Abstract
Estrogens and progestogens influence the bone. The major physiological effect of estrogen is the inhibition of bone resorption whereas progestogens exert activity through binding to specific progesterone receptors. New estrogen-free contraceptive and its possible implication on bone turnover are discussed in this review. Insufficient bone acquisition during development and/or accelerated bone loss after attainment of peak bone mass (PBM) are 2 processes that may predispose to fragility fractures in later life. The relative importance of bone acquisition during growth versus bone loss during adulthood for fracture risk has been explored by examining the variability of areal bone mineral density (BMD) (aBMD) values in relation to age. Bone mass acquired at the end of the growth period appears to be more important than bone loss occurring during adult life. The major physiological effect of estrogen is the inhibition of bone resorption. When estrogen transcription possesses binds to the receptors, various genes are activated, and a variety modified. Interleukin 6 (IL-6) stimulates bone resorption, and estrogen blocks osteoblast synthesis of IL-6. Estrogen may also antagonize the IL-6 receptors. Additionally, estrogen inhibits bone resorption by inducing small but cumulative changes in multiple estrogen-dependent regulatory factors including TNF-α and the OPG/RANKL/RANK system. Review on existing data including information about new estrogen-free contraceptives. All progestins exert activity through binding to specific progesterone receptors; hereby, three different groups of progestins exist: pregnanes, gonanes, and estranges. Progestins also comprise specific glucocorticoid, androgen, or mineralocorticoid receptor interactions. Anabolic action of a progestogen may be affected via androgenic, anti-androgenic, or synadrogenic activity. The C 19 nortestosterone class of progestogens is known to bind with more affinity to androgen receptors than the C21 progestins. This article reviews the effect of estrogens and progestogens on bone and presents new data of the currently approved drospirenone-only pill. The use of progestin-only contraceptives leading to an estradiol level between 30 and 50 pg/ml does not seem to lead to an accelerate bone loss.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoporosis is characterized by decreased bone mass and microarchitectural deterioration of the bone, leading to increased risk of fragility fracture (Kanis et al. [1]). The prevalence of osteoporosis increases with age and the burden of osteoporosis is expected to increase with aging populations. Hereby, the number of individuals at high risk of fragility fractures has been estimated to increase twofold from 158 million in 2010 to 319 million in 2040 (Kanis et al. [2]). Osteoporosis is a major public health problem, with an estimated 3.5 million fragility fractures sustained in 2010, resulting in a cost of approximately EUR 35 billion (Hernlund et al. [3]). In the absence of clear data between bone fracture and the influence of female steroidal hormones on this etiology, the following review will focus on the development of bone mineral density and female sexual hormones.
Bone and estrogen
Bone development
Although osteoporosis-related fracture typically occurs at higher age, one cornerstone may be laid as early as puberty, at time of bone acquisition. Bonjour et al. [4] have recently reviewed the topic of bone development during puberty. They start by quoting Professor Charles Dent who coined the aphorism, “Senile osteoporosis is a pediatric disease,” the concept that fracture risk later in life is the result of poor bone development during youth.
Insufficient bone acquisition during development and/or accelerated bone loss after attainment of peak bone mass (PBM) are, theoretically, the 2 processes that predispose to fragility fractures in later life. The relative importance of bone acquisition during growth versus bone loss during adulthood for fracture risk has been explored by examining the variability of areal bone mineral density (aBMD) values in relation to age. Bone mass acquired at the end of the growth period appears to be more important than bone loss occurring during adult life. A model using several variables indicated that an increase in PBM of 10% alters the onset of osteoporosis by 13 years. In comparison, a 10% increase in the age of menopause or a 10% reduction in age-related (non-menopausal) bone loss delays the onset of osteoporosis by only 2 years. Epidemiological studies suggest that a 10% increase (about 1 SD) in PBM might then reduce the risk of fracture by 50% in women after the menopause.
During puberty, the rate of bone formation at the spine and hip increases by approximately fivefold. During growth, the increase in bone mass is mainly due to an increase in bone size with very little change in bone density. Accelerated change in height does not correlate with accelerated increase in mass and an asynchrony between areal and volumetric bone mineral density. In apparently healthy young women who had a later onset of puberty were found to have low trabecular vBMD and thickness in the distal radius, findings were associated with reduced bone strength and increased fracture risk during growth. Later puberty is associated with increased incidence of fracture during childhood and adolescence [5]. Cadogan et al. [6] sustain these facts. Levels of endogenous estradiol during normal bone development are in the range of 100–500 pmol/L, peaking at 15–30 months after menarche. Seeman [7] reported that independent of estradiol values, there is no one cause of bone fragility; genetic and environmental factors play a part in development of smaller bones, fewer or thinner trabeculae, and thin cortices, all of which result in low peak bone mineral density.
Estrogen and bone
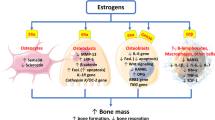
The major physiological effect of estrogen is the inhibition of bone resorption. When estrogen transcription possesses binds to the receptors, various genes are activated, and a variety modified. Interleukin 6 (IL-6) stimulates bone resorption, and estrogen blocks osteoblast synthesis of IL-6. Estrogen may also antagonize the interleukin 6 receptors. Additionally, estrogen inhibits bone resorption by inducing small but cumulative changes in multiple estrogen-dependent regulatory factors including TNF-α and the OPG/RANKL/RANK system (Riggs [8]).
Growth hormone (GH)/insulin-like growth factor 1 (IGF-1) axis also has a critical role in pubertal bone growth. There is an increase in GH and IGF-1 levels during puberty, and it is thought that sex steroids induce higher GH/IGF-1 action during growth. Recent studies indicate that estrogen increases GH secretion in boys and girls, with the effect in boys being mediated via estrogen produced by aromatase activity on testosterone, not by testosterone itself. Estrogen is also responsible for epiphyseal fusion in young men and women.
Cadogan et al. [6] have shown that increases in serum estradiol levels precede menarche and are associated with slowing of growth velocity and a decrease in bone turnover markers. IGF-I levels continue to increase, despite the deceleration in height velocity. The maximum gain in bone mineral content occurs at menarche and subsequently serum PTH levels decline. These data were obtained in healthy girls entering the study at ages 11 to 12 years, with 18 months of follow-up. The fact that bone turnover markers correlate with height velocity and not with bone gain suggests that bone turnover markers are likely to reflect statuary growth rather than bone mineral accrual and may not be the best measure of bone “health” when evaluating teenagers.
Lloyd et al. [9] reported that 12-year-old adolescents had reached 90% of adult height and attained 83% of total body bone mineral density (TBBMD) yet reached only 68% of adult weight and 58% of total body bone mineral content (TBBMC). This suggests that the schedule and mediators for TBBMD and TBBMC diverge.
While there is a broad consensus that in women, 90% of peak bone mass is determined by age 18, studies with extended longitudinal time spans have suggested that bone maturation may be a much more prolonged process. Berger et al. [10] reported that lumbar spine PBM (1.046 ± 0.123 g/cm2) occurred at ages 33 to 40 years in women and at 19 to 33 years in men (1.066 ± 0.129 g/cm2). Total hip PBM (0.981 ± 0.122 g/cm2) occurred at ages 16 to 19 years in women and 19 to 21 years in men (1.093 ± 0.169 g/cm2). This suggests that if estrogen is of predominant importance in bone development, lower estrogen levels might have adverse effects even in women over the age of 25.
Level of estrogen needed for the maintenance of bone health
The basis of the estrogen threshold hypothesis formulated by Barbieri et al. [11] implies that tissues vary in their sensitivity to estradiol and that a concentration of estradiol between 30 and 45 pg/ml is enough for preventing bone loss (see Figs. 1 and 2). Hereby, we believe that it is preferential to rather imply the existence of a range of estradiol level which has been demonstrated “bone safe” instead of an arbitrary cutoff value, which does not comprise the inter-individual variability and fluctuations over time. In postmenopausal women, Mawi et al. [12] showed that there were significant BMD differences depending on the serum estradiol levels. Women with levels > 5 pg/ml had a significant higher BMD compared with those with levels < 5 pg/ml. These values differ significantly from the proposed values of 30–45 pg/ml from Barbieri et al. In the second study in postmenopausal women, Bagur et al. [13] demonstrated women with estradiol levels > 10 pg/ml had a significant higher BMD at the lumbar spine (+ 14%), the proximal femur (+ 6%), and the total skeleton (+ 7%). In the study of osteoporotic fractures (SOF), Cummings et al. additionally underlined that endogenous estradiol levels of < 5 pg/ml versus > 5–9 pg/ml were associated with a 50–70% reduced risk of spine and hip fractures in a prospective cohort study (Cummings S et al. [14]). These estradiol levels required for preservation of BMD in postmenopausal women may not be representative for levels needed in the adolescents and in premenopausal women.
The estrogen threshold theory. Modified from Barbieri [11]
E2 levels and effects on organs. Modified from Barbieri [11]
Bone and combined oral contraceptives
Combined oral contraceptives and bone health
The most recent Cochrane Collaborative Review on combined oral contraceptives (COCs) did not find any detrimental effects of COCs on bone health. In the absence of long-term fracture data, the authors concluded: “Whether steroidal contraceptives influence fracture risk cannot be determined from existing information” [15].
A recent large-scale study including 12,970 women by Dombrowski et al. [16] investigated the effect of COC use regarding fracture incidence. Hereby, the usage of oral contraception was associated with a significantly lower risk of bone fracture (OR 0.81, 95% CI 0.74–0.90). This effect was strongest in the age groups 18–25 and 26–35 and in patients using COC and a treatment duration of more than 1 year. Additionally, the significant decreased fracture risk was even further reduced with longer duration of COC usage (Figs. 3 and 4).
Mean E2 levels of the patients with total mean levels under 51 pg/ml in the study of Duijkers et al [44] 19 cases drospirenone und 15 cases desogestrel
Mean estradiol levels of the patients receiving 4 mg drospirenone [44]
Influence of low-dose COC
There is some concern about BMD with the use of so-called ultra-low-dose COCs, those with less than 20 μg ethinyl estradiol, while those COCs with 20 to 30 μg ethinyl estradiol appear to have no adverse effect and may even protect against bone loss, at least among women 30 years of age or more (Cromer [17]). Additionally, Cibula et al. [18] investigated the effect of COCs with a dose of 15 μg versus 30 μg ethinyl estradiol and found a significant lower increase in BMD at the spine with the lower dose.
Influence of age at initiation
The effects in younger women may be due to modifications of bone architecture during the critical window, when bone formation is predominant. There are several reports regarding negative effects of COCs on bone health. Hartard et al. investigated ever versus never COC users and divided all women in 5 COC groups according to duration and time of initiation of COC. Women with > 2 years of COC use and COC initiation within 3 years after menarche are characterized by a 10% lower femoral neck areal BMD (P < 0.001), 5% lower spine areal BMD (not significant, P = 0.101), 7% lower distal tibial total BMC (P < 0.05), and 6% lower total BMC at the tibial shaft (P < 0.05) relative to never users. Ever users had lower bone mass at the femoral neck and tibial shaft, despite similar age, height, weight, BMI, hours of exercise, and calcium intake compared with never users. At the tibial shaft, COC users showed reduced total cross-sectional area, and increased cortical BMD [19].
Additionally, Almstedt et al. [20] reported a study including 98 COC users age 20–24 versus 58 age-matched controls, who had significantly higher BMD than COC users at the AP and lateral spine, femoral neck, trochanter, total hip, and whole body (P < 0.05).
Herrmann and Seibel [21] reported in a meta-analysis that combined oral contraceptives are associated with significant reductions in most if not all markers of bone turnover. Additionally, early users of COCs had significant lower Z-scores when compared with older adolescents indicating a deleterious effect of the early start of COC usage. Potential effects of these metabolic changes on bone health are currently a matter of debate. Although the available studies are not consistent in terms of bone health outcomes, the largest and most powerful investigations suggest a slight increase in fracture risk at any site.
The potential pathophysiological mechanisms by which COCs might have deleterious effects on bone health in very young adolescent as well as the effect of ultra-low dose today are not fully understood, since COCs provide adequate serum estrogens for both bone accumulation and maintenance. One hypothesis is that bone growth and mineralization processes may get uncoupled with the administration of exogenous steroids, but there is no support for this theory in animal studies of osteoporosis.
Bone and progestogens
Do progestins have significant independent effects on bone not mediated by estrogen?
All progestins exert activity through binding to specific progesterone receptors. There are three different groups of progestins: pregnanes, gonanes, and estranges. Progestins also comprise specific glucocorticoid, androgen, or mineralocorticoid receptor interactions. Anabolic action of a progestogen may be affected via androgenic, anti-androgenic, or synadrogenic activity. The C 19 nortestosterone class of progesterone is known to bind with more affinity to androgen receptors than the C21 progestins.
Animal studies by Broulik et al. [22] showed that MPA had no effect on BMD. Of various studies on progestins and bone, only studies using high doses (5 mg/day for 9 weeks) of norethindrone acetate (NETA) exerted a small positive effect on BMD. Hereby, it has been postulated by Onobrakpeya et al. [23] that this positive effect on bone is related to the 5% of NETA, which is converted to ethinyl estradiol. Additionally, norethindrone (NET) appears to have a bone-sparing effect. When compared with MPA and micronized progesterone (P4), Liu et al. [24] showed that women treated with E2 or E2 +MPA, BMD at L2–L4 increased by + 2 to + 4% over 2 years. Bone mineral density (BMD) at the spine showed a decline with MPA, P 4, and placebo treatments. With NET treatment, BMD did not change from baseline. At the femoral neck site, BMD did not change significantly for any treatment group. Bone resorption and bone formation markers decreased with E2 or E2 +MPA treatment and did not show any changes appreciably with all 3 progestin-alone treatments.
DeCherney [25] reviewed studies in postmenopausal women and studies of add-back therapy in younger women and reported that norethindrone, but not MPA, has a bone-sparing effect on cortical bone but not on trabecular bone.
Hartard et al. [26] compared the skeletal effects of DSG and LNG, both combined with 20 μg of EE, in young women, and found that LNG group did not lose vertebral aBMD, whereas women in the DSG group showed a decrease of − 1.5% at the distal radius and the tibia. LNG induced an increase in total cross-sectional area, indicating increased periosteal bone formation. Radial trabecular BMD declined by − 1.4 in the DSG group, while it remained unchanged in the LNG group. The lack consistency suggests that the treatment effects are small or that the study is perhaps too small to detect meaningful differences between groups.
Long-acting progestogens
Intrauterine device or intrauterine system
For the levonorgestrel intrauterine system (IUS) today, no mechanism indicating a negative effect on bone health is apparent. However, a case-control study reported a reduced fracture risk for ever-use and long-term use of hormonal intrauterine device (IUD) (Black et al. [27]) and (Mansour D [28]).
Contraceptive implants
For contraceptive implants, a head-to-head study of an etonogestrel implant with one rod compared with a two-rod levonorgestrel implant showed a greater decrease in bone density. However, other implant studies could not support these findings (Safarti et al., Modesto et al., Pettiti et al. [29, 30, 31]).
Beerthuizen et al. [32] could show that the use of the long-term progestogen implant Implanon (= 68 mg etonogestrel) for 3 years was not associated with a decrease of the BMD. The estradiol levels at the end of the study were 110 pg/ml in the Implanon group and 85 in the control group with no differences between both groups regarding bone mineral density.
Depot medroxyprogesterone acetate
Some hormonal contraceptives, especially injectable depot medroxyprogesterone acetate (DMPA), have been associated with changes in markers of bone formation and turnover, bone mineral density, and fracture risk.
DMPA has been shown to induce a state of hypoestrogenism that leads to a significant increase in makers of bone resorption and a decrease in BMD. One of the first studies investigating the relationship between DMPA and BMD was conducted by Cundy et al. [33, 34], with several confirmatory studies thereafter [35, 36].
Kyvernitakis et al. [37] identified 4189 women between 20 and 44 years of age and the use of DMPA for contraception with a first-time fracture diagnosis and matched them with 4189 random, healthy controls. They showed that DMPA exposure was associated with increased fracture risk and may have negative effects on bone metabolism, resulting in impaired bone mineral acquisition during adolescence and accelerated bone loss in adult life.
DMPA effect on bone regarding age at initiation
The BMD decrease related to DMPA is more pronounced in women under the age of 20 and to its prolonged use [37]. Hereby, different case-control studies comprised an increased fracture risk with long-term current DMPA use (Vestergaard et al., Meier et al., Cromer et al. [38, 39, 40].
In 2004, the US Food and Drug Administration inserted a black box warning for DMPA labeling. Yet the response from most health organizations has been less strident. WHO and the CDC Medical Eligibility Criteria rate DMPA in women aged 18 to 45 as a category 1 method (no restriction of method uses). In women aged < 18 or > 45, DMPA is rated as category 2 (the advantages of the method generally outweigh the theoretical or proven risks).
BMD and DMPA in relation to age and serum estradiol levels
Walsh et al. [35] showed that DMPA had a negative effect on the BMD. When stratifying between the age and the serum E2 levels, he reported that the young users of DPMA (18–25 years) had mean serum E2 levels 12 months after treatment of 25.6 pg/ml and a significant reduction in the BMD of the lumbar spine, total hip, and distal forearm to the control group (p < 0.05). In contrast, no statistical difference was found in the older group (age 35–45) for these parameters when compared with controls. The mean estradiol level of these women was 35.1 pg/ml after the 12 months of treatment.
DMPA has been shown to significantly decrease BMD and increase fracture risk (Cochrane Analysis; [37]). This effect may be linked to the glucocorticoid partial effect that could directly affect bone. Additionally, Miller et al. showed [41] a significant decrease in the mean serum estradiol level from 99.9 to 26.6 pg/ml (P < 0.001) which could also explain the detrimental effect on DMPA on bone health.
Oral-administered progestogens
Progestin-only oral contraceptives
In the USA, Micronor (50 μg norethindrone) was introduced in 1971 and Ovrette (0.075 mg levonorgestrel) in 1973, long before any concerns about bone health and progestin-only oral contraceptives were raised [42]. Today, a variety of progestin-only oral contraceptives (POPs) has been introduced using 75 μg levonorgestrel; 350 μg norethindrone (norethisterone); 500 μg ethynodiol diacetate; 30 μg levonorgestrel, 75 μg desogestrel, and 500 μg lynestrenol.
POPs have received little attention thus far with respect to their effect on BMD. Only one study has been identified, which included nine breastfeeding women using POPs and compared them to 19 women using barrier methods as controls. However, half of the control group (n = 10) was formula feeding. Although all women showed a significant decrease in lumbar spine BMD at 6 months postpartum, the decrease was significantly lower in POP users compared with that in non-users. This study conducted by Caird et al. [43] did not control for frequency of breastfeeding, and with the small number of women, it is not possible to draw any conclusion about any relationship between POPs and BMD.
In 2007, Thijssen [44] concluded in a review that among adolescents (menarche to 518 years), the advantages of using progestin-only contraceptives outweigh the theoretical safety concerns regarding fracture risk. The WHO statement concludes that there should be no restriction on the use of progestin-only contraceptive methods among women who are otherwise eligible to use these methods.
Different POP studies, estradiol levels, and bone mineral density
Dienogest
Stowitzki et al. [45] investigated the influence of 2 mg dienogest in women with endometriosis. Hereby, serum estradiol levels after 6 months of treatment were 68 pg/ml, with no significant decrease of BMD. In accordance with these results, Klipping et al. [46] reported mean values for estradiol of 39 pg/ml after a 6-month treatment with 2 mg dienogest. Momoeda et al. [47] investigated the effect of dienogest for 12 months on BMD. This study showed a significant decrease in BMD at the lumbar spine of − 1.7% with the greatest change in the first 24 weeks with an estradiol level between 28.8 and 37.2 pg/ml.
Desogestrel and levonorgestrel
Rice et al. [48] compared serum estradiol levels of 75 μg desogestrel per day with those of 30 μg levonorgestrel daily. After 12 months of treatment, the mean estradiol levels were 74 pg/ml for desogestrel and 147 pg/ml for levonorgestrel. Data regarding bone mineral density have never been presented as the E2 levels were in a safe range and no data of adolescents in regulatory studies have been obtained.
Drospirenone, E2 levels, and bone mineral density
Drospirenone (DRSP) is a novel synthetic progestogen, combining potent progestogenic with anti-mineralocorticoid and anti-androgenic activities. DRSP has a high affinity for progesterone receptor (PR) and mineralocorticoid receptor (MR), and low binding to the androgen receptor (AR) like progesterone. Unlike progesterone, drospirenone has low binding to glucocorticoid receptor (GR). Neither drospirenone nor progesterone binds to the estrogen receptor (ER) (Fuhrmann et al. [49]).
A study with 64 volunteers (Duijkers et al. [50]) showed that the values of estradiol at day 24 of the second cycle were below 51 pg/ml, which implies that a treatment with drospirenone had no impact in decreasing the estradiol levels below treatment initiation. The difference of estradiol levels versus women on desogestrel was statistically not significant. With this recommended dosing regimen (24 + 4), the ovary seems to secret enough endogenous estradiol for the maintenance of bone health.
The drospirenone values at day 3 of the first cycle were 36.7 pg/ml for the group with a total mean value under 51 pg/ml and at day 27 of the second cycle 49.2 pg/ml. This implies that in accordance with the window of opportunity hypothesis, no reduction of estradiol levels could be described due to the application of 4 mg drospirenone over 24 days with a pause of 4 days. Consequently, no negative effect of the bone health is expected as the study endpoint values of estradiol were even higher than the baseline values (see figure 3).
Serum estradiol levels of drospirenone were equivalent to those of dienogest and significantly not different to those of desogestrel in a study by Rice et al. [51] (54.4 pg/ml) (see figure 4). Therefore, 4 mg drospirenone given in a dosing regimen of 24/4 day does not seem to suppress the E2 levels under 30 pg/ml, which is considered the cutoff value for a detrimental effect on the bone (Doran et al. [52]).
Further studies must evaluate if these hormonal values are enough for preventing bone mineral loss. A drospirenone-only pill has been recently approved by the FDA. There are no warnings regarding bone mineral density in the summary of product characteristics, but there is a statement that the product “leads to decreased estradiol serum levels and it is unknown if this may cause a clinically relevant loss of bone mineral density.” On the other site, the evaluated hormonal levels were all in the range of the early follicular phase [53].
Table 1 depicts the different progestogens and the estradiol levels after use of them. Table 2 depicts the main clinical data, hormonal values, and BMD data of the reported progestogens.
Conclusions to progestin-only contraceptives and bone health
The threshold values postulated by Barbieri support two distinct groups according to estradiol levels:
-
Group A: The use of progestin-only contraceptives leading to an estradiol level between 30 and 50 pg/ml or higher does not seem to lead to an accelerate bone loss.
-
Group B: Serum estradiol levels between 20 and 30 pg/ml as reported with the use of DMPA seem detrimental to bone health and should therefore be avoided.
All the tested progestin-only contraceptives seem to be bone safe.
Change history
07 May 2020
A Correction to this paper has been published: https://doi.org/10.1007/s00198-020-05426-9
References
Kanis JA, Brazier JE, Stevenson M, Calvert NW, Lloyd JM (2002) Treatment of established osteoporosis: a systematic review and cost-utility analysis. Health Technol Assess 6(29):1–146. https://doi.org/10.3310/hta6290
Kanis JA, McCloskey EV, Harvey NC, Johansson H, Leslie WD (2015) Intervention thresholds and the diagnosis of osteoporosis. J Bone Miner Res 30(10):1747–1753. https://doi.org/10.1002/jbmr.2531
Hernlund E, Svedbom A, Ivergård M, Compston J, Cooper C, Stenmark J, McCloskey EV, Jönsson B, Kanis JA (2013) Osteoporosis in the European Union: medical management, epidemiology and economic burden. A report prepared in collaboration with the International Osteoporosis Foundation (IOF) and the European Federation of Pharmaceutical Industry Associations (EFPIA). Arch Osteoporos 8:136. https://doi.org/10.1007/s11657-013-0136-1
Bonjour JP, Chevalley T (2014) Pubertal timing, bone acquisition, and risk of fracture throughout life. Endocr Rev 35(5):820–847. https://doi.org/10.1210/er.2014-1007
Chevalley T, Bonjour JP, van Rietbergen B, Rizzoli R, Ferrari S (2012) Fractures in healthy females followed from childhood to early adulthood are associated with later menarcheal age and with impaired bone microstructure at peak bone mass. J Clin Endocrinol Metab 97(11):4174–4181. https://doi.org/10.1210/jc.2012-2561
Cadogan J, Blumsohn A, Barker ME, Eastell R (1998) A longitudinal study of bone gain in pubertal girls: anthropometric and biochemical correlates. J Bone Miner Res 13(10):1602–1612. https://doi.org/10.1359/jbmr.1998.13.10.1602
Seeman E (2002) Pathogenesis of bone fragility in women and men. Lancet 359:1841–1850. https://doi.org/10.1016/S0140-6736(02)08706-8
Riggs BL (2000) The mechanisms of estrogen regulation of bone resorption. J Clin Investig 106(10):1203–1204. https://doi.org/10.1172/JCI11468
Lloyd T, Rollings N, Andon MB, Demers LM, Eggli DF, Kieselhorst K, Kulin H, Landis JR, Martel JK, Orr G et al (1992) Determinants of bone density in young women. I. Relationships among pubertal development, total body bone mass, and total body bone density in premenarchal females. J Clin Endocrinol Metab 75(2):383–387. https://doi.org/10.1210/jcem.75.2.1639940
Berger C, Goltzman D, Langsetmo L, Joseph L, Jackson S, Kreiger N, Tenenhouse A, Davison KS, Josse RG, Prior JC, Hanley DA, CaMos Research Group (2010) Peak bone mass from longitudinal data: implications for the prevalence, pathophysiology, and diagnosis of osteoporosis. J Bone Miner Res 25(9):1948–1957. https://doi.org/10.1002/jbmr.95
Barbieri RL (1992) Hormone treatment of endometriosis: the estrogen threshold hypothesis. Am J Obstet Gynecol 166(2):740–745. https://doi.org/10.1016/0002-9378(92)91706-G
Mawi M (2010) Serum estradiol levels and bone mineral density in postmenopausal women. Univ Med 29:90–95
Bagur A, Oliveri B, Mautalen C, Belotti M, Mastaglia S, Yankelevich D, Sayegh F, Royer M (2004) Low levels of endogenous estradiol protect bone mineral density in young postmenopausal women. Climacteric 7(2):181–188. https://doi.org/10.1080/13697130410001713788
Cummings SR, Browner WS, Bauer D, Stone K, Ensrud K, Jamal S, Ettinger B (1998) Endogenous hormones and the risk of hip and vertebral fractures among older women. Study of Osteoporotic Fractures Research Group. N Engl J Med 339(11):733–738. https://doi.org/10.1056/NEJM199809103391104
Lopez LM, Grimes DA, Schultz KF, Curtis KM, Chen M. (2014) Steroidal contraceptives: effect on bone fractures in women. Cochrane Database of System Rev (6):CD006033. https://doi.org/10.1002/14651858.CD006033.pub5
Dombrowski S, Jacob L, Hadji P, Kostev K (2017) Oral contraceptive risk- a retrospective study of 12,970 women in the UK. Osteoporos Int 28(8):2349–2355. https://doi.org/10.1007/s00198-017-4036-X
Cromer BA (2003) Bone mineral density in adolescent and young adult women on injectable or oral contraception. Curr Opin Obstet Gynecol 15(5):353–357. https://doi.org/10.1097/01.gco.0000094695.87578.57
Cibula D, Skrenkova J, Hill M, Stepan JJ (2012) Low-dose estrogen combined oral contraceptives may negatively influence physiological bone mineral density acquisition during adolescence. Eur J Endocrinol 166(6):1003–1011. https://doi.org/10.1530/EJE-11-1047
Hartard M, Kleinmond C, Wiseman M (2007) Detrimental effect of oral contraceptives on parameters of bone mass and geometry in a cohort of 248 young women. Bone. 40(2):444–450. https://doi.org/10.1016/j.bone.2006.08.001
Almstedt SH, Snow CM (2005) Oral contraceptive use in young women is associated with lower bone mineral density than that of controls. Osteoporos Int 16(12):1538–1544. https://doi.org/10.1007/s00198-005-1868-6
Herrmann M, Seibel MJ (2010) The effects of hormonal contraceptives on bone turnover markers and bone health. Clin Endocrinol 72(5):571–583. https://doi.org/10.1111/j.1365-2265.2009.03688.x
Broulík PD, Broulíková K, Nečas E (2006) Progestogens androgenic action on the bone of male castrated mice. Prague Medical Report 107(4):401–408
Onobrakpeya OA, Fall PM, Willard A, Chakravarthi P, Hansen A, Raisz LG (2001) Effect of norethindrone acetate on hormone levels and markers of bone turnover in estrogen-treated postmenopausal women. Endocr Res 27(4):473–480
Liu JH, Muse KN (2005) The effects of progestins on bone density and bone metabolism in postmenopausal women: a randomized controlled trial. Am J Obstet Gynecol 192(4):1316–1323; discussion 1323–4. https://doi.org/10.1016/j.ajog.2004.12.067
DeCherney A (1993) Physiologic and pharmacologic effects of estrogen and progestins on bone. J Reprod Med 38(12 Sup):1007–1014 Review
Hartard M, Kleinmond C, Luppa P (2006) Comparison of the skeletal effects of the progestogens desogestrel and levonorgestrel in oral contraceptive preparations in young women: controlled, open, partly randomized investigation over 13 cycles. Contraception. 74(5):365–375. https://doi.org/10.1016/j.contraception.2006.06.005
Black A, Guilbert Q, Costescu D, Dunn S, Fisher W, Kives S, Mirosh M, Norman W, Pymar H, Reid R, Roy G, Varto H, Waddington A, Wagner MS, Whelan AM, Mansouri S (2016) Canadian contraception Consensus (Part 3 of 4): Chapter 7 – Intrauterine contraception. J Obstet Gynaecol Can 38(2):182–222. https://doi.org/10.1016/j.jogc.2015.12.002
Mansour D (2012) The benefits and risks of using a levonorgestrel-releasing intrauterine system for contraception. Contraception. https://doi.org/10.1016/j.contraception.2011.08.003
Sarfati J, Marie-Christine De Vernejoul MC (2009) Impact of combined and progestogen-only contraceptives on bone mineral density. Joint Bone Spine 76(2):134–138. https://doi.org/10.1016/j.jbspin.2008.09.014
Modesto W, Dal Ava N, Monteiro I, Bahamondes L (2015) Body composition and bone mineral density in users of the etonogestrel-releasing contraceptive implant. Arch Gynecol Obstet 292(6):1387–1391. https://doi.org/10.1007/s00404-015-3784-0
Petitti DB, Piagio G, Metha S, Cravioto MC, Meirik O (2000) Steroid hormone contraception and bone mineral density: a cross-sectional study in an international population. Obstet Gynecol 96(5 - part 19):736–744. https://doi.org/10.1016/S0029-7844(00)00782-1
Beerthuizen R, van Beek A, Massai R, Mäkäräinen L, In’t Hout J, Bennink HC (2000) Bone mineral density during long-term use of the progestogen contraceptive implant Implanon compared to a non-hormonal method of contraception. Hum Reprod 15(1):118–122. https://doi.org/10.1093/humrep/15.1.118
Cundy T, Evans M, Roberts H (1991) Bone density in women receiving depot medroxyprogesterone acetate for contraception. BMJ. 303(6793):13–16. https://doi.org/10.1136/bmj.303.6793.13
Cundy T, Ames R, Horne A, Clearwater J, Roberts H, Gamble G et al (2003) A randomized controlled trial of estrogen replacement therapy in long-term users of depot medroxyprogesterone acetate. J Clin Endocrinol Metab 88(1):78–81. https://doi.org/10.1210/jc.2002-020874
Walsh JS, Eastell R, Peel NF (2008) Effects of depot medroxyprogesterone acetate on bone density and bone metabolism before and after peak bone mass: a case-control study. J Clin Endocrinol Metab 93(4):1317–1323. https://doi.org/10.1210/jc.2007-2201
Ott SM, Scholes D, Lacroix AZ, Ichikawa LE, Yoshida CK, Barlow WE (2001) Effects of contraceptive use on bone biochemical markers in young women. J Clin Endocrinol Metab 86(1):179–185. https://doi.org/10.1210/jcem.86.1.7118
Kyvernitakis I, Kostev K, Nassour T, Thomasius F, Hadji P (2017) The impact of depot medroxyprogesterone acetate on fracture risk: a case-control study from the UK. Osteoporos Int 28(1):291–297. https://doi.org/10.1007/s00198-016-3714-4
Vestergaard P, Rejnmark L, Mosekilde L (2006) Oral contraceptive use and risk of fracture. Contraception 73(6):571–576. https://doi.org/10.1016/j.contraception.2006.01.006
Meier C, Brauchli YB, Jick SS, Kraenzlin ME, Meier CR (2010) Use of depot medroxyprogesterone acetate and fracture risk. J Clin Endocrinol Metab 95(11):4909–4916. https://doi.org/10.1210/jc.2010-0032
Cromer BA, Blair JM, Mahan JD et al (1996) A prospective comparison of bone density in adolescent girls receiving depot medroxyprogesterone acetate (Depo-Provera), levonorgestrel (Norplant), or oral contraceptives. J Pediatr 129(5):671–676. https://doi.org/10.1016/S0022-3476(96)70148-8
Miller L, Patton DL, Meier A, Thwin SS, Hooton TM, David A, Eschenbach DA (2000) Depomedroxyprogesterone-induced hypoestrogenism and changes in vaginal flora and epithelium. Obstet Gynecol 96(3):431–439
ORTHO-McNEIL (1998) Ortho Micronor® tablets (noretindrone) Pharmaceutical, INC. http://www.accessdata.fda.gov/drugsatfda_docs/label/2008/016954s101lbl.pdf.
Caird LE, Reid-Thomas V, Hannan WJ et al (1994) Oral progestogen-only contraception may protect against loss of bone mass in breastfeeding women. Clin Endocrinol 41(6):739–745. https://doi.org/10.1111/j.1365-2265.1994.tb02788.x
Thijssen JH (2007) Long-term effects of progestins on bone quality and fractures. Gynecol Endocrinol 23(Sup1):45–52. https://doi.org/10.1080/09513590701584931
Strowitzki T, Marr J, Gerlinger C, Faustmann T, Seitz C (2010) Dienogest is as effective as leuprolide acetate in treating the painful symptoms of endometriosis: a 24-week, randomized, multicentre, open-label trial. Hum Reprod 25:633–641. https://doi.org/10.1093/humrep/dep469
Klipping C, Duijkers I, Remmers A, Faustmann T, Zurth C, Klein S, Schuett B (2012) Ovulation-inhibiting effects of dienogest in a randomized, dose-controlled pharmacodynamic trial of healthy women. J Clin Pharmacol 52(11):1704–1713. https://doi.org/10.1177/0091270011423664
Momoeda M, Harada T, Terakawa N, Aso T, Fukunaga M, Hagino H, Taketani Y (2009) Long-term use of dienogest for the treatment of endometriosis. J Obstet Gynaecol Res 35(6):1069–1076. https://doi.org/10.1111/j.1447-0756.2009.01076.x
Rice CF, Killick SR, Dieben T, Bennink HC (1999) A comparison of the inhibition of ovulation achieved by desogestrel 75 mg and levonorgestrel 30 mg daily. Hum Reprod 14(4):982–985. https://doi.org/10.1093/humrep/14.4.982
Fuhrmann U, Krattenmacher R, Slater EP, Fritzemeier KH (1996) The novel progestin drospirenone and its natural counterpart progesterone: biochemical profile and antiandrogenic potential. Contraception. 54(4):243–251. https://doi.org/10.1016/S0010-7824(96)00195-3
Duijkers IJM, Herger-Mahn D, Drouin D, Skouby S (2015) A randomised study comparing the effect on ovarian activity of a progestogen-only pill (POP) containing desogestrel and a new POP containing drospirenone in a 24/4 regimen. Eur J Contracept Reprod Health Care 20(6):419–427. https://doi.org/10.3109/13625187.2015.1044082
Rice C, Killick S, Hickling D, Bennink HC (1996) Ovarian activity and vaginal bleeding patterns with a desogestrel-only preparation at three different doses. Hum Reprod 11(4):737–740. https://doi.org/10.1093/oxfordjournals.humrep.a019245
Doran PM, Riggs BL, Atkinson EJ, Khosla S (2001) Effects of raloxifene, a selective estrogen receptor modulator, on bone turnover markers and serum sex steroid and lipid levels in elderly men. J Bone Miner Res 16(11):2118–2125. https://doi.org/10.1359/jbmr.2001.16.11.2118
Slynd ®: https://www.accessdata.fda.gov/drugsatfda_docs/label/2019/211367s000lbl.pdf
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Peyman Hadji had received traveling support and speaker’s fees from Amgen, Dr. Kade/Besin, Elly Lilly, Exeltis, Gedeon Richter, MEDA, MSD, Mylan, Theramex, and UCB: Enrico Colli and Pedro-Antonio Regidor are employees of Exeltis Healthcare.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Hadji, P., Colli, E. & Regidor, PA. Bone health in estrogen-free contraception. Osteoporos Int 30, 2391–2400 (2019). https://doi.org/10.1007/s00198-019-05103-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05103-6