Abstract
Purpose
To determine whether the use of an unloading brace can increase the thickness of cartilage regenerate after microfracture surgery.
Methods
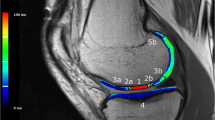
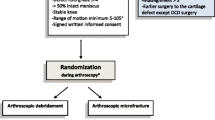
This is a randomized (1:1) controlled clinical trial. Twenty-four patients who underwent microfracture between 2012 and 2015 were identified and were randomly assigned to an unloading brace group or a no-brace group. All patients were kept non-weight bearing for the first eight weeks after surgery and then patients in the intervention group began using an unloading brace for an average of 63.9 (SD = 41.6) days to protect clot stability by exerting a varus or valgus force on the knee to decrease the force on the knee’s lateral or medial compartment, respectively. Quality of the cartilage repair was assessed with knee magnetic resonance imaging to determine repair tissue thickness (primary outcome), repair tissue volume, and T2 relaxation times at 12 and 24 months after surgery. Clinical outcomes were evaluated with KOOS, Tegner, SF12, and Lysholm questionnaires at six, 12 and 24 months after surgery.
Results
Three patients were lost to follow-up, resulting in 21 patients ultimately analyzed. The unloading brace repair tissue was greater than the no-brace group in volume (26.8 ± 23.7 mm3 vs − 8.4 ± 22.7 mm3, p = 0.005) and thickness (0.2 ± 0.2 mm versus − 0.4 ± 0.3 mm, p = 0.001) at 12 months and in cartilage thickness in the unloading brace group at 24 months (0.4 ± 0.4 mm versus − 0.1 ± 0.3 mm, p = 0.029). There was a positive correlation between wearing the brace longer and improved 6-month KOOS symptom scores (r = 0.82, p = 0.013), 6-month KOOS QOL scores (r = 0.80, p = 0.017), 6-month Tegner scores (r = 0.94, p = 0.002), and Tegner score changes from baseline to 6 months (r = 0.80, p = 0.032).
Conclusion
This study found a significant mid-term increase in cartilage repair tissue thickness following unloading bracing in patients recovering from microfracture for isolated chondral defects.
Level of evidence
II.



Similar content being viewed by others
References
Bacon K, LaValley MP, Jafarzadeh SR, Felson D (2020) Does cartilage loss cause pain in osteoarthritis and if so, how much? Ann Rheum Dis 79:1105–1110
Brinkhof S, Te Moller N, Froeling M, Brommer H, van Weeren R, Ito K et al (2020) T2* mapping in an equine articular groove model: Visualizing changes in collagen orientation. J Orthop Res. https://doi.org/10.1002/jor.24764
Chaudhari AS, Black MS, Eijgenraam S, Wirth W, Maschek S, Sveinsson B et al (2018) Five-minute knee MRI for simultaneous morphometry and T2 relaxometry of cartilage and meniscus and for semiquantitative radiological assessment using double-echo in steady-state at 3T. J Magn Reson Imaging 47:1328–1341
Chimutengwende-Gordon M, Donaldson J, Bentley G (2020) Current solutions for the treatment of chronic articular cartilage defects in the knee. EFORT Open Rev 5:156–163
Gross KD, Hillstrom HJ (2008) Noninvasive devices targeting the mechanics of osteoarthritis. Rheum Dis Clin N Am 34:755–776
Hjartarson HF, Toksvig-Larsen S (2018) The clinical effect of an unloader brace on patients with osteoarthritis of the knee, a randomized placebo controlled trial with one year follow up. BMC Musculoskelet Disord 19:341
Hunter DJ, March L, Sambrook PN (2003) The association of cartilage volume with knee pain. Osteoarthr Cartil 11:725–729
Karuppal R (2017) Current concepts in the articular cartilage repair and regeneration. J Orthop 14:A1–A3
Miller DJ, Smith MV, Matava MJ, Wright RW, Brophy RH (2015) Microfracture and osteochondral autograft transplantation are cost-effective treatments for articular cartilage lesions of the distal femur. Am J Sports Med 43:2175–2181
Moher D, Schulz KF, Altman DG, Group C (2003) The CONSORT statement: revised recommendations for improving the quality of reports of parallel-group randomised trials. Clin Oral Investig 7:2–7
Mosher TJ, Zhang Z, Reddy R, Boudhar S, Milestone BN, Morrison WB et al (2011) Knee articular cartilage damage in osteoarthritis: analysis of MR image biomarker reproducibility in ACRIN-PA 4001 multicenter trial. Radiology 258:832–842
Oneto JM, Ellermann J, LaPrade RF (2010) Longitudinal evaluation of cartilage repair tissue after microfracture using T2-mapping: a case report with arthroscopic and MRI correlation. Knee Surg Sports Traumatol Arthrosc 18:1545–1550
Petersen W, Ellermann A, Henning J, Nehrer S, Rembitzki IV, Fritz J et al (2018) Non-operative treatment of unicompartmental osteoarthritis of the knee: a prospective randomized trial with two different braces-ankle-foot orthosis versus knee unloader brace. Arch Orthop Trauma Surg 139:155–166
Roos EM, Lohmander LS (2003) The Knee injury and Osteoarthritis Outcome Score (KOOS): from joint injury to osteoarthritis. Health Qual Life Outcomes 1:64
Simon TM, Jackson DW (2006) Articular cartilage: injury pathways and treatment options. Sports Med Arthrosc Rev 14:146–154
Sophia Fox AJ, Bedi A, Rodeo SA (2009) The basic science of articular cartilage: structure, composition, and function. Sports Health 1:461–468
Steadman JR, Rodkey WG, Briggs KK (2002) Microfracture to treat full-thickness chondral defects: surgical technique, rehabilitation, and outcomes. J Knee Surg 15:170–176
Steadman JR, Rodkey WG, Briggs KK, Rodrigo JJ (1999) The microfracture technic in the management of complete cartilage defects in the knee joint. Oper Tech Orthop 28:26–32
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res 198:43–49
Theodoropoulos J, Dwyer T, Whelan D, Marks P, Hurtig M, Sharma P (2012) Microfracture for knee chondral defects: a survey of surgical practice among Canadian orthopedic surgeons. Knee Surg Sports Traumatol Arthrosc 20:2430–2437
Ware J Jr, Kosinski M, Keller SD (1996) A 12-Item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Med Care 34:220–233
Wirth W, Eckstein F (2008) A technique for regional analysis of femorotibial cartilage thickness based on quantitative magnetic resonance imaging. IEEE Trans Med Imaging 27:737–744
Wirth W, Eckstein F, Boeth H, Diederichs G, Hudelmaier M, Duda GN (2014) Longitudinal analysis of MR spin-spin relaxation times (T2) in medial femorotibial cartilage of adolescent vs mature athletes: dependence of deep and superficial zone properties on sex and age. Osteoarthr Cartil 22:1554–1558
Funding
Funding was provided by the Department of Orthopedic Surgery at Stanford University. The unloading braces and iButtons were donated by Ossur.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Author J.D. is a consultant for Ossur, Authors J.K. and A.F. report no conflicts of interest.
Ethical approval
IRB: Stanford Institutional Review Board, IRB number 17985, RCT: NCT02016300.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Konopka, J.A., Finlay, A.K., Eckstein, F. et al. Effects of unloader bracing on clinical outcomes and articular cartilage regeneration following microfracture of isolated chondral defects: a randomized trial. Knee Surg Sports Traumatol Arthrosc 29, 2889–2898 (2021). https://doi.org/10.1007/s00167-020-06228-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-06228-6