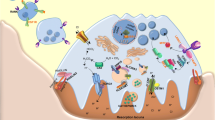
Abstract
Summary
This article reports a taxonomic classification of rare skeletal diseases based on metabolic phenotypes. It was prepared by The Skeletal Rare Diseases Working Group of the International Osteoporosis Foundation (IOF) and includes 116 OMIM phenotypes with 86 affected genes.
Introduction
Rare skeletal metabolic diseases comprise a group of diseases commonly associated with severe clinical consequences. In recent years, the description of the clinical phenotypes and radiographic features of several genetic bone disorders was paralleled by the discovery of key molecular pathways involved in the regulation of bone and mineral metabolism. Including this information in the description and classification of rare skeletal diseases may improve the recognition and management of affected patients.
Methods
IOF recognized this need and formed a Skeletal Rare Diseases Working Group (SRD-WG) of basic and clinical scientists who developed a taxonomy of rare skeletal diseases based on their metabolic pathogenesis.
Results
This taxonomy of rare genetic metabolic bone disorders (RGMBDs) comprises 116 OMIM phenotypes, with 86 affected genes related to bone and mineral homeostasis. The diseases were divided into four major groups, namely, disorders due to altered osteoclast, osteoblast, or osteocyte activity; disorders due to altered bone matrix proteins; disorders due to altered bone microenvironmental regulators; and disorders due to deranged calciotropic hormonal activity.
Conclusions
This article provides the first comprehensive taxonomy of rare metabolic skeletal diseases based on deranged metabolic activity. This classification will help in the development of common and shared diagnostic and therapeutic pathways for these patients and also in the creation of international registries of rare skeletal diseases, the first step for the development of genetic tests based on next generation sequencing and for performing large intervention trials to assess efficacy of orphan drugs.








Similar content being viewed by others
References
(2013) Report on the state of the art of rare disease activities in Europe; European Union Committee of Expert on Rare Disease. Overview of rare disease activities in Europe. Part I; pp. 1–78 http://www.eucerd.eu/upload/file/Reports/2013ReportStateofArtRDActivities.pdf
Ayme S, Schmidtke J (2007) Networking for rare diseases: a necessity for Europe. Bundesgesundheitsbl Gesundheitsforsch Gesundheitsschutz 50:1477–1483
Available from: National Organization for Rare Diseases (NORD) of the United States: www.rarediseases.org. Accessed Jan 2015
Haffner ME, Whitley J, Moses M (2002) Two decades of orphan product development. Nat Rev Drug Discov 10:821–825
Braun MM, Farag-El-Massah S, Xu K, Coté TR (2010) Emergence of orphan drugs in the United States: a quantitative assessment of the first 25 years. Nature Reviews Drug Discovery 9:519–522
For a list of rare diseases and their prevalence, please consult the Orphanet Reports Series “Prevalence of rare diseases: bibliographic data”, Orphanet Report Series, Rare Diseases collection, Number 1: Listed in alphabetical order of diseases, http://www.orpha.net/orphacom/cahiers/docs/GB/Prevalence_of_rare_diseases_by_alphabetical_list.pdf. Accessed Jan 2015
Villa S, Compagni A, Reich MR (2009) Orphan drug legislation: lessons for neglected tropical diseases. Int J Health Plann Manage 24:27–42
(2010) 5th European conference on rare diseases. European reference networks & centers of expertise for rare diseases, pp. 1–75
Available from: EUROPLAN website: www.europlanproject.eu. Accessed Jan 2015
Commission Regulation (EC) No 847/2000 of 27 April 2000; OJ L 103, 28.4.2000
Macarthur D (2011) Orphan drugs in Europe: pricing, reimbursement, funding & market access issues, Edition www.justpharmareports.com
Inventory of Community and Member States’ incentive measures to aid the research, marketing, development and availability of orphan medicinal products. Revision 2005, http://ec.europa.eu/health/files/orphanmp/doc/inventory_2006_08_en.pdf. Accessed Jan 2015
Available from: Orphabioetic foundation: www.orphanbiotec-foundation.com. Accessed Jan 2015
Commission Regulation (EC) No 847/2000 of 27 April 2000 laying down the provisions for implementation of the criteria for designation of a medicinal product as an orphan medicinal product and definitions of the concepts ‘similar medicinal product’ and ‘clinical superiority’. Off J Eur Commun 103/5-103/8
Available from: Orphanet Activity Report 2012, http://www.orpha.net/orphacom/cahiers/docs/GB/ActivityReport2012.pdf. Accessed Jan 2015
Thorat C, Xu K, Freeman SN, Bonnel RA, Joseph F, Phillips MI, Imoisili MA (2012) What the Orphan Drug Act has done lately for children with rare diseases: a 10-year analysis. Pediatrics 129:516–521
Forman J, Taruscio D, Llera VA, Barrera LA, Coté TR, Edfjall C, Gahved D, Haffner ME, Nishimura Y, Posada M, Tambuyzer E, Groft SC, Henter J-I (2012) The need for world-wide policy and actions plans for rare diseases. Acta Pediatr 101:805–807
Roldán EJA (2013) Proceedings from the VIII International Conference on Rare Diseases and Orphan Drugs (ICORD), St Petersburg (Russia). Rare J 1(suppl 1):1–48
Mäkitie O (2011) Molecular defects causing skeletal dysplasias. Camacho-Hübner C, Nilsson O, SŠvendahl L (eds) Cartilage and bone development and its disorders. Endocr Dev. Basel, Karger, vol 21, pp 78–84
(1970) International nomenclature of constitutional diseases of bones. Ann Radiol (Paris) 13(7):455–464
(1971a) A nomenclature for constitutional (intrinsic) diseases of bones. J Pediatr 78(1):177–179
(1971b) International nomenclature of constitutional bone diseases. Constitutional bone diseases without known pathogenesis. Arch Fr Pediatr 28(5):553–557
Nomenclature for constitutional (intrinsic) diseases of bones. (1971c) Pediatrics 47(2):431–344. Nomenclature for the constitutional (intrinsic) diseases of bone. Radiology. 1971d; 99(3):699–702
McKusick VA, Scott CI (1971) A nomenclature for constitutional disorders of bone. J Bone Joint Surg Am 53(5):978–986
Warman ML, Cormier-Daire V, Hall C, Krakow D, Lachman R, LeMerrer M, Mortier G, Mundlos S, Nishimura G, Rimoin DL, Robertson S, Savarirayan R, Sillence D, Spranger J, Unger S, Zabe B, Superti-Furga A (2011) Nosology and classification of genetic skeletal disorders—2010 revision. Am J Med Genet A 155A(5):943–968
Superti-Furga A, Unger S (2007) Nosology and classification of genetic skeletal disorders: 2006 revision. Am J Med Genet A 143(1):1–18
Boyce BF, Zuscik MJ, Xing L (2013) Biology of bone and cartilage. In: Thakker RV, Whyte MP, Eisman JA, Igarashi T (eds) 1 edn. Genetics of bone biology and skeletal diseases. Ch. 1 pp. 3–24
Pagani F, Francucci CM, Moro L (2005) Markers of bone turnover: biochemical and clinical perspectives. J Endocrinol Invest 28:8–13
Berndt TJ, Schiavi S, Kumar R (2005) Phosphatonins and the regulation of phosphorus homeostasis. Am J Renal Physiol 289:1170–1182
Kumar R, Riggs R (1980) Pathologic bone physiology. In: Urist MR (ed) Fundamental and clinical bone physiology. Lippincott, Philadelphia, pp 394–406
Schiavi SC, Moe OW (2002) Phosphatonins: a new class of phosphate regulating proteins. Curr Opin Nephrol Hypertens 11:423–430
Brown EM, MacLeod RJ (2001) Extracellular calcium sensing and extracellular calcium signaling. Physiol Rev 81:239–297
Alfadda TI, Saleh AM, Houllier P, Gaidel JP (2014) Calcium-sensing receptor 20 years later. Am J Physiol 307(3):C221–C231
Kumar R (1990) Vitamin D metabolism and mechanisms of calcium transport. J Am Soc Nephrol 1:30–42
Fleisch H (1980) Homeostasis of inorganic phosphate. In: Urist MR (ed) Fundamental and clinical bone physiology. Lippincott, Philadelphia, pp 268–282
Burtis WJ, Wu T, Bunch C, Wysolmerski JJ, Insogna KL, Weir EC, Broadus AE, Stewart AF (1987) Identification of a novel 17,000-dalton parathyroid hormone-like adenylate cyclase-stimulating protein from a tumor associated with humoral hypercalcemia of malignancy. J Biol Chem 262:7151–7156
Kronenberg HM (2003) Developmental regulation of the growth plate. Nature 2423:332–336
Juppner H, Silve C (2013) Genetic disorders affecting PTH/PTHrP receptor function. In: Thakker RV, Whyte MP, Eisman JA, Igarashi T (eds) Genetics of bone biology and skeletal diseases. Ch. 28, pp. 441–457
Qin C, Baba O, Butler WT (2004) Post-translational modifications of sibling proteins and their roles in osteogenesis and dentinogenesis. Crit Rev Oral Biol Med 15:126–136
Econs MJ, Drezner MK (1994) Tumor induced osteomalacia unveiling a new hormone. N Engl J Med 330:1679–1681
Quarles LD (2003) FGF23, PHEX, and MEPE regulation of phosphate homeostasis and skeletal mineralization. Am J Physiol Endocrinol Metab 285:E1–9
Boyce BF, Yao Z, Zing L (2009) Osteoclasts have multiple roles in bone in addition to bone resorption. Crit Rev Eukaryot Gene Expr 19:171–80
Fukuchi M, Fukai Y, Masuda N, Miyazaki T, Nakajima M, Sohda M, Manda R, Tsukada K, Kato H, Kuwano H (2002) High-level expression of the Smad ubiquitin ligase Smurf2 correlates with poor prognosis in patients with esophageal squamous cell carcinoma. Cancer Res 62:7162–7165
Takayanagi H (2007) Osteoimmunology: shared mechanisms and crosstalk between the immune and bone systems. Nat Rev Immunol 7:292–304
Hofbauer LC, Kühne CA, Viereck V (2004) The OPG/RANKL/RANK system in metabolic bone diseases. J Musculoskelet Neuronal Interact 4:268–75
Henriksen K, Bollerslev J, Everts V, Karsdal MA (2011) Osteoclast activity and subtypes as a function of physiology and pathology—implications for future treatments of osteoporosis. Endocrine Reviews 32:31–63
Ross PF (2013) Osteoclast biology and bone resorption. In: Primer on the metabolic bone diseases and disorders of mineral metabolism. Official publication of the American Society for Bone and Mineral Research (ASBMR) 8 edn Ch. 3 pp.25–33
Blair HC, Teitelbaum SL, Ghiselli R, Gluck S (1989) Osteoclastic bone resorption by a polarized vacuolar proton pump. Science 245:855–857
Blair HC, Teitelbaum SL, Tan HL, Koziol CM, Schlesinger PH (1991) Passive chloride permeability charge coupled to H(+)-ATPase of avian osteoclast ruffled membrane. Am J Physiol 260:C1315–C1324
Josephsen K, Praetorius J, Frische S, Gawenis LR, Kwon TH, Agre P, Nielsen S, Fejerskov O (2009) Targeted disruption of the Cl/HCO3 exchanger Ae2 results in osteopetrosis in mice. Proc Natl Acad Sci USA 106:1638–1641
Baron R, Neff L, Louvard D, Courtoy PJ (1985) Cell-mediated extracellular acidification and bone resorption: evidence for a low pH in resorbing lacunae and localization of a 100-kD lysosomal membrane protein at the osteoclast ruffled border. J Cell Biol 101:2210–2222
Frattini A, Orchard PJ, Sobacchi C, Giliani S, Abinun M, Mattsson JP, Keeling DJ, Andersson AK, Wallbrandt P, Zecca L, Notarangelo LD, Vezzoni P, Villa A (2000) Defects in TCIRG1 subunit of the vacuolar proton pump are responsible for a subset of human autosomal recessive osteopetrosis. Nat Genet 25:343–346
Karsdal MA, Henriksen K, Sørensen MG, Gram J, Schaller S, Dziegiel MH, Heegaard AM, Christophersen P, Martin TJ, Christiansen C, Bollerslev J (2005) Acidification of the osteoclastic resorption compartment provides insight into the coupling of bone formation to bone resorption. Am J Pathol 166:467–47
Henriksen K, Gram J, Schaller S, Dahl BH, Dziegiel MH, Bollerslev J, Karsdal MA (2004) Characterization of osteoclasts from patients harboring a G215R mutation in ClC-7 causing autosomal dominant osteopetrosis type II. Am J Pathol 164:1537–1545
Arnett TA (2008) Extracellular pH regulates bone cell function. J Nutr 138:415S–418S
Tolar J, Teitelbaum SL, Orchard PJ (2004) Osteopetrosis. N Engl J Med 351:2839–2849
Jansen ID, Mardones P, Lecanda F, de Vries TJ, Recalde S, Hoeben KA, Schoenmaker T, Ravesloot JH, van Borren MM, van Eijden TM, Bronckers AL, Kellokumpu S, Medina JF, Everts V, Oude Elferink RP (2009) Ae2a, b-deficient mice exhibit osteopetrosis of long bones but not of calvaria. FASEB J 23:3470–3481
Gowen M, Lazner F, Dodds R, Kapadia R, Field J, Tavaria M, Bertoncello I, Drake F, Zavarselk S, Tellis I, Hertzog P, Debouck C, Kola I (1999) Cathepsin K knockout mice develop osteopetrosis due to a deficit in matrix degradation but not demineralization. J Bone Miner Res 14:1654–1663
Calvo MS, Eyre DR, Gundberg CM (1996) Molecular basis and clinical application of biological markers of bone turnover. Endocr Rev 17:333–368
Singer FR, Eyre MD (2008) Using biochemical markers of bone turnover in clinical practice. Cleveland Clinic Journal of Medicine 75:739–750
Bergmann P, Body JJ, Boonen S, Boutsen Y, Devogelaer JP, Goemaere S, Kaufman JM, Rozenberg S, Reginster JY (2009) Evidence-based guidelines for the use of biochemical markers of bone turnover in the selection and monitoring of bisphosphonate treatment in osteoporosis: a consensus document of the Belgian Bone Club. Int J Clin Pract 63:19–26
Suwanwalaikorn S, Van Auken M, Kang MI, Alex S, Braverman LE, Baran DT (1997) Site selectivity of osteoblast gene expression response to thyroid hormone localized by in situ hybridization. Am J Physiol 272(2 Pt 1):E212–217
Kasperk C, Wergedal J, Strong D, Farley J, Wangerin K, Gropp H, Ziegler R, Baylink DJ (1995) Human bone cell phenotypes differ depending on their skeletal site of origin. J Clin Endocrinol Metab 80(8):2511–2517
Orimo H (2010) The mechanism of mineralization and the role of alkaline phosphatase in health and disease. J Nippon Med Sch 77:4–12
Mortland M, Robison R (1929) The preparation and use of the phosphatase. Biochem J 23:237–242
Seibel MJ (2005) Biochemical markers of bone turnover: part I: biochemistry and variability. Clin Biochem Rev 26:97–122
Gundberg CM, Markowitz ME, Mizruchi M, Rosen JF (1985) Osteocalcin in human serum: a circadian rhythm. J Clin Endocrinol Metab 60:736–739
Delmas PD, Wilson DM, Mann KG, Riggs BL (1983) Effect of renal function on plasma levels of bone Gla-protein. J Clin Endocrinol Metab 57:1028–1030
Bergmann P, Body JJ, Boonen S, Boutsen Y, Devogelaer JP, Goemaere S, Kaufman JM, Reginster JY, Gangji V, Members of Advisory Board on Bone Markers (2009) Evidence-based guidelines for the use of biochemical markers, bone turnover: biomarkers of bone turnover. Int J Clin Pract CME 63(1):19–26
Keen RW (2013) Sclerosing and displastic bone diseases. In: Primer on the metabolic bone diseases and disorders of mineral metabolism. 8 edn, Wiley, Ames, section VIII, pp 767–842
Franz-Odendaal TA, Hall BK, Witten PE (2006) Buried alive: how osteoblasts become osteocytes. Dev Dyn 235:176–190
Burger EH, Klein-Nulend J (1999) Mechanotransduction in bone—role of the lacuno-canalicular network. FASEB J 13(Suppl):S101–112
Li X, Liu P, Liu W, Maye P, Zhang J, Zhang Y, Hurley M, Guo C, Boskey A, Sun L, Harris SE, Rowe DW, Ke HZ, Wu D, Liu LX (2005) Dkk2 has a role in terminal osteoblast differentiation and mineralized matrix formation. Nat Genet 37:945–952
Bonewald LF, Johson ML (2008) Osteocytes, mechanosensing and Wnt signaling. Bone 42:606–615
Tatsumi S, Ishii K, Amizuka N, Li M, Kobayashi T, Kohno K, Ito M, Takeshita S, Ikeda K (2007) Targeted ablation of osteocytes induces osteoporosis with defective mechanotransduction. Cell Metabolism 5:464–475
Moriishi T, Fukuyama R, Ito M, Miyazaki T, Maeno T, Kawai Y, Komori H, Komori T (2012) Osteocyte network; a negative regulatory system for bone mass augmented by the induction of Rankl in osteoblasts and Sost in osteocytes at unloading. PLoS ONE 7(6):e401–443
Bonewald LF (2007) Osteocytes as dynamic multifunctional cells. Ann N Y Acad Sci 1116:281–290
Kneissel M (2009) The promise of sclerostin inhibition for the treatment of osteoporosis. IBMS BoneKEy 6:259–264
Dalla SL, Bonewald LF (2010) Dynamics of the transition from osteoblast to osteocyte. Ann N Y Acad Sci 1192:437–443
Guo D et al (2006) Identification of proteins involved in cytoskeletal rearrangement, anti-hypoxia and membrane channels in osteocytes over osteoblasts. J Bone Miner Res 21:S168
Gentili C, Cancedda R (2009) Cartilage and bone extracellular matrix. Curr Pharm Des 15:1334–1348
Robey PG, Boskey AL. The composition of bone. In: Primer on the bone metabolic diseases and disorders of mineral metabolism. Seventh ed. Official publication of the American Society for Bone and Mineral Research Ch. 6 pp. 32–38
Rossert J, de Crombrugghe B (1996) Type I collagen: structure, synthesis, and regulation. In: JP Bilezikian, Raisz LC, Rodan Ga (eds) Principle of bone biology. 1st edn. Ch. 10 pp. 127–142
Lian JB, Stein GS (2006) The cells of bone. In: Seibel MJ, Robins S, Bilezikian JP (eds) Dynamics of bone and cartilage metabolism. Academic, San Diego
Lee NK, Sowa H, Hinoi E, Ferron M, Ahn JD, Confavreux C, Dacquin R, Mee PJ, McKee MD, Jung DY, Zhang Z, Kim JK, Mauvais-Jarvis F, Ducy P, Karsenty G (2007) Endocrine regulation of energy metabolism by the skeleton. Cell 130:456–469
Acknowledgments
This paper was supported by the IOF.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Footnote: In the tables, biochemical markers have been indicated with abbreviations as described in the Addendum section.
ESM 1
(DOCX 63.0 KB)
Rights and permissions
About this article
Cite this article
Masi, L., Agnusdei, D., Bilezikian, J. et al. Taxonomy of rare genetic metabolic bone disorders. Osteoporos Int 26, 2529–2558 (2015). https://doi.org/10.1007/s00198-015-3188-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-015-3188-9