Abstract
Introduction and hypothesis
Limited data exist comparing different surgical approaches in women with advanced vaginal prolapse. This study compared 2-year surgical outcomes of uterosacral ligament suspension (ULS) and sacrospinous ligament fixation (SSLF) in women with advanced prolapse (stage III–IV) and stress urinary incontinence.
Methods
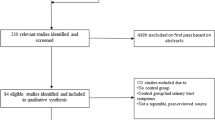
This was a secondary analysis of a multicenter 2 × 2 factorial randomized trial comparing (1) ULS versus SSLF and (2) behavioral therapy with pelvic floor muscle training versus usual care. Of 374 subjects, 117/188 (62.7%) in the ULS and 113/186 (60.7%) in the SSLF group had advanced prolapse. Two-year surgical success was defined by the absence of (1) apical descent > 1/3 into the vaginal canal, (2) anterior/posterior wall descent beyond the hymen, (3) bothersome bulge symptoms, and (4) retreatment for prolapse. Secondary outcomes included individual success outcome components, symptom severity measured by the Pelvic Organ Prolapse Distress Inventory, and adverse events. Outcomes were also compared in women with advanced prolapse versus stage II prolapse.
Results
Success did not differ between groups (ULS: 58.2% [57/117] versus SSLF: 58.5% [55/113], aOR 1.0 [0.5–1.8]). No differences were detected in individual success components (p > 0.05 for all components). Prolapse symptom severity scores improved in both interventions with no intergroup differences (p = 0.82). Serious adverse events did not differ (ULS: 19.7% versus SSLF: 16.8%, aOR 1.2 [0.6–2.4]). Success was lower in women with advanced prolapse compared with stage II (58.3% versus 73.2%, aOR 0.5 [0.3–0.9]), with no retreatment in stage II.
Conclusions
Surgical success, symptom severity, and overall serious adverse events did not differ between ULS and SSLF in women with advanced prolapse.
ClinicalTrials.gov Identifier: NCT01166373.
Similar content being viewed by others
References
FDA. Urogynecologic surgical mesh: update on the safety and effectiveness of transvaginal mesh placement for pelvic organ prolapse. Washington, DC: US Food and Drug Administration; 2011.
Boyles SH, Weber AM, Meyn L. Procedures for pelvic organ prolapse in the United States, 1979–1997. Am J Obstet Gynecol. 2003;188(1):108–15.
Montoya TI, Grande KB, Rahn DD. Apical vaginal prolapse surgery: practice patterns and factors guiding route of repair. Female Pelvic Med Reconstr Surg. 2012;18(6):315–20.
Wu JM, et al. Prevalence and trends of symptomatic pelvic floor disorders in US women. Obstet Gynecol. 2014;123(1):141–8.
Denman MA, et al. Reoperation 10 years after surgically managed pelvic organ prolapse and urinary incontinence. Am J Obstet Gynecol. 2008;198(5):555 e1–5.
Margulies RU, Rogers MA, Morgan DM. Outcomes of transvaginal uterosacral ligament suspension: systematic review and metaanalysis. Am J Obstet Gynecol. 2010;202(2):124–34.
Whiteside JL, et al. Risk factors for prolapse recurrence after vaginal repair. Am J Obstet Gynecol. 2004;191(5):1533–8.
Qatawneh A, et al. Risk factors of surgical failure following sacrospinous colpopexy for the treatment of uterovaginal prolapse. Arch Gynecol Obstet. 2013;287(6):1159–65.
Barber MD, et al. Comparison of 2 transvaginal surgical approaches and perioperative behavioral therapy for apical vaginal prolapse: the OPTIMAL randomized trial. JAMA. 2014;311(10):1023–34.
Barber MD, et al. Operations and pelvic muscle training in the management of apical support loss (OPTIMAL) trial: design and methods. Contemp Clin Trials. 2009;30(2):178–89.
Barber MD, et al. Psychometric evaluation of 2 comprehensive condition-specific quality of life instruments for women with pelvic floor disorders. Am J Obstet Gynecol. 2001;185(6):1388–95.
Barber MD, Walters MD, Bump RC. Short forms of two condition-specific quality-of-life questionnaires for women with pelvic floor disorders (PFDI-20 and PFIQ-7). Am J Obstet Gynecol. 2005;193(1):103–13.
Barber MD, et al. Defining success after surgery for pelvic organ prolapse. Obstet Gynecol. 2009;114(3):600–9.
Fialkow MF, Newton KM, Weiss NS. Incidence of recurrent pelvic organ prolapse 10 years following primary surgical management: a retrospective cohort study. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19(11):1483–7.
Morgan DM, et al. Heterogeneity in anatomic outcome of sacrospinous ligament fixation for prolapse: a systematic review. Obstet Gynecol. 2007;109(6):1424–33.
Acknowledgements
In addition to the authors, the following members of the Pelvic Floor Disorders Network participated in the Operations and Pelvic Muscle Training in the Management of Apical Support Loss (OPTIMAL) trial:
RTI International.
Klein Warren, Lauren.
Matthews, Daryl.
Shaffer, Amanda.
Terry, Tamara T.
Thornberry, Jutta.
Wallace, Dennis.
Wilson, Kevin A.
Hartmann, Katherine.
University of Alabama at Birmingham.
Ballard, Alicia.
Burge, Julie.
Burgio, Kathryn L.
Carter, Kathy.
Goode, Patricia S.
Markland, Alayne D.
Pair, Lisa S.
Parker-Autry, Candace.
Varner, R Edward.
Wilson, Tracey S.
Duke University.
Amundsen, Cindy L.
Harm-Ernandes, Ingrid.
Raynor, Mary.
Siddiqui, Nazema Y.
Weidner, Alison C.
Wu, Jennifer M.
University of California at San Diego.
Albo, Michael E.
Grimes, Cara.
Nager, Charles W.
Kaiser Permanente-Downey.
Nguyen, John N.
Kaiser Permanente-Bellflower.
Jakus-Waldman, S.
Kaiser Permanente-San Diego.
Diwadkar, Gouri.
Dyer, Keisha Y.
Hall, Lynn M.
Mackinnon, Linda M.
Menefee, Shawn A.
Tan-Kim, Jasmine.
Zazueta-Damian, Gisselle.
University of Texas-Southwestern.
Atnip, Shanna.
Moore, Elva Kelly.
Rahn, David.
Schaffer, Joseph.
University of Pittsburgh.
Borello-France, D.
Former NICHD.
Meikle, Susan F.
Cleveland Clinic.
Barber, Matthew D.
Frick, Anna.
Jelovsek, John Eric.
O’Dougherty, Betsy
Paraiso, Marie FR.
Pung, Ly.
Ridgeway, Beri M.
Williams, Cheryl.
Loyola University Chicago.
Brubaker, Linda.
Mueller, Elizabeth.
Tulke, Mary.
University of Michigan.
Casher, Yang Wang.
Chen, Yeh-Hsin.
DiFranco, Donna.
Marchant, Bev.
Spino, Cathie.
Wei, John T.
University of Utah Medical Center.
Baker, Jan.
Hsu, Yvonne.
Masters, Maria.
Orr, Amy.
Financial support
Supported by grants from the Eunice Kennedy Shriver National Institute of Child Health and Human Development (UG1 HD054241, UG1 HD041261, UG1 HD054214, UG1 HD041267, UG1 HD069010, UG1 HD069006, UG1 HD069013, U24 HD069031) and the National Institutes of Health Office of Research on Women’s Health.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflicts of interest
I Meyer, RE Whitworth, AL Smith, VW Sung, MF Ackenbom, C Wai: No conflict of interest.
ES Lukacz: Research Support: Boston Scientific, Uroplasty/Cogentix, Pfizer; Consultant: Axonics.
AG Visco: Stock ownership: NinoMed.
D Mazloomdoost: Research Grant: Boston Scientific.
MG Gantz: Research Grant: Boston Scientific.
HE Richter: Research Grant: Renovia, Allergan;
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Meyer, I., Whitworth, R.E., Lukacz, E.S. et al. Outcomes of native tissue transvaginal apical approaches in women with advanced pelvic organ prolapse and stress urinary incontinence. Int Urogynecol J 31, 2155–2164 (2020). https://doi.org/10.1007/s00192-020-04271-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-020-04271-y