Abstract
Summary
In this national cohort study, the patients with acromegaly had significantly higher risks of clinical vertebral (HR 2.09 [1.58–2.78]) and hip (HR 2.52 [1.61–3.95]) fractures than the controls. The increased fracture risk in patients with acromegaly was time-dependent and was observed even during the early period of follow-up.
Purpose
Acromegaly is characterized by the overproduction of growth hormone (GH) and insulin-like growth factor-1 (IGF-1), both play important roles in regulating bone metabolism. We investigated the risk of vertebral and hip fractures in patients with acromegaly compared to age- and sex-matched controls.
Methods
This nationwide population-based cohort study included 1,777 patients with acromegaly aged 40 years or older in 2006–2016 and 8,885 age- and sex-matched controls. A Cox proportional hazards model was used to estimate the adjusted hazard ratio (HR) [95% confidence interval].
Results
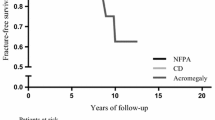
The mean age was 54.3 years and 58.9% were female. For approximately 8.5 years of follow-up, the patients with acromegaly had significantly higher risks of clinical vertebral (HR 2.09 [1.58–2.78]) and hip (HR 2.52 [1.61–3.95]) fractures than the controls in the multivariate analyses. There were significant differences in the risks of clinical vertebral (P < 0.0001) and hip (P < 0.0001) fractures between the patients with acromegaly and the controls in the Kaplan–Meier survival analysis. The multivariable-adjusted HRs for clinical vertebral fractures comparing the patients with acromegaly with controls during and excluding the first 7 years of observation were 1.69 [1.15–2.49] and 2.70 [1.75–4.17], respectively. The HRs for hip fractures during and excluding the first 7 years of observation were 2.29 [1.25–4.18] and 3.36 [1.63–6.92], respectively.
Conclusions
The patients with acromegaly had a higher risk of hip fractures as well as clinical vertebral fractures than the controls. The increased fracture risk in patients with acromegaly was time-dependent and was observed even during the early period of follow-up.


Similar content being viewed by others
References
Eller-Vainicher C, Falchetti A, Gennari L, Cairoli E, Bertoldo F, Vescini F, Scillitani A, Chiodini I (2019) DIAGNOSIS OF ENDOCRINE DISEASE: evaluation of bone fragility in endocrine disorders. Eur J Endocrinol. https://doi.org/10.1530/EJE-18-0991
Giustina A (2020) Acromegaly and vertebral fractures: facts and questions. Trends Endocrinol Metab 31(4):274–275. https://doi.org/10.1016/j.tem.2020.01.011
Carrone F, Ariano S, Piccini S, Milani D, Mirani M, Balzarini L, Lania AG, Mazziotti G (2021) Update on vertebral fractures in pituitary diseases: from research to clinical practice. Hormones (Athens) 20(3):423–437. https://doi.org/10.1007/s42000-021-00275-5
Hong S, Kim KS, Han K, Park CY (2022) Acromegaly and cardiovascular outcomes: a cohort study. Eur Heart J 43(15):1491–1499. https://doi.org/10.1093/eurheartj/ehab822
Mazziotti G, Biagioli E, Maffezzoni F, Spinello M, Serra V, Maroldi R, Floriani I, Giustina A (2015) Bone turnover, bone mineral density, and fracture risk in acromegaly: a meta-analysis. J Clin Endocrinol Metab 100(2):384–394. https://doi.org/10.1210/jc.2014-2937
Fleseriu M, Biller BMK, Freda PU et al (2021) A Pituitary Society update to acromegaly management guidelines. Pituitary 24(1):1–13. https://doi.org/10.1007/s11102-020-01091-7
Giustina A, Barkan A, Beckers A et al (2020) A consensus on the diagnosis and treatment of acromegaly comorbidities: an update. J Clin Endocrinol Metab 105(4). https://doi.org/10.1210/clinem/dgz096
Mazziotti G, Lania AGA, Canalis E (2019) MANAGEMENT OF ENDOCRINE DISEASE: Bone disorders associated with acromegaly: mechanisms and treatment. Eur J Endocrinol 181(2):R45–R56. https://doi.org/10.1530/EJE-19-0184
Anthony JR, Ioachimescu AG (2014) Acromegaly and bone disease. Curr Opin Endocrinol Diabetes Obes 21(6):476–482. https://doi.org/10.1097/MED.0000000000000109
Tran O, Silverman S, Xu X, Bonafede M, Fox K, McDermott M, Gandra S (2021) Long-term direct and indirect economic burden associated with osteoporotic fracture in US postmenopausal women. Osteoporos Int 32(6):1195–1205. https://doi.org/10.1007/s00198-020-05769-3
Uygur MM, Yazici DD, Bugdayci O, Yavuz DG (2021) Prevalence of vertebral fractures and serum sclerostin levels in acromegaly. Endocrine 73(3):667–673. https://doi.org/10.1007/s12020-021-02751-9
Frara S, Melin Uygur M, di Filippo L, Doga M, Losa M, Santoro S, Mortini P, Giustina A (2022) High prevalence of vertebral fractures associated with preoperative GH levels in patients with recent diagnosis of acromegaly. J Clin Endocrinol Metab 107(7):e2843–e2850. https://doi.org/10.1210/clinem/dgac183
Mazziotti G, Bianchi A, Porcelli T, Mormando M, Maffezzoni F, Cristiano A, Giampietro A, De Marinis L, Giustina A (2013) Vertebral fractures in patients with acromegaly: a 3-year prospective study. J Clin Endocrinol Metab 98(8):3402–3410. https://doi.org/10.1210/jc.2013-1460
Wassenaar MJ, Biermasz NR, Hamdy NA et al (2011) High prevalence of vertebral fractures despite normal bone mineral density in patients with long-term controlled acromegaly. Eur J Endocrinol 164(4):475–483. https://doi.org/10.1530/EJE-10-1005
Mazziotti G, Bianchi A, Bonadonna S, Cimino V, Patelli I, Fusco A, Pontecorvi A, De Marinis L, Giustina A (2008) Prevalence of vertebral fractures in men with acromegaly. J Clin Endocrinol Metab 93(12):4649–4655. https://doi.org/10.1210/jc.2008-0791
Ha J, Jeong C, Han KD, Lim Y, Kim MK, Kwon HS, Song KH, Kang MI, Baek KH (2021) Comparison of fracture risk between type 1 and type 2 diabetes: a comprehensive real-world data. Osteoporos Int 32(12):2543–2553. https://doi.org/10.1007/s00198-021-06032-z
Bolanowski M, Halupczok J, Jawiarczyk-Przybylowska A (2015) Pituitary disorders and osteoporosis. Int J Endocrinol 2015(206853. https://doi.org/10.1155/2015/206853
Petrossians P, Daly AF, Natchev E et al (2017) Acromegaly at diagnosis in 3173 patients from the Liege Acromegaly Survey (LAS) database. Endocr Relat Cancer 24(10):505–518. https://doi.org/10.1530/ERC-17-0253
Kwon H, Jung JH, Han KD, Park YG, Cho JH, Lee DY, Han JM, Park SE, Rhee EJ, Lee WY (2018) Prevalence and annual incidence of thyroid disease in Korea from 2006 to 2015: a nationwide population-based cohort study. Endocrinol Metab (Seoul) 33(2):260–267. https://doi.org/10.3803/EnM.2018.33.2.260
Wang SM, Han KD, Kim NY, Um YH, Kang DW, Na HR, Lee CU, Lim HK (2020) Association of alcohol intake and fracture risk in elderly varied by affected bones: A nationwide longitudinal study. Psychiatry Investig 17(10):1013–1020. https://doi.org/10.30773/pi.2020.0143
Ueland T, Fougner SL, Godang K, Schreiner T, Bollerslev J (2006) Serum GH and IGF-I are significant determinants of bone turnover but not bone mineral density in active acromegaly: a prospective study of more than 70 consecutive patients. Eur J Endocrinol 155(5):709–715. https://doi.org/10.1530/eje.1.02285
Bolanowski M, Daroszewski J, Medraś M, Zadrozna-Sliwka B (2006) Bone mineral density and turnover in patients with acromegaly in relation to sex, disease activity, and gonadal function. J Bone Miner Metab 24(1):72–78. https://doi.org/10.1007/s00774-005-0649-9
Piskinpasa ME, Piskinpasa H (2022) Bone biochemical markers in acromegaly: An association with disease activity and gonadal status. North Clin Istanb 9(1):74–81. https://doi.org/10.14744/nci.2020.35467
Madeira M, Neto LV, de Paula Paranhos Neto F, Barbosa Lima IC, Carvalho de Mendonca LM, Gadelha MR, Fleiuss de Farias ML (2013) Acromegaly has a negative influence on trabecular bone, but not on cortical bone, as assessed by high-resolution peripheral quantitative computed tomography. J Clin Endocrinol Metab 98(4):1734–1741. https://doi.org/10.1210/jc.2012-4073
Ott SM (2018) Cortical or trabecular bone: What’s the difference? Am J Nephrol 47(6):373–375. https://doi.org/10.1159/000489672
Godang K, Lekva T, Normann KR, Olarescu NC, Øystese KAB, Kolnes A, Ueland T, Bollerslev J, Heck A (2019) Hip structure analyses in acromegaly: decrease of cortical bone thickness after treatment: a longitudinal cohort study. JBMR Plus 3(12):e10240. https://doi.org/10.1002/jbm4.10240
Mazziotti G, Lania AG, Canalis E (2022) Skeletal disorders associated with the growth hormone-insulin-like growth factor 1 axis. Nat Rev Endocrinol 18(6):353–365. https://doi.org/10.1038/s41574-022-00649-8
Liu Z, Solesio ME, Schaffler MB, Frikha-Benayed D, Rosen CJ, Werner H, Kopchick JJ, Pavlov EV, Abramov AY, Yakar S (2019) Mitochondrial function is compromised in cortical bone osteocytes of long-lived growth hormone receptor null mice. J Bone Miner Res 34(1):106–122. https://doi.org/10.1002/jbmr.3573
Dalle Carbonare L, Micheletti V, Cosaro E, Valenti MT, Mottes M, Francia G, Davì MV (2018) Bone histomorphometry in acromegaly patients with fragility vertebral fractures. Pituitary 21(1):56–64. https://doi.org/10.1007/s11102-017-0847-1
Malgo F, Hamdy NAT, Rabelink TJ, Kroon HM, Claessen K, Pereira AM, Biermasz NR, Appelman-Dijkstra NM (2017) Bone material strength index as measured by impact microindentation is altered in patients with acromegaly. Eur J Endocrinol 176(3):339–347. https://doi.org/10.1530/eje-16-0808
Cellini M, Biamonte E, Mazza M et al (2021) Vertebral fractures associated with spinal sagittal imbalance and quality of life in acromegaly: a radiographic study with EOS 2D/3D technology. Neuroendocrinology 111(8):775–785. https://doi.org/10.1159/000511811
Vestergaard P, Mosekilde L (2004) Fracture risk is decreased in acromegaly–a potential beneficial effect of growth hormone. Osteoporos Int 15(2):155–159. https://doi.org/10.1007/s00198-003-1531-z
Valassi E, Crespo I, Malouf J, Llauger J, Aulinas A, Marin AM, Biagetti B, Webb SM (2016) Reduction of trabecular and cortical volumetric bone mineral density at the proximal femur in patients with acromegaly. Eur J Endocrinol 174(2):107–114. https://doi.org/10.1530/EJE-15-0931
Appelman-Dijkstra NM, Biermasz NR (2017) Understanding and predicting fracture risk in acromegaly. Endocrine 55(3):662–663. https://doi.org/10.1007/s12020-017-1238-0
Ribeiro de Moura C, Campos Lopes S, Monteiro AM (2022) Determinants of skeletal fragility in acromegaly: a systematic review and meta-analysis. Pituitary 25(6):780–794. https://doi.org/10.1007/s11102-022-01256-6
Sorohan MC, Poiana C (2022) Vertebral fractures in acromegaly: a systematic review. J Clin Med 12(1). https://doi.org/10.3390/jcm12010164
Chiloiro S, Giampietro A, Frara S et al (2020) Effects of Pegvisomant and Pasireotide LAR on vertebral fractures in acromegaly resistant to first-generation SRLs. J Clin Endocrinol Metab 105(3). https://doi.org/10.1210/clinem/dgz054
Vitali E, Palagano E, Schiavone ML, Mantovani G, Sobacchi C, Mazziotti G, Lania A (2022) Direct effects of octreotide on osteoblast cell proliferation and function. J Endocrinol Invest 45(5):1045–1057. https://doi.org/10.1007/s40618-022-01740-7
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
Hyemi Kwon, Kyung-Do Han, Bong-Sung Kim, Sun Joon Moon, Se Eun Park, Eun-Jung Rhee, and Won-Young Lee declare that they have no conflict of interest.
Financial disclosure
Hyemi Kwon, Kyung-Do Han, Bong-Sung Kim, Sun Joon Moon, Se Eun Park, Eun-Jung Rhee, and Won-Young Lee declare that they have nothing to declare.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Hyemi Kwon and Kyung-Do Han contributed equally (co-first authors).
Eun-Jung Rhee and Won-Young Lee contributed equally (co-corresponding authors).
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kwon, H., Han, KD., Kim, BS. et al. Acromegaly and the long-term fracture risk of the vertebra and hip: a national cohort study. Osteoporos Int 34, 1591–1600 (2023). https://doi.org/10.1007/s00198-023-06800-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-023-06800-z