Abstract
Summary
RANKL-OPG should be explored in DMD patients to potentially provide targeted therapy. We quantified RANKL and OPG levels in DMD patients compared with controls. RANKL, OPG, and RANKL:OPG significantly declined with age in DMD patients suggesting some bone turnover markers are difficult to assess or use as therapeutic indicators.
Introduction
Osteoporosis in Duchenne muscular dystrophy (DMD) is multi-factorial in nature with high prevalence of fractures. RANKL-OPG should be explored to potentially provide targeted therapy for these patients. We quantified RANKL, OPG, and RANKL:OPG levels in DMD patients compared with controls and analyzed the influence of age, glucocorticoid use, ambulatory status, bone density, and fracture history.
Methods
DMD patients were enrolled at CHLA. Controls were recruited from general pediatric clinic and in collaboration with samples from a previously completed study. Free soluble RANKL and OPG levels were quantified using a sandwich ELISA.
Results
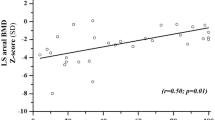
Fifty DMD patients and 50 controls were enrolled. DMD patients had a significant decline in RANKL, OPG, and RANKL:OPG with age (p = < 0.0001, p = 0.026, and p = 0.002, respectively) while healthy controls showed no significant change. RANKL trended lower in patients on glucocorticoids (p = 0.05), attributed to the significantly older age in the treatment group. RANKL and RANKL:OPG levels were significantly lower in the non-ambulatory group compared with the ambulatory group (p = 0.010 and 0.036 respectively), again likely due to their older age. There was no correlation of RANKL, OPG, or RANKL:OPG with DXA Z-score or presence of vertebral fractures.
Conclusion
There was significant decline in RANKL, OPG, and RANKL:OPG with age in DMD patients compared with controls, potentially due to disease severity or worsening osteoblastic function. This suggests some bone turnover markers may be difficult to assess or use as therapeutic indicators in DMD patients. Larger studies are needed to evaluate the role of RANKL-OPG in DMD patients to provide better targeted therapy.




Similar content being viewed by others
References
Flanigan KM (2012) The muscular dystrophies. Semin Neurol 32(3):255–263
Balaban B, Matthews DJ, Clayton GH, Carry T (2005) Corticosteroid treatment and functional improvement in Duchenne muscular dystrophy: long-term effect. Am J Phys Med Rehabil 84(11):843–850
Yilmaz O, Karaduman A, Topaloglu H (2004) Prednisolone therapy in Duchenne muscular dystrophy prolongs ambulation and prevents scoliosis. Eur J Neurol 11(8):541–544
Birnkrant DJ, Bushby K, Bann CM, Alman BA, Apkon SD, Blackwell A, Case LE, Cripe L, Hadjiyannakis S, Olson AK, Sheehan DW, Bolen J, Weber DR, Ward LM (2018) Diagnosis and management of Duchenne muscular dystrophy, part 2: respiratory, cardiac, bone health, and orthopaedic management. Lancet Neurol 17(4):347–361
Tian C, Wong B, Hornung L, Khoury J, Miller L, Bange J, Rybalsky I, Rutter M (2014) Age-specific prevalence of osteoporosis and frequency of poor bone health indices in Duchenne muscular dystrophy. Neuromuscul Disord 24(9–10):857
Boyce BF, Xing L (2007) The RANKL/RANK/OPG pathway. Curr Osteoporos Rep 5(3):98–104
Boyce BF, Xing L (2008) Functions of RANKL/RANK/OPG in bone modeling and remodeling. Arch Biochem Biophys 473(2):139–146
Boyce BF, Xing L (2007) Biology of RANK, RANKL, and osteoprotegerin. Arthritis Res Ther 9(Suppl 1):S1
Rouster-Stevens KA, Langman CB, Price HE, Seshadri R, Shore RM, Abbott K, Pachman LM (2007) RANKL:osteoprotegerin ratio and bone mineral density in children with untreated juvenile dermatomyositis. Arthritis Rheum 56(3):977–983
Lien G, Ueland T, Godang K, Selvaag AM, Forre OT, Flato B (2010) Serum levels of osteoprotegerin and receptor activator of nuclear factor -kappaB ligand in children with early juvenile idiopathic arthritis: a 2-year prospective controlled study. Pediatr Rheumatol Online J 8:30
Tsentidis C, Gourgiotis D, Kossiva L, Doulgeraki A, Marmarinos A, Galli-Tsinopoulou A, Karavanaki K (2016) Higher levels of s-RANKL and osteoprotegerin in children and adolescents with type 1 diabetes mellitus may indicate increased osteoclast signaling and predisposition to lower bone mass: a multivariate cross-sectional analysis. Osteoporos Int 27(4):1631–1643
Wasilewska A, Rybi-Szuminska A, Zoch-Zwierz W (2010) Serum RANKL, osteoprotegerin (OPG), and RANKL/OPG ratio in nephrotic children. Pediatr Nephrol 25(10):2067–2075
Olney RC, Permuy JW, Prickett TC, Han JC, Espiner EA (2012) Amino-terminal propeptide of C-type natriuretic peptide (NTproCNP) predicts height velocity in healthy children. Clin Endocrinol 77(3):416–422
Crabtree NJ, Arabi A, Bachrach LK, Fewtrell M, El-Hajj Fuleihan G, Kecskemethy HH, Jaworski M, Gordon CM (2014) Dual-energy X-ray absorptiometry interpretation and reporting in children and adolescents: the revised 2013 ISCD pediatric official positions. J Clin Densitom 17(2):225–242
Rufo A, Del Fattore A, Capulli M, Carvello F, De Pasquale L, Ferrari S, Pierroz D, Morandi L, De Simone M, Rucci N, Bertini E, Bianchi ML, De Benedetti F, Teti A (2011) Mechanisms inducing low bone density in Duchenne muscular dystrophy in mice and humans. J Bone Miner Res 26(8):1891–1903
Nakagaki WR, Bertran CA, Matsumura CY, Santo-Neto H, Camilli JA (2011) Mechanical, biochemical and morphometric alterations in the femur of mdx mice. Bone 48(2):372–379
Fewtrell MS (2003) Bone densitometry in children assessed by dual x ray absorptiometry: uses and pitfalls. Arch Dis Child 88(9):795–798
Funding
This study was funded by Parent Project Muscular Dystrophy, The Growth and Bone Foundation at Children’s Hospital Los Angeles, and The Skirball Fellowship Research Award at the Children’s Hospital Los Angeles.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Pisit Pitukcheewanont had research funding from Ultragenyx, Amgen, and Shire; salary from Ascendis Pharma. Anna Ryabets-Lienhard has research funding from Ultragenyx, Amgen, and Shire. The remaining authors have nothing to disclose.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee. Informed consent was obtained for all subjects.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Akhtar Ali, S., Kang, H., Olney, R. et al. Evaluating RANKL and OPG levels in patients with Duchenne muscular dystrophy. Osteoporos Int 30, 2283–2288 (2019). https://doi.org/10.1007/s00198-019-05077-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05077-5