500:121–35. https://doi.org/10.1016/j.chroma.2017.04.022 .
Lugoboni B, Gazzotti T, Zironi E, Barbarossa A, Pagliuca G. Development and validation of a liquid chromatography/tandem mass spectrometry method for quantitative determination of amoxicillin in bovine muscle. J Chromatogr B Analyt Technol Biomed Life Sci. 2011;879(21):1980–6. https://doi.org/10.1016/j.jchromb.2011.05.038 .
Reyns T, Cherlet M, de Baere S, de Backer P, Croubels S. Rapid method for the quantification of amoxicillin and its major metabolites in pig tissues by liquid chromatography-tandem mass spectrometry with emphasis on stability issues. J Chromatogr B Analyt Technol Biomed Life Sci. 2008;861(1):108–16. https://doi.org/10.1016/j.jchromb.2007.11.007 .
Torkington MS, Davison MJ, Wheelwright EF, Jenkins PJ, Anthony I, Lovering AM, et al. Bone penetration of intravenous flucloxacillin and gentamicin as antibiotic prophylaxis during total hip and knee arthroplasty. Bone Joint J. 2017;99-B(3):358–64. https://doi.org/10.1302/0301-620X.99B3.BJJ-2016-0328.R1 .
Martin C, Mallet MN, Sastre B, Viviand X, Martin A, de Micco P, et al. Comparison of concentrations of two doses of clavulanic acid (200 and 400 milligrams) administered with amoxicillin (2,000 milligrams) in tissues of patients undergoing colorectal surgery. Antimicrob Agents Chemother. 1995;39(1):94–8. https://doi.org/10.1128/aac.39.1.94 .
Cross SE, Thompson MJ, Roberts MS. Distribution of systemically administered ampicillin, benzylpenicillin, and flucloxacillin in excisional wounds in diabetic and normal rats and effects of local topical vasodilator treatment. Antimicrob Agents Chemother. 1996;40(7):1703–10. https://doi.org/10.1128/AAC.40.7.1703 .
Gibson MJ, Karpinski MR, Slack RC, Cowlishaw WA, Webb JK. The penetration of antibiotics into the normal intervertebral disc. J Bone Joint Surg Br. 1987;69(5):784–6.
Frank U, Schmidt-Eisenlohr E, Schlosser V, Spillner G, Schindler M, Daschner FD. Concentrations of flucloxacillin in heart valves and subcutaneous and muscle tissues of patients undergoing open-heart surgery. Antimicrob Agents Chemother. 1988;32(6):930–1. https://doi.org/10.1128/aac.32.6.930 .
Averono G, Vidali M, Olina M, Basile M, Bagnati M, Bellomo G, et al. Evaluation of amoxicillin plasma and tissue levels in pediatric patients undergoing tonsillectomy. Int J Pediatr Otorhinolaryngol. 2010;74(9):995–8. https://doi.org/10.1016/j.ijporl.2010.05.023 .
Cazorla-Reyes R, Romero-González R, Frenich AG, Rodríguez Maresca MA, Martínez Vidal JL. Simultaneous analysis of antibiotics in biological samples by ultra high performance liquid chromatography-tandem mass spectrometry. J Pharm Biomed Anal. 2014;89:203–12. https://doi.org/10.1016/j.jpba.2013.11.004 .
Barré J, Chamouard JM, Houin G, Tillement JP. Equilibrium dialysis, ultrafiltration, and ultracentrifugation compared for determining the plasma-protein-binding characteristics of valproic acid. Clin Chem. 1985;31(1):60–4.
Wong G, Brinkman A, Benefield RJ, Carlier M, de Waele JJ, El Helali N, et al. An international, multicentre survey of β-lactam antibiotic therapeutic drug monitoring practice in intensive care units. J Antimicrob Chemother. 2014;69(5):1416–23. https://doi.org/10.1093/jac/dkt523 .
Kratzer A, Liebchen U, Schleibinger M, Kees MG, Kees F. Determination of free vancomycin, ceftriaxone, cefazolin and ertapenem in plasma by ultrafiltration: impact of experimental conditions. J Chromatogr B. 2014;961:97–102. https://doi.org/10.1016/j.jchromb.2014.05.021 .
Wong G, Briscoe S, McWhinney B, Ally M, Ungerer J, Lipman J, et al. Therapeutic drug monitoring of β-lactam antibiotics in the critically ill: direct measurement of unbound drug concentrations to achieve appropriate drug exposures. J Antimicrob Chemother. 2018;73(11):3087–94. https://doi.org/10.1093/jac/dky314 .
Zeitlinger MA, Derendorf H, Mouton JW, Cars O, Craig WA, Andes D, et al. Protein binding: do we ever learn? Antimicrob Agents Chemother. 2011;55(7):3067–74. https://doi.org/10.1128/AAC.01433-10 .
Kawakami A, Kubota K, Yamada N, Tagami U, Takehana K, Sonaka I, et al. Identification and characterization of oxidized human serum albumin. A slight structural change impairs its ligand-binding and antioxidant functions. FEBS J. 2006;273(14):3346–57. https://doi.org/10.1111/j.1742-4658.2006.05341.x .
Fournier T, Medjoubi-N N, Porquet D. Alpha-1-acid glycoprotein. Biochim Biophys Acta. 2000;1482(1–2):157–71. https://doi.org/10.1016/s0167-4838(00)00153-9 .
Liebchen U, Kratzer A, Wicha SG, Kees F, Kloft C, Kees MG. Unbound fraction of ertapenem in intensive care unit patients. J Antimicrob Chemother. 2014;69(11):3108–11. https://doi.org/10.1093/jac/dku226 .
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The analyzed authentic samples belonged to individuals who provided an informed consent for their use and all analyses were carried out according to the ethical standards of the University Hospital Basel.
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rehm, S., Rentsch, K.M. A 2D HPLC-MS/MS method for several antibiotics in blood plasma, plasma water, and diverse tissue samples. Anal Bioanal Chem 412, 715–725 (2020). https://doi.org/10.1007/s00216-019-02285-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00216-019-02285-0