Abstract
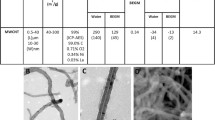
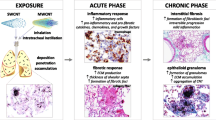
Pulmonary exposure to inhaled particulates elicits complex inflammatory and fibrotic responses that may progress to chronic fibrosis. The fibrogenic potentials of respirable particulates are influenced by their physicochemical properties and their interactions with major pathways to drive fibrotic development in the lung. Macrophages were exposed to six carbon nanotubes (CNTs) of varying dimensions, crystalline silica, or carbon black (CB), with lipopolysaccharide (LPS) and transforming growth factor (TGF)-β1 as positive controls. Macrophage-conditioned media was collected and applied to cultures of human pulmonary fibroblast line WI38-VA13 to induce myofibroblast transformation. Multi-walled and single-walled CNTs (MWCNTs and SWCNTs, respectively) and silica, but not CB, stimulated robust myofibroblast transformation through macrophage-conditioned media. On an equal weight basis, MWCNTs induced higher induction than SWCNTs. High induction was observed for MWCNTs with a long and slender or a short and rigid shape, and silica, at levels comparable to those by LPS and TGF-β1. Fibrogenic particulates induced high levels of IL-1β mRNA expression and protein secretion that are required for macrophage-guided myofibroblast transformation. Induction of IL-1β is dependent on the activation of the NLRP3 (NOD-like receptor family, pyrin domain containing 3) inflammasome and ROS (reactive oxygen species) production in macrophages, as inhibition of NLRP3 by MCC950 and reduction of ROS production by N-acetylcysteine blocked NLRP3 activation, IL-1β induction, and fibroblast activation and differentiation. Therefore, fibrogenic CNTs and silica, but not CB, elicit robust macrophage-guided myofibroblast transformation, which depends on the induction of IL-1β through the NLRP3 inflammasome pathway and the increased production of ROS in macrophages.









Similar content being viewed by others
References
Abderrazak A, Syrovets T, Couchie D et al (2015) NLRP3 inflammasome: from a danger signal sensor to a regulatory node of oxidative stress and inflammatory diseases. Redox Biol 4:296–307. https://doi.org/10.1016/j.redox.2015.01.008
Birch ME, Ruda-Eberenz TA, Chai M, Andrews R, Hatfield RL (2013) Properties that influence the specific surface areas of carbon nanotubes and nanofibers. Ann Occup Hyg 57(9):1148–1166. https://doi.org/10.1093/annhyg/met042
Borthwick LA (2016) The IL-1 cytokine family and its role in inflammation and fibrosis in the lung. Semin Immunopathol 38(4):517–534. https://doi.org/10.1007/s00281-016-0559-z
Coll RC, Robertson AA, Chae JJ et al (2015) A small-molecule inhibitor of the NLRP3 inflammasome for the treatment of inflammatory diseases. Nat Med 21(3):248–255. https://doi.org/10.1038/nm.3806
de Zoete MR, Palm NW, Zhu S, Flavell RA (2014) Inflammasomes. Cold Spring Harb Perspect Biol 6(12):a016287. https://doi.org/10.1101/cshperspect.a016287
Dinarello CA (2009) Immunological and inflammatory functions of the interleukin-1 family. Annu Rev Immunol 27:519–550. https://doi.org/10.1146/annurev.immunol.021908.132612
Donaldson K, Seaton A (2012) A short history of the toxicology of inhaled particles. Part Fibre Toxicol 9:13. https://doi.org/10.1186/1743-8977-9-13
Donaldson K, Aitken R, Tran L et al (2006) Carbon nanotubes: a review of their properties in relation to pulmonary toxicology and workplace safety. Toxicol Sci 92(1):5–22. https://doi.org/10.1093/toxsci/kfj130
Dong J, Ma Q (2015) Advances in mechanisms and signaling pathways of carbon nanotube toxicity. Nanotoxicology 9(5):658–676. https://doi.org/10.3109/17435390.2015.1009187
Dong J, Ma Q (2016a) In vivo activation of a T helper 2-driven innate immune response in lung fibrosis induced by multi-walled carbon nanotubes. Arch Toxicol 90(9):2231–2248. https://doi.org/10.1007/s00204-016-1711-1
Dong J, Ma Q (2016b) Myofibroblasts and lung fibrosis induced by carbon nanotube exposure. Part Fibre Toxicol 13(1):60. https://doi.org/10.1186/s12989-016-0172-2
Dong J, Ma Q (2016c) Suppression of basal and carbon nanotube-induced oxidative stress, inflammation and fibrosis in mouse lungs by Nrf2. Nanotoxicology 10(6):699–709. https://doi.org/10.3109/17435390.2015.1110758
Dong J, Ma Q (2017a) Osteopontin enhances multi-walled carbon nanotube-triggered lung fibrosis by promoting TGF-beta1 activation and myofibroblast differentiation. Part Fibre Toxicol 14(1):18. https://doi.org/10.1186/s12989-017-0198-0
Dong J, Ma Q (2017b) TIMP1 promotes multi-walled carbon nanotube-induced lung fibrosis by stimulating fibroblast activation and proliferation. Nanotoxicology 11(1):41–51. https://doi.org/10.1080/17435390.2016.1262919
Dong J, Ma Q (2018a) Macrophage polarization and activation at the interface of multi-walled carbon nanotube-induced pulmonary inflammation and fibrosis. Nanotoxicology. https://doi.org/10.1080/17435390.2018.1425501
Dong J, Ma Q (2018b) Type 2 Immune Mechanisms in Carbon Nanotube-Induced Lung Fibrosis. Front Immunol 9:1120. https://doi.org/10.3389/fimmu.2018.01120
Dong J, Porter DW, Batteli LA, Wolfarth MG, Richardson DL, Ma Q (2015) Pathologic and molecular profiling of rapid-onset fibrosis and inflammation induced by multi-walled carbon nanotubes. Arch Toxicol 89(4):621–633. https://doi.org/10.1007/s00204-014-1428-y
Dong J, Yu X, Porter DW, Battelli LA, Kashon ML, Ma Q (2016) Common and distinct mechanisms of induced pulmonary fibrosis by particulate and soluble chemical fibrogenic agents. Arch Toxicol 90(2):385–402. https://doi.org/10.1007/s00204-015-1589-3
Dostert C, Petrilli V, Van Bruggen R, Steele C, Mossman BT, Tschopp J (2008) Innate immune activation through Nalp3 inflammasome sensing of asbestos and silica. Science 320(5876):674–677. https://doi.org/10.1126/science.1156995
Duffield JS, Lupher M, Thannickal VJ, Wynn TA (2013) Host responses in tissue repair and fibrosis. Annu Rev Pathol 8:241–276. https://doi.org/10.1146/annurev-pathol-020712-163930
Duke KS, Bonner JC (2018) Mechanisms of carbon nanotube-induced pulmonary fibrosis: a physicochemical characteristic perspective. Wiley Interdiscip Rev Nanomed Nanobiotechnol 10(3):e1498. https://doi.org/10.1002/wnan.1498
Elliott EI, Sutterwala FS (2015) Initiation and perpetuation of NLRP3 inflammasome activation and assembly. Immunol Rev 265(1):35–52. https://doi.org/10.1111/imr.12286
Fraga D, Meulia T, Fenster S (2008) Real-time PCR. Current protocols essential laboratory techniques. Wiley, p 10.3.1–10.3.33. https://doi.org/10.1002/9780470089941.et1003s0
Gasse P, Mary C, Guenon I et al (2007) IL-1R1/MyD88 signaling and the inflammasome are essential in pulmonary inflammation and fibrosis in mice. J Clin Invest 117(12):3786–3799. https://doi.org/10.1172/JCI32285
Gieseck RL 3rd, Wilson MS, Wynn TA (2017) Type 2 immunity in tissue repair and fibrosis. Nat Rev Immunol. https://doi.org/10.1038/nri.2017.90
Guo H, Callaway JB, Ting JP (2015) Inflammasomes: mechanism of action, role in disease, and therapeutics. Nat Med 21(7):677–687. https://doi.org/10.1038/nm.3893
Halasi M, Wang M, Chavan TS, Gaponenko V, Hay N, Gartel AL (2013) ROS inhibitor N-acetyl-l-cysteine antagonizes the activity of proteasome inhibitors. Biochem J 454(2):201–208. https://doi.org/10.1042/BJ20130282
Hamilton RF Jr, Wu Z, Mitra S, Shaw PK, Holian A (2013) Effect of MWCNT size, carboxylation, and purification on in vitro and in vivo toxicity, inflammation and lung pathology. Part Fibre Toxicol 10(1):57. https://doi.org/10.1186/1743-8977-10-57
He X, Ma Q (2012) Redox regulation by nuclear factor erythroid 2-related factor 2: gatekeeping for the basal and diabetes-induced expression of thioredoxin-interacting protein. Mol Pharmacol 82(5):887–897. https://doi.org/10.1124/mol.112.081133
He X, Young SH, Schwegler-Berry D, Chisholm WP, Fernback JE, Ma Q (2011) Multiwalled carbon nanotubes induce a fibrogenic response by stimulating reactive oxygen species production, activating NF-κB signaling, and promoting fibroblast-to-myofibroblast transformation. Chem Res Toxicol 24(12):2237–2248. https://doi.org/10.1021/tx200351d
Hindman B, Ma Q (2018) Carbon nanotubes and crystalline silica induce matrix remodeling and contraction by stimulating myofibroblast transformation in a three-dimensional culture of human pulmonary fibroblasts: role of dimension and rigidity. Arch Toxicol 92(11):3291–3305. https://doi.org/10.1007/s00204-018-2306-9
Hinz B, Phan SH, Thannickal VJ et al (2012) Recent developments in myofibroblast biology: paradigms for connective tissue remodeling. Am J Pathol 180(4):1340–1355. https://doi.org/10.1016/j.ajpath.2012.02.004
Hornung V, Bauernfeind F, Halle A et al (2008) Silica crystals and aluminum salts activate the NALP3 inflammasome through phagosomal destabilization. Nat Immunol 9(8):847–856. https://doi.org/10.1038/ni.1631
Jacobsen NR, White PA, Gingerich J et al (2011) Mutation spectrum in FE1-MUTA(TM) Mouse lung epithelial cells exposed to nanoparticulate carbon black. Environ Mol Mutagen 52(4):331–337. https://doi.org/10.1002/em.20629
Jiao Y, Ma S, Wang Y et al (2016) N-Acetyl cysteine depletes reactive oxygen species and prevents dental monomer-induced intrinsic mitochondrial apoptosis in vitro in human dental pulp cells. PLoS One 11(1):e0147858. https://doi.org/10.1371/journal.pone.0147858
Jo EK, Kim JK, Shin DM, Sasakawa C (2016) Molecular mechanisms regulating NLRP3 inflammasome activation. Cell Mol Immunol 13(2):148–159. https://doi.org/10.1038/cmi.2015.95
Khare S, Radian AD, Dorfleutner A, Stehlik C (2016) Measuring NLR oligomerization I: size exclusion chromatography, co-immunoprecipitation, and cross-linking. Methods Mol Biol 1417:131–143. https://doi.org/10.1007/978-1-4939-3566-6_8
Liu W, Ding I, Chen K et al (2006) Interleukin 1beta (IL1B) signaling is a critical component of radiation-induced skin fibrosis. Radiat Res 165(2):181–191
Mercer RR, Scabilloni JF, Hubbs AF et al (2013) Distribution and fibrotic response following inhalation exposure to multi-walled carbon nanotubes. Part Fibre Toxicol 10:33. https://doi.org/10.1186/1743-8977-10-33
Mia MM, Boersema M, Bank RA (2014) Interleukin-1beta attenuates myofibroblast formation and extracellular matrix production in dermal and lung fibroblasts exposed to transforming growth factor-beta1. PLoS One 9(3):e91559. https://doi.org/10.1371/journal.pone.0091559
Morgan WKC, Seaton A (1995) Occupational lung diseases, 3rd edn. W.B. Saunders Company, Philadelphia
Murray PJ, Wynn TA (2011) Protective and pathogenic functions of macrophage subsets. Nat Rev Immunol 11(11):723–737. https://doi.org/10.1038/nri3073
Nagai H, Okazaki Y, Chew SH et al (2011) Diameter and rigidity of multiwalled carbon nanotubes are critical factors in mesothelial injury and carcinogenesis. Proc Natl Acad Sci USA 108(49):E1330–E1338. https://doi.org/10.1073/pnas.1110013108
NIOSH (2002) Health effects of occupational exposure to respirable crystalline silica. DHHS (NIOSH) Publication No. 2002-129. DHHS CDC NIOSH, Cincinnati
Palomaki J, Valimaki E, Sund J et al (2011) Long, needle-like carbon nanotubes and asbestos activate the NLRP3 inflammasome through a similar mechanism. ACS Nano 5(9):6861–6870. https://doi.org/10.1021/nn200595c
Porter DW, Hubbs AF, Mercer RR et al (2010) Mouse pulmonary dose- and time course-responses induced by exposure to multi-walled carbon nanotubes. Toxicology 269(2–3):136–147. https://doi.org/10.1016/j.tox.2009.10.017
Pozarowski P, Darzynkiewicz Z (2004) Analysis of cell cycle by flow cytometry. Methods Mol Biol 281:301–311. https://doi.org/10.1385/1-59259-811-0:301
Rathinam VA, Vanaja SK, Fitzgerald KA (2012) Regulation of inflammasome signaling. Nat Immunol 13(4):333–342. https://doi.org/10.1038/ni.2237
Sager TM, Castranova V (2009) Surface area of particle administered versus mass in determining the pulmonary toxicity of ultrafine and fine carbon black: comparison to ultrafine titanium dioxide. Part Fibre Toxicol 6:15. https://doi.org/10.1186/1743-8977-6-15
Sargent LM, Porter DW, Staska LM et al (2014) Promotion of lung adenocarcinoma following inhalation exposure to multi-walled carbon nanotubes. Part Fibre Toxicol 11:3. https://doi.org/10.1186/1743-8977-11-3
Sester DP, Zamoshnikova A, Thygesen SJ et al (2016) Assessment of inflammasome formation by flow cytometry. Curr Protoc Immunol 114:14.40.1–14.40.29. https://doi.org/10.1002/cpim.13
Shvedova AA, Kisin ER, Mercer R et al (2005) Unusual inflammatory and fibrogenic pulmonary responses to single-walled carbon nanotubes in mice. Am J Physiol Lung Cell Mol Physiol 289(5):L698–L708. https://doi.org/10.1152/ajplung.00084.2005
Sun SY (2010) Enhancing perifosine’s anticancer efficacy by preventing autophagy. Autophagy 6(1):184–185
Sun B, Wang X, Ji Z et al (2015) NADPH oxidase-dependent NLRP3 inflammasome activation and its important role in lung fibrosis by multiwalled carbon nanotubes. Small 11(17):2087–2097. https://doi.org/10.1002/smll.201402859
Suzui M, Futakuchi M, Fukamachi K et al (2016) Multiwalled carbon nanotubes intratracheally instilled into the rat lung induce development of pleural malignant mesothelioma and lung tumors. Cancer Sci 107(7):924–935. https://doi.org/10.1111/cas.12954
Teran FDE (2016) A new approach towards understanding the ion transfer dynamics in nanostructured carbon-based thin films for energy storage applications. Universite Pierre et Marie Curie, Paris
Tomasek JJ, Gabbiani G, Hinz B, Chaponnier C, Brown RA (2002) Myofibroblasts and mechano-regulation of connective tissue remodelling. Nat Rev Mol Cell Biol 3(5):349–363. https://doi.org/10.1038/nrm809
Tschopp J, Schroder K (2010) NLRP3 inflammasome activation: the convergence of multiple signalling pathways on ROS production? Nat Rev Immunol 10(3):210–215. https://doi.org/10.1038/nri2725
Vesey DA, Cheung C, Cuttle L, Endre Z, Gobe G, Johnson DW (2002) Interleukin-1beta stimulates human renal fibroblast proliferation and matrix protein production by means of a transforming growth factor-beta-dependent mechanism. J Lab Clin Med 140(5):342–350. https://doi.org/10.1067/mlc.2002.128468
Wynn TA, Ramalingam TR (2012) Mechanisms of fibrosis: therapeutic translation for fibrotic disease. Nat Med 18(7):1028–1040. https://doi.org/10.1038/nm.2807
Wynn TA, Vannella KM (2016) Macrophages in tissue repair, regeneration, and fibrosis. Immunity 44(3):450–462. https://doi.org/10.1016/j.immuni.2016.02.015
Yazdi AS, Guarda G, Riteau N et al (2010) Nanoparticles activate the NLR pyrin domain containing 3 (Nlrp3) inflammasome and cause pulmonary inflammation through release of IL-1alpha and IL-1beta. Proc Natl Acad Sci USA 107(45):19449–19454. https://doi.org/10.1073/pnas.1008155107
Funding
This work was funded to Q.M. by the Health Effects Laboratory Division and the Nanotechnology Research Center at National Institute for Occupational Safety and Health, Centers for Disease Control and Prevention, USA, No. 8939050W.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare there are no competing financial interests. The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the National Institute for Occupational Safety and Health, Centers for Disease Control and Prevention.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hindman, B., Ma, Q. Carbon nanotubes and crystalline silica stimulate robust ROS production, inflammasome activation, and IL-1β secretion in macrophages to induce myofibroblast transformation. Arch Toxicol 93, 887–907 (2019). https://doi.org/10.1007/s00204-019-02411-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00204-019-02411-y