Abstract
Introduction and hypothesis
The current study was aimed at addressing two questions: first, is any conventional vaginal prolapse repair effective in curing obstructed defecation symptoms, and second, is there evidence to suggest that a sacrocolpopexy will increase the risk of worsening or new-onset obstructed defecation symptoms?
Methods
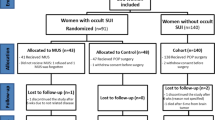
This is a sub-analysis of two major clinical trials performed by the Pelvic Floor Disorders Network: the Colpopexy and Urinary Reduction Efforts (CARE) trial and the Operations and Pelvic Muscle Training in the Management of Apical Support Loss (OPTIMAL) trial. Two-year follow-up data were included. Demographics, pelvic organ prolapse quantification examination, and symptoms were compared between first, two surgical arms in the OPTIMAL study and second, CARE and OPTIMAL datasets using Chi-squared test for categorical variables and Student’s t test or Mann–Whitney U test for continuous variables.
Results
A total of 353 subjects form the OPTIMAL study and 279 subjects from the CARE study met the inclusion criteria. Regardless of trial, obstructed defecation symptoms were present in more than half of the patients at the initial visit before the surgical intervention, and interestingly, about one third of the patients were symptomatic at the 24-month follow-up in all surgical groups.
Conclusion
The conventional vaginal prolapse surgeries, with or without posterior vaginal wall repair, improved obstructed defecation symptoms by 50%, but about 35% of patients were suffering from at least one of the aspects of obstructed defecation at the 24-month follow-up. It is also important to note that about a quarter of the patients experienced persisting or worsening of their obstructed defecation symptoms in the absence of anatomical failure.

Similar content being viewed by others
References
Bradley CS, Brown MB, Cundiff GW, Goode PS, Kenton KS, Nygaard IE, et al. Bowel symptoms in women planning surgery for pelvic organ prolapse. Am J Obstet Gynecol. 2006;195(6):1814–9.
Bradley CS, Nygaard IE, Brown MB, Gutman RE, Kenton KS, Whitehead WE, Goode PS, Wren PA, Ghetti C, Weber AM (2007) Bowel symptoms in women 1 year after sacrocolpopexy. Am J Obstet Gynecol 197(6):642.e641-8.
Rostaminia G, Abramowitch S, Chang C, Goldberg RP. Descent and hypermobility of the rectum in women with obstructed defecation symptoms. Int Urogynecol J 2019. https://doi.org/10.1007/s00192-019-03934-9.
Grimes C, Lukacz ES, Gantz MG, Warren LK, Brubaker L, Zyczynski HM, et al. What happens to the posterior compartment and bowel symptoms after sacrocolpopexy? Evaluation of 5-year outcomes from E-CARE. Female Pelvic Med Reconstruct Surg. 2014;20(5):261.
Baessler K, Schuessler B. Abdominal sacrocolpopexy and anatomy and function of the posterior compartment. Obstet Gynecol. 2001;97(5):678–84.
Pilsgaard K, Mouritsen L. Follow-up after repair of vaginal vault prolapse with abdominal colposacropexy. Acta Obstet Gynecol Scand. 1999;78(1):66–70.
Rostaminia G, Routzong M, Chang C, Goldberg RP, Abramowitch S. Motion of the vaginal apex during strain and defecation. Int Urogynecol J. 2019:1–10.
Brubaker L, Cundiff G, Fine P, Nygaard I, Richter H, Visco A, et al. A randomized trial of colpopexy and urinary reduction efforts (CARE): design and methods. Control Clin Trials. 2003;24(5):629–42.
Brubaker L, Cundiff GW, Fine P, Nygaard I, Richter HE, Visco AG, et al. Abdominal sacrocolpopexy with Burch colposuspension to reduce urinary stress incontinence. N Engl J Med. 2006;354(15):1557–66.
Nygaard I, Brubaker L, Zyczynski HM, Cundiff G, Richter H, Gantz M, et al. Long-term outcomes following abdominal sacrocolpopexy for pelvic organ prolapse. JAMA. 2013;309(19):2016–24.
Barber MD, Brubaker L, Menefee S, Norton P, Borello-France D, Varner E, et al. Operations and pelvic muscle training in the management of apical support loss (OPTIMAL) trial: design and methods. Contemp Clin Trials. 2009;30(2):178–89.
Matthew D, Barber M, Brubaker L, Burgio K. Factorial comparison of two transvaginal surgical approaches and of perioperative behavioral therapy for women with apical vaginal prolapse: the OPTIMAL randomized trial. JAMA. 2014;311(10):1023–34.
Jelovsek JE, Barber MD, Brubaker L, Norton P, Gantz M, Richter HE, et al. Effect of uterosacral ligament suspension vs sacrospinous ligament fixation with or without perioperative behavioral therapy for pelvic organ vaginal prolapse on surgical outcomes and prolapse symptoms at 5 years in the OPTIMAL randomized clinical trial. JAMA. 2018;319(15):1554–65.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rostaminia, G., Abramowitch, S., Chang, C. et al. The role of conventional pelvic floor reconstructive surgeries in obstructed defecation symptoms change: CARE and OPTIMAL trials sub-analysis of 2-year follow-up data. Int Urogynecol J 31, 1325–1334 (2020). https://doi.org/10.1007/s00192-019-04190-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-019-04190-7