Abstract
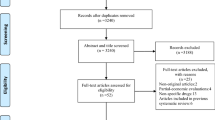
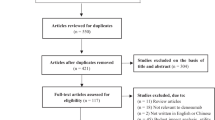
Sequential treatment of osteoporosis has been increasingly mentioned in recent years. However, the corresponding systematic review has not been reported. This study aims to systematically review and assess all full-text pharmacoeconomic studies of sequential treatment for osteoporosis. A comprehensive literature search was performed using PubMed, EMBASE (Ovid), CNKI, and Wanfang Database to identify original articles, published before June 17, 2022. The quality of included articles was evaluated by the updated Consolidated Health Economic Evaluation Reporting Standards (CHEERS 2022) and the European Society for Clinical and Economic Aspects of Osteoporosis, Osteoarthritis and Musculoskeletal Diseases International Osteoporosis Foundation (ESCEO-IOF). In general, ten articles were included in this review. For the comparison between sequential treatment and bisphosphonate monotherapy, more than 75% of studies demonstrated the sequential treatment was cost-effective or dominant, with the exception of sequential treatment involving teriparatide. When the comparisons occurred between the two sequential treatment groups, the sequential treatments associated with either abaloparatide or romosozumab were cost-effective or dominant compared to the sequential treatment involving teriparatide. Several major key drivers of cost-effectiveness included drug cost, medication persistence and adherence, drug effect on fracture risk, offset effect, time horizon, and baseline fracture risk. The most of studies were identified as high quality in CHEERS (2022) and ESCEO-IOF. The cost-effectiveness of sequential treatment for osteoporosis is influenced by multiple factors. Generally, the sequential treatments involving abaloparatide, romosozumab, denosumab, and bisphosphonates may be considered as the preferred option for osteoporosis with high fracture risk, while the sequential treatment with teriparatide was not a cost-effectiveness strategy. The ESCEO-IOF and CHEER (2022) increase the transparency, comparability, extrapolation, and quality of research, engage patients and the general public in research on health services and policies, and help improve the quality of health technology assessment.


Similar content being viewed by others
Data availability
Data availability.
References
Kanis JA et al (2020) Algorithm for the management of patients at low, high and very high risk of osteoporotic fractures. Osteoporos Int 31(1):1–12
Black DM, Rosen CJ (2016) Clinical practice Postmenopausal Osteoporosis. N Engl J Med 374(3):254–262
Rashki Kemmak A et al (2020) Economic burden of osteoporosis in the world: a systematic review. Med J Islam Repub Iran 34:154
Munoz M, Robinson K, Shibli-Rahhal A (2020) Bone health and osteoporosis prevention and treatment. Clin Obstet Gynecol 63(4):770–787
Management of Osteoporosis in Postmenopausal Women: The Position Statement of The North American Menopause Society'' Editorial, P (2021) Management of osteoporosis in postmenopausal women: the 2021 position statement of The North American Menopause Society. Menopause 28(9): 973–997.
Curtis EM et al (2016) Epidemiology of fractures in the United Kingdom 1988–2012: variation with age, sex, geography, ethnicity and socioeconomic status. Bone 87:19–26
Kanis JA et al (2019) Executive summary of the European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Calcif Tissue Int 104(3):235–238
Parthan A et al (2013) Cost effectiveness of denosumab versus oral bisphosphonates for postmenopausal osteoporosis in the US. Appl Health Econ Health Policy 11(5):485–497
Chinese Medical Association (2019) Epidemiological survey of osteoporosis in China and “Healthy Bones” special action results released.
Liu H, Li B (2017) Prospect of combination and sequential therapies for postmenopausal osteoporosis. Curr Pharm Des 23(41):6251–6255
Cheng C, Wentworth K, Shoback DM (2020) New Frontiers in Osteoporosis Therapy. Annu Rev Med 71:277–288
Curtis EM et al (2022) Management of patients at very high risk of osteoporotic fractures through sequential treatments. Aging-Clinical & Experimental Research 34(4):695–714
Langdahl B (2020) Treatment of postmenopausal osteoporosis with bone-forming and antiresorptive treatments: combined and sequential approaches. Bone 139:115516
Frost HM (1979) Treatment of osteoporoses by manipulation of coherent bone cell populations. Clin Orthop Relat Res 143:227–244
Abrahamsen B (2015) Bone: sequential osteoporosis treatment–the order of things. Nat Rev Endocrinol 11(10):570–572
Schafer AL et al (2012) Six months of parathyroid hormone (1–84) administered concurrently versus sequentially with monthly ibandronate over two years: the PTH and ibandronate combination study (PICS) randomized trial. J Clin Endocrinol Metab 97(10):3522–3529
Reginster J et al (2019) Abaloparatide for risk reduction of nonvertebral and vertebral fractures in postmenopausal women with osteoporosis: a network meta-analysis. Osteoporos Int 30(7):1465–1473
Reginster JY et al (2018) Effect of a sequential treatment combining abaloparatide and alendronate for the management of postmenopausal osteoporosis. Expert Opin Pharmacother 19(2):159–161
Hiligsmann M et al (2015) A systematic review of cost-effectiveness analyses of drugs for postmenopausal osteoporosis. Pharmacoeconomics 33(3):205–224
Li N et al (2021) An updated systematic review of cost-effectiveness analyses of drugs for osteoporosis. Pharmacoeconomics 39(2):181–209
Page MJ et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71
Husereau D et al (2022) Consolidated Health Economic Evaluation Reporting Standards 2022 (CHEERS 2022) statement: updated reporting guidance for health economic evaluations. Value Health 25(1):3–9
World Congress on Osteoporosis (2020) Osteoarthritis and Musculoskeletal Diseases (WCO-IOF-ESCEO 2020): ESPRM-ESCEO-IOF symposium abstracts. Osteoporos Int 31(Suppl 1):71–73
Le QA et al (2019) Cost-effectiveness analysis of sequential treatment of abaloparatide followed by alendronate versus teriparatide followed by alendronate in postmenopausal women with osteoporosis in the United States. Ann Pharmacother 53(2):134–143
Soreskog E et al (2021) Cost-effectiveness of romosozumab for the treatment of postmenopausal women with severe osteoporosis at high risk of fracture in Sweden. Osteoporos Int 32(3):585–594
Mori T et al (2021) Cost-effectiveness of sequential daily teriparatide/weekly alendronate compared with alendronate monotherapy for older osteoporotic women with prior vertebral fracture in Japan. Arch Osteoporos 16(1):72
You R et al (2022) Cost-effectiveness of sequential denosumab/zoledronic acid compared with zoledronic acid monotherapy for postmenopausal osteoporotic women in China. Front Pharmacol 13:816248
Mori T, Crandall CJ, Ganz DA (2019) Cost-effectiveness of sequential teriparatide/alendronate versus alendronate-alone strategies in high-risk osteoporotic women in the US: analyzing the impact of generic/biosimilar teriparatide. JBMR Plus 3(11):e10233
You R et al (2022) Cost-effectiveness of sequential teriparatide/zoledronic acid compared with zoledronic acid monotherapy for postmenopausal osteoporotic women in China. Front Public Health 10:794861
Hiligsmann M et al (2020) Cost-effectiveness of sequential treatment with abaloparatide followed by alendronate vs. alendronate monotherapy in women at increased risk of fracture a US payer perspective. Semin Arthritis Rheum 50(3):394–400
Hiligsmann M et al (2019) Cost-effectiveness of sequential treatment with abaloparatide vs teriparatide for United States women at increased risk of fracture. Semin Arthritis Rheum 49(2):184–196
Mori T et al (2021) Cost-effectiveness of zoledronic acid compared with sequential denosumab/alendronate for older osteoporotic women in Japan. Arch Osteoporos 16(1):113
Hagino H et al (2021) Cost effectiveness of romosozumab versus teriparatide for severe postmenopausal osteoporosis in Japan. Osteoporos Int 32(10):2011–2021
Stahl JE (2008) Modelling methods for pharmacoeconomics and health technology assessment: an overview and guide. Pharmacoeconomics 26(2):131–148
Min C et al (2021) An overview of the characteristics and quality assessment criteria in systematic review of pharmacoeconomics. PLoS ONE 16(2):e0246080
Azharuddin M et al (2020) Systematic evidence of health economic evaluation of drugs for postmenopausal osteoporosis: a quality appraisal. Osteoporos Sarcopenia 6(2):39–52
Morizio P, Burkhart JI, Ozawa S (2018) Denosumab: a unique perspective on adherence and cost-effectiveness compared with oral bisphosphonates in osteoporosis patients. Ann Pharmacother 52(10):1031–1041
Hamine S et al (2015) Impact of mHealth chronic disease management on treatment adherence and patient outcomes: a systematic review. J Med Internet Res 17(2):e52
Ha Dinh TT et al (2016) The effectiveness of the teach-back method on adherence and self-management in health education for people with chronic disease: a systematic review. JBI Database System Rev Implement Rep 14(1):210–247
Pisani P et al (2016) Major osteoporotic fragility fractures: risk factor updates and societal impact. World J Orthop 7(3):171–181
Bouxsein ML et al (2019) Change in bone density and reduction in fracture risk: a meta-regression of published trials. J Bone Miner Res 34(4):632–642
Hiligsmann, M., et al (2022) Improving the reporting of economic evaluation in osteoporosis: the value of CHEERS 2022 statement. Osteoporos Int
Ni W, Jiang Y (2017) Evaluation on the cost-effective threshold of osteoporosis treatment on elderly women in China using discrete event simulation model. Osteoporos Int 28(2):529–538
Sugrue DM et al (2019) Economic modelling of chronic kidney disease: a systematic literature review to inform conceptual model design. Pharmacoeconomics 37(12):1451–1468
Caro JJ, Moller J (2016) Advantages and disadvantages of discrete-event simulation for health economic analyses. Expert Rev Pharmacoecon Outcomes Res 16(3):327–329
Milne R, Carswell C (2022) CHEERS to 30 years of pharmacoeconomics. Pharmacoeconomics 40(1):5–6
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yu, G., Tong, S., Liu, J. et al. A systematic review of cost‑effectiveness analyses of sequential treatment for osteoporosis. Osteoporos Int 34, 641–658 (2023). https://doi.org/10.1007/s00198-022-06626-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-022-06626-1