Abstract
Introduction and hypothesis
The objective of this study was to identify the predictors for persistent urodynamic stress incontinence (P-USI) in women following extensive pelvic reconstructive surgery (PRS) with and without midurethral sling (MUS).
Mmethods
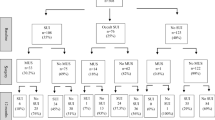
A total of 1,017 women who underwent pelvic organ prolapse (POP) surgery from January 2005 to December 2013 in our institutions were analyzed. We included 349 USI women who had extensive PRS for POP stage III or more of whom 209 underwent concomitant MUS.
Results
Of the women who underwent extensive PRS without MUS, 64.3 % (90/140) developed P-USI compared to only 10.5 % (22/209) of those who had concomitant MUS. Those with concomitant MUS and PRS alone were at higher risk of developing P-USI if they had overt USI [odds ratio (OR) 2.2, 95 % confidence interval (CI) 1.3–4.0, p = 0.014 and OR 4.7, 95 % CI 2.0–11.3, p < 0.001, respectively], maximum urethral closure pressure (MUCP) of < 60 cm H2O (OR 5.0, 95 % CI 3.0–8.1, p < 0.001 and OR 5.3, 95 % CI 2.7–10.4, p < 0.001, respectively), and functional urethral length (FUL) of < 2 cm (OR 5.4, 95 % CI 2.7–8.8, p < 0.001 and OR 3.9, 95 % CI 2.4–6.9, p < 0.001, respectively). Parity ≥ 6 (OR 3.9, 95 % CI 1.7–5.2, p < 0.001) and Prolift T (OR 3.1, 95 % CI 1.9–4, p < 0.001) posed a higher risk of P-USI in those with concomitant surgery. Perigee and Avaulta A seemed to be protective against P-USI in those without MUS.
Conclusions
Overt USI with advanced POP together with low MUCP and FUL values have a higher risk of developing P-USI. Therefore, counseling these women is worthwhile while considering the type of mesh used.

Similar content being viewed by others

References
Grody MH (1998) Urinary incontinence and concomitant prolapse. Clin Obstet Gynecol 41:777–785
Lensen EJM, Withagen MIJ, Kluivers KB et al (2013) Urinary incontinence after surgery for pelvic organ prolapse. Neurourol Urodyn 32:455–459
Fatton B (2009) Is there any evidence to advocate SUI prevention in continent women undergoing prolapse repair? An overview. Int Urogynecol J Pelvic Floor Dysfunct 20:235–245
Gordon D, Gold RS, Pauzner D, Lessing JB, Groutz A (2001) Combined genitourinary prolapse repair and prophylactic tension-free vaginal tape in women with severe prolapse and occult stress urinary incontinence: preliminary results. Urology 58:547–550
Groutz A, Gold R, Pauzner D et al (2004) Tension-free vaginal tape (TVT) for the treatment of occult stress urinary incontinence in women undergoing prolapse repair: a prospective study of 100 consecutive cases. Neurourol Urodyn 23:632–635
Rogers RG (2006) The vexing problem of hidden incontinence. N Engl J Med 354:1627–1629
Aungst MJ, Friedman EB, von Pechmann WS, Horbach NS, Welgoss JA (2009) De novo stress incontinence and pelvic muscle symptoms after transvaginal mesh repair. Am J Obstet Gynecol 201:73.e1–73.e7
Fatton B, Amblard J, Debodinance P et al (2007) Transvaginal repair of genital prolapse: preliminary results of a new tension-free vaginal mesh (Prolift technique)—a case series multicentric study. Int Urogynecol J Pelvic Floor Dysfunct 18:743–752
Brubaker L, Nygaard I, Richter HE, Visco A, Weber AM, Cundiff GW et al (2008) Two-year outcomes after sacrocolpopexy with and without Burch to prevent stress urinary incontinence. Obstet Gynecol 112:49–55
Wei JT, Nygaard I, Richter HE, Nager CW, Barber MD, Kenton K et al (2012) A midurethral sling to reduce incontinence after vaginal prolapse repair. N Engl J Med 366:2358–2367
Borstad E, Abdelnoor M, Mogimi K et al (2008) Surgery for concomitant pelvic organ prolapse and urinary stress incontinence. A multicenter prospective randomized trial to compare the results of an incontinence procedure performed at the same time of prolapse repair or 3 months after. Neurourol Urodyn 27:713
Vandenbroucke JP, von Elm E, Altman DG, Gøtzsche PC, Mulrow CD, Pocock SJ et al (2007) Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): explanation and elaboration. PLoS Med 4(10):e297. doi:10.1371/journal.pmed.0040297
Liang CC, Chang YL, Chang SD, Lo TS, Soong YK (2004) Pessary test to predict postoperative urinary incontinence in women undergoing hysterectomy for prolapse. Obstet Gynecol 104:795–800
Abrams P, Cardozo L, Fall M et al (2002) The standardization of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Neurourol Urodyn 21:167–178
Rane A, Kannan K, Barry C, Balakrishnan S, Lim Y, Corstiaans A (2008) Prospective study of the Perigee system for the management of cystoceles—medium-term follow-up. Aust N Z J Obstet Gynaecol 48:427–432
Lo TS, Ashok K (2011) Combined anterior trans-obturator mesh and sacrospinous ligament fixation in women with severe prolapse—a case series of 30 months follow-up. Int Urogynecol J 22(3):299–306. doi:10.1007/s00192-010-1266-2
Lo TS, Tan YL, Khanuengkitkong S, Dass AK, Wu PY, Cortes EFM et al (2014) Assessment of collagen coated anterior mesh through morphology and clinical outcomes in pelvic reconstructive surgery for pelvic organ prolapse. J Minim Invasive Gynecol 21:753–761
Lo TS (2010) One-year outcome of the concurrent anterior and posterior transvaginal mesh surgery for treatment of advanced urogenital prolapse: case series. J Minim Invasive Gynecol 17(4):473–479
Lo TS, Karim NB, Cortes EFM, Wu PY, Lin YH, Tan YL (2015) Comparison between Elevate anterior/apical system and Perigee system in pelvic organ prolapse surgery: clinical and sonographic outcomes. Int Urogynecol J 26:391–400
Miyazaki FS (1987) Miya Hook ligature carrier for sacrospinous ligament fixation. Obstet Gynecol 70(2):286–288
de Tayrac R, Gervaise A, Chauveaud-Lambling A, Fernandez H (2004) Combined genital prolapse repair reinforced with a polypropylene mesh and tension-free vaginal tape in women with genital prolapse and stress urinary incontinence: a retrospective case-control study with short-term follow-up. Acta Obstet Gynecol Scand 83: 950–954
Borstad E, Abdelnoor M, Staff AC, Kulseng-Hanssen S (2010) Surgical strategies for women with pelvic organ prolapsed and urinary stress incontinence. Int Urogynecol J 21:179–186
Winters JC (2008) A critical appraisal of preventive slings and prolapse surgery—what’s a urologist to do? J Urol 180:809–810
Maher CM, Feiner B, Baessler K et al (2011) Surgical management of pelvic organ prolapse in women: the updated summary version Cochrane review. Int Urogynecol J 22:1445–1457
Constantini E, Lazzeri M, Bini V, Del Zingaro M, Zucchi A, Porena M (2008) Burch colposuspension does not provide any additional benefit to pelvic organ prolapse repair in patients with urinary incontinence: a randomized surgical trial. J Urol 180:1007–1012
Sørensen S, Waechter PB, Constantinou CE, Kirkeby HJ, Jønler M, Djurhuus JC (1991) Urethral pressure and pressure variations in healthy fertile and postmenopausal women with reference to the female sex hormones. J Urol 146:1434–1440
Gad N, Duvvuru A, Burchgart B (2013) Outcome of Prolift repair in treatment of pelvic organ prolapsed and its effect on lower urinary tract symptoms: 5-year retrospective case study. J Obstet Gynaecol Res 39(1):243–249
Kawasaki A, Wu JM, Amundsen CL et al (2012) Do urodynamic parameters predict persistent postoperative stress incontinence after midurethral sling? A systematic review. Int Urogynecol J 23:813–822
Acknowledgments
Many thanks to all the colleagues for their contribution to this study.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lo, TS., Nawawi, E.A., Wu, PY. et al. Predictors for persistent urodynamic stress incontinence following extensive pelvic reconstructive surgery with and without midurethral sling. Int Urogynecol J 27, 399–406 (2016). https://doi.org/10.1007/s00192-015-2837-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-015-2837-z