Abstract
Purpose
The purpose of this study was to analyze the diagnostic accuracy of magnetic resonance imaging (MRI) to detect and grade the severity of patellofemoral (PF) cartilage injuries.
Methods
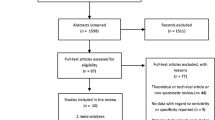
A systematic review was conducted on PubMed, EMBASE and Cochrane Library databases (up to July 1st 2022) to search for studies that reported the diagnostic accuracy of MRI to detect and grade PF cartilage injuries as compared to diagnostic arthroscopy. Risk of bias was judged using the QUADAS-2 tool. Quantitative syntheses were performed to calculate the diagnostic accuracy metric—sensitivity, specificity, positive likelihood (LR+) and negative likelihood (LR−) ratios, diagnostic odds ratio (DOR)—and presented as median with 25% and 75% percentiles. The summary receiver operating characteristic (SROC) curves were also calculated. Diagnostic accuracy metrics were calculated for all PF cartilage injuries and then sub-grouped by patellar and trochlear lesions. Diagnostic accuracy was also calculated according to the grading of cartilage injuries.
Results
Forty-five studies were included for qualitative analyses and forty studies were included for quantitative synthesis. A total of 3534 participants with a weighted mean age of 38.1 years were included. Diagnostic accuracy was generally high: sensitivity (0.8, 0.6–1.0), specificity (0.9, 0.8–1.0), LR+ (6.4, 3.1–15.3), LR− (0.3, 0.2–0.4) and DOR (21.3, 9.9–121.1). The area under the curve (AUC) of the SROC was 0.9. The diagnostic accuracy was slightly higher for patellar (sensitivity 0.8, specificity 0.8, LR+ 5.3, LR− 0.2, DOR 28.8) than for trochlear lesions (sensitivity 0.7, specificity 0.9, LR+ 5.5, LR− 0.4, DOR 14.3). The sensitivity was generally higher when grading advanced (vs. early or intermediate) cartilage injuries of the patella.
Conclusion
The MRI is able to diagnose PF cartilage injuries with reasonably high diagnostic accuracy (as compared to arthroscopy). Clinicians can rely on MRI to reliably diagnose PF cartilage injuries (with some limitations) which will play an important role in deciding for surgical or non-operative treatment.
Level of evidence
Level III.




Similar content being viewed by others
References
Adhikari K, Kumar Gupta M, Devkota K, Baral P, Koirala S (2021) Magnetic resonance imaging evaluation of patellofemoral joint. J Nepal Health Res Counc 19:122–126
Ahmad Z, Murakami AM, Engebretsen L, Jarraya M, Roemer FW, Guermazi A et al (2020) Knee cartilage damage and concomitant internal derangement on MRI in athletes competing at the Rio de Janeiro 2016 Summer Olympics. Eur J Radiol Open 7:100258
Andrade R, Nunes J, Hinckel BB, Gruskay J, Vasta S, Bastos R et al (2021) Cartilage restoration of patellofemoral lesions: a systematic review. Cartilage 13:57S-73S
Andrade R, Vasta S, Papalia R, Pereira H, Oliveira JM, Reis RL et al (2016) Prevalence of articular cartilage lesions and surgical clinical outcomes in football (Soccer) players’ knees: a systematic review. Arthroscopy 32:1466–1477
Åroøen A, Løken S, Heir S, Alvik E, Ekeland A, Granlund OG et al (2004) Articular cartilage lesions in 993 consecutive knee arthroscopies. Am J Sports Med 32:211–215
Baker H, Dickherber J, Reddy M, Rizzi A, Kahn A, Athiviraham A (2021) Diagnostic value of MRI and radiographs of the knee to identify osteochondral lesions in acute patellar instability. J Knee Surg. https://doi.org/10.1055/s-0041-1729551
Brown TR, Quinn SF (1993) Evaluation of chondromalacia of the patellofemoral compartment with axial magnetic resonance imaging. Skeletal Radiol 22:325–328
Chia L, Silva DDO, Whalan M, McKay MJ, Sullivan J, Fuller CW et al (2022) Epidemiology of gradual-onset knee injuries in team ball-sports: a systematic review with meta-analysis of prevalence, incidence, and burden by sex, sport, age, and participation level. J Sci Med Sport 25:S1440-2440
Chien A, Weaver JS, Kinne E, Omar I (2020) Magnetic resonance imaging of the knee. Polish J Radiol 85:e509–e531
Danieli MV, Guerreiro JPF, Queiroz A de O, Pereira H da R, Tagima S, Marini MG, et al. (2016) Diagnosis and classification of chondral knee injuries: comparison between magnetic resonance imaging and arthroscopy. Knee Surg Sports Traumatol Arthrosc 24:1627–1633
Disler DG, McCauley TR, Kelman CG, Fuchs MD, Ratner LM, Wirth CR et al (1996) Fat-suppressed three-dimensional spoiled gradient-echo MR imaging of hyaline cartilage defects in the knee: comparison with standard MR imaging and arthroscopy. AJR Am J Roentgenol 167:127–132
Duc SR, Koch P, Schmid MR, Horger W, Hodler J, Pfirrmann CWA (2007) Diagnosis of articular cartilage abnormalities of the knee: prospective clinical evaluation of a 3D water-excitation true FISP sequence. Radiology 243:475–482
van Eck CF, Kingston RS, Crues JV, Kharrazi FD (2017) Magnetic resonance imaging for patellofemoral chondromalacia: is there a role for T2 mapping? Orthop J Sports Med 5:2325967117740554
von Engelhardt LV, Raddatz M, Bouillon B, Spahn G, Dvid A, Haage P et al (2010) How reliable is MRI in diagnosing cartilaginous lesions in patients with first and recurrent lateral patellar dislocations? BMC Musculoskelet Disord 11:149
von Engelhardt LV, Kraft CN, Pennekamp PH, Schild HH, Schmitz A, von Falkenhausen M (2007) The evaluation of articular cartilage lesions of the knee with a 3-tesla magnet. Arthroscopy 23:496–502
Figueroa D, Calvo R, Vaisman A, Carrasco MA, Moraga C, Delgado I (2007) Knee chondral lesions: incidence and correlation between arthroscopic and magnetic resonance findings. Arthroscopy 23:312–315
Flanigan DC, Harris JD, Trinh TQ, Siston RA, Brophy RH (2010) Prevalence of chondral defects in athletes’ knees: a systematic review. Med Sci Sports Exerc 42:1795–1801
Friemert B, Oberländer Y, Schwarz W, Häberle HJ, Bähren W, Gerngroß H et al (2004) Diagnosis of chondral lesions of the knee joint: can MRI replace arthroscopy?: a prospective study. Knee Surg Sports Traumatol Arthrosc 12:58–64
Gagliardi JA, Chung EM, Chandnani VP, Kesling KL, Christensen KP, Null RN et al (1994) Detection and staging of chondromalacia patellae: relative efficacies of conventional MR imaging, MR arthrography, and CT arthrography. AJR Am J Roentgenol 163:629–636
Galea A, Giuffre B, Dimmick S, Coolican MRJ, Parker DA (2009) The accuracy of magnetic resonance imaging scanning and its influence on management decisions in knee surgery. Arthroscopy 25:473–480
Gückel C, Jundt G, Schnabel K, Gächter A (1995) Spin-echo and 3D gradient-echo imaging of the knee joint: a clinical and histopathological comparison. Eur J Radiol 21:25–33
Hadley CJ, Rao S, Ajami G, Ludwick L, Liu JX, Tjoumakaris FP et al (2021) Articular cartilage damage worsens from first-time to recurrent patellar dislocation—a longitudinal magnetic resonance imaging study. Arthrosc Sports Med Rehabil 4:e343–e347
Harman M, Ipeksoy U, Dogan A, Arslan H, Etlik O (2003) MR arthrography in chondromalacia patellae diagnosis on a low-field open magnet system. Clin Imaging 27:194–199
Harris JD, Brand JC, Cote MP, Dhawan A (2017) Research pearls: the significance of statistics and perils of pooling. Part 3: pearls and pitfalls of meta-analyses and systematic reviews. Arthroscopy 33:1594–1602
Harris JD, Brophy RH, Jia G, Price B, Knopp M, Siston RA et al (2012) Sensitivity of magnetic resonance imaging for detection of patellofemoral articular cartilage defects. Arthroscopy 28:1728–1737
Harris M, Edwards S, Rio E, Cook J, Cencini S, Hannington MC et al (2021) Nearly 40% of adolescent athletes report anterior knee pain regardless of maturation status, age, sex or sport played. Phys Ther Sport 51:29–35
Hinckel BB, Pratte EL, Baumann CA, Gowd AK, Farr J, Liu JN et al (2020) Patellofemoral cartilage restoration: a systematic review and meta-analysis of clinical outcomes. Am J Sports Med 48:1756–1772
Horga LM, Hirschmann AC, Henckel J, Fotiadou A, Di Laura A, Torlasco C et al (2020) Prevalence of abnormal findings in 230 knees of asymptomatic adults using 3.0 T MRI. Skeletal Radiol 49:1099–1107
Huegli RW, Moelleken SMC, Stork A, Bonel HM, Bredella MA, Meckel S et al (2005) MR imaging of post-traumatic articular cartilage injuries confined to the femoral trochlea: arthroscopic correlation and clinical significance. Eur J Radiol 53:90–95
Jandaghi AB, Mardani-Kivi M, Mirbolook A, Emami-Meybodi MK, Mohammadzadeh S, Farahmand M (2016) Comparison of indirect MR arthrography with conventional MRI in the diagnosis of knee pathologies in patients with knee pain. Trauma Mon 21:e20718
Jarraya M, Roemer FW, Engebretsen L, Kompel AJ, Small KM, Smith SE et al (2021) Association of markers of patellofemoral maltracking to cartilage damage and bone marrow lesions on MRI: data from the 2016 Olympic Games of Rio De Janeiro. Eur J Radiol Open 8:100381
Kakouris N, Yener N, Fong DTP (2021) A systematic review of running-related musculoskeletal injuries in runners. J Sport Health Sci 10:513–522
Kaplan DJ, Mojica ES, Ortega PF, Triana J, Strauss EJ, Jazrawi LM et al (2022) Posterior tibial tubercle measured by the sagittal TT-TG distance correlates with increased risk for patellofemoral chondral lesions. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-022-06988-3
Khoo P, Ghoshal A, Byrne D, Subramaniam R, Moran R (2019) A novel clinical test for assessing patellar cartilage changes and its correlation with magnetic resonance imaging and arthroscopy. Physiother Theory Pract 35:781–786
Kijowski R, Blankenbaker DG, Munoz del Rio A, Baer GS, Graf BK (2013) Evaluation of the articular cartilage of the knee joint: value of adding a T2 mapping sequence to a routine MR imaging protocol. Radiology 267:503–513
Kohl S, Meier S, Ahmad SS, Bonel H, Exadaktylos AK, Krismer A et al (2015) Accuracy of cartilage-specific 3-Tesla 3D-DESS magnetic resonance imaging in the diagnosis of chondral lesions: comparison with knee arthroscopy. J Orthop Surg Res 10:191
Krieger EAG, Karam FC, Soder RB, da Silva JLB (2020) Prevalence of patellar chondropathy on 3.0 T magnetic resonance imaging. Radiol Bras 53:375
LaPrade RF, Cram TR, Mitchell JJ, Geeslin AG, Lockard CA, Fitzcharles EK et al (2018) Axial-oblique versus standard axial 3-T magnetic resonance imaging for the detection of trochlear cartilage lesions: a prospective study. Orthop J Sports Med 6:2325967118801009
Lee SH, Suh JS, Cho J, Kim SJ, Kim SJ (2001) Evaluation of chondromalacia of the patella with axial inversion recovery-fast spin-echo imaging. J Magn Reson Imaging 13:412–416
Leigheb M, Guzzardi G, Barini M, Abruzzese M, Riva S, Paschè A et al (2019) Role of low field MRI in detecting knee lesions. Acta Biomed 90:116–122
Li X, Yu C, Wu H, Daniel K, Hu D, Xia L, Pan C et al (2009) Prospective comparison of 3D FIESTA versus fat-suppressed 3D SPGR MRI in evaluating knee cartilage lesions. Clin Radiol 64:1000–1008
Mandell JC, Rhodes JA, Shah N, Gaviola GC, Gomoll AH, Smith SE (2017) Routine clinical knee MR reports: comparison of diagnostic performance at 1.5 T and 3.0 T for assessment of the articular cartilage. Skeletal Radiol 46:1487–1498
Mattila VM, Weckström M, Leppänen V, Kiuru M, Pihlajamäki H (2012) Sensitivity of MRI for articular cartilage lesions of the patellae. Scand J Surg 101:56–61
McCauley TR, Kier R, Lynch KJ, Jokl P (1992) Chondromalacia patellae: diagnosis with MR imaging. AJR Am J Roentgenol 158:101–105
McInnes MDF, Moher D, Thombs BD, McGrath TA, Bossuyt PM, Clifford T et al (2018) Preferred reporting items for a systematic review and meta-analysis of diagnostic test accuracy studies the PRISMA-DTA statement. JAMA 319:388–396
Milewski MD, Smitaman E, Moukaddam H, Katz LD, Essig DA, Medvecky MJ et al (2012) Comparison of 3D vs. 2D fast spin echo imaging for evaluation of articular cartilage in the knee on a 3T system scientific research. Eur J Radiol 81:1637–1643
Mohr A (2003) The value of water-excitation 3D FLASH and fat-saturated PDw TSE MR imaging for detecting and grading articular cartilage lesions of the knee. Skeletal Radiol 32:396–402
Murphy BJ (2001) Evaluation of grades 3 and 4 chondromalacia of the knee using T2*-weighted 3D gradient-echo articular cartilage imaging. Skeletal Radiol 30:305–311
Nakanishi K, Inoue M, Harada K, Ikezoe J, Murakami T, Nakamura H et al (1992) Subluxation of the patella: evaluation of patellar articular cartilage with MR imaging. Br J Radiol 65:662–667
Ochi M, Sumen Y, Kanda T, Ikuta Y, Itoh K (1994) The diagnostic value and limitation of magnetic resonance imaging on chondral lesions in the knee joint. Arthroscopy 10:176–183
Palmowski Y, Jung T, Doering AK, Gwinner C, Schatka I, Bartek B (2021) Analysis of cartilage injury patterns and risk factors for knee joint damage in patients with primary lateral patella dislocations. PLoS ONE 16:e0258240
Pihlajamäki HK, Kuikka PI, Leppänen VV, Kiuru MJ, Mattila VM (2010) Reliability of clinical findings and magnetic resonance imaging for the diagnosis of chondromalacia patellae. J Bone Joint Surg Am 92:927–934
Potter HG, Linklater JM, Allen AA, Hannafin JA, Haas SB (1998) Magnetic resonance imaging of articular cartilage in the knee. An evaluation with use of fast-spin-echo imaging. J Bone Joint Surg Am 80:1276–1284
Recht MP, Piraino DW, Paletta GA, Schils JP, Belhobek GH (1996) Accuracy of fat-suppressed three-dimensional spoiled gradient-echo FLASH MR imaging in the detection of patellofemoral articular cartilage abnormalities. Radiology 198:209–212
Reiser MF, Bongartz G, Erlemann R, Strobel M, Pauly T, Gaebert K et al (1988) Magnetic resonance in cartilaginous lesions of the knee joint with three-dimensional gradient-echo imaging. Skeletal Radiol 17:465–471
Rose PM, Demlow TA, Szumowski J, Quinn SF (1994) Chondromalacia patellae: fat-suppressed MR imaging. Radiology 193:437–440
Ruehm S, Zanetti M, Romero J, Hodler J (1998) MRI of patellar articular cartilage: evaluation of an optimized gradient-echo sequence (3D-DESS). J Magn Reson Imaging 8:1246–1251
Russell GGQ, Johnson M, Johnston DWC, Arnett G, Swersky J (1994) Imaging studies in surgically proven chondromalacia patellae. Clin J Sport Med 4:11–13
Saragaglia D, Banihachemi JJ, Refaie R (2020) Acute instability of the patella: is magnetic resonance imaging mandatory? Int Orthop 44:2299–2303
Schmid MR, Pfirrmann CWA, Koch P, Zanetti M, Kuehn B, Hodler J (2005) Imaging of patellar cartilage with a 2D multiple-echo data image combination sequence. AJR Am J Roentgenol 184:1744–1748
Schnaiter JW, Roemer F, McKenna-Kuettner A, Patzak H-J, May MS, Janka R et al (2018) Diagnostic accuracy of an MRI protocol of the knee accelerated through parallel imaging in correlation to arthroscopy. Rofo 190:265–272
De Smet AA, Monu JUV, Fisher DR, Keene JS, Graf BK (1992) Signs of patellar chondromalacia on sagittal T2-weighted magnetic resonance imaging. Skeletal Radiol 21:103–105
Sonin AH, Pensy RA, Mulligan ME, Hatem S (2002) Grading articular cartilage of the knee using fast spin-echo proton density-weighted MR imaging without fat suppression. AJR Am J Roentgenol 179:1159–1166
Tawfik AI, Kamr WH, Taman SE (2019) Comparison of 2D fat suppressed proton density (FS-PD) and 3D (WATS-c) MRI pulse sequences in evaluation of chondromalacia patellae. Egypt J Radiol Nucl Med 50:1–6
Vallotton JA, Meuli RA, Leyvraz PF, Landry M (1995) Comparison between magnetic resonance imaging and arthroscopy in the diagnosis of patellar cartilage lesions—a prospective study. Knee Surg Sports Traumatol Arthrosc 3:157–162
Wang SF, Cheng HC, Chang CY (1999) Fat-suppressed three-dimensional fast spoiled gradient-recalled echo imaging: a modified FS 3D SPGR technique for assessment of patellofemoral joint chondromalaci. Clin Imaging 23:177–180
Whiting PF, Rutjes AWS, Westwood ME, Mallett S, Deeks JJ, Reitsma JB et al (2011) Quadas-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med 155:529–536
Yulish BS, Montanez J, Goodfellow DB, Bryan PJ, Mulopulos GP, Modic MT (1987) Chondromalacia patellae: assessment with MR imaging. Radiology 164:763–766
Funding
There is no funding source.
Author information
Authors and Affiliations
Contributions
All authors were involved both in the idealization of the systematic review and preparation of the manuscript. FXL and RA were involved in the databases searches and data extraction. FXL and AV performed the data collection and organization in coordination with RA and CV. CV and RA performed all data analysis and interpretation of results. FXL and AV judged the risk of bias of the studies included in the systematic review. JEM guided and provided advice during all steps of the development of the systematic review. All authors contributed to drafting and approving the final manuscript prior to submission to the peer-reviewed journal.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Non-applicable for this type of study.
Informed consent
Non-applicable for this type of study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xará-Leite, F., Vinha, A., Valente, C. et al. Magnetic resonance imaging is able to detect patellofemoral focal cartilage injuries: a systematic review with meta-analysis. Knee Surg Sports Traumatol Arthrosc 31, 2469–2481 (2023). https://doi.org/10.1007/s00167-022-07203-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-07203-z