Abstract
Purpose
To evaluate whether joint effusion at 3 months after anterior cruciate ligament (ACL) reconstruction is associated with ACL reinjury.
Methods
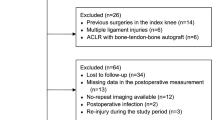
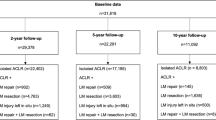
The medical records of 227 consecutive patients who underwent single-bundle ACL reconstruction between 2015 and 2018 were reviewed in this retrospective single-center study. Demographic data such as sex and age at surgery, as well as data on preinjury Tegner activity scale score, time from injury to surgery, presence of meniscus and cartilage injuries, and the occurrence of ACL reinjury within 2 years, were collected. Joint effusion was defined as grade 3 (range 0–3) according to the ACL Osteoarthritis Score by magnetic resonance imaging at 3 months postoperatively. Multivariate logistic regression analysis was performed to control for potential confounders.
Results
A total of 176 patients (mean age 22.5 ± 9.9 years) were included. Among these patients, 18 (10.2%) had ACL reinjury. At the multivariate logistic regression analysis, higher Tegner activity scale (odds ratio [OR] 3.12; 95% confidence interval [CI] 1.61–6.04; p < 0.001) and presence of joint effusion (OR 34.5; 95% CI 6.63–179.7; p < 0.001) increased the odds of ACL reinjury, and older age (OR 0.68; 95% CI 0.51–0.92; p = 0.012) decreased the odds of ACL reinjury.
Conclusions
Joint effusion with a larger fluid volume at 3 months postoperatively was one of the risk factors for ACL reinjury independent of confounders, such as age and activity level. This result suggests the possibility of postoperative intervention for ACL reinjury.
Level of evidence
III.

Similar content being viewed by others
Abbreviations
- ACL:
-
Anterior cruciate ligament
- ACLR:
-
Anterior cruciate ligament reconstruction
- MRI:
-
Magnetic resonance imaging
- CT:
-
Computed tomography
- ACLOAS:
-
Anterior Cruciate Ligament Osteoarthritis Score
- KOOS:
-
Knee Injury and Osteoarthritis Outcome Score
- OR:
-
Odds ratio
- CI:
-
Confidence interval
References
Anil U, Jejurikar N, Kenny L, Strauss EJ (2019) Changes in synovial fluid biomarker concentration before and after ACL reconstruction. Bull Hosp Joint Dis (2013) 77:189–193
Arundale AJH, Capin JJ, Zarzycki R, Smith AH, Snyder-Mackler L (2018) Two year ACL reinjury rate of 2.5%: outcomes report of the men in a secondary ACL injury prevention program (ACL-sports). Int J Sports Phys Ther 13:422–431
Brophy RH, Schmitz L, Wright RW, Dunn WR, Parker RD, Andrish JT, McCarty EC, Spindler KP (2012) Return to play and future ACL injury risk after ACL reconstruction in soccer athletes from the Multicenter Orthopaedic Outcomes Network (MOON) group. Am J Sports Med 40:2517–2522
Cai WS, Li HH, Konno SI, Numazaki H, Zhou SQ, Zhang YB, Han GT (2019) Patellofemoral MRI alterations following single bundle ACL reconstruction with hamstring autografts are associated with quadriceps femoris atrophy. Curr Med Sci 39:1029–1036
Chen CPC, Cheng CH, Hsu CC, Lin HC, Tsai YR, Chen JL (2017) The influence of platelet rich plasma on synovial fluid volumes, protein concentrations, and severity of pain in patients with knee osteoarthritis. Exp Gerontol 93:68–72
Cristiani R, Forssblad M, Edman G, Eriksson K, Stålman A (2021) Age, time from injury to surgery and quadriceps strength affect the risk of revision surgery after primary ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 29:4154–4162
Culvenor AG, Collins NJ, Guermazi A, Cook JL, Vicenzino B, Khan KM, Beck N, van Leeuwen J, Crossley KM (2015) Early knee osteoarthritis is evident one year following anterior cruciate ligament reconstruction: a magnetic resonance imaging evaluation. Arthritis Rheumatol 67:946–955
Fältström A, Hägglund M, Magnusson H, Forssblad M, Kvist J (2016) Predictors for additional anterior cruciate ligament reconstruction: data from the Swedish national ACL register. Knee Surg Sports Traumatol Arthrosc 24:885–894
Frobell RB, Le Graverand MP, Buck R, Roos EM, Roos HP, Tamez-Pena J, Totterman S, Lohmander LS (2009) The acutely ACL injured knee assessed by MRI: changes in joint fluid, bone marrow lesions, and cartilage during the first year. Osteoarthr Cartil 17:161–167
Grassi A, Macchiarola L, Urrizola Barrientos F, Zicaro JP, Costa Paz M, Adravanti P, Dini F, Zaffagnini S (2019) Steep posterior tibial slope, anterior tibial subluxation, deep posterior lateral femoral condyle, and meniscal deficiency are common findings in multiple anterior cruciate ligament failures: an MRI case-control study. Am J Sports Med 47:285–295
Hays PL, Kawamura S, Deng XH, Dagher E, Mithoefer K, Ying L, Rodeo SA (2008) The role of macrophages in early healing of a tendon graft in a bone tunnel. J Bone Joint Surg Am 90:565–579
Higuchi H, Shirakura K, Kimura M, Terauchi M, Shinozaki T, Watanabe H, Takagishi K (2006) Changes in biochemical parameters after anterior cruciate ligament injury. Int Orthop 30:43–47
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Larsson S, Struglics A, Lohmander LS, Frobell R (2017) Surgical reconstruction of ruptured anterior cruciate ligament prolongs trauma-induced increase of inflammatory cytokines in synovial fluid: an exploratory analysis in the KANON trial. Osteoarthr Cartil 25:1443–1451
Lindström M, Wredmark T, Wretling ML, Henriksson M, Felländer-Tsai L (2015) Post-operative bracing after ACL reconstruction has no effect on knee joint effusion. A prospective, randomized study. Knee 22:559–564
Logan CA, Aman ZS, Kemler BR, Storaci HW, Dornan GJ, LaPrade RF (2019) Influence of medial meniscus bucket-handle repair in setting of anterior cruciate ligament reconstruction on tibiofemoral contact mechanics: a biomechanical study. Arthroscopy 35:2412–2420
Mathiessen A, Conaghan PG (2017) Synovitis in osteoarthritis: current understanding with therapeutic implications. Arthritis Res Ther 19:18
Mohan R, Webster KE, Johnson NR, Stuart MJ, Hewett TE, Krych AJ (2018) Clinical outcomes in revision anterior cruciate ligament reconstruction: a meta-analysis. Arthroscopy 34:289–300
Morimoto Y, Ferretti M, Ekdahl M, Smolinski P, Fu FH (2009) Tibiofemoral joint contact area and pressure after single- and double-bundle anterior cruciate ligament reconstruction. Arthroscopy 25:62–69
Ogura T, Asai S, Akagi R, Fukuda H, Yamaura I, Sakai H, Ichino Y, Takahashi T, Omodani T, Saito C, Ninomiya T, Shiko Y, Kawasaki Y, Tsuchiya A, Takahashi K, Sasho T (2021) Joint effusion at 6 months is a significant predictor of joint effusion 1 year after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 29:3839–3845
Rahardja R, Zhu M, Love H, Clatworthy MG, Monk AP, Young SW (2020) Effect of graft choice on revision and contralateral anterior cruciate ligament reconstruction: results from the New Zealand ACL registry. Am J Sports Med 48:63–69
Roemer FW, Frobell R, Lohmander LS, Niu J, Guermazi A (2014) Anterior cruciate ligament osteoarthritis score (ACLOAS): longitudinal MRI-based whole joint assessment of anterior cruciate ligament injury. Osteoarthr Cartil 22:668–682
Runer A, Csapo R, Hepperger C, Herbort M, Hoser C, Fink C (2020) Anterior cruciate ligament reconstructions with quadriceps tendon autograft result in lower graft rupture rates but similar patient-reported outcomes as compared with hamstring tendon autograft: a comparison of 875 patients. Am J Sports Med 48:2195–2204
Snaebjörnsson T, Hamrin-Senorski E, Svantesson E, Karlsson L, Engebretsen L, Karlsson J, Samuelsson K (2019) Graft diameter and graft type as predictors of anterior cruciate ligament revision: a cohort study including 18,425 patients from the Swedish and Norwegian National Knee Ligament Registries. J Bone Joint Surg Am 101:1812–1820
Song B, Jiang C, Luo H, Chen Z, Hou J, Zhou Y, Yang R, Shen H, Li W (2017) Macrophage M1 plays a positive role in aseptic inflammation-related graft loosening after anterior cruciate ligament reconstruction surgery. Inflammation 40:1815–1824
Sonnery-Cottet B, Saithna A, Quelard B, Daggett M, Borade A, Ouanezar H, Thaunat M, Blakeney WG (2019) Arthrogenic muscle inhibition after ACL reconstruction: a scoping review of the efficacy of interventions. Br J Sports Med 53:289–298
Yao SY, Cao MD, He X, Fu BSC, Yung PSH (2021) Biological modulations to facilitate graft healing in anterior cruciate ligament reconstruction (ACLR), when and where to apply? A systematic review. J Orthop Transl 30:51–60
Zysk SP, Fraunberger P, Veihelmann A, Dörger M, Kalteis T, Maier M, Pellengahr C, Refior HJ (2004) Tunnel enlargement and changes in synovial fluid cytokine profile following anterior cruciate ligament reconstruction with patellar tendon and hamstring tendon autografts. Knee Surg Sports Traumatol Arthrosc 12:98–103
Acknowledgements
The authors would like to thank Editage for English language editing.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
NK conceived and designed the study, analyzed and interpreted the data, drafted the manuscript, approved the final version of the manuscript to be published, and agrees to be accountable for all aspects of the work if questions arise related to its accuracy or integrity. AK conceived and designed the study, contributed on interpreted the data, revised the manuscript critically for important intellectual content, approved the final version of the manuscript to be published, and agrees to be accountable for all aspects of the work if questions arise related to its accuracy or integrity. KO contributed to the acquisition of the data, revised the manuscript critically for important intellectual content, approved the final version of the manuscript to be published, and agrees to be accountable for all aspects of the work if questions arise related to its accuracy or integrity. NA contributed to the interpretation of the data, revised the manuscript critically for important intellectual content, approved the final version of the manuscript to be published, and agrees to be accountable for all aspects of the work if questions arise related to its accuracy or integrity. KH contributed to the interpretation of the data, revised the manuscript critically for important intellectual content, approved the final version of the manuscript to be published, and agrees to be accountable for all aspects of the work if questions arise related to its accuracy or integrity. TY contributed to the interpretation of the data, revised the manuscript critically for important intellectual content, approved the final version of the manuscript to be published, and agree to be accountable for all aspects of the work if questions arise related to its accuracy or integrity. MY contributed to the interpretation of the data, revised the manuscript critically for important intellectual content, approved the final version of the manuscript to be published, and agrees to be accountable for all aspects of the work if questions arise related to its accuracy or integrity.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
This study was approved by the Medical Ethical Committee of the University of Tsukuba (No. R03-257).
Informed consent
The need for informed consent was waived by the Medical Ethical Committee of the University of Tsukuba (no. R03-257) because of the retrospective nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kikuchi, N., Kanamori, A., Okuno, K. et al. Joint effusion at 3 months after anterior cruciate ligament reconstruction is associated with reinjury. Knee Surg Sports Traumatol Arthrosc 31, 1798–1804 (2023). https://doi.org/10.1007/s00167-022-07081-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-07081-5