Abstract
Background
Antibacterial drugs are successful in combating most types of infections. Irrational use and higher consumption of these drugs can give rise to the antibiotic resistance globally.
Objective
To evaluate antibacterial drug prescribing patterns and antibiogram in infectious disease cases admitted to the hospital.
Methods
A cross-sectional, observational study was conducted from September 2019 to February 2020 among inpatients ward at the hospital after ethical approval. All the data was analysed by the mean and percentage values using Microsoft excel.
Results
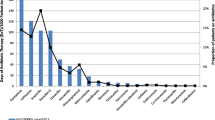
Out of 250 admitted patients, males and females were 156 (62%) and 94 (38%) respectively. The majority of patients 79 (32%) belonged to the age group of 20–40 years. The majority of prescriptions reported were for viral fever 48 (19%), lower respiratory tract infections 40 (16%) and dengue 33 (13%). Antibacterial drugs administered through the intravenous route and the oral route were 301 (83%) and 63 (17%) respectively. The most frequently utilized antibacterial drugs were beta-lactam class ceftriaxone 149 (60%) and the fixed-dose combination, amoxicillin plus clavulanic acid 65 (26%). Further highly prescribed antibacterial drugs were metronidazole 52 (21%), azithromycin 36 (15%), and levofloxacin 24 (10%). In Gram-negative bacteria, Escherichia coli 6 (30%) contributed majorly, while in Gram-positive coagulase-negative, Staphylococci 6 (30%) contributed the highest growth of bacteria for the specific infections in the admitted cases.
Conclusion
Ceftriaxone and the amoxicillin-clavulanic acid combination were highly prescribed among all antibacterial drugs, followed by metronidazole and azithromycin. The current study showed that in the antibiogram pattern, Escherichia coli and coagulase-negative Staphylococci contributed significantly as causative organisms for infectious disease cases. The present study highlighted demographic distribution, infectious diseases with their antibacterial drug utilization patterns and antibiogram assessment in the admitted patients.
Similar content being viewed by others
Data availability
All the data with respect to study presented in the manuscript only.
References
Ali AK, Hartzema AG (2018) Post-authorization Safety studies of medicinal products: The PASS Book. 107–163. Academic Press
Al Shimemeri A, Al Ghadeer H, Memish Z (2011) Antibiotic utilization pattern in a general medical ward of a tertiary medical center in Saudi Arabia. Avicenna J Med 1(1):8
Amaha ND, Berhe YH, Kaushik A (2018) Assessment of inpatient antibiotic use in Halibet National Referral Hospital using WHO indicators: a retrospective study. BMC Res Notes 11(1):1–5
Charles MP, Kali A, Easow JM, Joseph NM, Ravishankar M, Srinivasan S, Kumar S, Umadevi S (2014) Ventilator-associated pneumonia. Australas Med J 7(8):334–344. https://doi.org/10.4066/AMJ.2014.2105
Delgado-Valverde M, Conejo MD, Serrano L, Fernández-Cuenca F, Pascual A (2020) Activity of cefiderocol against high-risk clones of multidrug-resistant Enterobacterales, Acinetobacter baumannii, Pseudomonas aeruginosa and Stenotrophomonas maltophilia. J Antimicrob Chemother 75(7):1840–1849
Demoz GT, Kasahun GG, Hagazy K, Woldu G, Wahdey S, Tadesse DB et al (2020) Prescribing pattern of antibiotics using who prescribing indicators among inpatients in Ethiopia: a need for antibiotic stewardship program. Infect Drug Resist 13:2783–2794
Fridkin S, Baggs J, Fagan R, Magill S, Pollack LA, Malpiedi P, Slayton R, Khader K, Rubin MA, Jones M, Samore MH (2014) Vital signs: improving antibiotic use among hospitalized patients. MMWR Morb Mortal Wkly Rep 63(9):194
Friedman ND, Temkin E, Carmeli Y (2016) The negative impact of antibiotic resistance. Clin Microbiol Infect 22(5):416–422. https://doi.org/10.1016/j.cmi.2015.12.002
Gajic I, Kabic J, Kekic D, Jovicevic M, Milenkovic M, MiticCulafic D, Trudic A, Ranin L, Opavski N (2022) Antimicrobial susceptibility testing: a comprehensive review of currently used methods. Antibiotics (basel) 11(4):427. https://doi.org/10.3390/antibiotics11040427
International Classification of Diseases 11th Revision. The global standard for diagnostic health information. https://icd.who.int/en (referred on 1st July, 2023)
Joshi S (2010) Hospital antibiogram: a necessity. Indian J Med Microbiol 28(4):277–280. https://doi.org/10.4103/0255-0857.71802
Luyt CE, Bréchot N, Trouillet JL, Chastre J (2014) Antibiotic stewardship in the intensive care unit. Crit Care 18(5):1–12
Meena VK, Atray M, Agrawal A (2016) Evaluation of drug utilization pattern in indoor patients of medicine department at tertiary care teaching hospital in Southern Rajasthan. Int J Pharm Sci Res 7(9):3835
Meher BR, Mukharjee D, Shankar U (2014) A study on antibiotic utilization pattern in a general medicine ward of a tertiary care teaching hospital. J Chem Pharm Res. 6:1847–9
Moehring RW, Hazen KC, Hawkins MR, Drew RH, Sexton DJ, Anderson DJ (2015) Challenges in preparation of cumulative antibiogram reports for community hospitals. J Clin Microbiol 53(9):2977–2982. https://doi.org/10.1128/JCM.01077-15
Nagvekar V, Sawant S, Amey S (2020) Prevalence of multidrug-resistant Gram-negative bacteria cases at admission in a multispeciality hospital. J Glob Antimicrob Resist 22:457–461. https://doi.org/10.1016/j.jgar.2020.02.030
Parthasarathi G, Nyfort Hansen K, Nahan MC (2012) A text book of clinical pharmacy practice: essential concepts and skills. Orient Blackswan edition
Pottegård A, Broe A, Aabenhus R, Bjerrum L, Hallas J, Damkier P (2015) Use of antibiotics in children: a Danish nationwide drug utilization study. Pediatr Infect Dis J 34(2):e16-22. https://doi.org/10.1097/INF.0000000000000519
Rangdal K, Kanaki A, Patil K (2019) Drug utilization study of antibiotics in infectious diseases in a tertiary care hospital. Int J Basic Clin Pharmacol 8(3):469
Sawant PM, Padwal LS, Kale SA, Pise NH, Shinde MR (2017) Study of drug prescription pattern among COPD patients admitted to medicine in-patient department of tertiary care hospital. IJBCP 6(9):2228–32. https://doi.org/10.18203/2319-2003.ijbcp20173750
Seifert R, Schirmer B (2021) Problems associated with the use of the term “antibiotics.” Naunyn Schmiedebergs Arch Pharmacol 394(11):2153–2166. https://doi.org/10.1007/s00210-021-02144-9
Sharma S (2018) Tools for assessing and monitoring medicine use. In Pharmaceutical Medicine and Translational Clinical Research, 445–463. Academic Press
Singha J, Chowdhury D, Hazarika H, Krishnatreyya H (2020) Pharmacy practice & drug research https://doi.org/10.21276/ijppdr.2018.8.1.7
Solanki ND, Patel P (2017) Drug utilization pattern and pharmacoeconomic analysis of antihypertensive drugs prescribed in secondary care hospital in Gujarat India. Asian J Pharm Clin Res 10(3):120–4. https://doi.org/10.22159/ajpcr.2017.v10i3.15537
Solanki N, Patel Y (2019) Drug utilization pattern and drug interaction study of antibiotics prescribed to orthopedic patients in private hospital. Arch Pharm Pract 10(4):114–117
Solanki N, Patel V, Patel R (2019) Prescribing trends in cardiovascular conditions: a prospective cross-sectional study. J Basic Clin Pharma 10:23–26
Solanki N, Pandit D, Desai S (2021) Effectiveness and safety assessment of beta-blockers, calcium channel blockers, and angiotensin receptor blockers in hypertensive patients: a prospective study. Am J Cardiovasc Dis 11(5):601
Solanki N, Champaneri I, Patel V (2023) Assessing drug utilization and drug–drug interactions in the management of epilepsy, Alzheimer’s, Parkinson’s disease and migraine. J Pharm Health Serv Res rmad034. https://doi.org/10.1093/jphsr/rmad034
Acknowledgements
The authors acknowledge Ramanbhai Patel College of Pharmacy, Charotar University of Science and Technology and CHARUSAT Hospital, Changa, Gujarat, for providing the necessary facilities and support during the course of the study.
Author information
Authors and Affiliations
Contributions
The authors declare that all data were generated in-house and that no paper mill was used.
Corresponding author
Ethics declarations
Ethical approval
The Institutional Ethics Committee for Human Research of the University ethically approved this study with reference number RPCP/IECHR/2/2019-20/PG/R-02, and permission was obtained from participants for the study and publication.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nilay, S., Shreya, P. & Vivek, S. Assessment of antibacterial drug utilization patterns and antibiogram in infectious diseases: a prospective cross-sectional study. Naunyn-Schmiedeberg's Arch Pharmacol 397, 1053–1059 (2024). https://doi.org/10.1007/s00210-023-02659-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00210-023-02659-3