Abstract
Introduction and hypothesis
The aim of the study was to identify the differential expression of estrogen-related genes that may be involved in the menopause and pelvic organ prolapse (POP) using microarray analysis.
Methods
An age, parity, and menopausal status-matched case–control study with 12 POP patients and 5 non-POP patients was carried out. The study was conducted from January to December 2010 at Yonsei University, Severance Hospital. We examined microarray gene expression profiles in uterosacral ligaments (USLs) from POP and non-POP patients. Total RNA was extracted from USL samples to generate labeled cDNA, which was hybridized to microarrays and analyzed for the expression of 44,049 genes. We identified differentially expressed genes and performed functional clustering. After clustering, we focused on transcriptional response and signal transduction gene clusters, which are associated with estrogen, and then validated the changes of gene expression levels observed with the microarray analysis using quantitative polymerase chain reaction (qPCR).
Results
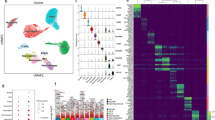
The data from the microarray analysis using more than a 1.5-fold change with p value <0.05 resulted in 143 upregulated genes and 87 downregulated genes. Of 59 genes identified to be associated with signal transduction and transcription, 4 genes were chosen for qPCR that have been classified to be associated with estrogen. We found that estrogen receptor-related receptor-α (ERRα) was downregulated and that the expression of death-associated protein kinase 2 (DAPK 2), signal-transducing adaptor protein-2 (STAP-2), and interleukin (IL)-15 were upregulated.
Conclusions
We found four differentially expressed genes by microarray analysis that may account for the way in which changes in estrogen level affect POP pathophysiology.

Similar content being viewed by others
References
Wu JM, Hundley AF, Fulton RG, Myers ER (2009) Forecasting the prevalence of pelvic floor disorders in U.S. women: 2010 to 2050. Obstet Gynecol 114(6):1278–1283
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89(4):501–506
Jelovsek JE, Maher C, Barber MD (2007) Pelvic organ prolapse. Lancet 369(9566):1027–1038
DeLancey JO (1992) Anatomic aspects of vaginal eversion after hysterectomy. Am J Obstet Gynecol 166(6 Pt 1):1717–1724, discussion 1724–1718
Moon YJ, Choi JR, Jeon MJ, Kim SK, Bai SW (2011) Alteration of elastin metabolism in women with pelvic organ prolapse. J Urol 185(5):1786–1792
Suzme R, Yalcin O, Gurdol F, Gungor F, Bilir A (2007) Connective tissue alterations in women with pelvic organ prolapse and urinary incontinence. Acta Obstet Gynecol Scand 86(7):882–888
Sze EH, Hobbs G (2012) A prospective cohort study of pelvic support changes among nulliparous, multiparous, and pre- and post-menopausal women. Eur J Obstet Gynecol Reprod Biol 160(2):232–235
Jackson S, James M, Abrams P (2002) The effect of oestradiol on vaginal collagen metabolism in postmenopausal women with genuine stress incontinence. BJOG 109(3):339–344
Hundley AF, Yuan L, Visco AG (2008) Gene expression in the rectus abdominus muscle of patients with and without pelvic organ prolapse. Am J Obstet Gynecol 198(2):220.e221–220.e227
Brizzolara SS, Killeen J, Urschitz J (2009) Gene expression profile in pelvic organ prolapse. Mol Hum Reprod 15(1):59–67
Tseng LH, Chen I, Lin YH, Chen MY, Lo TS, Lee CL (2010) Genome-based expression profiles study for the pathogenesis of pelvic organ prolapse: an array of 33 genes model. Int Urogynecol J 21(1):79–84
Hendrix SL, Cochrane BB, Nygaard IE, Handa VL, Barnabei VM, Iglesia C et al (2005) Effects of estrogen with and without progestin on urinary incontinence. JAMA 293(8):935–948
Goldstein SR, Nanavati N (2002) Adverse events that are associated with the selective estrogen receptor modulator levormeloxifene in an aborted phase III osteoporosis treatment study. Am J Obstet Gynecol 187(3):521–527
Chen H, Chung Y, Lin W, Chen W, Tsai F, Tsai C (2008) Estrogen receptor alpha polymorphism is associated with pelvic organ prolapse risk. Int Urogynecol J Pelvic Floor Dysfunct 19(8):1159–1163
Skala CE, Petry IB, Albrich S, Puhl A, Naumann G, Koelbl H (2011) The effect of genital and lower urinary tract symptoms on steroid receptor expression in women with genital prolapse. Int Urogynecol J Pelvic Floor Dysfunct 22(6):705–712
Bonnelye E, Aubin JE (2005) Estrogen receptor-related receptor alpha: a mediator of estrogen response in bone. J Clin Endocrinol Metab 90(5):3115–3121
Bonnelye E, Merdad L, Kung V, Aubin JE (2001) The orphan nuclear estrogen receptor-related receptor alpha (ERRalpha) is expressed throughout osteoblast differentiation and regulates bone formation in vitro. J Cell Biol 153(5):971–984
Verma S, Hiby SE, Loke YW, King A (2000) Human decidual natural killer cells express the receptor for and respond to the cytokine interleukin 15. Biol Reprod 62(4):959–968
Chegini N, Ma C, Roberts M, Williams RS, Ripps BA (2002) Differential expression of interleukins (IL) IL-13 and IL-15 throughout the menstrual cycle in endometrium of normal fertile women and women with recurrent spontaneous abortion. J Reprod Immunol 56(1–2):93–110
Kitaya K, Yasuda J, Yagi I, Tada Y, Fushiki S, Honjo H (2000) IL-15 expression at human endometrium and decidua. Biol Reprod 63(3):683–687
Chen B, Wen Y, Yu X, Polan ML (2005) Elastin metabolism in pelvic tissues: is it modulated by reproductive hormones? Am J Obstet Gynecol 192(5):1605–1613
Lin Y, Hupp TR, Stevens C (2010) Death-associated protein kinase (DAPK) and signal transduction: additional roles beyond cell death. FEBS J 277(1):48–57
Liu SB, Zhang N, Guo YY, Zhao R, Shi TY, Feng SF et al (2012) G-protein-coupled receptor 30 mediates rapid neuroprotective effects of estrogen via depression of NR2B-containing NMDA receptors. J Neurosci 32(14):4887–4900
Levy D, Plu-Bureau G, Decroix Y, Hugol D, Rostene W, Kimchi A et al (2004) Death-associated protein kinase loss of expression is a new marker for breast cancer prognosis. Clin Cancer Res 10(9):3124–3130
Tanaka T, Bai T, Yukawa K (2010) Death-associated protein kinase is essential for the survival of various types of uterine cancer cells. Int J Oncol 37(4):1017–1022
Takacs P, Nassiri M, Gualtieri M, Candiotti K, Medina CA (2009) Uterosacral ligament smooth muscle cell apoptosis is increased in women with uterine prolapse. Reprod Sci 16(5):447–452
Sekine Y, Ikeda O, Mizushima A, Ueno Y, Muromoto R, Yoshimura A et al (2012) STAP-2 interacts with and modulates BCR-ABL-mediated tumorigenesis. Oncogene 31:(40)4384–4396
Ikeda O, Sekine Y, Mizushima A, Nakasuji M, Miyasaka Y, Yamamoto C et al (2010) Interactions of STAP-2 with Brk and STAT3 participate in cell growth of human breast cancer cells. J Biol Chem 285(49):38093–38103
Visco AG, Yuan L (2003) Differential gene expression in pubococcygeus muscle from patients with pelvic organ prolapse. Am J Obstet Gynecol 189(1):102–112
Funding
This study was supported by the Basic Science Research Program through the National Research Foundation of Korea, funded by the Ministry of Education, Science and Technology (2010–008482).
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moon, Y.J., Bai, S.W., Jung, CY. et al. Estrogen-related genome-based expression profiling study of uterosacral ligaments in women with pelvic organ prolapse. Int Urogynecol J 24, 1961–1967 (2013). https://doi.org/10.1007/s00192-013-2124-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-013-2124-9