Abstract
Purpose
Unicompartmental knee arthroplasty (UKA) is an effective treatment for late knee osteoarthritis (OA). Young age (< 60 years) has been associated with worse outcomes. The goal of this systematic review and meta-analysis is to study the effect of age on UKA outcomes.
Methods
The primary objective was to compare the UKA revision rate in young patients with that of old patients, using the age thresholds of 60 and 55 years. Secondary objectives were patient-reported outcome measures (PROMs) and implant design. Five databases were searched in December 2021 for original comparative studies with a minimum of 1-year follow-up. No restrictions were placed on the type of UKA prosthesis.
Results
A total of 11 observational studies with 6130 knees were included. A mean MINORS score of 19 was assigned to the review. The mean age of patients was 64 years, with average follow-up of 7.5 ± 2.98 years. There was no significant difference in revision rate, incident or PROMs between young and old patients in the analysis for each age threshold. Further sub-analysis adjusting for implant type in mobile- and fixed-bearing prostheses also showed similar results between those above and under 60 and 55 years.
Conclusion
Young age was not associated with a higher revision rate or lower functional scores. Thus, this review provides evidence that age alone is not a contraindication to UKA, but the surgical choice must be based on several elements, and this finding should be applied in context, given the binary division and heterogeneity of patients.
Level of evidence
III.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Although indications for unicompartmental knee arthroplasty (UKA) remain controversial, UKA contributed to 11% of all primary knee replacements in the UK in 2019 [5, 35]. UKA is a minimally invasive procedure that preserves normal knee kinematics and if performed well, offers excellent 15-year survivorship of over 91% [32]. Furthermore, TOPKAT, a large multicentric randomized controlled trial, has also found a similar revision rate in both UKA and TKA (0.75, 0.37–1.53; p = NS) and comparable OKS (mean difference 1.04, 95% CI –0.42 to 2.50; p = NS) at 5-year follow-up [3], advocating the use of UKA as a first choice when properly indicated.
In their landmark paper published in 1989, Kozinn and Scott [18] proposed strict criteria for UKA that deemed patients younger than 60 not ideal candidates for the procedure. In contrast, subsequent studies [25, 33] advocated performing UKA based on pathoanatomy, particularly in mobile-bearing UKA, and disregarded the age criterion as an unnecessary contraindication.
Conflicting findings from registry data and other studies exist regarding the effect of age on UKA outcomes [15, 32, 35]. There are currently no systematic reviews assessing this relationship within the UKA cohorts; therefore, such a review, which is the first to investigate all non-registry data, would help guide surgical management and inform how surgeons select those patients that are likely to benefit from UKA.
This review aims to investigate how patient’s age affects revision rate and patient-reported outcome measures (PROMs) following UKA by comparing patients older than 60 with patients younger than 60. In addition, a subgroup analysis for the cut-off age of 55 to further assess the optimal age threshold for UKA candidacy was performed. Additional analysis of how age affects fixed- and mobile-bearing prostheses was done. Thus, the null hypothesis is that there is no significant difference in revision rate and functional outcome scores between younger (< 60 years) and older (> 60 years) patients undergoing UKA.
Methods
This systematic review was conducted in line with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [24]. To ensure transparency and efficiency, a protocol registration was sought in advance on the International Prospective Register of Systematic Reviews (PROSPERO) with the registration number: CRD42021248322.
Search strategy
PubMed/Medline, Ovid, Web of Science, Google Scholar and Cochrane library databases were searched until December 2021 with the following keywords and their derivatives: “age”, “unicompartmental”, “unicondylar”, “knee”, “arthroplasty”, “replacement”, “UKA”, “UKR”, “revision”, and “outcome”—see appendices for detailed examples of database searches. Two authors independently screened the search results based on the title and/or abstract. Conflicts were resolved via a discrepancy meeting with a third, more senior author. A full-text review of articles that met the eligibility criteria was performed, and references of included articles were manually sought to ensure all relevant studies were included.
Outcomes of interest
In this review, revision is the primary outcome and is defined as “Any operation performed to add, remove or modify one or more components of a joint replacement” [35]. Functional outcome measures, including the Knee Society Score (KSS) [28] and Oxford Knee Score (OKS) [26], were used as secondary outcomes of interest to compare younger and older patients undergoing UKA.
Eligibility criteria
Studies comparing the revision rate and PROMs (KSS, OKS) between younger patients (< 60 years) and older patients (> 60 years) following UKA were included. Also, studies in which these two UKA outcomes were compared in patients younger than 55 and in patients older than 55 were included to explore further the influence of different age groups on UKA outcomes. No restrictions were placed on the type of UKA prosthesis. Exclusion criteria entailed noncomparative studies, reviews, and studies with short follow-up of less than one year, or unextractable data needed for analysis. Table 1 summarizes the complete list of inclusion and exclusion criteria.
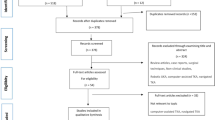
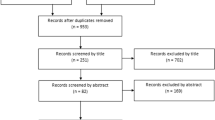
Rayyan AI website was used to manage search results [31]. Searching the databases identified 1841 papers, and after removing 361 duplicates, 1380 records were screened by title and abstracts, of which 1354 were excluded. A total of 26 papers were eligible for a full-text review. As a result, 11 studies met the eligibility criteria and were included in the qualitative and quantitative synthesis (Fig. 1).
Data extraction and items
Two independent reviewers used a pre-designed data collection sheet (Appendices) in Microsoft Excel to extract data. The extracted demographic data included the first authors’ surnames, study year, design and location, prosthesis type, mean age of patients, number of participants and knees, age groups, follow-up time, number of revisions, functional outcomes, statistical tests and conclusion.
Qualitative assessment
The risk of bias for each study was assessed using the Methodological Index for Non-Randomized Studies (MINORS) criteria [37]. Furthermore, for each study an Oxford Centre for Evidence-Based Medicine (OCEBM) [30] level of evidence (LoE) was assigned and then attributed an overall GRADE recommendation to the whole review, per the Cochrane collaboration handbook.
Quantitative analysis
The quantitative synthesis of data was performed using REVMAN 5.4 (Cochrane Collaboration, Copenhagen) review manager [36] and STATA statistical software [38]. The revision outcome was assessed using two methods; first, the raw number of revisions (incident) was calculated to compare between both age groups. Additionally, for the annual revision rate, revisions per 100 observed component years (CY) was adopted [11]; a widely accepted method in orthopedic literature and is used to overcome inconsistencies in data sources and follow-up periods across studies and ensure appropriate weighting in comparisons.
Odds ratio (OR) and 95% confidence interval (CI) for dichotomous variables (revision incident) and the means difference for continuous variables (annual revision rate and PROMS) were calculated. Mean and standard deviations were calculated using Poisson distribution. A p value less than 0.05 was considered significant. A random-effect model was utilized, and heterogeneity was quantified with the I2 statistic test. A sub-analysis based on prosthesis type (fixed or mobile-bearing) to explore the reasons for heterogeneity was performed.
Results
Study characteristics
Among the 11 included studies, 6 were used to compare how age affects UKA outcomes in patients younger than 60 and patients older than 60 years. The other five studies compared patients younger than 55 with patients older than 55 years. Moreover, three studies generated a meta-analysis of KSS functional outcomes. Five studies (45%) were retrospective, and six (55%) were prospective cohorts. There were no randomized controlled trials retrieved. A total of 6,130 knees were included, with a mean patient age of 64 ± 10.1 (Table 2).
Risk of bias and level of evidence (LoE)
Risk of bias assessment produced an average MINORS score of 19, ranging from 17 to 22 (Table 3). Based on the OCEBM criteria, six studies were level 2b, and five were level 3b (Table 2), with an overall grade B of recommendation assigned to the review. This grade indicates the consistency of findings across included studies and denotes that this piece of evidence can be recommended and generally followed in clinical practice [8].
Revision incident
The overall number of UKA revisions was 438, of which 106 were at the young age groups and 332 were in the older age groups. Analysis of studies of 60-year-olds revealed a nearly equivalent risk of revision in both age groups with an OR of 1.02 (95% CI 0.62, 1.67) and moderate heterogeneity (I2 = 61%) (Table 4). However, this was not statistically significant (p = 0.95) (Fig. 2). On the other hand, UKA revisions were 1.3 times (95% CI 0.55, 3.11) more likely in patients younger than 55 compared to those older than 55 years. This effect was not statistically significant (p = 0.55, I2 = 64%) (Fig. 3).
Revision rate
In studies of 60-year-olds (Fig. 4), the calculated annual revision rate was insignificant in patients younger than 60 years, with a mean difference of 0.05% per annum compared with that of patients older than 60 years (p = 0.87). In contrast, analysis of the studies of 55-year-olds (Fig. 5) yielded an annual revision rate 0.29% higher in patients younger than 55 years than in patients older than 55 years. Again, this result was not statistically significant (p = 0.41) with 95% CI − 0.39, 0.96.
Furthermore, subgroup analyses adjusting for the type of UKA design demonstrated no significant differences between age groups in 2878 mobile-bearing (NS) and 317 fixed-bearing (NS) prostheses and gave revision rates of 0.28% pa and 0.06% pa higher in older patients for each design, respectively (I2 > 92%). Table 5 highlights the exact component years and annual revision rate across age groups in each study.
KSS and OKS
Seven studies have reported a KSS outcome (Table 2), all of which demonstrated no statistical difference between younger and older age groups, with a trend towards better function in the young. The quantitative analysis of KSS in three studies showed a higher KSS score in the older than 60 age group, with a 6.69 mean difference in 95% CI (Fig. 6). However, this difference was insignificant and likely due to chance (p = 0.34). Five studies reported OKS(Table2), three of which were eligible for descriptive analysis [15, 20, 23] and showed comparable results with a mean score of 32.07 ± 9.9 in patients younger than 55 years and 34.03 ± 10 in patients older than 55 years at 10-year follow-up.
Discussion
In agreement with the null hypothesis, the main finding of this systematic review and meta-analysis is that the risk of UKA revision is not associated with age, as there was no significant difference observed in UKA outcomes between young patients and old patients. To demonstrate this, a comparison between patients younger than 60 and patients older than 60 was done, and in the older age group, the revision incident was equivalent, and the annual revision rate was 0.05% higher (0.5% at 10-year follow-up). Further analysis of the 55-year age threshold yielded results favouring patients older than 55: in patients younger than 55, the revision incident was 1.3 times higher, and the mean revision rate was 0.29% higher (2.9% at 10-year follow-up). However, these results were statistically insignificant (NS), which reflect comparable outcomes in both age groups.
Contrary to our and others findings, data from national registries [1] report a higher risk of revision (2.9 times) in the younger population, particularly in those aged less than 55 years. Kennedy et al. [15] attributed this observation to the variability in UKA indications adopted in registry studies versus non-registry studies. While UKA indications were mainly based on pathoanatomy [6] in database studies, registry data have little information on indications and techniques, which makes UKA candidacy assessment even more challenging [15, 33]. There is evidence that the premature performance of UKA with only partial cartilage thickness loss might be linked to the higher revision rate and poor outcomes in younger patients [9, 27]; however, if appropriately indicated in anteromedial bone-on-bone arthritis, UKA should have an equivalent if not lower revision rate than primary TKA [14, 15].
The qualitative analysis of seven studies reporting KSS and five studies reporting OKS showed no difference across various age groups. A limited analysis of three studies showed an insignificant difference (p = 0.34) of KSS score favouring patients older than 60 with a mean difference of 6.69. UKA is a minimally invasive surgical procedure characterized by the preservation of knee ligaments [29]. A substantial improvement in postoperative functional outcomes is usually seen, irrespective of age. As a result, higher PROMs are expected and likely attributed to the restoration of normal knee kinematics and leg alignment, particularly in younger patients, due to arthritic pain reduction [7, 15].
UKA outcomes can be influenced by type, design and implant properties [2]. Our review includes studies of mixed UKA designs, and we observed no statistical difference in the mobile- and fixed-bearing prosthesis revision rate between the young group and old group. This finding is supported by a recent meta-analysis of 17 studies (2612 knees) that compared mobile- and fixed-bearing UKAs and showed no difference in revision (OR = 0.96; 95% CI 0.63–1.46; p = 0.85) and radiological outcomes [41]. Another meta-analysis of 1,996 knees showed comparable survivorship and revision incident of 1.22 (95% CI: 0.83–1.80, p = 0.32) [12]. In contrast, a higher risk of polyethylene wear and aseptic loosening is evident in the fixed-bearing design [15]. In addition, a recent level III systematic review evaluated the effect of cementing in 10,736 UKAs and found that cementless UKA was associated with lower revision rate than the cemented UKA (0.45% pa vs 0.73% per annum, p < 0.001). However, this difference was insignificant (p = 0.41) in the non-Oxford UKAs with similar revision rates of cemented and cementless UKRs (0.57% pa vs 0.69% pa) [22].
As the effect of patient age at the time of operation on UKA outcomes remains highly debatable with conflicting findings and no consensus in the literature, this systematic review provides the most inclusive and highest evidence on the topic. As a result, a lower threshold for performing UKA in the younger population might be expected at the expense of TKA when indicated, regardless of the age factor. This shall delay the need for TKA in the appropriate candidates and reduce the associated health costs.
Although this review has many strengths, several limitations must be acknowledged. First, the review outcomes had moderate to substantial heterogeneity. This heterogeneity is probably related to the binary analysis of two dichotomous age categories (i.e. below and above 60 and 55 years). A better approach would be to compare more precise age groups: for example, younger than 40, 40–45, 45–50, 50–55, 55–60 years, and so on. However, due to limited studies and the inconsistent reporting of age in the literature, the exploration of only the 55-year and 60-year age cutoff points were possible. Hence, this heterogeneity was accepted based on the nature of the review and age being an inconsistent and non-binary variable. Therefore, cautious interpretation of the results of this review in clinical practice is warranted.
Considering that UKA surgery has a learning curve [21], another weakness was the inadequate reporting of such factors as surgeon/hospital volume and surgical technique. Also, matching for patient’s weight, activity level, and baseline comorbidities was not clearly stated in all studies. Cohort and retrospective studies were included, as they represented the highest available level of evidence. Future prospective studies, ideally multicentric, are needed to adjust for these confounders.
Finally, 8 out of 11 included studies used mobile-bearing UKA, with bigger sample sizes and longer follow-up, suggesting that our finding could be more representative in this implant type. However, the presence of at least three studies using fixed-bearing design enhanced the external validity and generalizability of our results.
Conclusion
This meta-analysis aimed to assess the impact of age on UKA outcomes by comparing younger age groups with older ones using 60-year and 55-year age thresholds. An equivalent revision rate between patients older than or younger than 60 and 55 years was demonstrated. Also, a comparable result between both arms of the study was observed with PROMs, namely KSS and OKS. Nevertheless, this evidence supports the finding that young age alone (below 60 years) should not be considered suboptimal in UKA.
References
AOANJRR (2020) Partial Knee Arthroplasty: Supplementary Report, in Hip, Knee & Shoulder Arthroplasty: 2020 Annual Report, AOA, Adelaide. https://aoanjrr.sahmri.com/annual-reports-2020/supplementary. Accessed 07 April 2021.
Argenson JN, Parratte S (2006) The unicompartmental knee: design and technical considerations in minimizing wear. Clin Orthop Relat Res 452:137–142
Beard DJ, Davies LJ, Cook JA, MacLennan G, Price A, Kent S et al (2019) The clinical and cost-effectiveness of total versus partial knee replacement in patients with medial compartment osteoarthritis (TOPKAT): 5-year outcomes of a randomised controlled trial. Lancet 394(10200):746–756
Collier MB, Eickmann TH, Sukezaki F, McAuley JP, Engh GA (2006) Patient, implant, and alignment factors associated with revision of medial compartment unicondylar arthroplasty. J Arthroplasty 21:108–115
Culliford D, Maskell J, Judge A, Cooper C, Prieto-Alhambra D, Arden NK (2015) Future projections of total hip and knee arthroplasty in the UK: results from the UK clinical practice research datalink. Osteoarthritis Cartilage 23(4):594–600
Goodfellow JW, Kershaw CJ, Benson MK, O’Connor JJ (1988) The Oxford Knee for unicompartmental osteoarthritis. The first 103 cases. J Bone Joint Surg Br 70(5):692–701
Gulati A, Pandit H, Jenkins C, Chau R, Dodd CA, Murray DW (2009) The effect of leg alignment on the outcome of unicompartmental knee replacement. J Bone Joint Surg Br 91:469–474
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P et al (2008) GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ 336(7650):924–926
Hamilton TW, Pandit HG, Inabathula A, Ostlere SJ, Jenkins C, Mellon SJ et al (2017) Unsatisfactory outcomes following unicompartmental knee arthroplasty in patients with partial thickness cartilage loss. Bone Joint J. 99(B4):475–482
Hamilton TW, Pandit HG, Jenkins C, Mellon SJ, Dodd CAF, Murray DW (2017) Evidence-based indications for mobile-bearing unicompartmental knee arthroplasty in a consecutive cohort of thousand knees. J Arthroplasty 32:1779–1785
Hauer G, Bernhardt GA, Hohenberger G, Leitner L, Ruckenstuhl P, Leithner A et al (2020) Similar revision rates in clinical studies and arthroplasty registers and no bias for developer publications in unicompartmental knee arthroplasty. Arch Orthop Trauma Surg 140(4):537–544
Huang F, Wu D, Chang J, Zhang C, Qin K, Liao F et al (2021) A Comparison of mobile- and fixed-bearing unicompartmental knee arthroplasties in the treatment of medial knee osteoarthritis: a systematic review and meta-analysis of 1861 patients. J Knee Surg 34:434–443
Ingale PA, Hadden WA (2013) A review of mobile bearing unicompartmental knee in patients aged 80 years or older and comparison with younger groups. J Arthroplasty 28:262-267.e262
Kennedy J, Mohammad H, Mellon S, Dodd CAF, Murray DW (2020) Age stratified, matched comparison of unicompartmental and total knee replacement. Knee 27(5):1332–1342
Kennedy JA, Matharu GS, Hamilton TW, Mellon SJ, Murray DW (2018) Age and outcomes of medial meniscal-bearing unicompartmental knee arthroplasty. J Arthroplasty 33:3153–3159
Kort NP, van Raay JJ, Cheung J, Jolink C, Deutman R (2007) Analysis of Oxford medial unicompartmental knee replacement using the minimally invasive technique in patients aged 60 and above: an independent prospective series. Knee Surg Sports Traumatol Arthrosc 15:1331–1334
Kort NP, van Raay JJ, van Horn JJ (2007) The Oxford phase III unicompartmental knee replacement in patients less than 60 years of age. Knee Surg Sports Traumatol Arthrosc 15:356–360
Kozinn SC, Scott R (1989) Unicondylar knee arthroplasty. J Bone Joint Surg Am 71:145–150
Kristensen PW, Holm HA, Varnum C (2013) Up to 10-year follow-up of the Oxford medial partial knee arthroplasty–695 cases from a single institution. J Arthroplasty 28:195–198
Lee M, Chen J, Shi LuC, Lo NN, Yeo SJ (2019) no differences in outcomes scores or survivorship of unicompartmental knee arthroplasty between patients younger or older than 55 years of age at minimum 10-year followup. Clin Orthop Relat Res 477:1434–1446
Liddle AD, Pandit H, Judge A, Murray DW (2016) Effect of surgical caseload on revision rate following total and unicompartmental knee replacement. J Bone Joint Surg Am 98:1–8
Mohammad HR, Bullock GS, Kennedy JA, Mellon SJ, Murray D, Judge A (2021) Cementless unicompartmental knee replacement achieves better ten-year clinical outcomes than cemented: a systematic review. Knee Surg Sports Traumatol Arthrosc 29:3229–3245
Mohammad HR, Mellon S, Judge A, Dodd C, Murray D (2021) The effect of age on the outcomes of cementless mobile bearing unicompartmental knee replacements. Knee Surg Sports Traumatol Arthrosc 30(3):928–938
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. J Clin Epidemiol 62:1006–1012
Murray DW, Goodfellow JW, O’Connor JJ (1998) The Oxford medial unicompartmental arthroplasty. J Bone Joint Surg Br 80(6):983–989
Murray DW, Fitzpatrick R, Rogers K, Pandit H, Beard DJ, Carr AJ et al (2007) The use of the Oxford hip and knee scores. J Bone Joint Surg Br 89(8):1010–1014
Niinimäki TT, Murray DW, Partanen J, Pajala A, Leppilahti JI (2011) Unicompartmental knee arthroplasties implanted for osteoarthritis with partial loss of joint space have high re-operation rates. Knee 18:432–435
Noble PC, Scuderi GR, Brekke AC, Sikorskii A, Benjamin JB, Lonner JH et al (2012) Development of a new knee society scoring system. Clin Orthop Relat Res 470:20–32
O’Connor JJ, Goodfellow JW, Dodd CA, Murray DW (2007) Development and clinical application of meniscal unicompartmental arthroplasty. Proc Inst Mech Eng H 221:47–59
OCEBM Levels of Evidence Working Group (2011) The Oxford Levels of Evidence 2. https://www.cebm.net/index.aspx?o=5653. Accessed 10 April 2022
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan—a web and mobile app for systematic reviews. Syst Rev 5:210
Pandit H, Hamilton TW, Jenkins C, Mellon SJ, Dodd CAF, Murray DW (2015) The clinical outcome of minimally invasive Phase 3 Oxford unicompartmental knee arthroplasty. Bone Joint J. 97(B11):1493–1499
Pandit H, Jenkins C, Gill HS, Smith G, Price AJ, Dodd CA et al (2011) Unnecessary contraindications for mobile-bearing unicompartmental knee replacement. J Bone Joint Surg Br 93:622–628
Price AJ, Dodd CAF, Svard UGC, Murray DW (2005) Oxford medial unicompartmental knee arthroplasty in patients younger and older than 60 years of age. J Bone Joint Surg Br 87(11):1488–1492
Registry NJ (2020) National Joint Registry 17th Annual Report. https://www.njrcentre.org.uk Accessed 01 June 2021.
Review Manager (RevMan) [Computer program]. Version 5.4 TCC, 2020. https://training.cochrane.org/online-learning/core-software-cochrane-reviews/revman/revman-non-cochrane-reviews. Accessed 03 March 2021
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73:712–716
StataCorp (2019) Stata Statistical Software: Release 16. College Station TSLAM
Venkatesh HK, Maheswaran SS (2019) Age and body mass index has no adverse effect on clinical outcome of unicompartmental knee replacement—midterm followup study. Indian J Orthop 53:442–445
Wang B, Sun H, Fu Z, Kang J, Yu X (2021) Application of unicompartmental knee arthroplasty in the treatment of knee osteoarthritis. Arthroplasty 3:1–7
Zhang W, Wang J, Li H, Wang W, George DM, Huang T (2020) Fixed- versus mobile-bearing unicompartmental knee arthroplasty: a meta-analysis. Sci Rep 10:19075
Acknowledgement
The authors would like to thank Dr Rajvir Singh for his statistical assistance and support.
Funding
Nothing to declare.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
LAS, AA, HK, GA, SGD and BK have no conflicts of interest. This is an adapted manuscript of a postgraduate university project submitted by LAS. DWM has an industrial grant from Zimmer Biomet paid to the University of Oxford. DWM receives consultancy payments and royalties from Zimmer Biomet relating to knee replacement.
Ethical approval
None required.
Informed consent
None required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
Appendices
Searching strategy examples: Database
(1) Medline (Ovid MEDLINE® Epub Ahead of Print, In-Process & Other Non-Indexed Citations, Ovid MEDLINE® Daily and Ovid MEDLINE®) 1946 to present. n = 831.
# | Query | Results from 1 Dec 2021 |
|---|---|---|
1 | age.mp. [mp = title, abstract, original title, name of substance word, subject heading word, floating sub-heading word, keyword heading word, organism supplementary concept word, protocol supplementary concept word, rare disease supplementary concept word, unique identifier, synonyms] | 9,156,352 |
2 | young*.mp. [mp = title, abstract, original title, name of substance word, subject heading word, floating sub-heading word, keyword heading word, organism supplementary concept word, protocol supplementary concept word, rare disease supplementary concept word, unique identifier, synonyms] | 1,528,140 |
3 | old*.mp. [mp = title, abstract, original title, name of substance word, subject heading word, floating sub-heading word, keyword heading word, organism supplementary concept word, protocol supplementary concept word, rare disease supplementary concept word, unique identifier, synonyms] | 1,547,553 |
4 | 1 or 2 or 3 | 9,920,818 |
5 | *Arthroplasty, Replacement, Knee/ | 22,839 |
6 | (unicompartmental knee arthroplasty or unicondylar knee arthroplasty or partial knee replacement).mp. [mp = title, abstract, original title, name of substance word, subject heading word, floating sub-heading word, keyword heading word, organism supplementary concept word, protocol supplementary concept word, rare disease supplementary concept word, unique identifier, synonyms] | 1,772 |
7 | ("UKA" or "UKR").mp. [mp = title, abstract, original title, name of substance word, subject heading word, floating sub-heading word, keyword heading word, organism supplementary concept word, protocol supplementary concept word, rare disease supplementary concept word, unique identifier, synonyms] | 1,510 |
8 | 6 or 7 | 2,112 |
9 | 5 and 8 | 1,448 |
10 | outcome*.mp. [mp = title, abstract, original title, name of substance word, subject heading word, floating sub-heading word, keyword heading word, organism supplementary concept word, protocol supplementary concept word, rare disease supplementary concept word, unique identifier, synonyms] | 2,656,185 |
11 | "revision*".mp. [mp = title, abstract, original title, name of substance word, subject heading word, floating sub-heading word, keyword heading word, organism supplementary concept word, protocol supplementary concept word, rare disease supplementary concept word, unique identifier, synonyms] | 103,997 |
12 | 10 or 11 | 2,725,609 |
13 | 4 and 9 and 12 | 831 |
(2) Web of science: n = 762

(3) Cochrane Library: n = 134 “unicompartmental knee arthroplasty” OR “unicondylar knee arthroplasty” OR “partial knee replac*” OR “UKA” OR”UKR” AND “age” OR “young*” OR “old*” AND “revision”
“PICOs” framework adopted
Population | Inclusion: adult patients > 18 years old, undergoing primary UKA indicated primarily for medial OA. Regardless of gender, BMI and ethnicity Exclusion: patients under 18 years, undergoing TKA, secondary UKA or having UKA for lateral compartment OA |
Intervention | Primary UKA in younger population Below 60 years Below 55 years (sub-analysis) |
Comparators | Primary UKA in older population Above 60 Y Above 55 Y (sub-analysis) |
Outcomes | Primary outcome: revision rate (CY) Secondary outcomes Revision incidents Patient-reported outcome measures: KSS, OKS |
Data collection form
Study |
Year of publication |
Country of study origin |
Study design, OCEBM score |
Number of dtudy participants |
Number of knees |
Mean age of patients |
UKA design used |
Number of UKAs in intervention group (young) |
Number of UKAs in control group (old) |
Age group classification |
Follow-up duration |
Number of revisions in intervention group (young) |
Number of revisions in control group (old) |
Revision rate in intervention group (young) |
Revision rate in in control group (old) |
KSS |
OKS |
Statistical tests used |
Study conclusion |
Other notes |
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Salman, L.A., Abudalou, A., Khatkar, H. et al. Impact of age on unicompartmental knee arthroplasty outcomes: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc 31, 986–997 (2023). https://doi.org/10.1007/s00167-022-07132-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-07132-x