Abstract
Summary
Although vertebral fracture is more common among alcoholic liver cirrhosis patients when compared to general population, current data on three-dimensional micro-architecture are scarce. Our study showed significant trabecular deterioration in lumbar vertebrae obtained from alcoholic liver cirrhosis donors, suggesting that they should be advised to undergo early-stage screening for osteoporosis.
Purpose
Recent studies showed an increased incidence of vertebral fractures in alcoholic liver cirrhosis (ALC) patients, while data about vertebral micro-structure are still limited. The aim of this study was to compare trabecular and cortical micro-architecture of lumbar vertebrae between ALC patients and healthy age- and sex-matched controls.
Methods
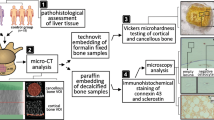
Our study included lumbar vertebral samples of male cadaveric donors, divided into ALC (n = 20, age: 59 ± 6 years) and control group (n = 20, age: 59 ± 8 years). Following pathohistological verification of liver cirrhosis, trabecular and cortical bone micro-architecture was analyzed by micro-computed tomography (micro-CT).
Results
Micro-CT evaluation of the trabecular bone in lumbar vertebrae showed a significant decrease in bone volume fraction, trabecular thickness, trabecular number, and connectivity (p < 0.01). In contrast to trabecular deterioration, prominent alteration in cortical parameters was not observed in lumbar vertebrae of ALC patients (p > 0.05).
Conclusions
Our data indicate that susceptibility to non-traumatic fractures in ALC patients could be explained by alterations in trabecular bone micro-architecture. Thus, we genuinely recommend osteological screening of the lumbar spine for all ALC patients in order to evaluate individual fracture risk.

Graphical abstract



Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this article [and its supplementary information files] and could be available from the corresponding author on request.
References
Blachier M, Leleu H, Peck-Radosavljevic M, Valla DC, Roudot-Thoraval F (2013) The burden of liver disease in Europe: a review of available epidemiological data. J Hepatol 58:593–608. https://doi.org/10.1016/j.jhep.2012.12.005
Streba LAM, Vere CC, Streba CT, Ciurea ME (2014) Focus on alcoholic liver disease: from nosography to treatment. World J Gastroenterol 20:8040–8047. https://doi.org/10.3748/wjg.v20.i25.8040
Crawford BAL, Kam C, Donaghy AJ, McCaughan GW (2003) The heterogeneity of bone disease in cirrhosis: a multivariate analysis. Osteoporos Int 14:987–994. https://doi.org/10.1007/s00198-003-1495-z
Alcalde Vargas A, Pascasio Acevedo JM, Gutiérrez Domingo I, García Jiménez R, Sousa Martín JM, Ferrer Ríos MT, Sayago Mota M, Giráldez Gallego A, Gómez Bravo MA (2012) Prevalence and characteristics of bone disease in cirrhotic patients under evaluation for liver transplantation. Transplant Proc 44:1496–1498. https://doi.org/10.1016/j.transproceed.2012.05.011
Culafić D, Djonic D, Culafic-Vojinovic V, Ignjatovic S, Soldatovic I, Vasic J, Beck TJ, Djuric M (2014) Evidence of degraded BMD and geometry at the proximal femora in male patients with alcoholic liver cirrhosis. Osteoporos Int 26:253–259. https://doi.org/10.1007/s00198-014-2849-4
Liang J, Meng WD, Yang JM, Li SL, Zhong MN, Hou XX, Wang R, Long YY, Bao LX, Bao M (2018) The association between liver cirrhosis and fracture risk: a systematic review and meta-analysis. Clin Endocrinol 89:408–413. https://doi.org/10.1111/cen.13762
Guañabens N, Parés A (2018) Osteoporosis in chronic liver disease. Liver Int 38:776–785. https://doi.org/10.1111/liv.13730
López-Larramona G, Lucendo AJ, González-Delgado L (2013) Alcoholic liver disease and changes in bone mineral density. Rev Española Enfermedades Dig 105:609–621. https://doi.org/10.4321/s1130-01082013001000006
Wibaux C, Legroux-Gerot I, Dharancy S, Boleslawski E, Declerck N, Canva V, Mathurin P, Pruvot FR, Cortet B (2011) Assessing bone status in patients awaiting liver transplantation. Jt Bone Spine 78:387–391. https://doi.org/10.1016/j.jbspin.2011.03.001
Kanis JA, Johansson H, Johnell O, Oden A, de Laet C, Eisman JA, Pols H, Tenenhouse A (2005) Alcohol intake as a risk factor for fracture. Osteoporos Int 16:737–742. https://doi.org/10.1007/s00198-004-1734-y
Chakkalakal DA (2005) Alcohol-induced bone loss and deficient bone repair. Alcohol Clin Exp Res 29:2077–2090. https://doi.org/10.1097/01.alc.0000192039.21305.55
Alvisa-Negrín J, González-Reimers E, Santolaria-Fernández F et al (2009) Osteopenia in alcoholics: effect of alcohol abstinence. Alcohol Alcohol 44:468–475. https://doi.org/10.1093/alcalc/agp038
González-Reimers E, Martín-González C, De la vega-Prieto MJ et al (2013) Serum sclerostin in alcoholics: a pilot study. Alcohol Alcohol 48:278–282. https://doi.org/10.1093/alcalc/ags136
Weitzmann MN (2017) Bone and the immune system. Toxicol Pathol 45:911–924. https://doi.org/10.1177/0192623317735316
González-Reimers E, Santolaria-Fernández F, Martín-González MC, Fernández-Rodríguez CM, Quintero-Platt G (2014) Alcoholism: a systemic proinflammatory condition. World J Gastroenterol 20:14660–14671. https://doi.org/10.3748/wjg.v20.i40.14660
Weitzmann MN, Ofotokun I (2016) Physiological and pathophysiological bone turnover-role of the immune system. Nat Rev Endocrinol 12:518–532. https://doi.org/10.1038/nrendo.2016.91
Santos LAA, Lima TB, Augusti L, Franzoni LC, Yamashiro FS, Bolfi F, Nunes VS, Dorna MS, de Oliveira CV, Caramori CA, Silva GF, Romeiro FG (2016) Handgrip strength as a predictor of bone mineral density in outpatients with cirrhosis. J Gastroenterol Hepatol 31:229–234. https://doi.org/10.1111/jgh.13062
D’Amelio P, Sassi F (2018) Gut microbiota, immune system, and bone. Calcif Tissue Int 102:415–425. https://doi.org/10.1007/s00223-017-0331-y
López-Larramona G, Lucendo AJ, González-Castillo S, Tenias JM (2011) Hepatic osteodystrophy: an important matter for consideration in chronic liver disease. World J Hepatol 3:300–307. https://doi.org/10.4254/wjh.v3.i12.300
Cohen A, Dempster DW, Müller R, Guo XE, Nickolas TL, Liu XS, Zhang XH, Wirth AJ, van Lenthe GH, Kohler T, McMahon DJ, Zhou H, Rubin MR, Bilezikian JP, Lappe JM, Recker RR, Shane E (2010) Assessment of trabecular and cortical architecture and mechanical competence of bone by high-resolution peripheral computed tomography: comparison with transiliac bone biopsy. Osteoporos Int 21:263–273. https://doi.org/10.1007/s00198-009-0945-7
Guichelaar MMJ, Malinchoc M, Sibonga J et al (2002) Bone metabolism in advanced cholestatic liver disease: analysis by bone histomorphometry. Hepatology 36:895–903. https://doi.org/10.1053/jhep.2002.36357
Wakolbinger R, Muschitz C, Scheriau G, Bodlaj G, Kocijan R, Feichtinger X, Schanda JE, Haschka J, Resch H, Pietschmann P (2019) Bone microarchitecture and bone turnover in hepatic cirrhosis. Osteoporos Int 30:1195–1204. https://doi.org/10.1007/s00198-019-04870-6
Jorge-Hernandez JA, Gonzalez-Reimers CE, Torres-Ramirez A, Santolaria-Fernandez F, Gonzalez-Garcia C, Batista-Lopez JN, Pestana-Pestana M, Hernandez-Nieto L (1988) Bone changes in alcoholic liver cirrhosis - a histomorphometrical analysis of 52 cases. Dig Dis Sci 33:1089–1095. https://doi.org/10.1007/BF01535783
O’Shea RS, Dasarathy S, McCullough AJ et al (2010) Alcoholic liver disease. Hepatology 51:307–328. https://doi.org/10.1002/hep.23258
vom Scheidt A, Grisolia Seifert EF, Pokrant C et al (2019) Subregional areal bone mineral density (aBMD) is a better predictor of heterogeneity in trabecular microstructure of vertebrae in young and aged women than subregional trabecular bone score (TBS). Bone 122:156–165. https://doi.org/10.1016/j.bone.2019.02.014
Kaiser J, Allaire B, Fein PM, Lu D, Adams A, Kiel DP, Jarraya M, Guermazi A, Demissie S, Samelson EJ, Bouxsein ML, Morgan EF (2020) Heterogeneity and spatial distribution of intravertebral trabecular bone mineral density in the lumbar spine is associated with prevalent vertebral fracture. J Bone Miner Res 35:641–648. https://doi.org/10.1002/jbmr.3946
Kim DG, Hunt CA, Zauel R, Fyhrie DP, Yeni YN (2007) The effect of regional variations of the trabecular bone properties on the compressive strength of human vertebral bodies. Ann Biomed Eng 35:1907–1913. https://doi.org/10.1007/s10439-007-9363-1
Schmidt T, Schmidt C, Schmidt FN, Butscheidt S, Mussawy H, Hubert J, Hawellek T, Oehler N, Barvencik F, Lohse AW, Schinke T, Schramm C, Amling M, Rolvien T (2018) Disease duration and stage influence bone microstructure in patients with primary biliary cholangitis. J Bone Miner Res 33:1011–1019. https://doi.org/10.1002/jbmr.3410
Schnitzler CM, Mesquita JM, Shires R (2010) Cortical and trabecular bone microarchitecture and turnover in alcohol-induced chronic pancreatitis: a histomorphometric study. J Bone Miner Metab 28:456–467. https://doi.org/10.1007/s00774-009-0151-x
Crilly RG, Anderson C, Hogan D, Delaquerrière-Richardson L (1988) Bone histomorphometry, bone mass, and related parameters in alcoholic males. Calcif Tissue Int 43:269–276. https://doi.org/10.1007/BF02556634
Shen C-L (2012) Alcohol-induced bone loss and quality during adolescence is improved by green tea polyphenols. J Clin Toxicol S7:4–11. https://doi.org/10.4172/2161-0495.s7-004
Callaci JJ, Himes R, Lauing K, Wezeman FH, Brownson K (2009) Binge alcohol-induced bone damage is accompanied by differential expression of bone remodeling-related genes in rat vertebral bone. Calcif Tissue Int 84:474–484. https://doi.org/10.1007/s00223-009-9240-z
Guañabens N, Parés A (2011) Management of osteoporosis in liver disease. Clin Res Hepatol Gastroenterol 35:438–445. https://doi.org/10.1016/j.clinre.2011.03.007
Jeong HM, Kim DJ (2019) Bone diseases in patients with chronic liver disease. Int J Mol Sci 20:4270. https://doi.org/10.3390/ijms20174270
Beck TJ, Ruff CB, Warden KE et al (2018) Osteoporosis in chronic liver disease. Liver Int 38:776–785. https://doi.org/10.1111/liv.13730
Wakolbinger R, Muschitz C, Wallwitz J, Bodlaj G, Feichtinger X, Schanda JE, Resch H, Baierl A, Pietschmann P (2020) Serum levels of sclerostin reflect altered bone microarchitecture in patients with hepatic cirrhosis. Wien Klin Wochenschr 132:19–26. https://doi.org/10.1007/s00508-019-01595-8
Seeman E (2008) Bone quality: the material and structural basis of bone strength. J Bone Miner Metab 26:1–8. https://doi.org/10.1007/s00774-007-0793-5
Van Der Linden JC, Homminga J, Verhaar JAN, Weinans H (2001) Mechanical consequences of bone loss in cancellous bone. J Bone Miner Res 16:457–465. https://doi.org/10.1359/jbmr.2001.16.3.457
Bang CS, Shin IS, Lee SW, Kim JB, Baik GH, Suk KT, Yoon JH, Kim YS, Kim DJ (2015) Osteoporosis and bone fractures in alcoholic liver disease: a meta-analysis. World J Gastroenterol 21:4038–4047. https://doi.org/10.3748/wjg.v21.i13.4038
Fazzalari NL, Parkinson IH, Fogg QA, Sutton-Smith P (2006) Antero-postero differences in cortical thickness and cortical porosity of T12 to L5 vertebral bodies. Jt Bone Spine 73:293–297. https://doi.org/10.1016/j.jbspin.2005.03.023
Osterhoff G, Morgan EF, Shefelbine SJ, Karim L, McNamara LM, Augat P (2016) Bone mechanical properties and changes with osteoporosis. Injury 47:S11–S20. https://doi.org/10.1016/S0020-1383(16)47003-8
Svedbom A, Ivergård M, Hernlund E, Rizzoli R, Kanis JA (2014) Epidemiology and economic burden of osteoporosis in Switzerland. Arch Osteoporos 9:187. https://doi.org/10.1007/s11657-014-0187-y
Milovanovic P, Rakocevic Z, Djonic D, Zivkovic V, Hahn M, Nikolic S, Amling M, Busse B, Djuric M (2014) Nano-structural, compositional and micro-architectural signs of cortical bone fragility at the superolateral femoral neck in elderly hip fracture patients vs. healthy aged controls. Exp Gerontol 55:19–28. https://doi.org/10.1016/j.exger.2014.03.001
Chen H, Zhou X, Fujita H, Onozuka M, Kubo KY (2013) Age-related changes in trabecular and cortical bone microstructure. Int J Endocrinol 2013:213234–213239. https://doi.org/10.1155/2013/213234
Funding
This work was supported by the Ministry of Education and Science of the Republic of Serbia [grant number 45005].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amandments or comparable ethical standards. For this type of study, formal consent of study participant could not be provided.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jadzic, J., Cvetkovic, D., Milovanovic, P. et al. The micro-structural analysis of lumbar vertebrae in alcoholic liver cirrhosis. Osteoporos Int 31, 2209–2217 (2020). https://doi.org/10.1007/s00198-020-05509-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-020-05509-7