Abstract
H2S-donors are cardioprotective in ischemia/reperfusion (I/R) injury. Some H2S-donors exert their beneficial effects in a nitric oxide (NO)-dependent manner, while others act using NO-independent pathways. The aims of the present study were to (i) evaluate whether H2S-donors with distinct pharmacodynamic properties act synergistically in I/R injury and (ii) determine if H2S-donors remain cardioprotective in obese mice. C57BL/6 mice were subjected to 30 min of ischemia followed by 120 min of reperfusion. Donors were administered intravenously at the end of ischemia (Na2S: 1 μmol/kg, GYY4137: 25 μmol/kg, AP39: 0,25 μmol/kg), while the 3-mercaptopyruvate sulfurtransferase (10 mg/kg) inhibitor was given intraperitonially 1 h prior to ischemia. Infarct size was estimated by 2,3,5-triphenyltetrazolium staining, while the area at risk was calculated using Evans blue. All three donors reduced infarct size when administered as a sole treatment. Co-administration of Na2S/GYY4137, as well as Na2S/AP39 reduced further the I/R injury, beyond what was observed with each individual donor. Since inhibition of the H2S-producing enzyme 3-mercaptopyruvate sulfurtransferase is known to reduce infarct size, we co-administered C3 with Na2S to determine possible additive effects between the two agents. In this case, combination of C3 with Na2S did not yield superior results compared to the individual treatments. Similarly, to what was observed in healthy mice, administration of a H2S-donor (Na2S or AP39) reduced I/R injury in mice rendered obese by consumption of a high fat diet. We conclude that combining a NO-dependent with a NO-independent H2S-donor leads to enhanced cardioprotection and that H2S-donors remain effective in obese animals.
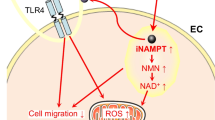
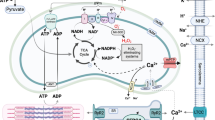
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Acute myocardial infarction (AMI) is a leading cause of morbidity and mortality worldwide (Timmis et al. 2022; Vos et al. 2012). Although advances in the treatment of AMI have translated into a considerable decline in mortality rates, heart failure (HF) remains a common complication of AMI, with an estimated incidence varying from 10 to 40% (Weir et al. 2006). The injury that the myocardium undergoes during ΑΜΙ, is due to both the ischemia and the subsequent therapeutic reperfusion. Reperfusion although beneficial, can itself induce myocardial damage and death (Yellon and Hausenloy 2007). Ischemia/reperfusion (I/R) injury is a complex process involving a multitude of triggers, mediators and effectors, each contributing to the final myocardial injury (Hausenloy and Yellon 2013; Heusch 2015). Ongoing research aims at discovering pharmacologic agents that when administered immediately prior to or at reperfusion, will be able to reduce myocardial infarct size.
H2S is a colorless, water-soluble, flammable gas with a characteristic unpleasant "rotten egg" odor. Until the 90s, it was studied exclusively for its toxic properties, but is now recognized as an important endogenous mediator (Cirino et al. 2023; Kimura 2014). Although H2S can be produced non-enzymatically, it is mainly generated through the action of three enzymes; cystathionine γ-lyase, cystathionine β-synthase and 3-mercaptopyruvate sulfurtransferase (Cirino et al. 2023; Filipovic et al. 2018; Wallace and Wang 2015). In the cardiovascular system, many studies have proven that H2S exerts beneficial/protective effects reducing blood pressure, promoting vasodilation, attenuating atherosclerosis and limiting endothelial dysfunction (Bibli et al. 2019; Coletta et al. 2012; Kanagy et al. 2017; Mani et al. 2013; Wang 2023; Wang et al. 2015; Yang and Wang 2015). In addition, H2S exerts antioxidant effects and stimulates angiogenesis (Filipovic et al. 2018; Kolluru et al. 2023; Papapetropoulos et al. 2009). Elrod et al., were the first to report on the cardioprotective effects of H2S in vivo; in a mouse I/R injury model, H2S limited oxidative stress and reduced infarct size (Elrod et al. 2007; Zhang et al. 2007). Many studies from several laboratories using H2S donors have confirmed and extended the finding that exogenously supplied H2S ameliorates I/R injury and reduces infarct size in rodents, pigs and dogs (Karwi et al. 2017a).
Several disease states are characterized by reduced levels of endogenous H2S (Cirino et al. 2023). For example, low H2S levels have been documented in heart failure, hypertension, atherosclerosis, diabetes and obesity. To effectively deliver H2S and replenish H2S levels, a variety of donors have been synthesized in recent years (Levinn et al. 2020; Szabo and Papapetropoulos 2017; Wallace and Wang 2015; Xu et al. 2019; Zheng et al. 2015). These donors differ in their pharmacokinetic profiles, the mechanism and the rate by which they release H2S. One distinct group of H2S donors that is widely used in the literature includes the sodium salts, sodium sulfide (Na2S) and sodium hydrosulfide (NaHS). These agents do not actually release H2S, but dissociate spontaneously to yield S−2 or HS− and produce H2S in a pH-dependent manner (Papapetropoulos et al. 2015). Their administration causes an initial rapid increase in H2S levels, which then decreases with an equally rapid speed (Kashfi and Olson 2013). A second distinct group of H2S donors includes slowly releasing donors that were designed to mimic the endogenous rate of release of H2S; GYY4137 (morpholin-4-ium 4-methoxyphenyl (morpholino) phosphinodithioate) is the first in class of this compounds (Li et al. 2008). In addition, AP39 (10-oxo-10-(4-(3-thioxo-3H-1,2-dithiol5yl)-phenoxy)decyl triphenylphosphonium bromide belongs to the mitochondrial-targeted class of donors; its triphenylphosphonium group allows it to gain access to the mitochondrial compartment, while its dithiolethione group releases H2S slowly (Szczesny et al. 2014).
Several mechanisms have been implicated in the cardioprotective actions of H2S donors, including SAFE, RISK and the NO/cGMP pathways, antioxidant and anti-inflammatory effects, as well as mitochondria-related processes (Donnarumma et al. 2017; Li et al. 2018). Our group has previously compared the cardioprotective mechanisms employed by the fast donor Na2S, the slowly releasing H2S donors GYY4137 and thiovaline, and the mitochondrial-targeted donor AP39. We observed that although all of the donors reduced infarct size to a similar extent, only the effect of Na2S was eNOS-dependent (Chatzianastasiou et al. 2016). Thiovaline, GYY4137 and AP39 acted independently of the NO/cGMP pathway.
The aim of the present study was to investigate whether co-administration of H2S donors with distinct mechanisms of action, Na2S, GYY4137 and AP39, shows additive effects, leading to an increased cardioprotective effect. As almost all studies so far with H2S donors in I/R injury have been done in healthy animals, we also tested the ability of H2S donors with different mechanisms of action to limit myocardial injury after ischemia/reperfusion in mice with comorbidities using obese mice.
Materials and methods
Reagents
Sodium GYY4137 and AP39 were synthesized as previously described (Le Trionnaire et al. 2014; Alexander et al. 2015). Compound 3 (2-[(4-hydroxy-6-methylpyrimidin-2-yl)sulfanyl]-1-(naphthalen-1-yl)ethan-1-one), abbreviated as C3 was purchased from MolPort (Riga, Latvia). Na2S, TTC (2,3,5- triphenyltetrazolium chloride), Evans Blue Dye (tetrasodium (6E,6'E)-6,6-[(3,3'-dimethylbiphenyl-4,4'-diyl)di(1E)hydrazin-2-yl-1-ylidene]bis(4-amino-5-oxo-5,6-dihydronaphthalene-1,3-disulfonate)) were purchased from Sigma-Aldrich Chemie GmbH (Taufkirchen, Germany). HFD (E15744-34) and CD (E157452) were purchased from Ssniff (ssniff-Spezialdiäten GmbH, Germany).
Animals
All animals used for experiments were bred/housed in individual cages under specific pathogen-free, temperature controlled (20–25 °C) and 12-h light/dark cycle conditions in full compliance with the guidelines of the Federation of Laboratory Animal Science Association recommendations in the Laboratory Animal Unit of the Hospital “Evangelismos” and allowed free access to diets and water. All studies were performed on male 8- to 16-week-old C57BL/6 J mice which were purchased from Alexander Fleming Institute (Athens, Greece). Mice were randomly assigned to diet or intervention groups. All animal procedures were in compliance with the European Community guidelines for the use of experimental animals; experimental protocols and all experimental procedures reported here were approved by the veterinary authority of the Prefecture of Athens, in accordance with the national Registration (Presidential Decree 56/2013) in harmony with the European Directive 63/2010.
To induce obesity, mice were fed for 10 weeks with a high fat diet (HFD) containing 45% calories from fat, 20% calories from protein, and 35% calories from carbohydrates. Control diet (CD) containing 10% calories from fat, 20% calories from protein and 70% calories from carbohydrates was used as the control diet. In all other experimental procedures, mice were fed a normal-fat regular diet (4RF22; Mucedola).
Ischemia–reperfusion injury model in vivo
Male mice (8–12 weeks old in the normal diet groups and 18–22 weeks old for the HFD/CD mice) were randomly divided into groups and anesthetized by intraperitoneal injection with a combination of ketamine and xylazine (0.01 mL/g, final concentrations of ketamine, xylazine 10 mg/mL and 2 mg/mL, respectively). Anesthetic depth was evaluated by the loss of pedal reflex to toe-pinch stimulus and breathing rate. A tracheotomy was performed for artificial respiration at 120–150 breaths/min and a volume of 0,2 mL. A thoracotomy was then performed between the fourth and fifth rib and the pericardium was carefully retracted to visualize the left anterior descending (LAD) coronary, which was ligated using a 6–0 silk suture (W888; Ethicon) placed 3 mm below the tip of the left atrium with the help of 5 mm piece of a 1 mm diameter catheter tube. The heart was allowed to stabilize for 20 min prior to ligation to induce ischemia. After the ischemic period, the ligature was released and allowed reperfusion of the myocardium. Throughout experiments, body temperature was maintained at 37 ± 0.5 °C by way of a heating pad and monitored via a thermocouple inserted rectally. After reperfusion hearts were rapidly excised from mice and directly cannulated and washed with normal saline for blood removal. Hearts were perfused with 400 μl 1% Evans blue, diluted in normal saline. Hearts were kept at -80 °C for 1 h and then sliced in 2 mm sections parallel to the atrioventricular groove. The slices were incubated in 2 mL of 1% TTC phosphate buffer (PBS pH = 7,4) at 37 °C for 15 min and then fixed in 10% formaldehyde overnight. Slices were then compressed between glass plates 1 mm apart and photographed with a Cannon Powershot A620 Digital Camera through a Zeiss 459300 microscope and measured with the NIH ImageJ. Measurements were performed in a blinded fashion. The myocardial area at risk as well as the infarcted and the total area were automatically transformed into volumes. Infarct and risk area volumes were expressed in cm3 and the percentage of infarct-to-risk area ratio (%I/AAR) and of area at risk to whole myocardial area (% AAR/All) were calculated.
Experimental protocol
Wild-type (WT) C57BL/6 J male mice were subjected to 30 min regional ischemia of the myocardium followed by 2 h of reperfusion with the following interventions. Control group (n = 10); Na2S group (n = 8): Na2S was administered as an IV bolus dose of 1 μmol/kg at the 20th min of ischemia; GYY-4137 group (n = 7): GYY-4137 was administered as an IV bolus dose of 25 μmol/kg at the 20th min of ischemia; AP39 group (n = 9): AP39 was administered as an IV bolus dose of 250 nmol/kg at the 20th min of ischemia; C3 group (n = 8): C3 was administered intraperitoneally at a dose of 10 mg/kg 1 h before ischemia; Na2S-AP39 (n = 8): AP39 was administered as an IV bolus dose of 250 nmol/kg at the 15th min of ischemia and Na2S was administered as an IV bolus dose of 1 μmol/kg at the 20th min of ischemia; Na2S-GYY-4137 (n = 7) group: GYY-4137 was administered as an IV bolus dose of 25 μmol/kg at the 15th min of ischemia and Na2S was administered as an IV bolus dose of 1 μmol/kg at the 20th min of ischemia; Na2S-C3 group (n = 7): C3 was administered intraperitoneally at a dose of 10 mg/kg 1 h before ischemia and Na2S was administered as an IV bolus dose of 1 μmol/kg at the 20th min of ischemia; The doses used for each donor were chosen based on the literature, including previous work from our group (Chatzianastasiou et al. 2016; Szabó et al. 2011). Na2S and GYY-4137 were dissolved in water for injection (WPI), while AP39 and C3 were dissolved in dimethylsulfoxide (DMSO). For iv administration, the volume of injection was 50 μl and the final concentration of DMSO was 0.05%. We have previously established that DMSO at this concentration exerts no pharmacological effects on the outcome of I/R injury. For each of the donors, the dose used was the lowest dose that was maximally effective in reducing infarct size that did not affect blood pressure.
For the obesity study, mice were randomly assigned to HFD and CD groups. The weight of the experimental animals was recorded on a weekly basis. Mice were subjected to 30 min regional ischemia of the myocardium followed by 2 h of reperfusion with the following interventions. Control CD group (n = 6); Control HFD group (n = 6); AP39 CD group (n = 6): AP39 was administered as an IV bolus dose of 250 nmol/kg at the 20th min of ischemia; AP39 HFD group (n = 6): AP39 was administered as an IV bolus dose of 250 nmol/kg at the 20th min of ischemia; Na2S CD group (n = 7): Na2S was administered as an IV bolus dose of 1 μmol/kg at the 20th min of ischemia; Na2S HFD group (n = 6): Na2S was administered as an IV bolus dose of 1 μmol/kg at the 20th min of ischemia.
Statistical analysis
Data are expressed as means ± SD. Student’s unpaired two- tailed t test was used for comparison between two groups, and one-way ANOVA was used to compare three or more groups followed by a post hoc test. Sample sizes are reported in the methods section and in the figure captions. P was considered significant when < 0.05. GraphPad Prism 9.0 software was used for statistical analysis.
Results
Na2S-GYY4137 co-administration offers additional protection against ischemia/re-perfusion injury
Similarly to what has been described by us and others, administration of the H2S donor Na2S at the end of the ischemic period, caused a significant reduction in infarct size compared to the control group (Fig. 1A). GYY4137 that has been previously shown to exert a cardioprotective effect that is independent of ΝΟ, also attenuated the infarct size when administered at the end of the ischemic period. This reduction was to a degree that was similar to that observed with Na2S. When GYY4137 was combined with Na2S that exerts its infarct-reducing action in a NO-dependent manner, the observed effect was greater than that observed with Na2S or GYY4137 alone, confirming the existence of two distinct H2S-triggered cardioprotective pathways that can act in an additive fashion. In this series of experiments, the percentage ratios of area at risk to total area (AAR/All%) were also calculated to verify that all groups received the same degree of ischemic occlusion (Fig. 1B). No change in the AAR/All% was observed among groups.
Na2S-GYY4137 coadministration reduces ischemia/reperfusion myocardial injury. A Comparison of the infarct area to area at risk ratio (I/AAR%) between Control, Na2S, GYY4137 and Na2S-GYY4137 groups. Mice were subjected to LAD ligation for 30 min; after removing the ligature, the hearts were reperfused for 2 h and stained as describe in the Methods section to determine the infarcted area and the area at risk. Na2S (1 μmol/kg) or GYY4137 (25 μmol/kg) were given intravenously at the 20th minute of ischemia (10 min prior to reperfusion). For the combination treatment, GYY4137 was given at the 15.th minute of ischemia followed by Na2S 5 min later. Data are presented as means ± SD; n = 7–9 mice/group; *p < 0.05 (B) The ratio area at risk/all of the Control, Na2S, GYY4137 and Na2S-GYY4137 groups was similar (ns p > 0.05)
Co-administration of Na2S and AP39 reduces myocardial injury additively
Infarct size was also reduced following administration of the mitochondrial-targeted H2S donor AP39. Interestingly, co-administration of Na2S and AP39, led to statistically significant cardioprotection over each individual donor. As shown in Fig. 2A, the percentage ratio of infarct to area at risk (I/AAR%) was 13.81 ± 2.13% for the Na2S group and 14.63 ± 2.39% for the AP39 group, while administration of both Na2S and AP39 resulted in enhanced cardioprotection (6.59 ± 1.29%). In this series of experiments, too, the AAR/All% were similar among groups (Fig. 2B).
Na2S-AP39 coadministration diminishes infarct size. A Comparison of the infarct area to area at risk ratio (I/AAR%) between Control, Na2S, AP39 and Na2S-AP39 groups. Mice were subjected to LAD ligation for 30 min; after removing the ligature, the hearts were reperfused for 2 h and stained as describe in the Methods section to determine the infarcted area and the area at risk. Na2S (1 μmol/kg) or AP39 (250 nmol/kg) were given intravenously at the 20th minute of ischemia (10 min prior to reperfusion). For the combination treatment, AP39 was given at the 15th minute of ischemia followed by Na2S 5 min later. Data are presented as means ± SD; n = 8–9 mice/group; *p < 0.05 (B) The ratio area at risk/all of the Control, Na2S, AP39 and Na2S-AP39 groups was similar (ns p > 0.05). Mice in the control and the Na2S groups are the same as in Fig. 1
Combining a H2S donor with 3MST inhibition does not yield additional cardioprotection
We have previously shown that mice lacking 3MST show reduced infarct size following ischemia/reperfusion injury and that pharmacological inhibition of 3MST also results in cardioprotection. In the present series of experiments, we observed that although Na2S and Compound 3 (C3) each reduced infarct size, coadministration of the two agents did not result in further inhibition of the ischemia/reperfusion injury (Fig. 3A). Our results are validated by the finding that the AAR/All% were not different in the groups tested (Fig. 3B).
H2S donation (Na2S) combined with 3-MST inhibition (C3) has no additive effect on the reduction of infarct size. A Comparison of the infarct area to area at risk ratio (I/AAR%) between Control, Na2S, C3 and Na2S-C3 groups. Mice were subjected to LAD ligation for 30 min; after removing the ligature, the hearts were reperfused for 2 h and stained as describe in the methods section to determine the infarcted area and the area at risk. Na2S (1 μmol/kg, iv) or C3 (10 mg/kg, ip) were given as follows. Compound 3 (C3) was given 1 h prior to ischemia and Na2S was given at the 20th minute of ischemia (10 min prior to reperfusion) both for the individual and the combination treatments. Data are presented as means ± SD; n = 7–9 mice/group; *p < 0.05 (B) The ratio area at risk/all of the Control, Na2S, C3 and Na2S-C3 was similar (ns p > 0.05). Mice in the control and the Na2S groups are the same as in Fig. 1
Cardioprotective effect of H2S donors in obese mice
Comorbidities can affect various cell signaling pathways and potentially eliminate the cardioprotective effect of a pharmacological agent (Ferdinandy et al. 2014). Obesity is a risk factor and can be characterized as a comorbidity in patients with AMI (Powell-Wiley et al. 2021).
To test the efficacy of H2S donors in obese mice we used a diet-induced obesity model. As shown in Fig. 4A, the weight of the mice that received a CD increases only slightly over the 10-week period, with an average initial weight of 26.57 ± 2.02 g and an average weight after 10-weeks of 28.03 ± 2.00 g. On the other hand, the weight of the mice fed a HFD increased significantly over the 10-week period (mean starting weight 26.02 ± 2.46 g vs mean weight after 10 weeks 40.83 ± 3.58 g).
H2S donors, Na2S and AP39 are cardioprotective in obese mice. A 6-week-old male WT mice were fed a control diet (CD; 10% calories from fat) or a high fat diet (HFD; 45% calories from fat) for 10 weeks, and body mass was measured weekly. Data are presented as means ± SD; n = 21 mice/group; *p < 0.05 from control diet. B Comparison of the infarct area to area at risk ratio (I/AAR%) between Control, Na2S and AP39 in CD and HFD fed mice. Mice were subjected to LAD ligation for 30 min; after removing the ligature, the hearts were reperfused for 2 h and stained as describe in the methods section to determine the infarcted area and the area at risk. Na2S (1 μmol/kg) or AP39 (250 nmol/kg) were given intravenously at the 20.th minute of ischemia (10 min prior to reperfusion). Data are presented as means ± SD; n = 6–7 mice/group; *p < 0.05. (C) No statistically significant difference of the ratio area at risk/all between Control CD/HFD, Na2S CD/HFD, AP39 CD/HFD groups (ns p > 0.05)
Obese mice suffered increased myocardial injury after ischemia/reperfusion compared to the control CD group (34.55 ± 1.94% vs 45.07 ± 5.70%; Fig. 4B). Administration of Na2S caused a significant reduction in infarct size compared to the control group in both CD and HFD groups. A reduction of similar magnitude was also observed when AP39 was given to obese and normal mice, suggesting that H2S donors retain their cardioprotective efficacy, irrespectively of their mechanism of action (NO-dependent vs NO-independent). The percentage ratios of AAR/All% was similar between the groups studied (Fig. 4C).
Discussion
A variety of H2S donors have been tested and have shown efficacy in preclinical I/R injury models (Karwi et al. 2017a, b; Li et al. 2018; Szabo and Papapetropoulos 2017). In some cases, the donors were administered prior to the ischemic insult, a condition that is not clinically relevant. More often, the H2S donor was given at the end of the ischemic period or at reperfusion to mimic the real-life conditions encountered during medical care of cardiac patients. The donors used that have been proven to be effective in limiting infarct size in animal models include the fast releasing sulfide salts (sodium sulfide and sodium hydrosulfide) (Bibli et al. 2015; Chatzianastasiou et al. 2016; Elrod et al. 2007), the prototype slow-releasing H2S donor GYY4137 (Chatzianastasiou et al. 2016; Karwi et al. 2016), the mitochondrial targeted donor AP39 (Chatzianastasiou et al. 2016; Karwi et al. 2017a, b), the thioaminoacid thiovaline (Chatzianastasiou et al. 2016), the pH-activated H2S donor (Kang et al. 2016), esterase-activated prodrugs (Zheng et al. 2017), thiol-activated compounds (Kang et al. 2016), naturally occurring polysulfide donors (Bradley et al. 2016; Predmore et al. 2012), cysteine-persulfides (Griffiths et al. 2023) and hydro-persulfides (Pharoah et al. 2022). In most of the published studies, although efficacy was demonstrated, the molecular pathways through which the donor exerts its effects was not investigated. Preservation of mitochondrial function and anti-oxidant effects actions have been reported to underlie the acute effects of H2S donors on I/R injury (Donnarumma et al. 2017).
One pathway that has been shown to mediate many of the effects of H2S in the cardiovascular system is the NO/cGMP pathway (Donnarumma et al. 2017; Szabo 2017). Work by others and us, has shown that pharmacological or genetic inhibition of eNOS blocks the infarct reduction brought about by sulfide salts (Bibli et al. 2015; Chatzianastasiou et al. 2016; King et al. 2014). Unlike NaHS and Na2S, we observed that thiovaline, GYY4137 and AP39 inhibited infarct size in a NO-independent manner in mice (Chatzianastasiou et al. 2016). In partial agreement to our findings, Karwi et al. observed that GYY4137 limits infarct size in rats through the PI3K/Akt/GSK-3β pathway, as inhibition of PI3K resulted in complete reversal of the protective effect of GYY4137 (Karwi et al. 2016). However, eNOS inhibition in rats reduced, albeit marginally, the effect of GYY4137 on infarct size, suggesting that NO plays a minor role in GYY4137 cardioprotection in this species. Both our work and that of Karwi et al., confirmed the NO-independent effect of AP39 on infarct size in rats and mice (Chatzianastasiou et al. 2016; Karwi et al. 2017a, b). The cardioprotective effect of AP39 in I/R is also independent of cytosolic kinases. It results from inhibition of mPTP opening through a CypD-independent mechanism, as well as from reduction in mitochondrial ROS production (Chatzianastasiou et al. 2016; Karwi et al. 2017b). Herein, we tested whether using a combination of donors with distinct mechanisms of action (NO-dependent and NO-independent) would provide additive or synergistic effects. Indeed, we have found that co-administration of Na2S and GYY4137 or Na2S and AP39 provides greater cardioprotection than each of the donors when used individually. These results confirm that H2S donors utilizing different signaling pathways to exert their protective effects work additively and provide the rationale for using a combination of donors to secure maximal cardioprotection after I/R.
Endogenously produced H2S has been shown to be essential for cardiovascular homeostasis (Kolluru et al. 2023). Several studies have demonstrated that CSE-derived H2S is important in cardiac physiology and exerts protective actions against heart disease (Cirino et al. 2023; Polhemus and Lefer 2014). Mice overexpressing CSE in cardiomyocytes (Elrod et al. 2007) or in endothelial cells (Xia et al. 2020) exhibit smaller infarcts after I/R, while mice lacking CSE suffer more severe cardiac damage in I/R injury models compared to wild-type animals (King et al. 2014). Similarly, mice with targeted deletion of CSE have significantly greater cardiac enlargement, greater pulmonary edema and left ventricular cavity dilatation and exhibit exacerbated cardiac dysfunction in pressure overload-induced heart failure (Kondo et al. 2013). Unlike what has been observed with CSE knockout mice, mice lacking 3MST are protected from myocardial ischemia (Peleli et al. 2020). Since 3MST KO mice did not benefit from ischemic pre- conditioning, the smaller myocardial damage in 3MST KO was proposed to be due to increased oxidative stress present in 3MST KO hearts, that prepares the myocardium against the I/R injury. Contrary to the findings in the acute I/R injury model, mice lacking 3MST, like CSE KO mice, displayed exacerbated heart failure with reduced ejection fraction phenotype after pressure overload (Li et al. 2022). While trying to unravel the reasons for the differential responses of CSE KO to 3MST in heart disease models, it should be kept in mind that the localization of the two enzymes differs: CSE is present in the cytosol, while 3MST resides in the mitochondria. Based on our previous observations for the protective action of 3MST inhibition in I/R injury, we tested whether blockade of this enzyme combined with simultaneous H2S donation would yield additive or synergistic effects. Our observations that individual treatments reduced infarct size, but co-treatment did not lead to additive effects, indicated that this is not a useful drug combination.
Many of the failures in translating the efficacy of treatments with compounds that reduce infarct size in animal models to humans have been attributed to the fact that humans who suffer an AMI also present with comorbidities and risk factors (Ferdinandy et al. 2023). Other factors have also been proposed to explain the lack of translation of preclinical findings, including reproducibility and rigor of animal experimentation, species differences, as well as the fact that patients with co-morbidities who suffer an AMI are already on medication that modifies cardioprotection, masking the effects of additional agents given at reperfusion (Kleinbongard et al. 2020; Lecour et al. 2021; Lefer and Marbán, 2017).
We, thus, proceeded to evaluate if H2S donors retain their efficacy in reducing infarct size in animals with co-morbidities. To determine if H2S can reduce I/R injury in obese mice, we used both types of donors: one that exerts its effects in a NO-dependent and one that acts independently of NO. Interestingly, obese animals exhibited greater myocardial infarcts compared to control mice. It should be noted that conflicting results for the role of obesity in rodents have been reported, with some studies showing that obesity has a cardioprotective effect (Edland et al. 2016; Inserte et al. 2019; Salie et al. 2014), while others report no difference or increased myocardial injury after ischemia/reperfusion (Guedes et al. 2019; Liu et al. 2014). The discrepancies could be due to strain differences (Inserte et al. 2019) or differences in the diet.
Acute administration of Na2S or AP39 reduced infarct size to the same extent in mice with normal weight and obese mice, suggesting that H2S donors, are also effective in non-healthy mice. Similarly to what we observed with obese mice, acute administration of sulfide salts reduced infarct size in diabetic mice (Lambert et al. 2014). Our predication was that the NO-dependent H2S cardioprotective action of sulfide salts would be attenuated in obese mice, since these animals exhibit endothelial dysfunction, reduced eNOS activity/function and lower NO levels (Lundberg and Weitzberg 2022). Since this was not the case, we conclude that obese mice have enough functionality of their eNOS/NO pathway to mediate the NO-dependent effect of fast releasing H2S donors, or that under conditions of low NO, sulfide salts utilize alternative pathways to exert their cardioprotective effects. It is worth mentioning that long-term administration of H2S donors, also ameliorates cardiac damage in diabetic cardiomyopathy and obesity-induced cardiac dysfunction (Barr et al. 2015; Sun et al. 2021).
In conclusion, we provide evidence that combining H2S donors that use different mechanisms to protect the heart against I/R injury leads to an additive cardioprotective effect (Fig. 5). Moreover, H2S donors are effective in obese animals, providing the rationale for further pre-clinical testing in animals with other diseases associated with myocardial infarction and paving the way to test these agents in the clinic.
Limitations of the study and future directions
In our experiments, infarct size and cardiac damage is assessed two hours post reperfusion, at a time point that is quite close to the onset of injury and rely on a single type of histochemical measurement. It would be useful to confirm our findings using a biomarker, such as troponin release and to evaluate the effectiveness of H2S donor treatment and their combination in leukocyte infiltration and inflammation in the heart, changes in cardiac metabolism, remodeling and fibrosis and to assess whether H2S donor treatment could prevent or delay the appearance of heart failure post myocardial infarction. Additionally, our study was conducted in male animals. Given the differences in drug responses that exist between males and females, it would be important to determine if our observations hold true in female mice. Useful insights might be gained by using combinations of submaximal concentrations of H2S donors to observe if additive or synergistic effects occur. Finally, it would be important to assess in more detail the underlaying molecular mechanisms that mediate the NO-dependent and NO-independent effects of H2S donors.
Data availability
Raw data from the experiments shown are available to referees and Editors of NSAP upon request.
Abbreviations
- 3MST:
-
3-Mercaptopyruvate sulfurtransferase
- AAR/All:
-
Area at Risk/All
- Akt:
-
Protein Kinase B
- AMI:
-
Acute Myocardial Infarction
- AP39:
-
10‐Oxo‐10‐(4‐(3‐thioxo‐3H‐1,2‐dithiol‐5yl)phenoxy)decyl) triphenylphosphonium bromide
- C3:
-
2-[(4-Hydroxy-6-methylpyrimidin-2-yl)sulfanyl]-1-(naphthalen-1-yl)ethan-1-one
- CD:
-
Control Diet
- cGMP:
-
Cyclic guanosine monophosphate
- CSE:
-
Cystathionine γ-lyase
- CypD:
-
Cyclophilin D
- eNOS:
-
Endothelial Nitric Oxide Synthase
- GSK-3β:
-
Glycogen synthase kinase-3 beta
- GYY4137:
-
[Morpholin-4-ium 4 methoxyphenyl(morpholino) phosphinodithioate]
- H2S:
-
Hydrogen Sulfide
- HF:
-
Heart Failure
- HFD:
-
High Fat Diet
- I/AAR:
-
Infarct/Area at Risk
- I/R:
-
Ischemia/Reperfusion
- IV:
-
Intravenous
- KO:
-
Knockout
- LAD:
-
Left Anterior Descending
- mPTP:
-
Mitochondrial permeability transition pore
- Na2S:
-
Sodium Sulfide
- NaHS:
-
Sodium Hydrosulfide
- NO:
-
Nitric Oxide
- PBS:
-
Phosphate-buffered saline
- PI3K:
-
Phosphoinositide 3-kinase
- RISK:
-
Reperfusion Injury Salvage Kinase
- ROS:
-
Reactive Oxygen Species
- SAFE:
-
Survivor Activating Factor Enhancement
- TTC:
-
2,3,5-Triphenyl-tetrazolium chloride
- WT:
-
Wild type
References
Alexander B, Coles SJ, Fox BC, Khan TF, Maliszewi J, Perry A, Pitak MP, Whiteman M, Wood ME (2015) Investigating the generation of hydrogen sulfide from the phosphinodithioate slow-release donor GYY4137. MedChemComm 6:1649–1655. https://doi.org/10.1039/C5MD00170F
Barr LA, Shimizu Y, Lambert JP, Nicholson CK, Calvert JW (2015) Hydrogen sulfide attenuates high fat diet-induced cardiac dysfunction via the suppression of endoplasmic reticulum stress. Nitric Oxide Biol Chem 46:145–156. https://doi.org/10.1016/J.NIOX.2014.12.013
Bibli SI, Andreadou I, Chatzianastasiou A, Tzimas C, Sanoudou D, Kranias E, Brouckaert P, Coletta C, Szabo C, Kremastinos DT, Iliodromitis EK, Papapetropoulos A (2015) Cardioprotection by H2S engages a cGMP-dependent protein kinase G/phospholamban pathway. Cardiovasc Res 106(3):432–442. https://doi.org/10.1093/CVR/CVV129
Bibli SI, Hu J, Sigala F, Wittig I, Heidler J, Zukunft S, Tsilimigras DI, Randriamboavonjy V, Wittig J, Kojonazarov B, Schürmann C, Siragusa M, Siuda D, Luck B, Abdel Malik R, Filis KA, Zografos G, Chen C, Wang DW, Pfeilschifter J, Brandes RP, Szabo C, Papapetropoulos A, Fleming I (2019) Cystathionine γ lyase sulfhydrates the RNA binding protein human antigen R to preserve endothelial cell function and delay atherogenesis. Circulation 139(1):101–114. https://doi.org/10.1161/CIRCULATIONAHA.118.034757
Bradley JM, Organ CL, Lefer DJ (2016) Garlic-Derived Organic Polysulfides and Myocardial Protection. J Nutr 146(2):403S-409S. https://doi.org/10.3945/JN.114.208066
Chatzianastasiou A, Bibli SI, Andreadou I, Efentakis P, Kaludercic N, Wood ME, Whiteman M, Lisa FD, Daiber A, Manolopoulos VG, Szabó C, Papapetropoulos DA (2016) Cardioprotection by H2S Donors: Nitric Oxide-Dependent and -Independent Mechanisms. J Pharmacol Exp Ther 358(3):431–440. https://doi.org/10.1124/jpet.116.235119
Cirino G, Szabo C, Papapetropoulos A (2023) Physiological roles of hydrogen sulfide in mammalian cells, tissues, and organs. Physiol Rev 103(1):31–276. https://doi.org/10.1152/PHYSREV.00028.2021
Coletta C, Papapetropoulos A, Erdelyi K, Olah G, Módis K, Panopoulos P, Asimakopoulou A, Gerö D, Sharina I, Martin E, Szabo C (2012) Hydrogen sulfide and nitric oxide are mutually dependent in the regulation of angiogenesis and endothelium-dependent vasorelaxation. Proc Natl Acad Sci USA 109(23):9161–9166. https://doi.org/10.1073/PNAS.1202916109
Donnarumma E, Trivedi RK, Lefer DJ (2017) Protective actions of H2S in acute myocardial infarction and heart failure. Compr Physiol 7(2):583–602. https://doi.org/10.1002/cphy.c160023
Edland F, Wergeland A, Kopperud R, Åsrud KS, Hoivik EA, Witsø SL, Æsøy R, Madsen L, Kristiansen K, Bakke M, Døskeland SO, Jonassen AK (2016) Long-term consumption of an obesogenic high fat diet prior to ischemia-reperfusion mediates cardioprotection via Epac1-dependent signaling. Nutr Metab 13(1):1–11. https://doi.org/10.1186/S12986-016-0147-1
Elrod JW, Calvert JW, Morrison J, Doeller JE, Kraus DW, Tao L, Jiao X, Scalia R, Kiss L, Szabo C, Kimura H, Chow CW, Lefer DJ (2007) Hydrogen sulfide attenuates myocardial ischemia-reperfusion injury by preservation of mitochondrial function. Proc Natl Acad Sci USA 104(39):15560–15565. https://doi.org/10.1073/pnas.0705891104
Ferdinandy P, Hausenloy DJ, Heusch G, Baxter GF, Schulz R (2014) Interaction of risk factors, comorbidities, and comedications with ischemia/reperfusion injury and cardioprotection by preconditioning, postconditioning, and remote conditioning. Pharmacol Rev 66(4):1142–1174. https://doi.org/10.1124/PR.113.008300
Ferdinandy P, Andreadou I, Baxter GF, Bøtker HE, Davidson SM, Dobrev D, Gersh BJ, Heusch G, Lecour S, Ruiz-Meana M, Zuurbier CJ, Hausenloy DJ, Schulz R (2023) Interaction of Cardiovascular Nonmodifiable Risk Factors, Comorbidities and Comedications With Ischemia/Reperfusion Injury and Cardioprotection by Pharmacological Treatments and Ischemic Conditioning. Pharmacol Rev 75(1):159–216. https://doi.org/10.1124/PHARMREV.121.000348
Filipovic MR, Zivanovic J, Alvarez B, Banerjee R (2018) Chemical Biology of H2S Signaling through Persulfidation. Chem Rev 118(3):1253–1337. https://doi.org/10.1021/ACS.CHEMREV.7B00205
Griffiths K, Ida T, Morita M, Lamb RJ, Lee JJ, Frenneaux MP, Fukuto JM, Akaike T, Feelisch M, Madhani M (2023) Cysteine hydropersulfide reduces lipid peroxidation and protects against myocardial ischaemia-reperfusion injury - Are endogenous persulfides mediators of ischaemic preconditioning? Redox Biology 60:102605. https://doi.org/10.1016/J.REDOX.2023.102605
Guedes EC, da Silva IB, Lima VM, Miranda JB, Albuquerque RP, Ferreira JCB, Barreto-Chaves MLM, Diniz GP (2019) High fat diet reduces the expression of miRNA-29b in heart and increases susceptibility of myocardium to ischemia/reperfusion injury. J Cell Physiol 234(6):9399–9407. https://doi.org/10.1002/jcp.27624
Hausenloy DJ, Yellon DM (2013) Myocardial ischemia-reperfusion injury: A neglected therapeutic target. J Clin Investig 123(1):92–100. https://doi.org/10.1172/JCI62874
Heusch G (2015) Molecular basis of cardioprotection: signal transduction in ischemic pre-, post-, and remote conditioning. Circ Res 116(4):674–699. https://doi.org/10.1161/CIRCRESAHA.116.305348
Inserte J, Aluja D, Barba I, Ruiz-Meana M, Miró E, Poncelas M, Vilardosa Ú, Castellano J, Garcia-Dorado D (2019) High-fat diet improves tolerance to myocardial ischemia by delaying normalization of intracellular PH at reperfusion. J Mol Cell Cardiol 133(June):164–173. https://doi.org/10.1016/j.yjmcc.2019.06.001
Kanagy NL, Szabo C, Papapetropoulos A (2017) Vascular biology of hydrogen sulfide. Am J Physiol Cell Physiol 312(5):C537–C549. https://doi.org/10.1152/AJPCELL.00329.2016
Kang J, Li Z, Organ CL, Park CM, Yang CT, Pacheco A, Wang D, Lefer DJ, Xian M (2016) pH-Controlled Hydrogen Sulfide Release for Myocardial Ischemia-Reperfusion Injury. J Am Chem Soc 138(20):6336–6339. https://doi.org/10.1021/JACS.6B01373
Karwi QG, Whiteman M, Wood ME, Torregrossa R, Baxter GF (2016) Pharmacological postconditioning against myocardial infarction with a slow-releasing hydrogen sulfide donor, GYY4137. Pharmacol Res 111:442–451. https://doi.org/10.1016/j.phrs.2016.06.028
Karwi QG, Bice JS, Baxter GF (2017a) Pre- and postconditioning the heart with hydrogen sulfide (H2S) against ischemia/reperfusion injury in vivo: a systematic review and meta-analysis. Basic Res Cardiol 113:1–21. https://doi.org/10.1007/S00395-017-0664-8
Karwi QG, Bornbaum J, Boengler K, Torregrossa R, Whiteman M, Wood ME, Schulz R, Baxter GF (2017b) AP39, a mitochondria-targeting hydrogen sulfide (H2S) donor, protects against myocardial reperfusion injury independently of salvage kinase signalling. Br J Pharmacol 174(4):287–301. https://doi.org/10.1111/bph.13688
Kashfi K, Olson KR (2013) Biology and therapeutic potential of hydrogen sulfide and hydrogen sulfide-releasing chimeras. Biochem Pharmacol 85(5):689–703. https://doi.org/10.1016/J.BCP.2012.10.019
Kimura H (2014) Production and Physiological Effects of Hydrogen Sulfide. Antioxid Redox Signal 20(5):783. https://doi.org/10.1089/ARS.2013.5309
King AL, Polhemus DJ, Bhushan S, Otsuka H, Kondo K, Nicholson CK, Bradley JM, Islam KN, Calvert JW, Tao YX, Dugas TR, Kelley EE, Elrod JW, Huang PL, Wang R, Lefer DJ (2014) Hydrogen sulfide cytoprotective signaling is endothelial nitric oxide synthase-nitric oxide dependent. Proc Natl Acad Sci USA 111(8):3182–3187. https://doi.org/10.1073/PNAS.1321871111
Kleinbongard P, Bøtker HE, Ovize M, Hausenloy DJ, Heusch G (2020) Co-morbidities and co-medications as confounders of cardioprotection-Does it matter in the clinical setting? Br J Pharmacol 177(23):5252–5269. https://doi.org/10.1111/BPH.14839
Kolluru GK, Shackelford RE, Shen X, Dominic P, Kevil CG (2023) Sulfide regulation of cardiovascular function in health and disease. Nat Rev Cardiol 20(2):109–125. https://doi.org/10.1038/S41569-022-00741-6
Kondo K, Bhushan S, King AL, Prabhu SD, Hamid T, Koenig S, Murohara T, Predmore BL, Gojon G, Wang R, Karusula N, Nicholson CK, Calvert JW, Lefer DJ (2013) H2S protects against pressure overload-induced heart failure via upregulation of endothelial nitric oxide synthase. Circulation 127(10):1116–1127. https://doi.org/10.1161/CIRCULATIONAHA.112.000855
Lambert JP, Nicholson CK, Amin H, Amin S, Calvert JW (2014) Hydrogen sulfide provides cardioprotection against myocardial/ischemia reperfusion injury in the diabetic state through the activation of the RISK pathway. Med Gas Res 4(1):1–11. https://doi.org/10.1186/S13618-014-0020-0/
Le Trionnaire S, Perry A, Szczesny B, Szabo C, Winyard PG, Whatmore JL, Wood ME, Whiteman M (2014) The synthesis and functional evaluation of a mitochondria-targeted hydrogen sulfide donor, (10-oxo-10-(4-(3-thioxo-3H-1,2-dithiol-5-yl)phenoxy)decyl)triphenylphosphonium bromide (AP39). MedChemComm 5:728–736. https://doi.org/10.1039/C3MD00323J
Lecour S, Andreadou I, Bøtker HE, Davidson SM, Heusch G, Ruiz-Meana M, Schulz R, Zuurbier CJ, Ferdinandy P, Hausenloy DJ, on behalf of the European Union-CARDIOPROTECTION COST ACTION CA16225 (2021) Improving preclinical assessment of cardioprotective therapies (IMPACT) criteria: guidelines of the EU-CARDIOPROTECTION COST Action. Basic Res Cardiol 116(1). https://doi.org/10.1007/S00395-021-00893-5
Lefer DJ, Marbán E (2017) Is Cardioprotection Dead? Circulation 136(1):98–109. https://doi.org/10.1161/CIRCULATIONAHA.116.027039
Levinn CM, Cerda MM, Pluth MD (2020) Activatable Small-Molecule Hydrogen Sulfide Donors. Antioxid Redox Signal 32(2):96–109. https://doi.org/10.1089/ARS.2019.7841
Li L, Whiteman M, Guan YY, Neo KL, Cheng Y, Lee SW, Zhao Y, Baskar R, Tan CH, Moore PK (2008) Characterization of a novel, water-soluble hydrogen sulfide-releasing molecule (GYY4137): new insights into the biology of hydrogen sulfide. Circulation 117(18):2351–2360. https://doi.org/10.1161/CIRCULATIONAHA.107.753467
Li Z, Polhemus DJ, Lefer DJ (2018) Evolution of Hydrogen Sulfide Therapeutics to Treat Cardiovascular Disease. Circ Res 123(5):590–600. https://doi.org/10.1161/CIRCRESAHA.118.311134
Li Z, Xia H, Sharp TE, Lapenna KB, Elrod JW, Casin KM, Liu K, Calvert JW, Chau VQ, Salloum FN, Xu S, Xian M, Nagahara N, Goodchild TT, Lefer DJ (2022) Mitochondrial H2S Regulates BCAA Catabolism in Heart Failure. Circ Res 131(3):222–235. https://doi.org/10.1161/CIRCRESAHA.121.319817
Liu J, Wang P, Zou L, Qu J, Litovsky S, Umeda P, Zhou L, Chatham J, Marsh SA, Dell’Italia LJ, Lloyd SG (2014) High-fat, low-carbohydrate diet promotes arrhythmic death and increases myocardial ischemia-reperfusion injury in rats. Am J Physiol Heart Circ Physiol 307(4):H598–H608
Lundberg JO, Weitzberg E (2022) Nitric oxide signaling in health and disease. Cell 185(16):2853–2878. https://doi.org/10.1016/J.CELL.2022.06.010
Mani S, Li H, Untereiner A, Wu L, Yang G, Austin RC, Dickhout JG, Lhoták Š, Meng QH, Wang R (2013) Decreased endogenous production of hydrogen sulfide accelerates atherosclerosis. Circulation 127(25):2523–2534. https://doi.org/10.1161/CIRCULATIONAHA.113.002208
Papapetropoulos A, Pyriochou A, Altaany Z, Yang G, Marazioti A, Zhou Z, Jeschke MG, Branski LK, Herndon DN, Wang R, Szabó C (2009) Hydrogen sulfide is an endogenous stimulator of angiogenesis. Proc Natl Acad Sci USA 106(51):21972–21977. https://doi.org/10.1073/PNAS.0908047106
Papapetropoulos A, Whiteman M, Cirino G (2015) Pharmacological tools for hydrogen sulphide research: a brief, introductory guide for beginners. Br J Pharmacol 172(6):1633–1637. https://doi.org/10.1111/BPH.12806
Peleli M, Bibli SI, Li Z, Chatzianastasiou A, Varela A, Katsouda A, Zukunft S, Bucci M, Vellecco V, Davos CH, Nagahara N, Cirino G, Fleming I, Lefer DJ, Papapetropoulos A (2020) Cardiovascular phenotype of mice lacking 3-mercaptopyruvate sulfurtransferase. Biochem Pharmacol 176(February):113. https://doi.org/10.1016/j.bcp.2020.113833
Pharoah BM, Khodade VS, Eremiev A, Bao E, Liu T, O’rourke B, Paolocci N, Toscano JP (2022) Hydropersulfides (RSSH) Outperform Post-Conditioning and Other Reactive Sulfur Species in Limiting Ischemia-Reperfusion Injury in the Isolated Mouse Heart. Antioxidants (Basel, Switzerland) 11(5):1010. https://doi.org/10.3390/ANTIOX11051010
Polhemus DJ, Lefer DJ (2014) Emergence of hydrogen sulfide as an endogenous gaseous signaling molecule in cardiovascular disease. Circ Res 114(4):730–737. https://doi.org/10.1161/CIRCRESAHA.114.300505
Powell-Wiley TM, Poirier P, Burke LE, Després JP, Gordon-Larsen P, Lavie CJ, Lear SA, Ndumele CE, Neeland IJ, Sanders P, St-Onge MP (2021) Obesity and Cardiovascular Disease: A Scientific Statement From the American Heart Association. Circulation 143(21):E984–E1010. https://doi.org/10.1161/CIR.0000000000000973
Predmore BL, Kondo K, Bhushan S, Zlatopolsky MA, King AL, Aragon JP, Bennett Grinsfelder D, Condit ME, Lefer DJ (2012) The polysulfide diallyl trisulfide protects the ischemic myocardium by preservation of endogenous hydrogen sulfide and increasing nitric oxide bioavailability. Am J Physiol Heart Circ Physiol 302(11):H2410–H2418. https://doi.org/10.1152/AJPHEART.00044.2012
Salie R, Huisamen B, Lochner A (2014) High carbohydrate and high fat diets protect the heart against ischaemia/reperfusion injury. Cardiovasc Diabetol 13(1):1–12. https://doi.org/10.1186/S12933-014-0109-8
Sun HJ, Wu ZY, Nie XW, Wang XY, Bian JS (2021) An Updated Insight Into Molecular Mechanism of Hydrogen Sulfide in Cardiomyopathy and Myocardial Ischemia/Reperfusion Injury Under Diabetes. Front Pharmacol 12:651884. https://doi.org/10.3389/FPHAR.2021.651884
Szabó G, Veres G, Radovits T, Ger D, Módis K, Miesel-Gröschel C, Horkay F, Karck M, Szabó C (2011) Cardioprotective effects of hydrogen sulfide. Nitric Oxide 25(2):201. https://doi.org/10.1016/J.NIOX.2010.11.001
Szabo C (2017) Hydrogen sulfide, an enhancer of vascular nitric oxide signaling: mechanisms and implications. Am J Physiol Cell Physiol 312(1):C3–C15. https://doi.org/10.1152/AJPCELL.00282.2016
Szabo C, Papapetropoulos A (2017) International Union of Basic and Clinical Pharmacology. CII: Pharmacological Modulation of H2S Levels: H2S Donors and H2S Biosynthesis Inhibitors. Pharmacol Rev 69(4):497–564. https://doi.org/10.1124/PR.117.014050
Szczesny B, Módis K, Yanagi K, Coletta C, Le Trionnaire S, Perry A, Wood ME, Whiteman M, Szabo C (2014) AP39, a novel mitochondria-targeted hydrogen sulfide donor, stimulates cellular bioenergetics, exerts cytoprotective effects and protects against the loss of mitochondrial DNA integrity in oxidatively stressed endothelial cells in vitro. Nitric Oxide - Biol Chem 41(April):120–130. https://doi.org/10.1016/j.niox.2014.04.008
Timmis A, Vardas P, Townsend N, Torbica A, Katus H, De Smedt D, Gale CP, Maggioni AP, Petersen SE, Huculeci R, Kazakiewicz D, de Benito Rubio V, Ignatiuk B, Raisi-Estabragh Z, Pawlak A, Karagiannidis E, Treskes R, Gaita D, Beltrame JF, McConnachie A, Bardinet I, Graham I, Flather M, Elliott P, Mossialos EA, Weidinger F, Achenbach S (2022) Atlas Writing Group, European Society of Cardiology: cardiovascular disease statistics 2021. Eur Heart J 43(8):716–799. https://doi.org/10.1093/EURHEARTJ/EHAB892
Flaxman AD, Naghavi M, Lozano R, Michaud C, Ezzati M, Shibuya K, Salomon JA, Abdalla S, Aboyans V, Abraham J, Ackerman I, Aggarwal R, Ahn SY, Ali MK, Alvarado M, Anderson RH, Anderson LM, Andrews KG, Atkinson C, Baddour LM, Bahalim AN, Barker-Collo S, Barrero LH, Bartels DH, Basáñez M-G, Baxter A, Bell ML, Benjamin EJ, Bennett D, Bernabé E, Bhalla K, Bhandari B, Bikbov B, Abdulhak AB, Birbeck G, Black JA, Blencowe H, Blore JD, Blyth F, Bolliger I, Bonaventure A, Boufous S, Bourne R, Boussinesq M, Braithwaite T, Brayne C, Bridgett L, Brooker S, Brooks P, Brugha TS, Bryan-Hancock C, Bucello C, Buchbinder R, Buckle G, Budke CM, Burch M, Burney P, Burstein R, Calabria B, Campbell B, Canter CE, Carabin H, Carapetis J, Carmona L, Cella C, Charlson F, Chen H, Cheng AT, Chou D, Chugh SS, Coffeng LE, Colan SD, Colquhoun S, Colson KE, Condon J, Connor MD, Cooper LT, Corriere M, Cortinovis M, Courville de Vaccaro K, Couser W, Cowie BC, Criqui MH, Cross M, Dabhadkar KC, Dahiya M, Dahodwala N, Damsere-Derry J, Danaei G, Davis A, De Leo D, Degenhardt L, Dellavalle R, Delossantos A, Denenberg J, Derrett S, Des Jarlais DC, Dharmaratne SD, Dherani M, Diaz-Torne C, Dolk H, Dorsey ER, Driscoll T, Duber H, Ebel B, Edmond K, Elbaz A, Ali SE, Erskine H, Erwin PJ, Espindola P, Ewoigbokhan SE, Farzadfar F, Feigin V, Felson DT, Ferrari A, Ferri CP, Fèvre EM, Finucane MM, Flaxman S, Flood L, Foreman K, Forouzanfar MH, Fowkes FGR, Franklin R, Fransen M, Freeman MK, Gabbe BJ, Gabriel SE, Gakidou E, Ganatra HA, Garcia B, Gaspari F, Gillum RF, Gmel G, Gosselin R, Grainger R, Groeger J, Guillemin F, Gunnell D, Gupta R, Haagsma J, Hagan H, Halasa YA, Hall W, Haring D, Haro JM, Harrison JE, Havmoeller R, Hay RJ, Higashi H, Hill C, Hoen B, Hoffman H, Hotez PJ, Hoy D, Huang JJ, Ibeanusi SE, Jacobsen KH, James SL, Jarvis D, Jasrasaria R, Jayaraman S, Johns N, Jonas JB, Karthikeyan G, Kassebaum N, Kawakami N, Keren A, Khoo J-P, King CH, Knowlton LM, Kobusingye O, Koranteng A, Krishnamurthi R, Lalloo R, Laslett LL, Lathlean T, Leasher JL, Lee YY, Leigh J, Lim SS, Limb E, Lin JK, Lipnick M, Lipshultz SE, Liu W, Loane M, Ohno SL, Lyons R, Ma J, Mabweijano J, MacIntyre MF, Malekzadeh R, Mallinger L, Manivannan S, Marcenes W, March L, Margolis DJ, Marks GB, Marks R, Matsumori A, Matzopoulos R, Mayosi BM, McAnulty JH, McDermott MM, McGill N, McGrath J, Medina-Mora ME, Meltzer M, Mensah GA, Merriman TR, Meyer A-C, Miglioli V, Miller M, Miller TR, Mitchell PB, Mocumbi AO, Moffitt TE, Mokdad AA, Monasta L, Montico M, Moradi-Lakeh M, Moran A, Morawska L, Mori R, Murdoch ME, Mwaniki MK, Naidoo K, Nair MN, Naldi L, Narayan KMV, Nelson PK, Nelson RG, Nevitt MC, Newton CR, Nolte S, Norman P, Norman R, O'Donnell M, O'Hanlon Olives SC, Omer SB, Ortblad K, Osborne R, Ozgediz D, Page A, Pahari B, Pandian JD, Rivero AP, Patten SB, Pearce N, Padilla RP, Perez-Ruiz F, o Perico N, Pesudovs K, Phillips D, Phillips MR, Pierce K, Pion S, Polanczyk GV, Polinder S, Pope CA 3rd, Popova S, Porrini E, Pourmalek F, Prince M, Pullan RL, Ramaiah KD, Ranganathan D, Razavi H, Regan M, Rehm JT, Rein DB, Remuzzi G, Richardson K, Rivara FP, Roberts T, Robinson C, De Leòn FR, Ronfani L, Room R, Rosenfeld LC, Rushton L, Sacco RL, Sukanta Saha, Uchechukwu Sampson, Lidia Sanchez-Riera, Ella Sanman, David C Schwebel, James Graham Scott, Maria Segui-Gomez, Shahraz S, Shepard DS, Shin H, Shivakoti R, Singh D, Singh GM, Singh JA, Singleton J, Sleet DA, Sliwa K, Smith E, Smith JL, Stapelberg NJC, Steer A, Steiner T, Stolk WA, Stovner LJ, Sudfeld C, Syed S, Tamburlini G, Tavakkoli M, Taylor HR, Taylor JA, Taylor WJ, Thomas B, Thomson WM, Thurston GD, Tleyjeh IM, Tonelli M, Towbin JA, Truelsen T, Tsilimbaris MK, Ubeda C, Undurraga EA, van der Werf MJ, van Os J, Vavilala MS, Venketasubramanian N, Wang M, Wang W, Watt K, Weatherall DJ, Weinstock MA, Weintraub R, Weisskopf MG, Weissman MM, White RA, Whiteford H, Wiersma ST, Wilkinson JD, Williams HC, Williams SRM, Witt E, Wolfe F, Woolf AD, Wulf S, Yeh P-H, Zaidi AKM, Zheng Z-J, Zonies D, Lopez AD, Murray CJL, AlMazroa MA, Memish ZA (2012) Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet (London, England) 380(9859):2163–2196. https://doi.org/10.1016/S0140-6736(12)61729-2
Wallace JL, Wang R (2015) Hydrogen sulfide-based therapeutics: exploiting a unique but ubiquitous gasotransmitter. Nat Rev Drug Discov 14(5):329–345. https://doi.org/10.1038/NRD4433
Wang R (2023) Roles of Hydrogen Sulfide in Hypertension Development and Its Complications: What, So What, Now What. Hypertension (Dallas, Tex. : 1979) 80(5):936–944. https://doi.org/10.1161/HYPERTENSIONAHA.122.19456
Wang R, Szabo C, Ichinose F, Ahmed A, Whiteman M, Papapetropoulos A (2015) The role of H2S bioavailability in endothelial dysfunction. Trends Pharmacol Sci 36(9):568–578. https://doi.org/10.1016/J.TIPS.2015.05.007
Weir RAP, McMurray JJV, Velazquez EJ (2006) Epidemiology of heart failure and left ventricular systolic dysfunction after acute myocardial infarction: prevalence, clinical characteristics, and prognostic importance. Am J Cardiol 97(10A):13–25. https://doi.org/10.1016/J.AMJCARD.2006.03.005
Xia H, Li Z, Sharp TE, Polhemus DJ, Carnal J, Moles KH, Tao YX, Elrod J, Pfeilschifter J, Beck KF, Lefer DJ (2020) Endothelial Cell Cystathionine γ-Lyase Expression Level Modulates Exercise Capacity, Vascular Function, and Myocardial Ischemia Reperfusion Injury. J Am Heart Assoc 9(19):e017544. https://doi.org/10.1161/JAHA.120.017544
Xu S, Hamsath A, Neill DL, Wang Y, Yang CT, Xian M (2019) Strategies for the Design of Donors and Precursors of Reactive Sulfur Species. Chemistry (Weinheim an Der Bergstrasse, Germany) 25(16):4005–4016. https://doi.org/10.1002/CHEM.201804895
Yang G, Wang R (2015) H2S and Blood Vessels: An Overview. Handb Exp Pharmacol 230:85–110. https://doi.org/10.1007/978-3-319-18144-8_4
Yellon DM, Hausenloy DJ (2007) Myocardial reperfusion injury. N Engl J Med 357(11):1121–1135. https://doi.org/10.1056/NEJMRA071667
Zhang Z, Huang H, Liu P, Tang C, Wang J (2007) Hydrogen sulfide contributes to cardioprotection during ischemia-reperfusion injury by opening K ATP channels. Can J Physiol Pharmacol 85(12):1248–1253. https://doi.org/10.1139/Y07-120
Zheng Y, Ji X, Ji K, Wang B (2015) Hydrogen sulfide prodrugs-a review. Acta Pharm Sin B 5(5):367–377. https://doi.org/10.1016/J.APSB.2015.06.004
Zheng Y, Yu B, Li Z, Yuan Z, Organ CL, Trivedi RK, Wang S, Lefer DJ, Wang B (2017) An Esterase-Sensitive Prodrug Approach for Controllable Delivery of Persulfide Species. Angew Chem (International Ed. in English) 56(39):11749–11753. https://doi.org/10.1002/ANIE.201704117
Acknowledgements
The authors wish to thank Prof. Matthew Whiteman for providing the GYY4137 sodium salt and the AP39 compound for the present study.
Funding
Open access funding provided by HEAL-Link Greece. This work was supported by the Hellenic Foundation for Research and Innovation under the “First Call for Research Projects to support Faculty members and Researchers and the procurement of high-cost research equipment grant” (Project number: HFRI-FM17-886) to AP and by an Onassis Foundation grant under the Onassis Foundation-BRFAA call to AP.
Author information
Authors and Affiliations
Contributions
AP conceived, designed and supervised research. SR and AC conducted experiments and analyzed the data. SR and AP wrote the manuscript. All authors read and approved the manuscript. The authors declare that all data were generated in-house and that no paper mill was used.
Corresponding author
Ethics declarations
Ethical approval
All animal procedures were in compliance with the European Community guidelines for the use of experimental animals; experimental protocols and all experimental procedures reported here were approved by the veterinary authority of the Prefecture of Athens, in accordance with the national Registration (Presidential Decree 56/2013) in harmony with the European Directive 63/2010 (license number 198212 as modified by 184305).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ravani, S., Chatzianastasiou, A. & Papapetropoulos, A. Using mechanism-based combinations of H2S-donors to maximize the cardioprotective action of H2S. Naunyn-Schmiedeberg's Arch Pharmacol 397, 1853–1864 (2024). https://doi.org/10.1007/s00210-023-02729-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-023-02729-6