Abstract
Purpose
Vertebral fractures (VFs) are a potential complication in acromegaly. However, the etiology of this skeletal fragility is unknown. This review aimed to evaluate the effect of acromegaly on VFs, bone turnover, areal bone mineral density (aBMD), and bone quality/microarchitecture. The effect of disease activity and gonadal status in these determinants of skeletal fragility was also evaluated.
Methods
Articles published in English until September 6, 2020 on PubMed and Embase that reported at least one determinant of skeletal fragility in acromegalic patients, were included. Odds ratio (OR) to evaluate the risk of VFs and the standardized mean difference (SMD) to evaluate bone turnover, aBMD and bone quality/microarchitecture were calculated.
Results
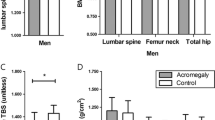
Fifty-eight studies met eligibility criteria, assembling a total of 2412 acromegalic patients. Of these, 49 studies were included in the meta-analysis. Acromegalic patients, when compared to non-acromegalic patients, had higher risk of VFs [OR 7.00; 95% confidence interval (CI) 2.80–17.52; p < 0.0001], higher bone formation (SMD 1.14; 95% CI 0.69–1.59; p < 0.00001), higher bone resorption (SMD 0.60; 95% CI 0.09–1.10; p = 0.02) and higher aBMD at the femoral neck (SMD 0.36; 95% CI 0.15–0.57; p = 0.0009). No significant differences were found regarding aBMD at lumbar spine. Considering the results of the different techniques evaluating bone quality/microarchitecture, the main reported alterations were a decrease in trabecular bone thickness and density, and an increase in trabecular separation. The presence of active disease and/or hypogonadism were associated with worst results.
Conclusion
Patients with acromegaly are at increased risk of VFs, mainly because of deterioration in bone microarchitecture.












Similar content being viewed by others
Data availability
The datasets generated during the current study are not publicly available but are available from the corresponding author on reasonable request.
Code availability
Not applicable.
References
Katznelson L, Laws ER, Melmed S, Molitch ME, Murad MH, Utz A et al (2014) Acromegaly: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 99(11):3933–3951. https://doi.org/10.1210/jc.2014-2700
Vilar L, Vilar CF, Lyra R, Lyra R, Naves LA (2017) Acromegaly: clinical features at diagnosis. Pituitary 20(1):22–32. https://doi.org/10.1007/s11102-016-0772-8
Wassenaar MJE, Biermasz NR, Hamdy NAT, Zillikens MC, Van Meurs JBJ, Rivadeneira F et al (2011) High prevalence of vertebral fractures despite normal bone mineral density in patients with long-term controlled acromegaly. Eur J Endocrinol 164(4):475–483. https://doi.org/10.1530/EJE-10-1005
Mazziotti G, Bianchi A, Bonadonna S, Cimino V, Patelli I, Fusco A et al (2008) Prevalence of vertebral fractures in men with acromegaly. J Clin Endocrinol Metab 93(12):4649–4655. https://doi.org/10.1210/jc.2008-0791
Giustina A, Mazziotti G, Canalis E (2008) Growth hormone, insulin-like growth factors, and the skeleton. Endocr Rev 29(5):535–559. https://doi.org/10.1210/er.2007-0036
Zgliczynski W, Kochman M, Misiorowski W, Zdunowski P (2007) In acromegaly, increased bone mineral density (BMD) is determined by GH-excess, gonadal function and gender. Neuroendocrinol Lett 28(5):621–628
Eller-Vainicher C, Falchetti A, Gennari L, Cairoli E, Bertoldo F, Vescini F et al (2019) Diagnosis of endocrine disease: evaluation of bone fragility in endocrine disorders. Eur J Endocrinol 180(6):R213–R232. https://doi.org/10.1530/EJE-18-0991
Kaji H, Sugimoto T, Nakaoka D, Okimura Y, Kaji H, Abe H et al (2001) Bone metabolism and body composition in Japanese patients with active acromegaly. Clin Endocrinol (Oxf) 55(2):175–181. https://doi.org/10.1046/j.1365-2265.2001.01280.x
Giustina A (2020) Acromegaly and vertebral fractures: facts and questions. Trends Endocrinol Metab 31(4):274–275. https://doi.org/10.1016/j.tem.2020.01.011
Mazziotti G, Frara S, Giustina A (2018) Pituitary diseases and bone. Endocr Rev 39(4):440–488. https://doi.org/10.1210/er.2018-00005
Liu YL, Hsu JT, Shih TY, Luzhbin D, Tu CY, Wu J (2018) Quantification of volumetric bone mineral density of proximal femurs using a two-compartment model and computed tomography images. Biomed Res Int. https://doi.org/10.1155/2018/6284269
Kužma M, Killinger Z, Jackuliak P, Vaòuga P, Hans D, Binkley N et al (2019) Pathophysiology of growth hormone secretion disorders and their impact on bone microstructure as measured by trabecular bone score. Physiol Res 68:121–129. https://doi.org/10.33549/physiolres.934303
Higgins J, Thompson S, Deeks J, Altman D (2003) Measuring inconsistency in meta-analyses. BMJ 327(7412):557–560. https://doi.org/10.1136/bmj.327.7414.557
Higgins J, Li T, Deeks J (2020) Chapter 6—choosing effect measures and computing estimates of effects. Cochrane. https://training.cochrane.org/handbook/current/chapter-06. Accessed 20 July 2020
Brozek JL, Akl EA, Alonso-Coello P, Lang D, Jaeschke R, Williams JW, Phillips B, Lelgemann M, Lethaby A, Bousquet J, Guyatt GH, Schünemann HJ, GRADE Working Group (2009) Grading quality of evidence and strength of recommendations in clinical practice guidelines. Part 1 of 3. An overview of the GRADE approach and grading quality of evidence about interventions. Allergy 64(5):669–677. https://doi.org/10.1111/j.1398-9995.2009.01973.x
Štěpán J, Marek J, Havránek T, Doležal V, Pacovský V (1979) Bone isoenzyme of serum alkaline phosphatase in acromegaly. Clin Chim Acta 93(3):355–363. https://doi.org/10.1016/0009-8981(79)90285-7
de la Piedra C, Larrañaga J, Castro N, Horcajada C, Rapado A, Herrera Pombo JL, Carbó E (1988) Correlation among plasma osteocalcin, growth hormone, and somatomedin C in acromegaly. Calcif Tissue Int 43(1):44–45. https://doi.org/10.1007/BF02555167
Diamond T, Nery L, Posen S (1989) Spinal and peripheral bone mineral densities in acromegaly: the effects of excess growth hormone and hypogonadism. Ann Intern Med 111(7):567–573. https://doi.org/10.7326/0003-4819-111-7-567
Ho PJ, Fig LM, Barkan AL, Shapiro B (1992) Bone mineral density of the axial skeleton in acromegaly. J Nucl Med 33(9):1608–1612
Marazuela M, Astigarraga B, Tabuenca MJ, Estrada J, Marín F, Lucas T (1993) Serum bone Gla protein as a marker of bone turnover in acromegaly. Calcif Tissue Int 52(6):419–421. https://doi.org/10.1007/BF00571329
Legovini P, De Menis E, Doroldi C, Carteri A, Billeci D, Roiter I et al (1993) Parathormone levels during treatment of acromegaly with octreotide: one-year follow-up. Curr Ther Res 53(4):360–366. https://doi.org/10.1016/S0011-393X(05)80195-X
Kotzmann H, Bernecker P, Hübsch P, Pietschmann P, Woloszczuk W, Svoboda T et al (1993) Bone mineral density and parameters of bone metabolism in patients with acromegaly. J Bone Miner Res 8(4):459–465. https://doi.org/10.1002/jbmr.5650080410
Piovesan A, Terzolo M, Reimondo G, Pia A, Codegone A, Osella G et al (1994) Biochemical markers of bone and collagen turnover in acromegaly or Cushing’s syndrome. Horm Metab Res 26(5):234–237. https://doi.org/10.1055/s-2007-1001672
Scillitani A, Chiodini I, Carnevale V, Giannatempo GM, Frusciante V, Villella M et al (1997) Skeletal involvement in female acromegalic subjects: the effects of growth hormone excess in amenorrheal and menstruating patients. J Bone Miner Res 12(10):1729–1736. https://doi.org/10.1359/jbmr.1997.12.10.1729
Longobardi S, Di Somma C, Di Rella F, Angelillo N, Ferone D, Colao A et al (1998) Bone mineral density and circulating cytokines in patients with acromegaly. J Endocrinol Investig 21(10):688–693. https://doi.org/10.1007/BF03350799
Bolanowski M, Wielgus W, Milewicz A, Marciniak R (2000) Axial bone mineral density in patients with acromegaly. Acad Radiol 7(8):592–594. https://doi.org/10.1016/s1076-6332(00)80573-5
Ueland T, Bollerslev J, Godang K, Müller F, Frøland SS, Aukrust P (2001) Increased serum osteoprotegerin in disorders characterized by persistent immune activation or glucocorticoid excess—possible role in bone homeostasis. Eur J Endocrinol 145(6):685–690. https://doi.org/10.1530/eje.0.1450685
Minisola S, Dionisi S, Pacitti MT, Paglia F, Carnevale V, Scillitani A et al (2002) Gender differences in serum markers of bone resorption in healthy subjects and patients with disorders affecting bone. Osteoporos Int 13(2):171–175. https://doi.org/10.1007/s001980200009
Ueland T, Ebbesen EN, Thomsen JS, Mosekilde L, Brixen K, Flyvbjerg A et al (2002) Decreased trabecular bone biomechanical competence, apparent density, IGF-II and IGFBP-5 content in acromegaly. Eur J Clin Investig 32(2):122–128. https://doi.org/10.1046/j.1365-2362.2002.00944.x
Bolanowski M, Jȩdrzejuk D, Milewicz A, Arkowska A (2002) Quantitative ultrasound of the heel and some parameters of bone turnover in patients with acromegaly. Osteoporos Int 13(4):303–308. https://doi.org/10.1007/s001980200030
Scillitani A, Battista C, Chiodini I, Carnevale V, Fusilli S, Ciccarelli E et al (2003) Bone mineral density in acromegaly: the effect of gender, disease activity and gonadal status. Clin Endocrinol (Oxf) 58(6):725–731. https://doi.org/10.1046/j.1365-2265.2003.01777.x
Matsuyama J, Eshima N, Fukunaga T, Hori S, Kobayashi H, Isono M (2003) Various risks of osteoporosis in patients with pituitary adenomas. J Bone Miner Metab 21(2):91–97. https://doi.org/10.1007/s007740300015
Parkinson C, Kassem M, Heickendorff L, Flyvbjerg A, Trainer PJ (2003) Pegvisomant-induced serum insulin-like growth factor-I normalization in patients with acromegaly returns elevated markers of bone turnover to normal. J Clin Endocrinol Metab 88(12):5650–5655. https://doi.org/10.1210/jc.2003-030772
Tütüncü NB, Erbaş T (2004) Factors associated with bone metabolism in acromegalic patients: hypogonadism and female gender. Exp Clin Endocrinol Diabetes 112(6):328–332. https://doi.org/10.1055/s-2004-820913
Bonadonna S, Mazziotti G, Nuzzo M, Bianchi A, Fusco A, De Marinis L et al (2005) Increased prevalence of radiological spinal deformities in active acromegaly: a cross-sectional study in postmenopausal women. J Bone Miner Res 20(10):1837–1844. https://doi.org/10.1359/JBMR.050603
Biermasz NR, Hamdy NAT, Pereira AM, Romijn JA, Roelfsema F (2005) Long-term maintenance of the anabolic effects of GH on the skeleton in successful treated patients with acromegaly. Eur J Endocrinol 152(1):53–60. https://doi.org/10.1530/eje.1.01820
Bolanowski M, Daroszewski J, Mȩdraś M, Zadrozna-Śliwka B (2006) Bone mineral density and turnover in patients with acromegaly in relation to sex, disease activity, and gonadal function. J Bone Miner Metab 24(1):72–78. https://doi.org/10.1007/s00774-005-0649-9
White HD, Ahmad AM, Durham BH, Chandran S, Patwala A, Fraser WD et al (2006) Effect of active acromegaly and its treatment on parathyroid circadian rhythmicity and parathyroid target-organ sensitivity. J Clin Endocrinol Metab 91(3):913–919. https://doi.org/10.1210/jc.2005-1602
Ueland T, Fougner SL, Godang K, Schreiner T, Bollerslev J (2006) Serum GH and IGF-I are significant determinants of bone turnover but not bone mineral density in active acromegaly: a prospective study of more than 70 consecutive patients. Eur J Endocrinol 155(5):709–715. https://doi.org/10.1530/eje.1.02285
Bolanowski M, Pluskiewicz W, Adamczyk P, Daroszewski J (2006) Quantitative ultrasound at the hand phalanges in patients with acromegaly. Ultrasound Med Biol 32(2):191–195. https://doi.org/10.1016/j.ultrasmedbio.2005.10.003
Kastelan D, Dusek T, Kraljevic I, Polasek O, Perkovic Z, Kardum I et al (2007) Bone properties in patients with acromegaly: quantitative ultrasound of the heel. J Clin Densitom 10(3):327–331. https://doi.org/10.1016/j.jocd.2007.03.103
Sasaki M, Okazaki R, Inoue D, Nakashima M, Ide F, Nakaguchi H et al (2009) Preoperative elevated serum growth hormone is preventive of osteopenia in postsurgical patients with pituitary somatotroph adenomas: comparison with clinically nonfunctioning adenomas. Endocrinologist 19(5):208–210
Battista C, Chiodini I, Muscarella S, Guglielmi G, Mascia ML, Carnevale V et al (2009) Spinal volumetric trabecular bone mass in acromegalic patients: a longitudinal study. Clin Endocrinol (Oxf) 70(3):378–382. https://doi.org/10.1111/j.1365-2265.2008.03322.x
Sucunza Alfonso N, Barahona MJ, Resmini E, Fernández-Real JM, Ricart W, Farrerons J et al (2009) A link between bone mineral density and serum adiponectin and visfatin levels in acromegaly. J Clin Endocrinol Metab 94(10):3889–3896. https://doi.org/10.1210/jc.2009-0474
Madeira M, Neto LV, De Lima GAB, Moreira RO, De Mendonça LMC, Gadelha MR et al (2010) Effects of GH-IGF-I excess and gonadal status on bone mineral density and body composition in patients with acromegaly. Osteoporos Int 21(12):2019–2025. https://doi.org/10.1007/s00198-009-1165-x
Padova G, Borzì G, Incorvaia L, Siciliano G, Migliorino V, Vetri M et al (2011) Prevalence of osteoporosis and vertebral fractures in acromegalic patients. Clin Cases Miner Bone Metab 8(3):37–43
Madeira M, Neto LV, De Paula Paranhos Neto F, Lima ICB, De Mendonça LMC, Gadelha MR et al (2013) Acromegaly has a negative influence on trabecular bone, but not on cortical bone, as assessed by high-resolution peripheral quantitative computed tomography. J Clin Endocrinol Metab 98(4):1734–1741. https://doi.org/10.1210/jc.2012-4073
Madeira M, Neto LV, Torres CH, de Mendonça LMC, Gadelha MR, de Farias MLF (2013) Vertebral fracture assessment in acromegaly. J Clin Densitom 16(2):238–243. https://doi.org/10.1016/j.jocd.2012.06.002
Mazziotti G, Bianchi A, Porcelli T, Mormando M, Maffezzoni F, Cristiano A et al (2013) Vertebral fractures in patients with acromegaly: a 3-year prospective study. J Clin Endocrinol Metab 98(8):3402–3410. https://doi.org/10.1210/jc.2013-1460
Serinsöz H, Ertörer ME, Başcıl S, Bakıner O, Bozkırlı E, Tütüncü NB (2015) Low prevalence of periodontitis in acromegaly: growth hormone may exert a protective effect. Turkish J Endocrinol Metab 19(2):42–48
Maffezzoni F, Maddalo M, Frara S, Mezzone M, Zorza I, Baruffaldi F et al (2016) High-resolution-cone beam tomography analysis of bone microarchitecture in patients with acromegaly and radiological vertebral fractures. Endocrine 54(2):532–542. https://doi.org/10.1007/s12020-016-1078-3
Hong AR, Kim JH, Kim SW, Kim SY, Shin CS (2016) Trabecular bone score as a skeletal fragility index in acromegaly patients. Osteoporos Int 27(3):1123–1129. https://doi.org/10.1007/s00198-015-3344-2
Valassi E, Crespo I, Malouf J, Vilades D, Leta R, Llauger J et al (2016) Epicardial fat is a negative predictor of spine volumetric bone mineral density and trabecular bone score in acromegaly. Endocrine 53(3):860–864. https://doi.org/10.1007/s12020-016-0945-2
Tuzcu S, Durmaz A, Carlıoğlu A, Demircan Z, Tuzcu A, Beyaz C et al (2017) The effects of high serum growth hormone and IGF-1 levels on bone mineral density in acromegaly. Z Rheumatol 76(8):716–722. https://doi.org/10.1007/s00393-016-0171-6
Malgo F, Hamdy NAT, Papapoulos SE, Appelman-Dijkstra NM (2017) Bone material strength index as measured by impact microindentation is low in patients with fractures irrespective of fracture site. Osteoporos Int 28(8):2433–2437. https://doi.org/10.1007/s00198-017-4054-8
Constantin T, Tangpricha V, Shah R, Oyesiku NM, Ioachimescu OC, Ritchie J et al (2017) Calcium and bone turnover markers in acromegaly: a prospective, controlled study. J Clin Endocrinol Metab 102(7):2416–2424. https://doi.org/10.1210/jc.2016-3693
Silva PPB, Amlashi FG, Yu EW, Pulaski-liebert KJ, Gerweck AV, Fazeli K et al (2017) Bone microarchitecture and estimated bone strength in men with active acromegaly. Eur J Endocrinol 177(5):409–420. https://doi.org/10.1530/EJE-17-0468
Chiloiro S, Mormando M, Bianchi A, Giampietro A, Milardi D, Bima C et al (2018) Prevalence of morphometric vertebral fractures in “difficult” patients with acromegaly with different biochemical outcomes after multimodal treatment. Endocrine 59(2):449–453. https://doi.org/10.1007/s12020-017-1391-5
Carbonare LD, Micheletti V, Cosaro E, Valenti MT, Mottes M, Francia G et al (2018) Bone histomorphometry in acromegaly patients with fragility vertebral fractures. Pituitary 21(1):56–64. https://doi.org/10.1007/s11102-017-0847-1
Valenti MT, Mottes M, Cheri S, Deiana M, Micheletti V, Cosaro E et al (2018) Runx2 overexpression compromises bone quality in acromegalic patients. Endocr Relat Cancer 25(3):269–277. https://doi.org/10.1530/ERC-17-0523
Ozer FF, Dagdelen S, Erbas T (2018) Relation of RANKL and OPG levels with bone resorption in patients with acromegaly and prolactinoma. Horm Metab Res 50(7):562–567. https://doi.org/10.1055/a-0630-1529
Qin L, Guo X, Gao L, Wang Z, Feng C, Deng K et al (2019) Preoperative and postoperative bone mineral density change and risk factor analysis in patients with a GH-secreting pituitary adenoma. Int J Endocrinol. https://doi.org/10.1155/2019/21012566
Godang K, Lekva T, Normann KR, Olarescu NC, Øystese KAB, Kolnes A et al (2019) Hip structure analyses in acromegaly: decrease of cortical bone thickness after treatment: a longitudinal cohort study. JBMR Plus 3(12):e10240. https://doi.org/10.1002/jbm4.10240
Kužma M, Vaňuga P, Ságova I, Pávai D, Jackuliak P, Killinger Z et al (2019) Non-invasive DXA-derived bone structure assessment of acromegaly patients: a cross-sectional study. Eur J Endocrinol 180(3):201–211. https://doi.org/10.1530/EJE-18-0881
Valassi E, García-Giralt N, Malouf J, Crespo I, Llauger J, Díez-Pérez A et al (2019) Circulating mir-103a-3p and mir-660-5p are associated with bone parameters in patients with controlled acromegaly. Endocr Connect 8(1):39–49. https://doi.org/10.1530/EC-18-0482
Chiloiro S, Giampietro A, Stefano F, Chiara B, Frederico D, Fleseriu M et al (2019) Effects of pegvisomant and pasireotide LAR on vertebral fractures in acromegaly resistant to first-generation SRLs. J Clin Endocrinol Metab 105(3):dgz054. https://doi.org/10.1210/clinem/dgz054
Pelsma ICM, Biermasz NR, Pereira AM, van Furth WR, Appelman-Dijkstra NM, Kloppenburg M et al (2020) Progression of vertebral fractures in long-term controlled acromegaly: a 9-year follow-up study. Eur J Endocrinol 183(4):427–437. https://doi.org/10.1530/EJE-20-0415
Zhang Y, Liu M, Chen H, Zhu K, Feng W, Zhu D et al (2020) Associations between circulating bone-derived hormones lipocalin 2, osteocalcin, and glucose metabolism in acromegaly. J Endocrinol Investig 43(9):1309–1316. https://doi.org/10.1007/s40618-020-01221-9
de Castro DO, de Azevedo BP, Dytz MG, Barbosa BA, Júnior AJ, Reggatieri NAT et al (2020) Entropy and uniformity as additional parameters to optimize the effectiveness of bone CT in the evaluation of acromegalic patients. Endocrine 69(2):368–376. https://doi.org/10.1007/s12020-020-02358-6
Mys K, Stockmans F, Vereecke E, van Lenthe GH (2017) Quantification of bone microstructure in the wrist using cone-beam computed tomography. Bone 2018(114):206–214. https://doi.org/10.1016/j.bone.2018.06.006
Parfitt AM (2002) Misconceptions (2): turnover is always higher in cancellous than in cortical bone. Bone 30(6):807–809. https://doi.org/10.1016/S8756-3282(02)00735-4
Claessen KMJA, Kroon HM, Pereira AM, Appelman-Dijkstra NM, Verstegen MJ, Kloppenburg M et al (2013) Progression of vertebral fractures despite long-term biochemical control of acromegaly: a prospective follow-up study. J Clin Endocrinol Metab 98(12):4808–4815. https://doi.org/10.1210/jc.2013-2695
Ott SM (2018) Cortical or trabecular bone: what’s the difference? Am J Nephrol 47(6):373–375. https://doi.org/10.1159/000489672
Wassenaar MJE, Biermasz NR, van Duinen N, van der Klaauw AA, Pereira AM, Roelfsena F et al (2009) High prevalence of arthropathy, according to the definitions of radiological and clinical osteoarthritis, in patients with long-term cure of acromegaly: a case–control study. Eur J Endocrinol 160(3):357–365. https://doi.org/10.1530/EJE-08-0845
Eller-Vainicher C, Cairoli E, Zhukouskaya VV, Morelli V, Palmieri S, Scillitani A et al (2013) Prevalence of subclinical contributors to low bone mineral density and/or fragility fracture. Eur J Endocrinol 169(2):225–237. https://doi.org/10.1530/EJE-13-0102
Giustina A, Barkan A, Beckers A, Biermasz N, Biller B, Boguszewski C et al (2020) A consensus on the diagnosis and treatment of acromegaly comorbidities: an uptade. J Clin Endocrinol Metab 105(4):dgz096. https://doi.org/10.1210/clinem/dgz096
Mazziotti G, Battista C, Maffezzoni F, Chiloiro S, Ferrante E, Prencipe N et al (2020) Treatment of acromegalic osteopathy in real-life clinical practice: the BAAC (Bone Active Drugs in Acromegaly) Study. J Clin Endocrinol Metab. https://doi.org/10.1210/clinem/dgaa363
Hardy RS, Zhou H, Seibel MJ, Cooper MS (2018) Glucocorticoids and bone: consequences of endogenous and exogenous excess and replacement therapy. Endocr Rev 39(5):519–548. https://doi.org/10.1210/er.2018-00097
Mercado M, Gonzalez B, Vargas G, Ramirez C, de los Monteros AL, Sosa E, Jervis P, Roldan P, Mendoza V, López-Félix B, Guinto G (2014) Successful mortality reduction and control of comorbidities in patients with acromegaly followed at a highly specialized multidisciplinary clinic. J Clin Endocrinol Metab 99:4438–4446. https://doi.org/10.1210/jc.2014-2670
Ceccato F, Lizzul L, Zilio M, Barbot M, Denaro L, Emanuelli E, Alessio L, Rolma G, Manara R, Saller A, Boscaro M, Scaroni C (2016) Medical treatment for acromegaly does not increase the risk of central adrenal insufficiency: a long-term follow-up study. Horm Metab Res 48(8):514–519
Sherlock M, Reulen RC, Alonso AA, Ayuk J, Clayton RN, Sheppard MC, Hawkins MM, Bates AS, Stewart PM (2009) ACTH deficiency, higher doses of hydrocortisone replacement, and radiotherapy are independent predictors of mortality in patients with acromegaly. J Clin Endocrinol Metab 94:4216–4223. https://doi.org/10.1210/jc.2009-1097
Schulz J, Frey KR, Cooper MS et al (2016) Reduction in daily hydrocortisone dose improves bone health in primary adrenal insufficiency. Eur J Endocrinol 174(4):531–538. https://doi.org/10.1530/EJE-15-1096
Krzentowska-Korek A, Gołkowski F, Bałdys-Waligórska A, Hubalewska-Dydejczyk A (2011) Efficacy and complications of neurosurgical treatment of acromegaly. Pituitary 14:157–162. https://doi.org/10.1007/s11102-010-0273-0
Katznelson L (2010) Approach to the patient with persistent acromegaly after pituitary surgery. J Clin Endocrinol Metab 95:4114–4123. https://doi.org/10.1210/jc.2010-0670
Minniti G, Jaffrain-Rea ML, Esposito V, Santoro A, Moroni C, Lenzi J, Tamburrano G, Cassone R, Cantore G (2001) Surgical treatment and clinical outcome of GH-secreting adenomas in elderly patients. Acta Neurochir 143:1205–1211. https://doi.org/10.1007/s007010100015
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
The study was conceptualized by AMM and supervised by AMM and SCL. All authors contributed to the study design. Material preparation, data collection, selection, and analysis were performed by CRM and SCL. Discrepancies in data selection were solved by AMM (senior). The first draft of the manuscript text was written by CRM and SCL and all authors participated in the revision of the manuscript. All authors read and approved the final manuscript. CRM and SCL should be considered as equally contributing authors (shared co-first authorship).
Corresponding author
Ethics declarations
Conflict of interest
The authors have nothing to disclose.
Ethical approval
The study followed the recommended guidelines for good clinical practice and ethics. The research protocol was submitted and approved by the Ethics Committee for Health of Hospital de Braga and the Ethics Committee for Life and Health Sciences of University of Minho. The protocol was registered with the International Prospective Register of Systematic Reviews (Registration No. CRD42021230349) in February 2021.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ribeiro de Moura, C., Campos Lopes, S. & Monteiro, A.M. Determinants of skeletal fragility in acromegaly: a systematic review and meta-analysis. Pituitary 25, 780–794 (2022). https://doi.org/10.1007/s11102-022-01256-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11102-022-01256-6