Abstract
Summary
The benefits of pharmaceutical treatment for osteoporosis may be limited for a number of patients, as they continue to experience fractures. Alternative treatments may be considered for subjects whom remain at high risk for future fractures.
Introduction
Previous studies have investigated the effects of good adherence to anti-osteoporosis medication. However, very few studies have described why some patients experience fractures and loss of BMD despite adherence to treatment. The aim of this study was to estimate the proportion of patients at high risk for fracture despite being compliant to bisphosphonate treatment and examine which factors influence why some osteoporotic patients remain at a high risk for fracture despite being compliant to bisphosphonate treatment.
Methods
This case-control study is based on Danish national health registry data. The subjects had to have either one BMD test or a fracture prior to inclusion. “High-risk” subjects (cases) were defined as BMD t-score < =−2.5 SD, any drop in BMD from baseline or a fracture 24–36 months following inclusion.
Results
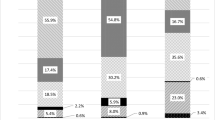
A total of 2406 subjects (66.3 % women; 33.7 % men) fulfilled the inclusion criteria, and of these, 352 (14.6 %) were identified as high risk subjects. A multiple logistical regression analysis showed that high risk subjects were more likely to have lower plasma calcium and/or vitamin D levels (OR: 2.9) and were more frequently diagnosed with hyperparathyroidism (OR: 2.6).
Conclusion
Based on Danish national health registry data, 14.6 % patients were identified as patients remaining at high risk for fracture despite being compliant to bisphosphonate treatment. Lower plasma calcium and/or vitamin D level is the greatest predictor of high risk for fracture despite persistent bisphosphonate treatment. Secondary causes of osteoporosis should be considered and alternative treatments may be advised for subjects whom remain at high risk.


Similar content being viewed by others
References
Epidemiology of fractures: Melton III LJ. Osteoporosis: etiology, diagnosis, and management. Lippincott-raven Publishers, 1995. ISBN 978–0781702751
Marshall DA, Johnell O, Wedel H (1996) Meta-analysis of how well measures of bone mineral density predict occurrence of osteoporotic fractures. BMJ 312:1254
Kanis JA, Melton LJ, Christiansen C, Johnston CC, Khaltaev N (1994) The diagnosis of osteoporosis. J Bone Miner Res 9:1137–1141
Manolagas S, Jilka R (1995) Bone marrow, cytokines, and bone remodeling—emerging insight into the pathophysiology of osteoporosis. N Engl J Med 332:305–311
Kanis J, Oden A, Johnell O, Jonsson B, De Laet C, Dawson A (2001) The burden of osteoporotic fractures : a method for setting intervention thresholds. Osteoporos Int 12:417–427
Vestergaard P, Rejnmark L, Mosekilde L (2005) Osteoporosis is markedly underdiagnosed: a nationwide study from Denmark. Osteoporos Int 16:134–141
Hansen L, Petersen KD, Eriksen SA, et al. (2015) Subsequent fracture rates in a nationwide population-based cohort study with a 10-year perspective. Osteoporos Int 26:513–519
Hansen L, Mathiesen AS, Vestergaard P, Ehlers LH, Petersen KD (2013) A health economic analysis of osteoporotic fractures: who carries the burden? Arch Osteoporos 8:126
Reginster JY, Seeman E, De Vernejoul MC, et al. (2005) Strontium ranelate reduces the risk of nonvertebral fractures in postmenopausal women with osteoporosis: treatment of peripheral osteoporosis (TROPOS) study. J Clin Endocrinol Metab 90:2816–2822
Black DM, Cummings SR, Karpf DB, et al. (1996) Randomised trial of effect of alendronate on risk of fracture in women with existing vertebral fractures. Lancet 348:1535–1541
Caro JJ, Ishak KJ, Huybrechts KF, Raggio G, Naujoks C (2004) The impact of compliance with osteoporosis therapy on fracture rates in actual practice. Osteoporos Int 15:1003–1008
Kanis JA, Cooper C, Hiligsmann M, Rabenda V, Reginster J-Y, Rizzoli R (2011) Partial adherence: a new perspective on health economic assessment in osteoporosis. Osteoporos Int 22:2565–2573
Olsen KR, Hansen C, Abrahamsen B (2013) Association between refill compliance to oral bisphosphonate treatment, incident fractures, and health care costs—an analysis using national health databases. Osteoporos Int 24:2639–2647
Mosbech J, Jørgensen J, Madsen M, Rostgaard K, Thornberg K, Poulsen T (1995) The national patient registry. Evaluation of data quality. Ugeskr Laeger 157:3741–3745
Andersen T, Madsen M, Jørgensen J, Mellemkjoer L, Olsen J (1999) The Danish National Hospital Register. A valuable source of data for modern health sciences. Danish Med Bull-J Heal Sci 46:263–268
Furu K, Wettermark B, Andersen M, Martikainen JE, Almarsdottir AB, Sørensen HT (2010) The Nordic countries as a cohort for pharmacoepidemiological research. Basic Clin Pharmacol Toxicol 106:86–94
Vestergaard P, Rejnmark L, Mosekilde L (2006) Socioeconomic aspects of fractures within universal public healthcare: a nationwide case-control study from Denmark. Scand J Public Health 34:371–377
Ryg J, Rejnmark L, Overgaard S, Brixen K, Vestergaard P (2009) Hip fracture patients at risk of second hip fracture: a nationwide population-based cohort study of 169, 145 cases during 1977–2001. J Bone Min Res 24:1299–1307
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chron Dis 40:373–383
Sundararajan V, Henderson T, Perry C, Muggivan A, Quan H, Ghali WA (2004) New ICD-10 version of the Charlson comorbidity index predicted in-hospital mortality. J Clin Epidemiol 57:1288–1294
Royston P, Altman DG (1994) Regression using fractional polynomials of continuous covariates: parsimonious parametric modelling. J R Stat Soc Ser C (Applied Stat) 43:429–467
Robertson C, Boyle P, Hsieh C-C, Macfarlane G, Maisonneuve P (1994) Some statistical considerations in the analysis of case-control studies when the exposure variables are continuous measurements. Epidemiology 5:164–170
Von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP (2008) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 61:344–349
Abrahamsen B, Rubin KH, Eiken PA, Eastell R (2013) Characteristics of patients who suffer major osteoporotic fractures despite adhering to alendronate treatment: a National Prescription registry study. Osteoporos Int 24:321–328
Siris ES, Harris ST, Rosen CJ, Barr CE (2006) Adherence to bisphosphonate therapy and fracture rates in osteoporotic women: relationship to vertebral and nonvertebral fractures from 2 US claims databases. Mayo Clin proceedings 81:1013–1022
Modi A, Tang J, Sen S, Diez-Pérez A (2015) Osteoporotic fracture rate among women with at least 1 year of adherence to osteoporosis treatment. Curr Med Res Opinion 31:767–777
Cooper C, Cole ZA, Holroyd CR, et al. (2011) Secular trends in the incidence of hip and other osteoporotic fractures. Osteoporos Int 22:1277–1288
Johnell O, Borgstrom F, Jonsson B, Kanis J (2007) Latitude, socioeconomic prosperity, mobile phones and hip fracture risk. Osteoporos Int 18:333–337
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Funding
This study was supported by a research grant from Merck/MSD Danmark ApS.
Conflicts of interest
Louise Hansen has received research grants from MSD Danmark, honoraria from Eli Lilly, and MSD Danmark. Karin Dam Petersen and Stine Aistrup Eriksen have no conflicts of interest. Fredrik Gerstoft was an employee of Merck or a subsidiary of Merck at the time of study. Peter Vestergaard received unrestricted research grants from Servier and MSD Danmark, and travel grants from Amgen, MSD, Eli Lilly, Novartis, and Servier.
Rights and permissions
About this article
Cite this article
Hansen, L., Petersen, K.D., Eriksen, S.A. et al. Subjects with osteoporosis to remain at high risk for fracture despite benefit of prior bisphosphonate treatment—a Danish case-control study. Osteoporos Int 28, 321–328 (2017). https://doi.org/10.1007/s00198-016-3720-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-016-3720-6