Abstract
Purpose
To investigate the relationship between glenoid width and other morphologic parameters using three-dimensional (3D) computed tomography (CT) images of native shoulders, and to create a new measurement tool to assess glenoid defects in a Canadian population with established anterior shoulder instability.
Methods
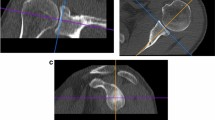
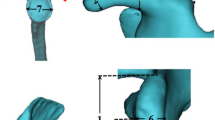
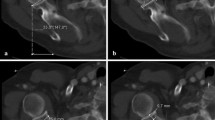
Forty-three glenoid CT scans were analyzed for patients who underwent contralateral shoulder glenoid reconstruction for anterior shoulder instability between 2012 and 2020. Demographic data were obtained including age, gender and BMI. The subjects were excluded if they had a prior history of ipsilateral shoulder instability, shoulder fractures, or bone tumors. The following glenoid parameters were measured: width (W), height (H), anteroposterior (AP) depth, superior–inferior (SI) depth and version. The shape of the glenoid was also classified into pear, inverted comma or oval.
Results
There were 35 male and 8 females with a mean age of 34.5 ± 12.9 years. The glenoid width was strongly correlated with the height (R2 = 0.9) and a regression model equation was obtained: W (mm) = 2.5 + 0.7*H (mm). There was also strong correlation with gender (P < 0.001), glenoid shape (P = 0.030), AP and SI depths (P = 0.006 and P < 0.001, respectively). Male gender was associated with higher measurement values for all parameters. The most common glenoid shapes were the pear (46.5%) and oval morphotypes (39.6%) for the whole study group.
Conclusion
The native glenoid width can be estimated based on glenoid height using ipsilateral 3D CT. This may help with preoperative planning and surgical decision-making for patients with anterior shoulder instability and glenoid bone loss.
Level of evidence
III.





Similar content being viewed by others
Change history
06 July 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00167-022-07055-7
References
Altan E, Ozbaydar MU, Tonbul M, Yalcin L (2014) Comparison of two different measurement methods to determine glenoid bone defects: area or width? J Shoulder Elbow Surg 23(8):1215–1222
Bakshi NK, Cibulas GA, Sekiya JK, Bedi A (2018) A clinical comparison of linear- and surface area-based methods of measuring glenoid bone loss. Am J Sports Med 46(10):2472–2477
Balg F, Boileau P (2007) The instability severity index score: a simple pre-operative score to select patients for arthroscopic or open shoulder stabilisation. J Bone Joint Surg 89(11):1470–1477
Barchilon VS, Kotz E, Barchilon Ben-Av M, Glazer E, Nyska M (2008) A simple method for quantitative evaluation of the missing area of the anterior glenoid in anterior instability of the glenohumeral joint. Skeletal Radiol 37(8):731–736
Baudi P, Righi P, Bolognesi D et al (2005) How to identify and calculate glenoid bone deficit. Chir Organi Mov 90(2):145–152
Bhatia S, Saigal A, Frank RM et al (2015) Glenoid diameter is an inaccurate method for percent glenoid bone loss quantification: analysis and techniques for improved accuracy. Arthroscopy 31(4):608-614.e1
Chen XZ, Liu TX, Chen Y, Du L, Liu WF, Lin P (2020) Simple linear calculating method of glenoid bone defects using 3-dimensional Computed tomography based on an East Asian population in China. Orthop J Sports Med 8(4):12–14
Cohn MR, DeFroda SF, Huddleston HP, Williams BT, Singh H, Vadhera A et al (2022) Does native glenoid anatomy predispose to shoulder instability? An MRI analysis. J Shoulder Elbow Surg S1058–2746(22):00337–00338
Dickens JF, Slaven SE, Cameron KL et al (2019) Prospective evaluation of glenoid bone loss after first-time and recurrent anterior glenohumeral instability events. Am J Sports Med 47(5):1082–1089
Dumont GD, Russell RD, Browne MG, Robertson WJ (2012) Area-based determination of bone loss using the glenoid arc angle. Arthroscopy 28(7):1030–1035
Galvin JW, Ernat JJ, Waterman BR, Stadecker MJ, Parada SA (2017) The epidemiology and natural history of anterior shoulder instability. Curr Rev Musculoskelet Med 10(4):411–424
Di Giacomo G, Itoi E, Burkhart SS (2014) Evolving concept of bipolar bone loss and the hill-sachs lesion: from “engaging/non-engaging” lesion to “on-track/off-track” lesion. Arthroscopy 30(1):90–98
Giles JW, Owens BD, Athwal GS (2015) Estimating glenoid width for instability-related bone loss: a CT evaluation of an MRI formula. Am J Sports Med 43(7):1726–1730
Haas M, Plachel F, Wierer G et al (2019) Glenoid morphology is associated with the development of instability arthropathy. J Shoulder Elbow Surg 28(5):893–899
Hurley ET, Matache BA, Wong I, Itoi E, Strauss EJ, Delaney RA et al (2022) Anterior shoulder instability part II—latarjet, remplissage, and glenoid bone-grafting—an international consensus statement. Arthroscopy 38(2):224–233
John R, Wong I (2019) Innovative approaches in the management of shoulder instability: current concept review. Curr Rev Musculoskelet Med 12(3):386–396
Kraeutler MJ, McCarty EC, Belk JW et al (2018) Descriptive epidemiology of the MOON shoulder instability cohort. Am J Sports Med 46(5):1064–1069
Kralinger F, Aigner F, Longato S, Rieger M, Wambacher M (2006) Is the bare spot a consistent landmark for shoulder arthroscopy? A study of 20 embalmed glenoids with 3-dimensional computed tomographic reconstruction. Arthroscopy 22(4):428–432
Leroux T, Wasserstein D, Veillette C et al (2014) Epidemiology of primary anterior shoulder dislocation requiring closed reduction in Ontario, Canada. Am J Sports Med 42(2):442–450
Owens BD, Burns TC, Campbell SE, Svoboda SJ, Cameron KL (2013) Simple method of glenoid bone loss calculation using ipsilateral magnetic resonance imaging. Am J Sports Med 41(3):622–624
Parada SA, Jones MC, DeFoor MT, Griswold BG, Roberts AD, Provencher MT (2020) Mathematical modeling of glenoid bone loss demonstrate differences in calculations that May affect surgical decision making. J Orthop 22:402–407
Provencher MT, Bhatia S, Ghodadra NS et al (2010) Recurrent shoulder instability: Current concepts for evaluation and management of glenoid bone loss. J Bone Joint Surg 92(SUPPL. 2):133–151
Rossi LA, Frank RM, Wilke D, Provencher CMT, Millet PJ, Romeo A et al (2021) Evaluation and management of glenohumeral instability with associated bone loss: an expert consensus statement using the modified Delphi technique. Arthroscopy 37(6):1719–1728
Sgroi M, Huzurudin H, Ludwig M, Zippelius T, Reichel H, Kappe T (2022) MRI allows accurate measurement of glenoid bone loss. Clin Orthop Relat Res. https://doi.org/10.1097/CORR.0000000000002215
Shin SJ, Jun BJ, Koh YW, McGarry MH, Lee TQ (2018) Estimation of anterior glenoid bone loss area using the ratio of bone defect length to the distance from posterior glenoid rim to the centre of the glenoid. Knee Surg Sports Traumatol Arthrosc 26(1):48–55
Sugaya H, Moriishi J, Dohi M, Kon Y, Tsuchiya A (2003) Glenoid rim morphology in recurrent anterior glenohumeral instability. J Bone Joint Surg 85(5):878–884
Tokish JM (2018) Editorial commentary: measurement of glenoid bone loss with computed tomography scan versus magnetic resonance imaging. Arthroscopy 34(12):3148–3149
Vandenbroucke JP, Von Elm E, Altman DG et al (2007) Strengthening the reporting of observational studies in Epidemiology (STROBE): explanation and elaboration. PLoS Med 4(10):1628–1654
Verweij LPE, Schuit AA, Kerkhoffs GMMJ, Blankevoort L, van den Bekerom MPJ, van Deurzen DFP (2020) Accuracy of currently available methods in quantifying anterior glenoid bone loss: controversy regarding gold standard—a systematic review. Arthroscopy 36(8):2295-2313.e1
Vopat BG, Cai W, Torriani M et al (2018) Measurement of glenoid bone loss with 3-dimensional magnetic resonance imaging: a matched computed tomography analysis. Arthroscopy 34(12):3141–3147
Weber AE, Bolia IK, Horn A, Villacis D, Omid R, Tibone JE et al (2021) Glenoid bone loss in shoulder instability: superiority of three-dimensional computed tomography over two-dimensional magnetic resonance imaging using established methodology. Clin Orthop Surg 13(2):223–228
Weil S, Arnander M, Pearse Y, Tennent D (2022) Reporting of glenoid bone loss measurement in clinical studies and the need for standardization: a systematic review. Bone Joint J. 104-B(1):12–18
Willemot LB, Elhassan BT, Verborgt O (2018) Bony reconstruction of the anterior glenoid rim. J Am Acad Orthop Surg 26(10):e207–e218
Funding
This study did not receive funding.
Author information
Authors and Affiliations
Contributions
JR: development of research project, literature review, data collection, and manuscript write-up; JX: development of research project, and data collection; SS: research ethics approval, data collection, and manuscript revision and review; JM: data management and analysis, and manuscript revision and review; LJ: data management and analysis, and manuscript revision and review; IW: development of research question, and manuscript revision and review.
Corresponding author
Ethics declarations
Conflict of interest
The authors declares that they have no conflict of interest.
Ethical approval
This study has been approved by Nova Scotia Health Research Ethics Board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: Figures incorrectly published now corrected.
Rights and permissions
About this article
Cite this article
Rayes, J., Xu, J., Sparavalo, S. et al. Calculating glenoid bone loss based on glenoid height using ipsilateral three-dimensional computed tomography. Knee Surg Sports Traumatol Arthrosc 31, 169–176 (2023). https://doi.org/10.1007/s00167-022-07020-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-07020-4