Abstract
Introduction and hypothesis
Stress urinary incontinence (SUI) and low back pain (LBP) are common postnatal problems. We aimed to compare the effects of stabilization exercises focusing on the pelvic floor on postnatal SUI and LBP.
Methods
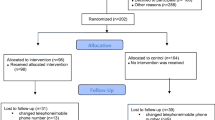
This two-arm, single-blind, parallel, randomized controlled trial was done on 80 women (mean age: 30.5, range: 20–45 years), with postnatal SUI and LBP. They were randomized into two equal control and intervention groups. The control group received no treatment while the intervention group received home-based stabilization exercises focusing on pelvic floor muscles (PFM) 3 days a week for 12 weeks, three sets a day; each set included three different types of exercise each week. Outcome measures were UI severity, assessed by ICIQ-UI-SF, low back pain functional disability, assessed by the Oswestry Disability Index (ODI), LBP severity, assessed by visual analog scale (VAS), and PFM strength and endurance, assessed by vaginal examination. Transverse abdominis (TrA) muscle strength was assessed by manometric biofeedback. All outcomes were measured directly before and after treatment.
Results
In the intervention group, PFM strength, TrA muscle strength, functional disability and pain severity were significantly improved (P < 0.05). Within-group results showed that all outcomes except pain severity (P = 0.06) had directly improved in the intervention group after treatment (P < 0.05), while in the control group only PFM strength and endurance and UI severity had improved (P < 0.05).
Conclusions
Home-based stabilization exercises focusing on the pelvic floor muscles could be effective for postnatal LBP and SUI.
Trial registration
Iranian Registry of Clinical Trials (Code: IRCT2017050618760N4).


Similar content being viewed by others
Abbreviations
- SUI:
-
Stress urinary incontinence
- LBP:
-
Low back pain
- PFM:
-
Pelvic floor muscles
- PFD:
-
Pelvic floor disorders
- ODI:
-
Oswestry Disability Index
- VAS:
-
Visual analog scale
- TrA:
-
Transverse abdominis
References
Katonis P, Kampouroglou A, Aggelopoulos A, Kakavelakis K, Lykoudis S, Makrigiannakis A, et al. Pregnancy-related low back pain. Hippokratia. 2011;15(3):205.
Ghaderi F, Asghari Jafarabadi M, Mohseni Bandpei MA. Prevalence of musculoskeletal pain and associated factors with low back pain during pregnancy. The Iranian Journal of Obstetrics, Gynecology and Infertility. 2013;15(41):9–16.
Mantle J, Haslam J, Barton S, Polden M. Physiotherapy in obstetrics and gynaecology. London: Butterworth-Heinemann; 2004.
Barr K, Griggs M, Cadby T. Lumbar stabilization: a review of core concepts and current literature, part 2. Am J Phys Med Rehabil. 2007;86(1):72–80.
Bayramoglu M, Akman M, Kilinç S, Çetin N, Yavuz N, Özker R. Isokinetic measurement of trunk muscle strength in women with chronic low back pain. Am J Phys Med Rehabil. 2001;80(9):650–5.
Danneels L, Vanderstraeten G, Cambier D, Witvrouw E, Cuyper H. CT imaging of trunk muscles in chronic low back pain patients and healthy control subjects. Eur Spine J. 2000;9(4):266–72.
Hodges P, Moseley G, Gabrielsson A, Gandevia S. Experimental muscle pain changes feed forward postural responses of the trunk muscles. Exp Brain Res. 2003;151(2):262–71.
Unsgaard-Tøndel M, Vasseljen O, Woodhouse A, Mørkved S. Exercises for women with persistent pelvic and low back pain after pregnancy. Global J Health Sci. 2016;8(9):107.
Bogaert J, Stack M, Partington S, Marceca J, Tremback-Ball A. The effects of stabilization exercise on low back pain and pelvic girdle pain in pregnant women. Ann Phys Rehabil Med. 2018;61:e157–8.
Hoyte L, Damaser M. Biomechanics of the female pelvic floor. 1st ed. United States: Academic; 2016.
Luo D, Chen L, Yu X, Ma L, Chen W, Zhou N, et al. Differences in urinary incontinence symptoms and pelvic floor structure changes during pregnancy between nulliparous and multiparous women. PeerJ. 2017;5:e3615.
Noor R, Neelam H, Bashir MS. Mode of delivery and pelvic floor disorder. Rawal Medical Journal. 2017;42(4):503–6.
Blomquist JL, Muñoz A, Carroll M, Handa VL. Association of delivery mode with pelvic floor disorders after childbirth. Jama. 2018;320(23):2438–47.
Memon HU, Handa VL. Vaginal childbirth and pelvic floor disorders. Women’s Health. 2013;9(3):265–77.
Thom DH, Rortveit G. Prevalence of postpartum urinary incontinence: a systematic review. Acta Obstet Gynecol Scand. 2010;89(12):1511–22.
Morkved S, Bo K. Effect of pelvic floor muscle training during pregnancy and after childbirth on prevention and treatment of urinary incontinence: a systematic review. Br J Sports Med. 2014;48(4):299–310.
Vermani E, Mittal R, Weeks A. Pelvic girdle pain and low back pain in pregnancy: a review. Pain Practice. 2010;10(1):60–71.
Ghaderi F, Oskouei AE. Physiotherapy for women with stress urinary incontinence: a review article. J Phys Ther Sci. 2014;26(9):1493–9.
Kim E, Kim S, Oh D. Pelvic floor muscle exercises utilizing trunk stabilization for treating postpartum urinary incontinence: randomized controlled pilot trial of supervised versus unsupervised training. Clin Rehabil. 2012;26(2):132–41.
Sapsford R. Rehabilitation of pelvic floor muscles utilizing trunk stabilization. Man Ther. 2004;9(1):3–12.
Sapsford R, Hodges P, Richardson C, Cooper D, Markwell S, Jull G. Co-activation of the abdominal and pelvic floor muscles during voluntary exercises. Neurourol Urodyn. 2001;20(1):31–42.
Ghaderi F, Mohammadi K, Amir Sasan R, Niko Kheslat S, Oskouei AE. Effects of stabilization exercises focusing on pelvic floor muscles on low back pain and urinary incontinence in women. Urology. 2016;93:50–4.
Thüroff J, Abrams P, Andersson K, Artibani W, Chapple C, Drake M, et al. EAU guidelines on urinary incontinence. Actas Urológicas Españolas (English Edition). 2011;7(35):373–88.
Maher C, Underwood M, Buchbinder R. Non-specific low back pain. Lancet. 2017;10070(389):736–47.
Asghari-Jafarabadi M, Sadeghi-Bazargani H. Randomization: techniques and software-aided implementation in medical studies. J Clin Res Gov. 2015;4(2):1–6.
Faul F, Erdfelder E, Lang A, Buchner A. G power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods. 2007;2(39):175–91.
Bijur PE, Silver W, Gallagher EJ. Reliability of the visual analog scale for measurement of acute pain. Acad Emerg Med. 2001;8(12):1153–7.
Mousavi SJ, Parnianpour M, Mehdian H, Montazeri A, Mobini B. The Oswestry disability index, the Roland-Morris disability questionnaire, and the Quebec back pain disability scale: translation and validation studies of the Iranian versions. Spine. 2006;31(14):E454–E9.
Hajebrahimi S, Nourizadeh D, Hamedani R, Pezeshki MZ. Validity and reliability of the international consultation on incontinence questionnaire-urinary incontinence short form and its correlation with urodynamic findings. Urol J. 2012;9(4):685–90.
Cynn H-S, Oh J-S, Kwon O-Y, Yi C-H. Effects of lumbar stabilization using a pressure biofeedback unit on muscle activity and lateral pelvic tilt during hip abduction in sidelying. Arch Phys Med Rehabil. 2006;87(11):1454–8.
Storheim K, Bø K, Pederstad O, Jahnsen R. Intra-tester reproducibility of pressure biofeedback in measurement of transversus abdominis function. Physiother Res Int. 2002;4(7):239–49.
Ferreira C, Barbosa P, de Oliveira SF, Antônio F, Franco M, Bø K. Inter-rater reliability study of the modified Oxford grading scale and the Peritron manometer. Physiotherapy. 2011;2(97):132–8.
Volløyhaug I, Mørkved S, Salvesen Ø, Salvesen KÅ. Assessment of pelvic floor muscle contraction with palpation, perineometry and transperineal ultrasound: a cross-sectional study. Ultrasound Obstet Gynecol. 2016;47(6):768–73.
Navarro Brazález B, Torres Lacomba M, de la Villa P, Sanchez Sanchez B, Prieto Gómez V, Asúnsolo del Barco Á, et al. The evaluation of pelvic floor muscle strength in women with pelvic floor dysfunction: a reliability and correlation study. Neurourol Urodyn. 2018;37(1):269–77.
Hayden J, Van Tulder M, Malmivaara A, Koes B. Meta-analysis: Exercice therapy for nonspecific low back pain. Ann Intern Med. 2005;142:765–75.
Liddle S, Baxter G, Gracey J. Exercice and chronic low back pain: what works? Pain. 2004;107:176–90.
França FR, Burke TN, Caffaro RR, Ramos LA, Marques AP. Effects of muscular stretching and segmental stabilization on functional disability and pain in patients with chronic low back pain: a randomized, controlled trial. J Manip Physiol Ther. 2012;35(4):279–85.
Kluge J, Hall D, Louw Q, Theron G, Grové D. Specific exercises to treat pregnancy-related low back pain in a south African population. Int J Gynecol Obstet. 2011;113(3):187–91.
Dougherty MC, Bishop KR, Abrams RM, Batich CD, Gimotty PA. The effect of exercise on the circumvaginal muscles in postpartum women. J Nurse Midwifery. 1989;34(1):8–14.
Acknowledgments
The authors thank all of the participants, the Physiotherapy Department of Tabriz University of Medical Sciences and Al-Zahra Hospital.
Author information
Authors and Affiliations
Contributions
F Ghaderi: Project development, Data Collection, Manuscript writing and editing
F Khorasani: Project development, Data collection
P Bastani: Data collection
P Sarbakhsh: Statistical Analysis
B Berghmans: Project Development, Manuscript writing and editing, English editing
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Khorasani, F., Ghaderi, F., Bastani, P. et al. The Effects of home-based stabilization exercises focusing on the pelvic floor on postnatal stress urinary incontinence and low back pain: a randomized controlled trial. Int Urogynecol J 31, 2301–2307 (2020). https://doi.org/10.1007/s00192-020-04284-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04284-7