Abstract
Purpose
To study the efficacy of lopinavir-ritonavir and hydroxychloroquine in critically ill patients with coronavirus disease 2019 (COVID-19).
Methods
Critically ill adults with COVID-19 were randomized to receive lopinavir-ritonavir, hydroxychloroquine, combination therapy of lopinavir-ritonavir and hydroxychloroquine or no antiviral therapy (control). The primary endpoint was an ordinal scale of organ support-free days. Analyses used a Bayesian cumulative logistic model and expressed treatment effects as an adjusted odds ratio (OR) where an OR > 1 is favorable.
Results
We randomized 694 patients to receive lopinavir-ritonavir (n = 255), hydroxychloroquine (n = 50), combination therapy (n = 27) or control (n = 362). The median organ support-free days among patients in lopinavir-ritonavir, hydroxychloroquine, and combination therapy groups was 4 (– 1 to 15), 0 (– 1 to 9) and—1 (– 1 to 7), respectively, compared to 6 (– 1 to 16) in the control group with in-hospital mortality of 88/249 (35%), 17/49 (35%), 13/26 (50%), respectively, compared to 106/353 (30%) in the control group. The three interventions decreased organ support-free days compared to control (OR [95% credible interval]: 0.73 [0.55, 0.99], 0.57 [0.35, 0.83] 0.41 [0.24, 0.72]), yielding posterior probabilities that reached the threshold futility (≥ 99.0%), and high probabilities of harm (98.0%, 99.9% and > 99.9%, respectively). The three interventions reduced hospital survival compared with control (OR [95% CrI]: 0.65 [0.45, 0.95], 0.56 [0.30, 0.89], and 0.36 [0.17, 0.73]), yielding high probabilities of harm (98.5% and 99.4% and 99.8%, respectively).
Conclusion
Among critically ill patients with COVID-19, lopinavir-ritonavir, hydroxychloroquine, or combination therapy worsened outcomes compared to no antiviral therapy.
Similar content being viewed by others
The Randomised, Embedded, Multifactorial Adaptive Platform (REMAP-CAP) trial is the largest randomized clinical trial in critically ill patients with COVID-19 to report the effects of lopinavir-ritonavir, hydroxychloroquine and combination therapy of lopinavir-ritonavir and hydroxychloroquine compared with no antiviral therapy. We found that, among critically ill patients with COVID-19, lopinavir-ritonavir, hydroxychloroquine and combination therapy reduced organ support-free days and survival compared to no COVID-19 antiviral therapy. |
Introduction
In less than 18 months, coronavirus disease 2019 (COVID-19), caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has infected more than 175 million people across the globe and caused more than 3.8 million deaths [1]. Given the emerging nature of the virus, several repurposed agents were considered as potential antiviral agents for COVID-19 [2]. Lopinavir-ritonavir and hydroxychloroquine were proposed based on data from severe acute respiratory syndrome (SARS) and middle east respiratory syndrome (MERS) [3,4,5,6,7,8]. In vitro, lopinavir and hydroxychloroquine inhibit SARS-CoV-2 replication [9,10,11]. A pharmacokinetic analysis predicted that therapeutic doses of lopinavir, ritonavir and hydroxychloroquine would achieve concentrations in both plasma and lungs that are inhibitory of SARS-CoV-2 [12] In a ferret infection model for SARS-CoV-2 infection, lopinavir-ritonavir or hydroxychloroquine resulted in improved clinical scores compared to the control group, although the virus titers were not different [13]. The two agents became widely used [14,15,16]. Several national guidelines for treatment of COVID-19 listed lopinavir-ritonavir and hydroxychloroquine (or chloroquine) as therapeutic options [17], and in March 2020, the US Food and Drug Administration (FDA) issued an Emergency Use Authorization for hydroxychloroquine, which was revoked later in June 2020[18]. Subsequently, clinical trials were published, including the RECOVERY and Solidarity trials, demonstrating lack of benefit of lopinavir-ritonavir and hydroxychloroquine in hospitalized patients with COVID-19, although the proportions of critically ill patients were small [19,20,21,22,23]. In addition, most trials tested individual interventions, therefore, the effect of the combination of lopinavir-ritonavir and hydroxychloroquine and the interaction with other agents used for the treatment of COVID-19 such as corticosteroids and interleukin-6 (IL-6) receptor antagonists are unknown.
The objective of this trial was to evaluate the effects of lopinavir-ritonavir, hydroxychloroquine, and combination therapy of lopinavir-ritonavir and hydroxychloroquine compared to no COVID-19 antiviral therapy on organ support-free days in critically ill patients with COVID-19.
Methods
Study design
The Randomized, Embedded, Multifactorial Adaptive Platform trial for Community-Acquired Pneumonia (REMAP-CAP, NCT02735707) is an ongoing international adaptive platform trial designed to determine the best treatment strategies for patients with severe pneumonia in both pandemic and non-pandemic settings [24]. In the pandemic stratum, patients requiring organ support in an intensive care unit were enrolled as Severe State, and hospitalized patients not receiving organ support in the intensive care unit (ICU) were enrolled as Moderate State. Within the COVID-19 Antiviral Therapy Domain, patients were randomized to receive lopinavir-ritonavir, hydroxychloroquine, combination therapy of lopinavir-ritonavir and hydroxychloroquine or control (no antiviral agents against COVID-19). The pandemic stratum included other domains each with multiple interventions, and patients could be randomized to interventions in multiple domains (Statistical Analysis Committee Primary Analysis Report, Supplementary Appendix). This report describes the results of the patients in the Severe State in the COVID-19 Antiviral Therapy Domain (Table S1). Some sites also enrolled patients in the Moderate State. These patients (n = 32) are not included in the current analysis, though descriptive data are reported in the Supplementary Appendix.
The trial's protocol documents (REMAP-CAP Core Protocol, REMAP-CAP Pandemic Appendix to the Core Protocol, COVID-19 Antiviral Therapy Domain-Specific Appendix) and statistical analysis plan (REMAP-CAP Statistical Analysis Appendix, COVID-19 Antiviral Domain Statistical Analysis Plan) were posted online (http://www.remapcap.org) before analysis and are available in the Supplementary Appendix. The trial is managed by a blinded International Trial Steering Committee and is overseen by an unblinded Data and Safety Monitoring Board (DSMB).
The trial was approved by the relevant ethics committees in all regions. Written or verbal informed consent, in accordance with regional legislation, was obtained from all patients or their surrogates.
Patients
Patients were eligible for the COVID-19 Antiviral Therapy Domain- Severe State if they were ≥ 18 years old, admitted with suspected or confirmed COVID-19, and were receiving respiratory or cardiovascular organ failure support in an intensive care unit (ICU). Organ support included the provision of invasive mechanical ventilation, non-invasive mechanical ventilation, high-flow nasal cannulae with a flow rate of at least 30 L per minute and a fractional inspired oxygen concentration of 0.4 or higher, or the infusion of vasopressor or inotropes for shock. In addition to patients enrolled in the COVID-19 Antiviral Therapy Domain, the primary model included patients enrolled in other domains in Severe State, for covariate adjustment. Patients were excluded from the platform if (1) death was deemed to be imminent during the next 24 h AND one or more of the patient, substitute decision-maker, or attending physician are not committed to full active treatment, (2) expected to be discharged from hospital the same day or the following day, (3) more than 14 days have elapsed while admitted to hospital with symptoms of an acute illness due to suspected or proven pandemic infection, or (4) previous participation in this REMAP-CAP within the last 90 days. Additionally, patients were excluded from the COVID-19 Antiviral Therapy Domain in the presence of any of the following exclusion criteria (1) known hypersensitivity to lopinavir-ritonavir and hydroxychloroquine, (2) receiving lopinavir-ritonavir or hydroxychloroquine as a usual medication prior to this hospitalization, (3) known human immunodeficiency (HIV) infection (an exclusion criterion from receiving lopinavir-ritonavir), (4) severe liver failure (an exclusion criterion from lopinavir-ritonavir), (5) known or suspected pregnancy, (6) receiving amiodarone as a usual medication prior to this hospitalization or any administration of amiodarone within the 72 h prior to the assessment of eligibility (an exclusion criterion from lopinavir-ritonavir), (7) high clinical risk of sustained ventricular dysrhythmia (an exclusion criterion from hydroxychloroquine). Detailed platform and COVID-19 Antiviral Therapy Domain-specific inclusion and exclusion criteria are listed in Table S2 in the Supplementary Appendix.
Randomization and masking
Using a concealed online randomization system, patients were randomized to receive lopinavir-ritonavir, hydroxychloroquine, combination therapy of lopinavir-ritonavir and hydroxychloroquine or control (no antiviral agents against COVID-19). Based on local equipoise and drug availability, investigators at each participating site selected a priori two or more interventions, one of which had to be control, to which patients could be randomized. The REMAP-CAP platform uses response-adaptive randomization; however, the allocation in the COVID-19 Antiviral Therapy Domain did not deviate from the starting equal ratio before enrollment was halted. Although the interventions were given as open-label drugs, neither the clinical staff nor the ITSC were provided any information about aggregate patient outcomes.
Interventions
Lopinavir-ritonavir was administered for 5 days minimum, up to a maximum of 14 days or until ICU discharge whichever occurred first. Lopinavir–ritonavir was administered at a dose of 400 mg of lopinavir and 100 mg of ritonavir (Kaletra, AbbVie) every 12 h. For patients with a gastric tube who were unable to swallow tablets, lopinavir-ritonavir (at the same dose) was administered as a 5-ml suspension every 12 h or alternatively as two dissolved tablets or four crushed tablets (double dose), noting that systemic absorption is reduced by approximately 50% for crushed tablets [25]. Hydroxychloroquine was administered as two loading doses of 800 mg, 6-h apart, followed 6 h later by 400 mg 12 hourly for 12 doses. This dose regimen was supported by pharmacokinetic modelling and by guidance regarding safety from clinicians with experience with the use of hydroxychloroquine for the treatment of severe malaria [26]. If a patient was unable to swallow, crushed hydroxychloroquine tablets were administered via an enteral tube. The study protocol provided guidance for monitoring for drug interactions and QTc prolongation (Supplementary Appendix). Other aspects of care were provided as per each site's standard of care.
Outcomes
The primary outcome was a composite ordinal scale of the number of respiratory and cardiovascular organ support-free days (OSFD) and in-hospital mortality with death assigned the worst outcome (− 1). Among survivors, respiratory and cardiovascular organ support-free days are calculated up to day 21, such that a higher number represents faster recovery. The definitions of respiratory and cardiovascular organ support were the same as in the inclusion criteria. This outcome was used in a recent FDA-approved registration trial, with a 1.5-day difference considered to be the minimal clinically important difference [27]. Each component of the composite, organ support free-days in survivors and in-hospital mortality, are reported separately. Secondary a priori outcomes were 90-day survival, respiratory support-free days, cardiovascular support-free days, time to ICU and hospital discharge, a composite outcome of progression to invasive mechanical ventilation, extracorporeal membrane oxygenation (ECMO), or death among those not ventilated at baseline, the World Health Organisation ordinal scale assessed at 14 days and SARS-CoV-2 RNA clearance from respiratory specimens (COVID-19 Antiviral Therapy Domain-Specific Appendix and COVID-19 Antiviral Domain SAP, Supplementary Appendix) [28]. The WHO scale is a clinical progression scale that reflects patient trajectory and resource use over the course of clinical illness and ranges from 0 (no disease) to 8 (death). Safety a priori outcomes included serious adverse events and serious ventricular arrhythmia or sudden unexpected death while not receiving continuous cardiac monitoring (COVID-19 Antiviral Therapy Domain-Specific Appendix and COVID-19 Antiviral Domain SAP, Supplementary Appendix).
Statistical analysis
REMAP-CAP uses a Bayesian design with no prespecified sample size; enrollment in any intervention continues until a pre-defined statistical trigger is met at an adaptive analysis. Detailed statistical analysis plan is provided in the Supplementary Appendix (COVID-19 Antiviral Domain SAP). The primary model was run by an unblinded Statistical Analysis Committee, who conduct all protocol-specified trial update analyses independently of the ITSC, reporting results directly to the DSMB (Supplementary appendix).
The primary analysis was intention-to-treat, with a Bayesian cumulative logistic model with neutral prior distributions for treatment effects. The model estimated the proportional odds ratio for the ordinal primary outcome of organ support-free days. The primary analysis was adjusted for location (site, nested within country), age (categorized into six groups), sex, and time period (2-week calendar epochs). The primary analysis was conducted on the REMAP-CAP Severe State cohort, including any patient randomized to at least one domain as of November 19, 2020 (Supplementary Appendix, Table S3). This approach allowed maximal incorporation of all information, providing a robust estimation of the coefficients of all covariates, as per the REMAP-CAP design [24]. Lopinavir-ritonavir and hydroxychloroquine were modeled hierarchically to allow for borrowing among the interventions' effect estimates. This meant that the effects of lopinavir-ritonavir and hydroxychloroquine shared a mean representing a common “antiviral effect”. Distinct intervention-specific effects were estimated but the effects of lopinavir-ritonavir and hydroxychloroquine were shrunk toward the overall estimate of antiviral effect based on the heterogeneity of effects in the data. The combination therapy effect was estimated as the sum of the lopinavir-ritonavir and hydroxychloroquine and effects with an interaction effect between lopinavir-ritonavir and hydroxychloroquine.
The analysis of the primary outcome was repeated in models restricted to patients in the Unblinded cohort, which included severe COVID-19 patients randomized to the COVID-19 Antiviral Therapy Domain or other previously reported interventions and domains (Corticosteroid Domain and reported arms of the Immune Modulation Therapy Domain). We conducted additional analyses restricting to patients who were randomized concurrently with the lopinavir-ritonavir group or with hydroxychloroquine and combination therapy groups. Other analyses were conducted excluding those who tested negative for SARS-CoV-2, those in the COVID-19 Antiviral Therapy Domain cohort with no adjustment for assignment to interventions in other domains, and on the per-protocol cohort (Supplementary Appendix, Table S3). Additional secondary and sensitivity analyses of the primary outcome are described in the Supplementary Appendix.
Similar primary, secondary, and sensitivity analyses were conducted to estimate the effect on hospital survival. Interactions of antiviral interventions with corticosteroid therapy and with IL-6 receptor antagonists (tocilizumab, sarilumab) were modeled. The effect of antiviral interventions on secondary outcomes was assessed using the Unblinded cohort (defined above).
The Bayesian analysis models result in posterior distributions for parameters of interest including proportional odds ratios. Results from models of ordinal and dichotomous endpoints are reported as posterior median odds ratios (OR) and 95% credible intervals. Results from models of time-to-event endpoints are reported as posterior median hazard ratios (HR) and 95% CrIs. For consistency of interpretation, all models are parameterized so that an OR/HR greater than 1 indicates patient benefit relative to the control group, and an OR/HR less than 1 indicates patient harm relative to the control group. The model allows the calculation of the posterior probability that each COVID-19 Antiviral Therapy Domain intervention (including the control group) was optimal, superior to control (OR/HR > 1), harmful (OR/HR < 1) or futile (OR/HR < 1.2). In this manuscript, we present the posterior probabilities of futility for the primary models and harm for all models; the posterior probabilities of being optimal or superior are available in the Statistical Analysis Committee Primary Analysis Report and ITSC Secondary Analysis Report in the Supplementary Appendix. An intervention was deemed harmful if the posterior probability of harm compared to control was greater than 90% (REMAP-CAP Pandemic Appendix to the Core Protocol-Supplementary Appendix). There was no imputation of missing primary (or secondary) outcomes.
Role of the funding source
The funders of the study had no role in study design, data collection, data analysis, data interpretation, or writing of the report. The unblinded Statistical Analysis Committee had full access to all the data in the study and all authors had final responsibility for the decision to submit for publication.
Results
Patients
Enrollment into the REMAP-CAP pandemic stratum started on March 9, 2020, and into the four arms of the COVID-19 Antiviral Therapy Domain on April 8, 2020, with patients enrolled from 99 sites across 8 countries (Table S1, Supplementary Appendix). Enrollment into the hydroxychloroquine and combination therapy arms was halted temporarily on May 23, 2020, based on published concerns regarding the safety and efficacy of hydroxychloroquine, but resumed later in a few sites, although only three patients (two in the hydroxychloroquine arm and one in the combination therapy arm) were enrolled after May 23, 2020, from one site. The hydroxychloroquine and combination therapy arms were closed completely on July 13, 2020. Enrollment into the lopinavir-ritonavir arm was halted on November 19, 2020, after reaching the prespecified futility threshold. Enrollment into the Corticosteroid Therapy Domain was halted on June 17-2020, while the COVID-19 Antiviral Therapy Domain was actively enrolling into the lopinavir-ritonavir and control groups, and enrollment into no immune modulation intervention in the Immune Modulation Domain was halted on November 19, 2020, simultaneously with lopinavir-ritonavir based on the results of the adaptive analysis. The reports of corticosteroids and IL-6 receptor antagonists (tocilizumab and sarilumab) have been published [29, 30].
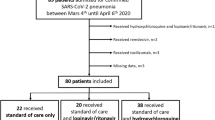
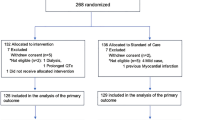
During the study period, 2046 patients with suspected or confirmed COVID-19 were enrolled in one or more REMAP-CAP domains (Fig. 1, Table S1, Supplementary Appendix), with 726 patients randomized within the COVID-19 Antiviral Therapy Domain (268 assigned to lopinavir-ritonavir, 52 to hydroxychloroquine, 29 to combination therapy of lopinavir-ritonavir and hydroxychloroquine and 377 to control). Within this domain, there were 32 patients for whom consent was withdrawn or not obtained and 17 patients with unavailable follow-up data on the primary outcome. As a result, 694 were included in this report, of whom 677 were analyzed for the primary outcome. Of the included patients, 502/694 (72.3%) were enrolled from the United Kingdom, 100/694 (14.4%) from Saudi Arabia, 42/694 (6.1%) from Canada, and remaining from other countries (Table S1).
Screening, randomization, and follow-up of patients in the REMAP-CAP COVID-19 Antiviral Therapy Domain randomized controlled trial. aPatients could meet more than one ineligibility criterion (Table S2, Supplementary Appendix). bDetails of platform exclusions are provided in the Supplementary Results (Supplementary Appendix). cThe primary analysis of organ support-free days (OSFD) and hospital survival were conducted on the REMAP-CAP intention-to-treat cohort which included all patients enrolled in the trial who met COVID-19 severe state criteria and were randomized within at least one domain, adjusting for patient factors and for assignment to interventions in other domains (Table S3, Supplementary Appendix). ^Contraindications include hypersensitivity, receiving the study drug as usual medication prior to hospitalization, human immune deficiency (HIV) infection (contraindication of lopinavir-ritonavir), severe liver failure (contraindication of lopinavir-ritonavir), receiving amiodarone as a usual medication prior to this hospitalization or any administration of amiodarone within the 72 h prior to assessment (contraindication of lopinavir-ritonavir) and high clinical risk of sustained ventricular dysrhythmia (contraindication of hydroxychloroquine) (Table S2, Supplementary Appendix)
The baseline characteristics were balanced across patients randomized concurrently with lopinavir-ritonavir (Table 1) and across patients randomized concurrently with hydroxychloroquine and combination therapy (Table S4). Of enrolled patients, 689/693 (99.4%) were receiving respiratory support (high-flow nasal cannula, noninvasive or invasive ventilation or ECMO) and 137/693 (19.8%) were receiving vasopressor support.
Intervention fidelity
Information on lopinavir-ritonavir and hydroxychloroquine dosing during the study period were available for 665/694 (95.8%) of patients (Tables S5 and S6, Supplementary Appendix). Among those assigned to the lopinavir-ritonavir, 220/247 (89.1%) received the allocated intervention for 7 days (5–12), among those assigned to hydroxychloroquine 46/49 (93.9%) received the allocated intervention for 7 days (5–12), among patients assigned to combination therapy 20/24 (83.3) received the allocated intervention for 11.5 days (5.8–14) and among those assigned to control group 360/362 (99.4%) received the allocated intervention (Tables S5 and S6, Supplementary Appendix). Concomitant therapy with corticosteroids, IL-6 receptor antagonists (Tocilizumab and Sarilumab), and remdesivir across patients randomized concurrently with lopinavir-ritonavir (Table S5, Supplementary Appendix) and across patients randomized concurrently with hydroxychloroquine and combination therapy (Table S6, Supplementary Appendix) were generally balanced.
Primary outcome
The median (IQR) organ support-free days among patients in lopinavir-ritonavir, hydroxychloroquine, and combination therapy groups were 4 (− 1 to 15), 0 (− 1 to 9) − 1 (− 1 to 7), respectively, compared to 6 (− 1 to 16) days in the control group (Table 2, Fig. 1). Compared with control, the corresponding median adjusted ORs (95% CrI) were 0.73 (0.55–0.99) for lopinavir-ritonavir, 0.57 (0.35–0.83) for hydroxychloroquine and 0.41 (0.24–0.72) for combination therapy, yielding posterior probabilities that reached the criteria for futility (all 99.9% or greater), yielding high posterior probabilities of harm (98%, 99.9% and > 99.9%, respectively, Table 2). In-hospital mortality among patients in lopinavir-ritonavir, hydroxychloroquine, combination therapy was 88/249 (35.3%), 17/49 (34.7%), 13/26 (50%), respectively, compared to 106/353 (30%) in the control group (Table 2, Fig. 2). In the primary analysis of hospital survival, the three interventions decreased survival compared to control, with the corresponding median adjusted ORs (95% CrI) of 0.65 (0.45–0.95), 0.56 (0.36–0.89), 0.36 (0.17–0.73), respectively, yielding high probabilities of harm (98.5% and 99.4% and 99.8%, respectively, Table 2). Estimates from secondary and sensitivity analyses of the organ support-free days and hospital survival, including analyses restricting to concurrent controls of lopinavir-ritonavir and concurrent controls of hydroxychloroquine/combination therapy groups were consistent with the primary analyses (Figure S1, Tables S7 and S8 in Supplementary appendix).
Organ support-free days and mortality. A Organ support-free days in patients allocated to lopinavir-ritonavir, hydroxychloroquine, combination therapy and control among critically ill patients in the COVID-19 Antiviral Therapy Domain of the REMAP-CAP trial. Distributions of organ support-free days are displayed as the cumulative proportion (y axis) for each study group by day (x axis). Curves that rise more slowly are more favorable. The height of each curve at “ − 1” indicates the in‐hospital mortality for each intervention. The height of each curve at any time point indicates the proportion of patients who had that number of organ support-free days or fewer. The difference in the height of the curves at any point represents the difference in the percentile in the distribution of organ support-free days associated with that number of days alive and free of organ support. B Organ support-free days are displayed as horizontally stacked proportions by study group. Red represents worse values and blue represents better values. On primary analysis of organ support-free days, the three interventions decreased organ support-free days compared to control, with corresponding median adjusted ORs and 95% credible intervals of 0.73 (0.55–0.99), 0.57 (0.35–0.83) and 0.41 (0.24–0.72), respectively, yielding high posterior probabilities of futility (99% or greater) and high posterior probabilities of harm compared to control (98%, 99.9% and > 99.9%, respectively). C Empirical distribution of survival for lopinavir–ritonavir, hydroxychloroquine, combination therapy and control. Lopinavir-ritonavir, hydroxychloroquine and combination therapy resulted in reduced survival over 90 days compared to control, with adjusted median hazard ratios (95% CrI) of 0.83 (0.65, 1.07), 0.71 (0.45, 0.97), 0.58 (0.36, 0.92), yielding high probabilities of harm compared with control of 92% and 98.4% and 98.7%, respectively
Secondary outcomes
Lopinavir-ritonavir, hydroxychloroquine, and combination therapy resulted in a longer time to both ICU and hospital discharge compared with control and reduced survival over 90 days. All secondary outcome analyses yielded high posterior probabilities of harm (Table 3). The distribution of SARS-CoV-2 RNA clearance among patients randomized to receive lopinavir–ritonavir, hydroxychloroquine, combination therapy, and control was not visually different (Figure S2, Supplementary Appendix). The full model was not performed for this outcome because of limited follow-up reverse transcription-polymerase chain reaction (RT-PCR) data.
Safety outcomes
Serious adverse events were reported in 13/255 (5.1%) patients randomized to lopinavir-ritonavir, 3/50 (6%) to hydroxychloroquine, 1/27 (3.7%) to combination therapy, and 12/362 (3.3%) to control. Serious ventricular arrhythmia or sudden unexpected death was reported in 6/239 (2.5%) patients randomized to lopinavir-ritonavir, 2/49 (4.1%) to hydroxychloroquine, 2/26 (7.7%) to combination therapy, and 10/435 (2.9%) to control (Table 3).
Subgroup analyses and interactions with corticosteroids and IL-6 antagonists
The effects of lopinavir-ritonavir, hydroxychloroquine and combination therapy on the primary outcome were similar across patients who were mechanically ventilated or not, and patients who were in shock or not, at the time of enrollment (Tables S9 and S10, Supplementary Appendix). There was no meaningful interaction between treatment with lopinavir-ritonavir, hydroxychloroquine, or combination therapy and the effects of corticosteroids or IL-6 receptor antagonists on organ support-free days or hospital survival. (Table S11, Table S12, and Statistical Analysis Committee Primary Analysis Report, Supplementary Appendix).
Discussion
Among critically ill patients with COVID-19, treatment with lopinavir-ritonavir, hydroxychloroquine or combination therapy did not improve outcomes and demonstrated a high probability of being harmful. The findings were robust on sensitivity analyses, including analyses restricting to patients randomized concurrently with lopinavir-ritonavir arm or patients randomized concurrently hydroxychloroquine/combination therapy arms, and were consistent across secondary outcomes. Treatment with lopinavir-ritonavir, hydroxychloroquine, or combination therapy demonstrated similar harm regardless of concomitant therapy with corticosteroids or IL-6 receptor antagonists with no differential effects across assignments to these therapies.
The observed clinical findings are discordant with in vitro data that demonstrate antiviral activity against SARS-CoV-2 [9,10,11]. This may be related to several factors. It is unclear whether standard doses of lopinavir-ritonavir and hydroxychloroquine achieve adequate, safe and sustainable SARS-CoV-2 inhibitory concentrations in the lung and plasma as predicted by pharmacokinetic studies [12, 31, 32]. Both lopinavir-ritonavir and hydroxychloroquine are known for drug interactions and for their effects on prolonging QT prolongation and inducing cardiac arrhythmia. Hydroxychloroquine could worsen acute organ injury in critically ill patients with COVID-19 by inhibiting autophagy [33]. Additionally, ritonavir may increase the blood levels of hydroxychloroquine, further increasing the risk of adverse events with combination therapy [34]. We did not document significantly higher reports of serious ventricular arrhythmia or sudden unexpected death, but this analysis may be limited by the low number of events.
Previous studies have demonstrated a lack of benefit of lopinavir-ritonavir and hydroxychloroquine among hospitalized patients. These trials included predominantly patients admitted to hospital wards [19, 20]. For example, 4% of patients in the RECOVERY trial were receiving invasive mechanical ventilation, and 9% of patients in the Solidarity trial were mechanically ventilated at enrollment. On the other hand, REMAP-CAP which enrolled critically ill patients with COVID-19 receiving respiratory or cardiovascular support demonstrates a high probability of harm with these treatments. The observed harm in the current trial may reflect the fact that critically ill patients are generally at a higher risk for harm compared to those who are less ill and are hospitalized on the wards [35]. Additionally, treatment at a later time point in the disease course, when the patient becomes critically ill, may correspond to viral replication becoming a less prominent feature in the disease pathogenesis, at which point the harm of antiviral therapy outweighs any potential benefit. The consistent findings from different sensitivity analyses, including the model restricted to patients in the COVID-19 Antiviral Therapy Domain, demonstrated the robustness of the findings.
This study highlights some of the features of the adaptive platform trial design used in REMAP-CAP. The adaptive platform trial design allows efficient enrollment into multiple therapeutic domains simultaneously and studying interactions with several agents; a feature that explains its increasing use in other medical fields including oncology and psychiatry. The design has the flexibility to allow different interventions to be added or removed into the platform, and to allow sites to choose some or all interventions, based on the local drug availability and equipoise. These features, along with the multicenter, multinational pragmatic conduct, contribute to the efficiency of the trial and the generalizability of the results, thus facilitating quick answers to multiple questions; a highly desirable feature during a global pandemic. Our study also illustrates the efficiency that is associated with the REMAP-CAP design; the ongoing recruitment of patients into the platform even after the hydroxychloroquine interventions stopped enrolling provided more information to be included in the analytical model, with appropriate adjustment for time, to inform specific treatment effects [36, 37]. The real-time adaptive analyses, which are based on data from patients with completed outcome information, allow quick decisions about halting interventions upon reaching futility thresholds. In the case of lopinavir-ritonavir, enrollment was halted once the futility threshold was met based on available data at the time of the adaptive analysis. By definition of the statistical triggers, the futility trigger must occur prior to the harm trigger. Because of this ordered relationship, the pre-specified trigger for harm is only evaluated at the final analysis while the futility trigger is evaluated at adaptive and final analyses. Once outcome data on the remaining patients were completed, the final analysis demonstrated that the intervention was not only futile, but also harmful. This feature of frequent adaptive analyses allows for ongoing assessment for futility, thus reducing the unnecessary exposure of additional patients to non-effective or harmful therapies, compared to standard RCT. The drawback of this study design is that study groups may end up unequal in size, may not be entirely concurrent in time, or balanced in some of the baseline characteristics despite equal randomization at any given point [38]. In our study, this explains the different sizes of the study groups. Additionally, patients were enrolled in the hydroxychloroquine and combination therapy groups at a time when ICUs were under strain and corticosteroid therapy was not the standard of care. To address these recognized issues with the adaptive platform design, the primary model adjusted for time and site and corticosteroid therapy. To further address the possible effect of concurrent control, we conducted additional analysis restricted to the concurrent controls of lopinavir-ritonavir and to the concurrent controls of hydroxychloroquine and combination therapy groups. These analyses demonstrated that baseline characteristics (including invasive mechanical ventilation) and co-interventions (including corticosteroids and remdesivir) were generally balanced between intervention groups and respected concurrent controls, and that the treatment effects are consistent results with the primary analysis. To limit potential sources of bias, we used a centralized randomization with concealed allocation and performed analysis based on the intention-to-treat principle. In addition, all analyses were specified prior to unblinding results. The study has limitations. Enrollment into the hydroxychloroquine and combination therapy study arms was halted before reaching any pre-specified internal trigger but based on external evidence. While the small sample size is a limitation of the current study, the strong signal observed in the small number of patients results in a high probability of harm. Data on the bioavailability of dissolved or crushed lopinavir-ritonavir tablets in critically ill patients are limited. The study used an open-label design, although clinician and patient awareness of study assignment likely had minimal effect on the organ support or mortality components of the primary outcome.
In conclusion, among critically ill patients with COVID-19, treatment with lopinavir-ritonavir, hydroxychloroquine, or combination therapy resulted in worse outcomes compared to no COVID-19 antiviral therapy.
Availability of data and material
Qualified researchers registered with an appropriate institution can request access to deidentified patient data after 9 months of publication through submission of a proposal to the corresponding author. The proposal will be reviewed and approved by the REMAP-CAP ITSC to ensure that any proposed publication is of high quality, honours the commitments made to the study patients in the consent documentation and ethical approvals, and is compliant with sponsor restrictions and relevant legal and regulatory requirements (e.g., relating to data protection and privacy). The ITSC committee will have the right to review and comment on any draft manuscripts before publication. A contract will also be signed.
References
World Health Organization. WHO Coronavirus (COVID-19) Dashboard: https://covid19.who.int/?adgroupsurvey=%7Badgroupsurvey%7D&gclid=Cj0KCQjwk4yGBhDQARIsACGfAesHuE0vTu-elrNpB95aO6wpEOC11Or3vRsIirn4MG8cGxi477Qb1pYaAnypEALw_wcB. Acessed 11 June 2021
Horie S, McNicholas B, Rezoagli E, Pham T, Curley G, McAuley D, O’Kane C, Nichol A, Dos Santos C, Rocco PRM, Bellani G, Laffey JG (2020) Emerging pharmacological therapies for ARDS: COVID-19 and beyond. Intensive Care Med 46:2265–2283
de Wilde AH, Jochmans D, Posthuma CC, Zevenhoven-Dobbe JC, van Nieuwkoop S, Bestebroer TM, van den Hoogen BG, Neyts J, Snijder EJ (2014) Screening of an FDA-approved compound library identifies four small-molecule inhibitors of Middle East respiratory syndrome coronavirus replication in cell culture. Antimicrob Agents Chemother 58:4875–4884
Chu CM, Cheng VC, Hung IF, Wong MM, Chan KH, Chan KS, Kao RY, Poon LL, Wong CL, Guan Y, Peiris JS, Yuen KY, Group HUSS (2004) Role of lopinavir/ritonavir in the treatment of SARS: initial virological and clinical findings. Thorax 59:252–256
Chan JF, Yao Y, Yeung ML, Deng W, Bao L, Jia L, Li F, Xiao C, Gao H, Yu P, Cai JP, Chu H, Zhou J, Chen H, Qin C, Yuen KY (2015) Treatment with lopinavir/ritonavir or interferon-beta1b improves outcome of MERS-CoV infection in a nonhuman primate model of common marmoset. J Infect Dis 212:1904–1913
Arabi YM, Asiri AY, Assiri AM, Balkhy HH, Al Bshabshe A, Al Jeraisy M, Mandourah Y, Azzam MHA, Bin Eshaq AM, Al Johani S, Al Harbi S, Jokhdar HAA, Deeb AM, Memish ZA, Jose J, Ghazal S, Al Faraj S, Al Mekhlafi GA, Sherbeeni NM, Elzein FE, Al-Hameed F, Al Saedi A, Alharbi NK, Fowler RA, Hayden FG, Al-Dawood A, Abdelzaher M, Bajhmom W, AlMutairi BM, Hussein MA, Alothman A, Saudi Critical Care Trials G (2020) Interferon beta-1b and lopinavir-ritonavir for middle east respiratory syndrome. N Engl J Med 383:1645–1656
Bouadma L, Lescure FX, Lucet JC, Yazdanpanah Y, Timsit JF (2020) Severe SARS-CoV-2 infections: practical considerations and management strategy for intensivists. Intensive Care Med 46:579–582
Arabi YM, Fowler R, Hayden FG (2020) Critical care management of adults with community-acquired severe respiratory viral infection. Intensive Care Med 46:315–328
Choy KT, Wong AY, Kaewpreedee P, Sia SF, Chen D, Hui KPY, Chu DKW, Chan MCW, Cheung PP, Huang X, Peiris M, Yen HL (2020) Remdesivir, lopinavir, emetine, and homoharringtonine inhibit SARS-CoV-2 replication in vitro. Antiviral Res 178:104786
Yao X, Ye F, Zhang M, Cui C, Huang B, Niu P, Liu X, Zhao L, Dong E, Song C, Zhan S, Lu R, Li H, Tan W, Liu D (2020) In vitro antiviral activity and projection of optimized dosing design of hydroxychloroquine for the treatment of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Clin Infect Dis 71:732–739
Wang M, Cao R, Zhang L, Yang X, Liu J, Xu M, Shi Z, Hu Z, Zhong W, Xiao G (2020) Remdesivir and chloroquine effectively inhibit the recently emerged novel coronavirus (2019-nCoV) in vitro. Cell Res 30:269–271
Arshad U, Pertinez H, Box H, Tatham L, Rajoli RKR, Curley P, Neary M, Sharp J, Liptrott NJ, Valentijn A, David C, Rannard SP, O’Neill PM, Aljayyoussi G, Pennington SH, Ward SA, Hill A, Back DJ, Khoo SH, Bray PG, Biagini GA, Owen A (2020) Prioritization of Anti-SARS-Cov-2 drug repurposing opportunities based on plasma and target site concentrations derived from their established human pharmacokinetics. Clin Pharmacol Ther 108:775–790
Park SJ, Yu KM, Kim YI, Kim SM, Kim EH, Kim SG, Kim EJ, Casel MAB, Rollon R, Jang SG, Lee MH, Chang JH, Song MS, Jeong HW, Choi Y, Chen W, Shin WJ, Jung JU, Choi YK (2020) Antiviral efficacies of FDA-approved drugs against SARS-CoV-2 infection in ferrets. mBio 11
Gonzalez Cortes R, Garcia-Salido A, Roca Pascual D, Slocker Barrio M, de Carlos Vicente JC, Patients SSGoS-C-iCIP (2020) A multicenter national survey of children with SARS-CoV-2 infection admitted to Spanish Pediatric Intensive Care Units. Intensive Care Med 46:1774–1776
Wang K, Zhang Z, Yu M, Tao Y, Xie M (2020) 15-day mortality and associated risk factors for hospitalized patients with COVID-19 in Wuhan, China: an ambispective observational cohort study. Intensive Care Med 46:1472–1474
Tu WJ, Cao J, Yu L, Hu X, Liu Q (2020) Clinicolaboratory study of 25 fatal cases of COVID-19 in Wuhan. Intensive Care Med 46:1117–1120
Dagens A, Sigfrid L, Cai E, Lipworth S, Cheng V, Harris E, Bannister P, Rigby I, Horby P (2020) Scope, quality, and inclusivity of clinical guidelines produced early in the covid-19 pandemic: rapid review. BMJ 369:m1936
Food and Drug Administration (FDA). https://www.fda.gov/media/138945/download. Accessed 27 Dec 2020
Axfors C, Schmitt AM, Janiaud P et al (2021) Mortality outcomes with hydroxychloroquine and chloroquine in COVID-19 from an international collaborative meta-analysis of randomized trials. Nat Commun 12:2349
Siemieniuk RA, Bartoszko JJ, Ge L et al (2020) Drug treatments for covid-19: living systematic review and network meta-analysis. BMJ 370:m2980
Pan H, Peto R, Henao-Restrepo AM et al (2021) Repurposed antiviral drugs for covid-19—Interim WHO Solidarity Trial Results. N Engl J Med 384:497–511
RECOVERY Collaborative Group, Horby P, Mafham M, Linsell L, Bell JL, Staplin N, Emberson JR, Wiselka M, Ustianowski A, Elmahi E, Prudon B, Whitehouse T, Felton T, Williams J, Faccenda J, Underwood J, Baillie JK, Chappell LC, Faust SN, Jaki T, Jeffery K, Lim WS, Montgomery A, Rowan K, Tarning J, Watson JA, White NJ, Juszczak E, Haynes R, Landray MJ (2020) Effect of hydroxychloroquine in hospitalized patients with covid-19. N Engl J Med 383:2030–2040
RECOVERY Collaborative Group (2020) Lopinavir-ritonavir in patients admitted to hospital with COVID-19 (RECOVERY): a randomised, controlled, open-label, platform trial. Lancet
Angus DC, Berry S, Lewis RJ, Al-Beidh F, Arabi Y, van Bentum-Puijk W, Bhimani Z, Bonten M, Broglio K, Brunkhorst F, Cheng AC, Chiche JD, De Jong M, Detry M, Goossens H, Gordon A, Green C, Higgins AM, Hullegie SJ, Kruger P, Lamontagne F, Litton E, Marshall J, McGlothlin A, McGuinness S, Mouncey P, Murthy S, Nichol A, O’Neill GK, Parke R, Parker J, Rohde G, Rowan K, Turner A, Young P, Derde L, McArthur C, Webb SA (2020) The REMAP-CAP (randomized embedded multifactorial adaptive platform for community-acquired pneumonia) study. rationale and design. Ann Am Thorac Soc 17:879–891
Best BM, Capparelli EV, Diep H, Rossi SS, Farrell MJ, Williams E, Lee G, van den Anker JN, Rakhmanina N (2011) Pharmacokinetics of lopinavir/ritonavir crushed versus whole tablets in children. J Acquir Immune Defic Syndr 58:385–391
Staff PM (2020) Correction: COVID-19 prevention and treatment: a critical analysis of chloroquine and hydroxychloroquine clinical pharmacology. PLoS Med 17:e1003445
Laterre PF, Berry SM, Blemings A, Carlsen JE, Francois B, Graves T, Jacobsen K, Lewis RJ, Opal SM, Perner A, Pickkers P, Russell JA, Windelov NA, Yealy DM, Asfar P, Bestle MH, Muller G, Bruel C, Brule N, Decruyenaere J, Dive AM, Dugernier T, Krell K, Lefrant JY, Megarbane B, Mercier E, Mira JP, Quenot JP, Rasmussen BS, Thorsen-Meyer HC, Vander Laenen M, Vang ML, Vignon P, Vinatier I, Wichmann S, Wittebole X, Kjolbye AL, Angus DC, Investigators S-A (2019) Effect of selepressin vs placebo on ventilator- and vasopressor-free days in patients with septic shock: the SEPSIS-ACT randomized clinical trial. JAMA 322:1476–1485
WHO Working Group on the Clinical Characterisation and Management of COVID-19 infection (2020) A minimal common outcome measure set for COVID-19 clinical research. Lancet Infect Dis 20:e192–e197
Angus DC, Derde L, Al-Beidh F et al (2020) Effect of hydrocortisone on mortality and organ support in patients with severe COVID-19: the REMAP-CAP COVID-19 corticosteroid domain randomized clinical trial. Jama 324:1317–1329
REMAP-CAP Investigators, Gordon AC, Mouncey PR et al (2021) Interleukin-6 receptor antagonists in critically ill patients with covid-19. N Engl J Med 384:1491–1502
Painvin B, Guillot P, Verdier MC, Gacouin A, Maamar A (2020) Hydroxychloroquine pharmacokinetic in COVID-19 critically ill patients: an observational cohort study. Intensive Care Med 46:1772–1773
Marzolini C, Stader F, Stoeckle M, Franzeck F, Egli A, Bassetti S, Hollinger A, Osthoff M, Weisser M, Gebhard CE, Baettig V, Geenen J, Khanna N, Tschudin-Sutter S, Mueller D, Hirsch HH, Battegay M, Sendi P (2020) Effect of systemic inflammatory response to SARS-CoV-2 on lopinavir and hydroxychloroquine plasma concentrations. Antimicrob Agents Chemother 64
Edelstein CL, Venkatachalam MA, Dong Z (2020) Autophagy inhibition by chloroquine and hydroxychloroquine could adversely affect acute kidney injury and other organ injury in critically ill patients with COVID-19. Kidney Int 98:234–235
Pastick KA, Okafor EC, Wang F, Lofgren SM, Skipper CP, Nicol MR, Pullen MF, Rajasingham R, McDonald EG, Lee TC, Schwartz IS, Kelly LE, Lother SA, Mitja O, Letang E, Abassi M, Boulware DR (2020) Review: hydroxychloroquine and chloroquine for treatment of SARS-CoV-2 (COVID-19). Open Forum Infect Dis 7:ofaa130
Perner A, Tirupakuzhi Vijayaraghavan BK, Venkatesh B (2020) How likely are COVID-19 interventions to benefit the sickest patients? Intensive Care Med 46:1441–1444
Bittl John A, He Y (2017) Bayesian analysis: a practical approach to interpret clinical trials and create clinical practice guidelines. Circ Cardiovasc Qual Outcomes 10:e003563
Quintana M, Viele K, Lewis RJ (2017) Bayesian analysis: using prior information to interpret the results of clinical trials. JAMA 318:1605–1606
Dodd LE, Freidlin B, Korn EL (2021) Platform trials—beware the noncomparable control group. N Engl J Med 384:1572–1573
Acknowledgements
We are grateful to the NIHR Clinical Research Network (UK), UPMC Health System Health Services Division (US), and the Direction de la Recherche Clinique et de l’Innovation de l’AP-HP (France) for their support of patient recruitment. We are grateful for the supply of study drugs to some of the sites by AbbVie. The views expressed in this publication are those of the author(s) and not necessarily those of the NHS, the National Institute for Health Research or the Department of Health and Social Care.
REMAP-CAP Trial Investigators & Collaborators: International Trial Steering Committee: Farah Al-Beidh, Derek Angus, Djillali Annane, Yaseen Arabi, Abi Beane, Wilma van Bentum-Puijk, Scott Berry, Zahra Bhimani, Marc Bonten, Charlotte Bradbury, Frank Brunkhorst, Meredith Buxton, Allen Cheng, Lennie Derde, Lise Estcourt, Herman Goossens, Anthony Gordon, Cameron Green, Rashan Haniffa, Francois Lamontagne, Patrick Lawler, Edward Litton, John Marshall, Colin McArthur, Daniel McAuley, Shay McGuinness, Bryan McVerry, Stephanie Montgomery, Paul Mouncey, Srinivas Murthy, Alistair Nichol, Rachael Parke, Jane Parker, Kathryn Rowan, Marlene Santos, Christopher Seymour, Alexis Turgeon, Anne Turner, Frank van de Veerdonk, Steve Webb (Chair), Ryan Zarychanski. Regional Management Committees: Australia and New Zealand: Yaseen Arabi, Lewis Campbell, Allen Cheng, Lennie Derde, Andrew Forbes, David Gattas, Cameron Green, Stephane Heritier, Peter Kruger, Edward Litton, Colin McArthur (Deputy Executive Director), Shay McGuinness (Chair), Alistair Nichol, Rachael Parke, Jane Parker, Sandra Peake, Jeffrey Presneill, Ian Seppelt, Tony Trapani, Anne Turner, Steve Webb (Executive Director), Paul Young. Canadian Regional Management Committee: Zahra Bhimani, Brian Cuthbertson, Rob Fowler, Francois Lamontagne, John Marshall (Executive Director), Venika Manoharan, Srinivas Murthy (Deputy Executive Director), Marlene Santos, Alexis Turgeon, Ryan Zarychanski. CRIT Care Asia (CCA) Regional Management Committee: Diptesh Aryal, Abi Beane (Chair), Arjen M Dondrop, Cameron Green, Rashan Haniffa (Executive Director), Madiha Hashmi, Issrah Jawad, Deva Jayakumar, John Marshall, Colin McArthur, Srinivas Murthy, Timo Tolppa, Vanessa Singh, Steve Webb. European Regional Management Committee: Farah Al-Beidh, Derek Angus, Djillali Annane, Wilma van Bentum-Puijk, Scott Berry, Marc Bonten (co-Executive Director), Frank Brunkhorst, Maurizio Cecconi, Lennie Derde (co-Executive Director and Chair), Stephan Ehrmann, Herman Goossens, Anthony Gordon, Colin McArthur, Paul Mouncey, Alistair Nichol, Lorraine Parker, Mathias Pletz, Pedro Póvoa, Gernot Rohde, Kathryn Rowan, Steve Webb. United States Regional Management Committee: Brian Alexander, Derek Angus (Executive Director), Kim Basile, Meredith Buxton (Chair), Timothy Girard, Christopher Horvat, David Huang, Kelsey Linstrum, Florian Mayr, Bryan McVerry, Stephanie Montgomery, Christopher Seymour. Regional Coordinating Centers: Australia, CCA region, and Saudi Arabia: The Australia and New Zealand Intensive Care Research Centre (ANZIC-RC), Monash University. Canada: St. Michael’s Hospital, Unity Health Toronto. Europe: University Medical Center Utrecht (UMCU). New Zealand: The Medical Research Institute of New Zealand (MRINZ). United States: Global Coalition for Adaptive Research (GCAR), and University of Pittsburgh Medical Center. CRIT Care Asia (CCA): NICS MORU. Domain-Specific Working Groups: Antibiotic and Macrolide Duration Domain-Specific Working Group: Richard Beasley, Marc Bonten, Allen Cheng (Chair), Nick Daneman, Lennie Derde, Robert Fowler, David Gattas, Anthony Gordon, Cameron Green, Peter Kruger, Colin McArthur, Steve McGloughlin, Susan Morpeth, Srinivas Murthy, Alistair Nichol, Mathias Pletz, David Paterson, Gernot Rohde, Steve Webb. Corticosteroid Domain-Specific Working Group: Derek Angus (Chair), Wilma van Bentum-Puijk, Lennie Derde, Anthony Gordon, Peter Kruger, Edward Litton, John Marshall, Colin McArthur, Srinivas Murthy, Alistair Nichol, Bala Venkatesh, Steve Webb. Influenza Antiviral Domain-Specific Working Group: Derek Angus, Scott Berry, Marc Bonten, Allen Cheng, Lennie Derde, Herman Goossens, Menno de Jong, John Marshall, Colin McArthur, Srinivas Murthy (Chair), Tim Uyeki, Steve Webb. COVID-19 Antiviral Domain-Specific Working Group: Derek Angus, Yaseen Arabi (Chair), Kenneth Baillie, Richard Beasley, Scott Berry, Marc Bonten, Allen Cheng, Menno de Jong, Lennie Derde, Eamon Duffy, Rob Fowler, Herman Goossens, Anthony Gordon, Cameron Green, Thomas Hills, Colin McArthur, Susan Morpeth, Srinivas Murthy, Alistair Nichol, Katrina Orr, Rachael Parke, Jane Parker, Asad Patanwala, Kathryn Rowan, Steve Tong, Tim Uyeki, Frank van de Veerdonk, Steve Webb. COVID-19 Immune Modulation Domain-Specific Working Group: Derek Angus, Yaseen Arabi, Kenneth Baillie, Richard Beasley, Scott Berry, Marc Bonten, Frank Brunkhorst, Allen Cheng, Nichola Cooper, Olaf Cremer, Menno de Jong, Lennie Derde (Chair), Eamon Duffy, James Galea, Herman Goossens, Anthony Gordon, Cameron Green, Thomas Hills, Andrew King, Helen Leavis, John Marshall, Florian Mayr, Colin McArthur, Bryan McVerry, Susan Morpeth, Srinivas Murthy, Mihai Netea, Alistair Nichol, Kayode Ogungbenro, Katrina Orr, Jane Parker, Asad Patawala, Ville Pettilä (Deputy Chair), Emma Rademaker, Kathryn Rowan, Manoj Saxena, Christopher Seymour, Wendy Sligl, Steven Tong, Tim Uyeki, Frank van de Veerdonk, Steve Webb, Taryn Youngstein. COVID-19 Immune Modulation -2 Domain-Specific Working Group: Derek Angus, Scott Berry, Lennie Derde, Cameron Green, David Huang, Florian Mayr, Bryan McVerry, Stephanie Montgomery, Christopher W. Seymour (Chair), Steve Webb. Therapeutic Anticoagulation Domain-Specific Working Group: Derek Angus, Diptesh Aryal, Scott Berry, Shilesh Bihari, Charlotte Bradbury, Marc Carrier, Dean Fergusson, Robert Fowler, Ewan Goligher (Deputy Chair), Anthony Gordon, Christopher Horvat, David Huang, Beverley Hunt, Devachandran Jayakumar, Anand Kumar, Mike Laffan, Patrick Lawler, Sylvain Lother, Colin McArthur, Bryan McVerry, John Marshall, Saskia Middeldorp, Zoe McQuilten, Matthew Neal, Alistair Nichol, Christopher Seymour, Roger Schutgens, Simon Stanworth, Alexis Turgeon, Steve Webb, Ryan Zarychanski (Chair). Vitamin C Domain-Specific Working Group: Neill Adhikari (Chair), Derek Angus, Djillali Annane, Matthew Anstey, Yaseen Arabi, Scott Berry, Emily Brant, Angelique de Man, Lennie Derde, Anthony Gordon, Cameron Green, David Huang, Francois Lamontagne (Chair), Edward Litton, John Marshall, Marie-Helene Masse, Colin McArthur, Shay McGuinness, Paul Mouncey, Srinivas Murthy, Rachael Parke, Alistair Nichol, Tony Trapani, Andrew Udy, Steve Webb. COVID-19 Immunoglobulin Domain-Specific Working Group: Derek Angus, Donald Arnold, Phillipe Begin, Scott Berry, Richard Charlewood, Michael Chasse, Mark Coyne, Jamie Cooper, James Daly, Lise Estcourt (Chair, UK lead), Dean Fergusson, Anthony Gordon, Iain Gosbell, Heli Harvala-Simmonds, Tom Hills (New Zealand lead), Christopher Horvat, David Huang, Sheila MacLennan, John Marshall, Colin McArthur (New Zealand lead), Bryan McVerry (USA lead), David Menon, Susan Morpeth, Paul Mouncey, Srinivas Murthy, John McDyer, Zoe McQuilten (Australia lead), Alistair Nichol (Ireland lead), Nicole Pridee, David Roberts, Kathryn Rowan, Christopher Seymour, Manu Shankar-Hari (UK lead), Helen Thomas, Alan Tinmouth, Darrell Triulzi, Alexis Turgeon (Canada lead), Tim Walsh, Steve Webb, Erica Wood, Ryan Zarychanski (Canada lead). Simvastatin Domain-Specific Working Group: Derek Angus, Yaseen Arabi, Abi Beane, Carolyn Calfee, Anthony Gordon, Cameron Green, Rashan Haniffa, Deva Jayakumar, Peter Kruger, Patrick Lawler, Edward Litton, Colin McArthur, Daniel McAuley (Chair), Bryan McVerry, Matthew Neal, Alistair Nichol, Cecilia O’Kane, Murali Shyamsundar, Pratik Sinha, Taylor Thompson, Steve Webb, Ian Young. Antiplatelet Domain-Specific Working Group: Derek Angus, Scott Berry, Shailesh Bihari, Charlotte Bradbury (Chair), Marc Carrier, Timothy Girard, Ewan Goligher, Anthony Gordon, Ghady Haidar, Christopher Horvat, David Huang, Beverley Hunt, Anand Kumar, Patrick Lawler, Patrick Lawless, Colin McArthur, Bryan McVerry, John Marshall, Zoe McQuilten, Matthew Neal, Alistair Nichol, Christopher Seymour, Simon Stanworth, Steve Webb, Alexandra Weissman, Ryan Zarychanski. Mechanical Ventilation Domain: Derek Angus, Wilma van Bentum-Puijk, Lewis Campbell, Lennie Derde, Niall Ferguson, Timothy Girard, Ewan Goligher, Anthony Gordon, Cameron Green, Carol Hodgson, Peter Kruger, John Laffey, Edward Litton, John Marshall, Colin McArthur, Daniel McAuley, Shay McGuinness, Alistair Nichol (Chair) Neil Orford, Kathryn Rowan, Ary Neto, Steve Webb. ACE-2 RAS Domain: Rebecca Baron, Lennie Derde, Slava Epelman, Claudia Frankfurter, David Gattas, Frank Gommans, Anthony Gordon, Rashan Haniffa, https://www.nihr.ac.uk/documents/urgent-public-health-group-members/24638#Members. REMAP-CAP was supported in Germany by the Deutsche Gesellschaft für Internistische Intensivmedizin und Notfallmedizin (DGIIN) / Center for Sepsis Control & Care (CSCC) network. REMAP-CAP was supported in France by the CRICS-TRIGGERSEP network. REMAP-CAP was supported in Ireland by the Irish Critical Care Clinical Trials Network and we acknowledge the contribution of Kate Ainscough, Kathy Brickell and Peter Doran. REMAP-CAP was supported in the Netherlands by the Research Collaboration Critical Care the Netherlands (RCC-Net). Site Investigators and Research Coordinators: Australia: The Alfred Hospital: Andrew Udy, PhD, Phoebe McCracken, MPH, Meredith Young, MPH, Jasmin Board, MPH, Emma Martin, BPharmSc; Ballarat Health Services: Khaled El-Khawas, FCICM, Angus Richardson, FCICM, Dianne Hill, BN GradCert(CritCare), Robert J Commons, PhD, Hussam Abdelkharim, FCICM; Bendigo Hospital: Cameron Knott, MBBS(Hons) GDipClinUS MClinEd FCICM FRACP, Julie Smith, GDipN(CritCare), Catherine Boschert, PGDip; Caboolture Hospital: Julia Affleck, MBiotech, Yogesh Apte, FCICM, Umesh Subbanna, FCICM, Roland Bartholdy, FCICM, Thuy Frakking, PhD; Campbelltown Hospital: Karuna Keat, MB BS(Hons), Deepak Bhonagiri, MD, Ritesh Sanghavi, MBBS, Jodie Nema, B.App.Sc.(Ag), Megan Ford, BSc; Canberra Hospital: Harshel G. Parikh, FCICM, Bronwyn Avard, MLMEd, Mary Nourse, PGCert(CritCare); Concord Repatriation General Hospital: Winston Cheung, MBChB, Mark Kol, MBBS, Helen Wong, RN, Asim Shah, MBChB, Atul Wagh, MBBS; Eastern Health (Box Hill, Maroondah & Angliss Hospitals): Joanna Simpson, FCICM FANZCA, Graeme Duke, FCICM, Peter Chan, FCICM, Brittney Carter, PGCert(CritCare), Stephanie Hunter, MN; Flinders Medical Centre: Shailesh Bihari, PhD, Russell D Laver, FCICM, Tapaswi Shrestha, MN, Xia Jin, MN; Fiona Stanley Hospital: Edward Litton, FCICM, Adrian Regli, FCICM, Susan Pellicano, PGCert, Annamaria Palermo, BA, Ege Eroglu, BSc(Hons); Footscray Hospital: Craig French, MBBS, Samantha Bates, RN GDipCritCare, Miriam Towns, MPH, Yang Yang, MBBS, Forbes McGain, PhD; Gold Coast University Hospital: James McCullough, FCICM, Mandy Tallott, MN; John Hunter Hospital: Nikhil Kumar, MBBS, Rakshit Panwar, FCICM, Gail Brinkerhoff, PGCert, Cassandra Koppen, BPharm, Federica Cazzola, MBBS; Launceston General Hospital: Matthew Brain, FCICM, FRACP, DDU; Sarah Mineall, MN; Lyell McEwin Hospital: Roy Fischer, FCICM, Vishwanath Biradar, FCICM, Natalie Soar, BSN; Logan Hospital: Hayden White, PhD, Kristen Estensen, MBBS, Lynette Morrison, PGCert(CritCare), Joanne Sutton, RN, Melanie Cooper, PGCert(CritCare); Monash Health (Monash Medical Centre, Dandenong Hospital & Casey Hospital): Yahya Shehabi, PhD, Wisam Al-Bassam, MBChB, Amanda Hulley, BSc; Umesh Kadam, MSc, Kushaharan Sathianathan, MSc; Nepean Hospital: Ian Seppelt, PhD, Christina Whitehead, MN, Julie Lowrey, BN, Rebecca Gresham, BN, Kristy Masters, BN; Princess Alexandra Hospital: Peter Kruger, PhD, James Walsham, FCICM, Mr Jason Meyer, BN, Meg Harward, MN, Ellen Venz, PGCert(CritCare); The Prince Charles Hospital: Kara Brady, MPharm, Cassandra Vale, GDipClinPharm, Kiran Shekar, PhD, Jayshree Lavana, FCICM, Dinesh Parmar, FCICM; The Queen Elizabeth Hospital: Sandra Peake, PhD, Patricia Williams, BN, Catherine Kurenda, RN; Rockhampton Hospital: Helen Miles, MBBS MPH FCICM, Antony Attokaran, MBBS FCICM FRACP; Royal Adelaide Hospital: Samuel Gluck, MD, Stephanie O’Connor, MNSc, Marianne Chapman, PhD, Kathleen Glasby, CCRN; Royal Darwin Hospital: Lewis Campbell, FCICM, Kirsty Smyth, PGCert(CritCare), Margaret Phillips, MN; Royal Melbourne Hospital: Jeffrey Presneill, PhD, Deborah Barge, CCRN, Kathleen Byrne, MNSc, Alana Driscoll GDipN(CritCare), Louise Fortune, MNSc; Royal North Shore Hospital: Pierre Janin, MD, Elizabeth Yarad, MN, Frances Bass, MSc, Naomi Hammond, PhD, Anne O’Connor, RN; Royal Perth Hospital: Sharon Waterson, PGCert(CritCare), Steve Webb, PhD, Robert McNamara, BMBS; Royal Prince Alfred Hospital: David Gattas, MMed(ClinEpid), Heidi Buhr, MScMed(ClinEpid), Jennifer Coles, GDipN(CritCare); Sir Charles Gardiner Hospital: Sacha Schweikert, FCICM, Bradley Wibrow, FCICM, Matthew Anstey, FCICM, Rashmi Rauniyar, MPH; St George Hospital: Kush Deshpande, FCICM, Pam Konecny, FRACP, Jennene Miller, BN, Adeline Kintono, BN, Raymond Tung B.Pharm, MPS, MSHP. St. John of God Midland Public and Private Hospitals: Ed Fysh, PhD, Ashlish Dawda, MD, Bhaumik Mevavala, MHA; St. John of God Hospital, Murdoch: Annamaria Palermo, BA, Adrian Regli, FCICM, Bart De Keulenaer, FCICM; St. John of God Hospital, Subiaco: Ed Litton, PhD, Janet Ferrier, BSc; St. Vincent’s Hospital (NSW): Priya Nair, PhD, Hergen Buscher, FCICM, Claire Reynolds, MClinNurse, Sally Newman, PGCert(CritCare); St. Vincent’s Hospital (VIC): John Santamaria, MDBS, Leanne Barbazza, PGCert(CritCare), Jennifer Homes, PGCert(CritCare), Roger Smith, MPH; Sunshine Coast University Hospital: Peter Garrett, FCICM, Lauren Murray, MSc, Jane Brailsford, PGCert(CritCare), Loretta Forbes, PGCert(CritCare), Teena Maguire, BA; Sunshine Hospital: Craig French, MBBS, Gerard Fennessy, MBBS, John Mulder, MBBS, Rebecca Morgan, RN PGCert(CritCare), Rebecca McEldrew, RN PGCert(CritCare); The Sutherland Hospital: Anas Naeem, MClinEd, Laura Fagan, GDipN(CritCare), Emily Ryan, PGCert(CritCare); Toowoomba Hospital: Vasanth Mariappa, FCICM, Judith Smith, PGCert; University Hospital Geelong: Scott Simpson, MBBS, Matthew Maiden, PhD, Allison Bone, GDipN(CritCare), Michelle Horton, MN, Tania Salerno, PGCert; Wollongong Hospital: Martin Sterba, PhD, Wenli Geng, MN; Belgium: Ghent University Hospital: Pieter Depuydt, Jan De Waele, , Liesbet De Bus,, Jan Fierens, Stephanie Bracke, Joris Vermassen, , Daisy Vermeiren. Canada: Brantford General Hospital: Brenda Reeve, MD, William Dechert, MSc; Centre de recherche de l’Institut universitaire de cardiologie et de pneumologie de Québec: Francois Lellouche, Patricia Lizotte. Centre Hospitalier de l’Universite de Montreal: Michaël Chassé, PhD, François Martin Carrier, MSc, Dounia Boumahni, BSc, Fatna Benettaib, MSc., Ali Ghamraoui, BSc; CHU de Québec – Université Laval: Alexis Turgeon, MSc, David Bellemare, BSc, Ève Cloutier, Rana Daher, François Lauzier, MSc, Charles Francoeur, MSc; Centre Hospitalier Universitaire de Sherbrooke: François Lamontagne, MD, Frédérick D’Aragon, MD, Elaine Carbonneau, BACC, Julie Leblond, BACC; Grace Hospital: Gloria Vazquez-Grande, Nicole Marten. Grand River Hospital (Kitchener): Theresa Liu, Atif Siddiqui. Health Sciences Centre, Winnipeg: Ryan Zarychanski, MD, Gloria Vazquez-Grande, MD, Nicole Marten, RN, Maggie Wilson, MSc; Hôpital du Sacré Coeur de Montréal: Martin Albert, MD, Karim Serri, MD, Alexandros Cavayas, MD, Mathilde Duplaix, MSc, Virginie Williams, PhD; Juravinski Hospital: Bram Rochwerg, MD, Tim Karachi, MD, Simon Oczkowski, MD, John Centofanti, MD, Tina Millen, RRT. McGill University Health Centre: Kosar Khwaja, Josie Campisi. Niagara Health (St. Catherine’s Hospital): Erick Duan, MD, Jennifer Tsang, MD, Lisa Patterson, BA; Regina General Hospital: Eric Sy, Chiraag Gupta, Sandy SHA Kassir. Royal Alexandra Hospital: Demetrios Kutsogiannis, Patricia Thompson. Sunnybrook Health Sciences Centre: Rob Fowler, Neill Adhikari, Maneesha Kamra, Nicole Marinoff. St. Boniface General Hospital: Ryan Zarychanski, Nicole Marten. St. Joseph’s Healthcare Hamilton: Deborah Cook, Frances Clarke. St. Mary's General Hospital (Kitchener): Rebecca Kruisselbrink, Atif Siddiqui. St. Michael’s Hospital: John Marshall, MD, Laurent Brochard, MD, Karen Burns, MD, Gyan Sandhu, RN, Imrana Khalid, MD. The Ottawa Hospital: Shane English, MSc, Irene Watpool, BScN, Rebecca Porteous, BSN, Sydney Miezitis, BSc, Lauralyn McIntyre, MSc; University Health Network: Elizabeth Wilcox, Lorenzo del Sorbo, Hesham Abdelhady, Tina Romagnuolo. University of Alberta: Wendy Sligl, Nadia Baig, Oleksa Rewa, Sean Bagshaw. William Osler Health System: Alexandra Binnie, MD, Elizabeth Powell, MD, Alexandra McMillan, MD, Tracy Luk, MD, Noah Aref, MSc. CCA: India Apollo Speciality Hospital—OMR, Chennai: Devachandran Jayakumar, MD, Suresh Babu BSc; Apollo Main Hospital, Chennai: C Vignesh, MD, Augustian James BSc. Apollo Speciality Vanagaram, Vanagaram, Chennai; R Ebenezer MD, S Krishnamurthy MD, Lakshmi Ranganathan PhD, Manisha, MD. Nepal Grande International Hospital : Sushil Khanal, MD, Sameena Amatya, RN; HAMS Hospital: Hem Raj Paneru, MD, Sabin Koirala, MD, Pratibha Paudel ,RN; Nepal Mediciti Hospital: Diptesh Aryal,MD, Kanchan Koirala,RN, Namrata Rai,RN, Subekshya Luitel, BSc; Tribhuvan University Teaching Hospital : Hem Raj Paneru,MD, Binita Bhattarai, RN; Pakistan (CCA): Ziauddin Hospital Clifton Campus: Madiha Hashmi, MD; Ashok Panjwani, MD; Zulfiqar Ali Umrani, Shoaib Siddiq; Mohiuddin Shaikh; National Institute of Cardiovascular Diseases Pakistan: Nawal Salahuddin, MD, Sobia Masood; Croatia: General Hospital Pozega: Zdravko Andric, Sabina Cviljevic, Renata Đimoti, Marija Zapalac, Gordan Mirković; University Hospital of Infectious Diseases “Dr Fran Milhajevid”: Bruno Baršić, Marko Kutleša, Viktor Kotarski; University Hospital of Zagreb: Ana Vujaklija Brajković, Jakša Babel, Helena Sever, Lidija Dragija, Ira Kušan; Finland: Helsinki University Hospital: Suvi Vaara, PhD, Leena Pettilä, Jonna Heinonen, Ville Pettilä, PhD; Tampere University Hospital: Anne Kuitunen, PhD, Sari Karlsson, PhD, Annukka Vahtera, PhD, Heikki Kiiski, PhD, Sanna Ristimäki; France: Ambroise Pare Hospital: Amine Azaiz, Cyril Charron, MD, Mathieu Godement, MD, Guillaume Geri, Antoine Vieillard-Baron; Centre Hospitalier de Melun: Franck Pourcine, Mehran Monchi; Centre Hospitalier Simone Veil, Beauvais: David Luis, MD, Romain Mercier, MD, Anne Sagnier, MD, Nathalie Verrier, MD, Cecile Caplin, MD, Jack Richecoeu, MD, Daniele Combaux, MD; Centre Hospitalier Sud Essonne: Shidasp Siami, PhD, Christelle Aparicio, Sarah Vautier, Asma Jeblaoui, Delphine Lemaire-Brunel; Centre Hospitalier Tenon: Muriel Fartoukh, MD, Laura Courtin, Vincent Labbe, MD , Guillaume Voiriot, MD, Sara Nesrine Salhi; Centre Hospitalier Victor Dupouy: Gaetan Plantefeve, MD, Cécile Leparco, RN, Damien Contou, MD; CHR d'Orleans: Grégoire Muller, MD, Mai-Anh Nay, MD, Toufik Kamel, MD, Dalila Benzekri, MD, Sophie Jacquier, MD, Isabelle Runge, MD, Armelle Mathonnet, MD, François Barbier, MD, Anne Bretagnol, MD; CHRU Tours Hopital Bretonneau: Emmanuelle Mercier, MD, Delphine Chartier, Charlotte Salmon, MD, Pierre-François Dequin, PhD, Denis GAROT, MD; CHU Dupuytren, Limoges study team. Hôpital Civil, Hôpitaux Universitaires de Strasbourg study team. Hôpital de Hautepierre, Hôpitaux Universitaires de Strasbourg: Francis Schneider, PhD, Vincent Castelain, PhD, Guillaume Morel, MD, Sylvie L’Hotellier, MSc; Hospital Nord Franche-Comté: Julio Badie, MD, Fernando Daniel Berdaguer, MD, Sylvain Malfroy, MD, Chaouki Mezher, MD, Charlotte Bourgoin, MSc, Guy Moneger, MD, Elodie Bouvier, MSc; Lariboisière Hospital: Bruno Megarbane, PhD, Sebastian Voicu, PhD, Nicolas Deye, PhD, Isabelle Malissin, MD, Laetitia Sutterlin, MD, Aymen Mrad, MD, Adrien Pépin Lehalleur, MD, Giulia Naim, MD, Philippe Nguyen, MD, Jean-Michel Ekhérian, MD, Yvonnick Boué, MD, Georgios Sidéris, PhD, Dominique Vodovar, PhD, Emmanuelle Guérin, MD, Caroline Grant, MD; Le Mans Hospital: Christophe Guitton, PhD, Cédric Darreau, MD, Mickaël Landais, MD, Nicolas Chudeau, MD, Alain Robert, PhD, Patrice Tirot, MD, Jean Christophe Callahan, MD, Marjorie Saint Martin, MD, Charlène Le Moal, MD, Rémy Marnai, MD, Marie Hélène Leroyer; Raymond Poincaré Hospital: Djillali Annane, MD, Pierre Moine, MD, Nicholas Heming, MD, Virginie Maxime, MD, Isabelle Bossard, MSc, Tiphaine Barbarin Nicholier, MD, Bernard Clair, MD, David Orlikowski, MD, Rania Bounab, MD, Lilia Abdeladim, MD; Vendee Hospital: Gwenhael Colin, MD, Vanessa Zinzoni, Natacha Maquigneau, Matthieu Henri-Lagarrigue, MD, Caroline Pouplet, MD; Germany: Carl-Thiem-Klinikum Cottbus gGmbH: Jens Soukup, PD, Richard Wetzold, Madlen Löbel, Dr. Ing, Lisa Starke, Patrick Grimm; Charité—Universitätsmedizin Berlin: André Finn, MD, Gabriele Kreß, Uwe Hoff, MD, Carl Friedrich Hinrichs, MD, Jens Nee, MD; Jena University Hospital: Mathias W. Pletz, PhD, Stefan Hagel, PhD, Juliane Ankert, MSc, Steffi Kolanos, BSc, Frank Bloos, PhD; Klinikum Dortmund gGmbH: Daniela Nickoleit-Bitzenberger, MD , Bernhard Schaaf, MD, Werner Meermeier, MD, Katharina Prebeg, Harun Said Azzaui, Martin Hower, Klaus-Gerd Brieger, Corinna Elender, Timo Sabelhaus, Ansgar Riepe, Ceren Akamp, Julius Kremling, Daniela Klein, Elke Landsiedel-Mechenbier; University Hospital of Leipzig: Sirak Petros, MD, Kevin Kunz, MD, Bianka Schütze, BSc; Universitätsklinikum Hamburg-Eppendorf: Stefan Kluge, MD, Axel Nierhaus, MD, Dominik Jarczak, MD, Kevin Roedl, MD; University Hospital of Frankfurt: Gernot Gerhard Ulrich Rohde, MD, Achim Grünewaldt, MD, Jörg Bojunga, MD; University Hospital of Wuerzburg: Dirk Weismann, MD, Anna Frey, MD; Maria Drayss, MD, M.E. Goebeler, MEG, Thomas Flor, Gertrud Fragner, Nadine Wahl, Juliane Totzke, Cyrus Sayehli, MD; Vivantes Klinikum Neukölln: Lorenz Reill, Michael Distler, MD, Astrid Maselli; Hungary: Almási Balogh Pál Hospital, Ózd: János Bélteczki, István Magyar, Ágnes Fazekas, Sándor Kovács, Viktória Szőke; Jósa András County Hospital, Nyíregyháza: Gábor Szigligeti, János Leszkoven; Ireland: Beacon Hospital Dublin: Daniel Collins, MRCPI, Kathy Brickell, RGN, Liadain Reid, MPH, Michelle Smyth, PgDip, Patrick Breen, MB FJFICMI, Sandra Spain, RGN; Beaumont Hospital: Gerard Curley; PhD, Natalie McEvoy, MSc, Pierce Geoghegan, MB, Jennifer Clarke, MB; Galway University Hospitals: John Laffey, MD, Bairbre McNicholas, PhD, Michael Scully, MD, Siobhan Casey, RN, Maeve Kernan, RN, Aoife Brennan, PhD, Ritika Rangan, PhD, Riona Tully, MB, Sarah Corbett, MB, Aine McCarthy, MB, Oscar Duffy, MB, David Burke, MB; St Vincent’s University Hospital, Dublin: Alistair Nichol, PhD, Kathy Brickell, RGN, Michelle Smyth, PGDip, Leanne Hayes, PhD, Liadain Reid, MPH, Lorna Murphy, RGN, Andy Neill, MB, Bryan Reidy, MSc, Michael O’Dwyer, PhD, Donal Ryan, MD, Kate Ainscough, PhD; Netherlands: Canisius Wilhelmina Ziekenhuis: Oscar Hoiting, MD, Marco Peters, MD, Els Rengers, MD, Mirjam Evers, RN, Anton Prinssen, RN; Deventer Hospital: Huub L.A. van den Oever, MD, Arriette Kruisdijk-Gerritsen, CCRN; Jeroen Bosch Ziekenhuis: Koen Simons, PhD, Tamara van Zuylen, RN, Angela Bouman, RN; Meander Medisch Centrum: Laura van Gulik, PhD; Radboud University Medical Center Nijmegen: Jeroen Schouten, PhD, Peter Pickkers, PhD, Noortje Roovers, BSc, Margreet Klop-Riehl, BSc, Hetty van der Eng, BSc; UMC Leiden: Evert de Jonge, PhD, Jeanette Wigbers, RN, Michael del Prado, RN; UMC Utrecht: Marc Bonten, PhD, Olaf Cremer, PhD, Lennie Derde, PhD, Diederik van Dijk, PhD, Emma Rademaker, MD, Jelle Haitsma Mulier, MD, Anna Linda Peters, PhD, Birgit Romberg, MD; Ziekenhuis Gelderse Vallei: Sjoerd van Bree, MD, Marianne Bouw-Ruiter, RN, Barbara Festen, MD, Fiona van Gelder, MD, Mark van Iperen, MD, Margreet Osinga, RN, Roel Schellaars, MD, Dave Tjan, MD, Ruben van der Wekken, MD, Max Melchers, MD, Arthur van Zanten, MD; New Zealand: Auckland City Hospital, Cardiothoracic and Vascular ICU: Shay McGuinness, MBChB, Rachael Parke, PhD, Eileen Guilder, MA, Magdalena Butler, RN, Keri-Anne Cowdrey, RN, Melissa Woollett, BHSc (Nurs); Auckland City Hospital, DCCM: Colin McArthur, FJFICM, Thomas Hills, DPhil, Lynette Newby, MN, Yan Chen, MN, Catherine Simmonds, PGDipHSc, Rachael McConnochie, MN, Caroline O’Connor; Christchurch Hospital: Jay Ritzema Carter, PhD, Seton Henderson, MD, Kymbalee Van Der Heyden, BSc, Jan Mehrtens, PGCert, Anna Morris, BN, Stacey Morgan, BN; Middlemore Hospital: Tony Williams, BMedSc, Alex Kazemi, BMedSc, Susan Morpeth, PhD, Rima Song, PGDip, Vivian Lai, MHSc, Dinuraj Girijadevi, PGCert; North Shore Hospital: Robert Everitt, FACEM, Robert Russell, BSc(Hons), Danielle Hacking, PGDipNurs; Rotorua Hospital: Ulrike Buehner, FCARCSI, Erin Williams, MSc; Tauranga Hospital: Troy Browne, FCICM, Kate Grimwade, FRACP, Jennifer Goodson, RN, Owen Keet, FANZCA, Owen Callender, FANZCA; Waikato Hospital: Robert Martynoga, FCICM, Kara Trask, PGCert, Amelia Butler, PGCert, Wellington Hospital: Paul Young, PhD, Chelsea Young, PGDip, Eden Lesona, MNSc, Shaanti Olatunji, MClinIm, Leanlove Navarra, BSc (Nurs), Raulle Sol Cruz, BSc (Nurs), Whangarei Hospital: Katherine Perry, FJFICM, Ralph Fuchs, FANZCA, Bridget Lambert, PGDip; Taranaki Base Hospital: Jonathan Albrett, FCICM, Carolyn Jackson, RN, Simon Kirkham, PGDip; Portugal: Hospital de Abrantes: Nuno José Teodoro Amaro dos Santos Catorze, MD, Tiago Nuno Alfaro Lima Pereira, MD, Ricardo Manuel Castro Ferreira, RN, Joana Margarida Pereira Sousa Bastos, PharmD, Teresa Margarida Oliveira Batista, RN; Romania: "Dr. Victor Babes" Clinical Hospital of Infectious and Tropical Diseases Bucharest: Simin Aysel Florescu, PhD, Delia Stanciu, MD, Mihaela Florentina Zaharia, MD, Alma Gabriela Kosa, MD, Daniel Codreanu; Saudi Arabia: King Abdulaziz Medical City- Riyadh: Yaseen M Arabi, MD, Eman Al Qasim, RN, MSN, Lolowa Alswaidan, MSc, Mohamed M Hegazy, MD, Hatim Arishi, MD, Ali Al Amri, MD, Samah Y AlQahtani, MBBS, Brintha Naidu, RN, Haytham Tlayjeh, MD, Sajid Hussain, MD, Farhan Al Enezi, MD, Sheryl Ann Abdukahil. Spain: Hospital del Mar: Rosana Muñoz-Bermúdez, MD, Judith Marin-Corral, PhD, Anna Salazar Degracia, PhD, Francisco Parrilla Gómez, MD, Maria Isabel Mateo López; Reina Sofia University Hospital: Rafael León López, MD, Jorge Rodriguez, PhD, Sheila Cárcel, Rosario Carmona, MD, Carmen de la Fuente, MD, Marina Rodriguez, MD; United Kingdom: Aberdeen Royal Infirmary: Callum Kaye, MBChB, Angela Allan, PGDip; Addenbrooke's Hospital: Charlotte Summers, PhD, Petra Polgarova MSc; Alder Hey Children’s NHS Foundation Trust: Stephen J McWilliam, PhD, Daniel B Hawcutt, MD, Laura Rad, BSc(Hons), Laura O’Malley, BSc(Hons), Jennifer Whitbread, BSc(Hons); Alexandra Hospital Redditch: Olivia Kelsall, MBChB, Nicholas Cowley MD, Laura Wild, BSc(Hons), Jessica Thrush, RGN, Hannah Wood, BSc(Hons), Karen Austin, RGN; Altnagelvin Hospital: Adrian Donnelly, FFICM, Martin Kelly, MD, Naoise Smyth MB ChB, Sinéad O’Kane, BSc(Hons), Declan McClintock, MSc, Majella Warnock, MPharm, Ryan Campbell BSc, Edmund McCallion MPharm; Antrim Area Hospital: Paul Johnson, FFARCSI, Shirley McKenna, MSc, Joanne Hanley, MSc, Andrew Currie, MSc, Barbara Allen, MPharm, Clare Mc Goldrick, MPhil, Moyra Mc Master, RGN, ; Barnet Hospital: Rajeev Jha, MD, Michael Kalogirou, MD, Christine Ellis, PhD, Vinodh Krishnamurthy, PhD, Vashish Deelchand, MSc, Aibhilin O’Connor, MSc; Basildon Universty Hospital: Dipak Mukherjee, MD, Agilan Kaliappan, MD, Anirudda Pai, MD,Mark Vertue, Anne Nicholson, Joanne Riches, Gracie Maloney, Lauren Kittridge, Amanda Solesbury, Kezia Allen. Belfast Health and Social Care Trust (Belfast City Hospital, Mater Infirmorium, Royal Victoria Hospital): Jon Silversides, PhD, Peter McGuigan, MBBCh, Kathryn Ward, BSc, Aisling O’Neill, BSc, Stephanie Finn, BSc; Brighton and Sussex University Hospitals Trust: Barbara Phillips, Laura Oritz-Ruiz de Gordoa, BSc; Bristol Royal Infirmary: Jeremy Bewley, MBChB, Matthew Thomas, MBChB, Katie Sweet, BSc(Hons), Lisa Grimmer, BSc(Hons), Rebekah Johnson, BSc(Hons); Calderdale and Huddersfield Foundation Trust: Jez Pinnell, MD, Matt Robinson, BSc(Hons), Lisa Gledhill, MSc, Tracy Wood, BSc(Hons); Cardiff and Vale University Health Board: Matt Morgan, PhD, Jade Cole, BSc, Helen Hill, BSc, Michelle Davies, BN, Angharad Williams, BSc, Emma Thomas, BSc, Rhys Davies, BSc, Matt Wise, DPhil; Charing Cross Hospital: David Antcliffe, PhD, Maie Templeton, MSc, Roceld Rojo, BSN, Phoebe Coghlan, MA, Joanna Smee, BSc; Chesterfield Royal Hospital: Euan Mackay, MD, Jon Cort, MD, Amanda Whileman, BSc, Thomas Spencer, Nick Spittle, Sarah Beavis, MD, Anand Padmakumar, MD, Katie Dale, BSc, Joanne Hawes, BSc, Emma Moakes, BSc, Rachel Gascoyne, BSc, Kelly Pritchard, BSc, Lesley Stevenson, BSc, Justin Cooke, MD, Karolina Nemeth-Roszpopa, MD; The Christie NHS Foundation Trust: Vidya Kasipandian, FFICM, Amit Patel, Suzanne Allibone, Roman Mary-Genetu, BSc; Colchester Hospital: Mohamed Ramali, FRCA, Ooi HC, MRCEM, Alison Ghosh, RN, Rawlings Osagie, PharmD, Malka Jayasinghe Arachchige, MBBS, Melissa Hartley, MBBS; Countess of Chester Hospital: Peter Bamford, FFICM, Emily London, MBChB, Kathryn Cawley, MRes, Maria Faulkner, BSc, Helen Jeffrey, DipNS; Croydon University Hospital: Ashok Sundar Raj, MD, Georgios Tsinaslanidis, MD, Reena Nair Khade, BSc, Gloria Nwajei Agha, BSc, Rose Nalumansi Sekiwala; Cumberland Infirmary: Tim Smith, FRCA, Chris Brewer, BPharm(Hons), Jane Gregory, BSc(Hons); Darlington Memorial Hospital: James Limb, FRCA, Amanda Cowton, BSc(Hons), Julie O’Brien, DipNurs, Kelly Postlethwaite, DipNurs; Derriford Hospital: Nikitas Nikitas, PhD, Colin Wells, MSc, Liana Lankester, PGCert, Helen McMillan, MSc; Dorset County Hospital: Mark Pulletz, FFICM, Patricia Williams, AdDip, Jenny Birch, BA, Sophie Wiseman, Mpharm, Sarah Horton, BA(Hons); East Kent Hospitals (Queen Elizabeth the Queen Mother Hospital): Ana Alegria, CCT, Salah Turki, MBBch, Tarek Elsefi, MRCP, Nikki Crisp, BSc, Louise Allen, BSc; East Lancashire Hospitals NHS Trust (Royal Blackburn Hospital): Matthew Smith, MD, Sri Chukkambotla, MD, Wendy Goddard, BSc, Stephen Duberley BSc; Freeman Hospital and Royal Victoria Infirmary, Newcastle upon Tyne: Iain J McCullagh, FRCA, Philip Robinson, MSc, Bijal Patel, MSc, Sinead Kelly, PGDip; Frimley Health NHS Foundation Trust: Omar Touma, MD, Susan Holland, Christopher Hodge, Holly Taylor, Meera Alderman, Nicky Barnes, Joana Da Rocha, BSc, Catherine Smith, BSc, Nicole Brooks, Thanuja Weerasinghe, BSc, Julie-Ann Sinclair, Yousuf Abusamra, MD, Ronan Doherty, MD, Joanna Cudlipp, MD, Rajeev Singh, MD, Haili Yu, MD, Admad Daebis, MD, Christopher NG, MD, Sara Kendrick, MD, Anita Saran, MD, Ahmed Makky, MD, Danni Greener, MD, Louise Rowe-Leete, Dip, Alexandra Edwards, Dip, Yvonne Bland, BSc, Rozzie Dolman, BSc, Tracy Foster, BSc; Gateshead Health NHS Trust: Vanessa Linnett, MD, Amanda Sanderson, Jenny Ritzema, Helen Wild; George Eliot Hospital: Divya Khare, FRCA, Meredith Pinder, BSN, Selvin Selvamoni, MSc, Amitha Gopinath, MBA; Glan Clwyd Hospital: Richard Pugh, FFICM, Daniel Menzies, FRCP, Richard Lean, MBChB, Xinyi Qiu, MBChB, Jeremy James Scanlon, MBChB; Glasgow Royal Infirmary: Kathryn Puxty, MD, Susanne Cathcart, BSc, Chris Mc Govern, MBChB, Samantha Carmichael, MRPharms, Dominic Rimmer, BSc; Glenfield Hospital Leicester: Hakeem Yusuff, FFICM, Graziella Isgro, FFICM, Chris Brightling, PhD, Michelle Bourne, BSc(Hons), Michelle Craner, DipHE, Rebecca Boyles, BSc (Hons); Grange University Hospital: Tamas Szakmany, PhD, Shiney Cherian, BSc, Gemma Williams, BSc, Christie James, MSc, Abby Waters, MSc; Great Western Hospitals NHS Foundation Trust: Malcolm Watters, MBBCh, Rachel Prout, MBChB, Louisa Davies, BSc, Suzannah Pegler, BSc(Hons), Lynsey Kyeremeh, BPharm, Aiman Mian, MBBS; Guy’s & St Thomas’ NHS Foundation Trust: Manu Shankar-Hari, PhD, Marlies Ostermann, PhD, Marina Marotti, BSc, Neus Grau Novellas, BSc, Aneta Bociek, BSc; Hammersmith Hospital: Stephen Brett, MD, Sonia Sousa Arias, BSc, Rebecca Elin Hall, BN; Homerton University Hospital NHS Foundation Trust: Susan Jain, MD, Abhinav Gupta MD, Catherine Holbrook. James Cook University Hospital: Jeremy Henning, MB, Stephen Bonner, BSc, Keith Hugill, BSc, Emanuel Cirstea, MSc, Dean Wilkinson, BSc, Jessica Jones, BSc; James Paget University Hospitals: Michal Karlikowski, MD, Helen Sutherland, BSc(Hons), Elva Wilhelmsen, DipHE, Jane Woods, BSc, Julie North, BSc(Hons); Kettering General Hospital: Dhinesh Sundaran, FFICM, Laszlo Hollos, FFICM, Susan Coburn, PGCert, Anna Williams, BSc, Samantha Saunders, BTEC; King’s College Hospital (Denmark Hill site): Phil Hopkins, MD, John Smith, RN, Harriet Noble, RN, Maria Theresa Depante, RN, Emma Clarey, RN; Lancashire Teaching Hospitals NHS Foundation Trust: Shondipon Laha, FFICM, Mark Verlander, MBA, Alexandra Williams, MSc; Leeds Teaching Hospitals Trust: Elankumaran Paramasivam, FRCP, Elizabeth Wilby, BSc (Hons), Bethan Ogg, BSc (Hons), Clare Howcroft, BSc (Hons), Angelique Aspinwall, BSc (Hons), Sam Charlton, BSc (Hons), Richard Gould, MBBS, Deena Mistry, MPharm, Sidra Awan, MPharm, Caroline Bedford, MPharm; Leicester General Hospital: Andrew Hall, MRCP, Jill Cooke, RGN, Caroline Gardiner-Hill, RGN, Carolyn Maloney, Nigel Brunskill, PhD; Leicester Royal Infirmary: Hafiz R Qureshi, MRCPI, Neil Flint, MBChB, Sarah Nicholson, Sara Southin, Andrew Nicholson, Amardeep Ghattaoraya, MSc; Lewisham and Greenwich NHS Trust: Dr Daniel Harding, MD, Sinead O’Halloran , Amy Collins Emma Smith , Estefania Trues; Liverpool Foundation Trust Aintree: Barbara Borgatta, PhD, Ian Turner-Bone, DipHE, Amie Reddy, Laura Wilding, DipHE; Liverpool Heart and Chest Hospital: Craig Wilson, Zuhra Surti; Luton and Dunstable University Hospital: Loku Chamara Warnapura, FFICM, Ronan Agno, BSc, Prasannakumari Sathianathan, MSc, Deborah Shaw, FFICM, Nazia Ijaz, FFICM, Dean Burns, MD, Mohammed Nisar, MD, Vanessa Quick, MD, Craig Alexander, BSc, Sanil Patel BSc, Nafisa Hussain, Yvynne Croucher, BSc, Eva-Maria Lang, MD, Banu Rudran, MD, Syed Gilani, MD, Talia Wieder, MD, Margaret Louise Tate, BSc; Maidstone and Tunbridge Wells NHS Trust: David Golden, FFICM, Miriam Davey, PGDip, Rebecca Seaman BSc (Hons); Manchester Royal Infirmary: Tim Felton, FFICM, Jonathan Bannard-Smith, FFICM, Joanne Henry, Richard Clark, DiPHE, Kathrine Birchall, BSc(Hons), Joanne Henry, MA, Fiona Pomeroy, BSc (Hons), Rachael Quayle, Dip.HE, Katharine Wylie, MSc, Anila Sukuraman, BSc, John McNamarra, MD; Medway Maritime Hospital: Arystarch Makowski, PhD, Beata Misztal, PhD, Iram Ahmed, PhD, Kevin Neicker, MBA, Sam Millington, BMBS, Rebecca Squires, BSc, Masroor Phulpoto, MBBS; Milton Keynes University Hospital: Richard Stewart, Esther Mwaura, BSc, Louise E Mew, BSc(Hons), Lynn Wren, BSc(Hons), Felicity Willams, PhD; Mid & South Essex NHS Foundation Trust: Aneta Oborska, FRCA, Rino Maeda, MBBS, Selver Kalchko-Veyssal, MD, Raji Orat Prabakaran, BSc, Bernard Hadebe, MSc, Eric Makmur, MBBS, Guy Nicholls, MBBS; Musgrove Park Hospital: Richard Innes, MBBCh, Patricia Doble, BSc(Hons), Libby Graham, RN, Charmaine Shovelton, RN; Nevill Hall Hospital: Vincent Hamlyn, MBBCh, Nancy Hawkins, PhD, Anna Roynon-Reed, MSc, Sean Cutler, MSc, Sarah Lewis, MBChB; Newham University Hospital: Juan Martin Lazaro, PhD, Tabitha Newman, MSc; Ninewells Hospital: Pauline Austin, MBChB, Susan Chapman, MBChB, Louise Cabrelli, BSc; Norfolk and Norwich University Hospital: Simon Fletcher, FFICM, Jurgens Nortje, FFICM, Deirdre Fottrell-Gould, Dip, Georgina Randell, Dip, Katie Stammers, BSc; Northampton General Hospital: Mohsin Zaman, MRCP, Einas Elmahi, MPhil, Andrea Jones, PhD, Kathryn Hall, Dip; Northern General Hospital, Sheffield: Gary H Mills, PhD, Kim Ryalls, RegPharmTech, Kate Harrington RCN, Helen Bowler, BSc, Jas Sall, BSc, Richard Bourne, PhD; North Manchester General Hospital: Zoe Borrill, MD, Tracy Duncan, MD, Thomas Lamb, MD, Joanne Shaw, BSc, Claire Fox, BSc, Kirstie Smith, BSc, Sarah Holland, Bethany Blackledge, BSc, Liam McMorrow, BSc, Laura Durrans, Jade Harris; North Middlesex University Hospital: Jeronimo Moreno Cuesta, MD, Kugan Xavier, MD, Dharam Purohit, EDIC, Munzir Elhassan, MBBS, Anne Haldeos, BSc, Rachel Vincent, DipHE, Marwa Abdelrazik, MBBCH, Samuel Jenkins, BMBS, Arunkumar Ganesan, MD, Rohit Kumar, DA, David Carter, MBBS, Dhanalakshmi Bakthavatsalam, BSc; Oxford University Hospitals: Matthew Rowland, FFICM, Paula Hutton, PGCert, Archana Bashyal, MSc, Neil Davidson, BSc, Clare Hird, MSc, Sally Beer, MSc; Pilgrim Hospital Boston: Manish Chhablani, FFICM, Gunjan Phalod, MPharm, Amy Kirkby, BSc(Hons), Simon Archer, BSc(Hons), Kimberley Netherton, RGN; Princess Royal Hospital: Barbara Philips, MD, Dee Mullan, BSc, Denise Skinner, BSc, Jane Gaylard, BSc, Julie Newman, BSc; Princess of Wales Hospital: Sonia Arun Sathe, MD, Lisa Roche, BSc, Ellie Davies, BSc, Keri Turner; Poole Hospital: Henrik Reschreiter, FFICM, Julie Camsooksai, PGDE, Sarah Patch, BSc(Hons), Sarah Jenkins, BSc(Hons), Charlotte Humphrey, BSc (Hons); Queen Alexandra Hospital Portsmouth: David Pogson, MSc, Steve Rose, BSc, Zoe Daly, BSc, Lutece Brimfield, BN, Angie Nown; Queen Elizabeth Hospital, Birmingham: Dhruv Parekh, PhD, Colin Bergin, BSc, Michelle Bates, BSc, Christopher McGhee, BSc, Daniella Lynch, BSc, Khushpreet Bhandal, Dip, Kyriaki Tsakiridou, MSc, Amy Bamford, BSc, Lauren Cooper, MSc, Tony Whitehouse, MD, Tonny Veenith, MD; Queen Elizabeth University Hospital, Glasgow: Malcolm A.B. Sim, MD, Sophie Kennedy Hay, BN, Steven Henderson, MPH, Maria Nygren, MSc, Eliza Valentine, HNC; Queen’s Hospital, Burton: Amro Katary, MD, Gill Bell, BSc, Louise Wilcox, BSc, Katy English BSc, Ann Adams; Queen’s Hospital, Romford: Mandeep-Kaur Phull, MBBS, Abbas Zaidi, MBBS, Tatiana Pogreban, BN, Lace Paulyn Rosaroso, BN; Queens Medical Centre and Nottingham City Hospital: Daniel Harvey, BMBS, Benjamin Lowe, BMBS, Megan Meredith, BSc(Hons), Lucy Ryan, MNSc, DREEAM Research Team; The Rotherham NHS Foundation Trust: Anil Hormis, FRCA, Rachel Walker, BA, Dawn Collier, BSc, Sarah Kimpton, MSc, Susan Oakley; Royal Alexandra Hospital: Kevin Rooney, MBChB, Natalie Rodden, BSc, Emma Hughes, BSc, Nicola Thomson, BSc(Hons), Deborah McGlynn, BSc, Charlotte Clark, Dip, Patricia Clark, BSc; Royal Berkshire Hospital: Andrew Walden, FFICM, Liza Keating, MBChB, Matthew Frise, DPhil, Tolu Okeke, BSc, Nicola Jacques, MSc, Holly Coles, BSc, Emma Tilney, BSc, Emma Vowell, DipHE; Royal Bournemouth and Christchurch Hospitals: Martin Schuster-Bruce, FRCA, Sally Pitts, BSc, Rebecca Miln, ADipHE, Laura Purandare, MBA, Luke Vamplew, BSc; Royal Brompton Hospital: Brijesh Patel, FRCA, Debra Dempster, Mahitha Gummadi, Natalie Dormand, Shu Fang Wang; Royal Cornwall NHS Trust: Michael Spivey, FFICM, Sarah Bean, RN, Karen Burt, RN, Lorraine Moore, MPharm; Royal Devon and Exeter NHS Foundation Trust: Christopher Day, MD, Charly Gibson, MBChB, Elizabeth Gordon, BSc, Letizia Zitter, BSc, Samantha Keenan, BSc; Royal Glamorgan Hospital: Jayaprakash Singh, MD, Ceri Lynch, MD, Lisa Roche, Justyna Mikusek, Bethan Deacon, Keri Turner; Royal Gwent Hospital: Tamas Szakmany, PhD, Evelyn Baker, MSc, Shiney Cherian, BSc(Hons), John Hickey, MSc, Shreekant Champanerkar, MBBS, Lindianne Aitken, MSc, Lorraine Lewis Prosser, MSc; Royal Hallamshire Hospital, Sheffield: Gary H Mills, PhD, Ajay Raithatha, FFICM, Kris Bauchmuller, FFICM, Norfaizan Ahmad, FFICM, Matt Wiles FFICM, Jayne Willson, RN; Royal Hampshire Hospitals: Irina Grecu, MD, Jane Martin, Caroline Wrey Brown, Ana-Marie Arias, Emily Bevan; Royal Infirmary of Edinburgh: Thomas H Craven, PhD, David Hope, PGDip, Jo Singleton, BN, Sarah Clark, MNurs, Corrienne McCulloch, PhD; Royal Liverpool University Hospital: Ingeborg D Welters, PhD, David Oliver Hamilton, BMBS, Karen Williams, RGN, Victoria Waugh, BA, David Shaw, DipHE, Suleman Mulla, MBChB, Alicia Waite, PhD, Jaime Fernandez Roman, BSc, Maria Lopez Martinez, BSc; Royal London Hospital: Zudin Puthucheary, PhD, Timothy Martin, BA(Hons), Filipa Santos, RN, Ruzena Uddin, MSc(Hons), Maria Fernandez, MSc, Fatima Seidu, MSc, Alastair Somerville, MSc, Mari Lis Pakats, MSc, Priya Dias, PhD, Salam Begum, BSc, Tasnin Shahid, BSc; The Royal Free Hospital: Sanjay Bhagani, FRCP, Mark De Neef, MSc, Helder Filipe, BSc, Sara Mingos, BSc, Amitaa Maharajh, BA, Glykeria Pakou, BA, Aarti Nandani, MPharm; The Royal Marsden NHS Foundation Trust: Kate Colette Tatham, PhD, Shaman Jhanji, PhD, Ethel Black, BSNurs, Arnold Dela Rosa, BSNurs, Ryan Howle, FRCA, Ravishankar Rao Baikady, FRCA; The Royal Oldham Hospital: Redmond P Tully, FFICM, Andrew Drummond, FFICM, Joy Dearden, BSc, Jennifer E Philbin, MSc, Sheila Munt, SRN; The Royal Wolverhampton NHS Trust: Shameer Gopal, MBBCh, Jagtar- Singh Pooni, MBBS, Saibal Ganguly, MBBS, Andrew Smallwood, RGN, Stella Metherell, RGN; Royal Papworth Hospital: Alain Vuylsteke, MD, Charles Chan, FRCA, Saji Victor, COVID Research Team, Papworth Hospital; Royal Stoke Hospital: Ramprasad Matsa, FRCP, Minerva Gellamucho, BSN, Michelle Davies, NVQ; Royal Surrey County Hospital: Ben Creagh-Brown, PhD, Joe Tooley, MSc, Laura Montague, BSc, Fiona De Beaux, BSc, Laetitia Bullman, MBChB; Royal United Hospital Bath: Ian Kerslake, FFICM, Carrie Demetriou, RN, Sarah Mitchard, MBBS, Lidia Ramos, RN, Katie White, MSc; Russells Hall Hospital: Michael Reay, FFICM, Steve Jenkins, MD, Caroline Tuckwell, Angela Watts, BSc, Eleanor Traverse, Stacey Jennings; Salisbury NHS Foundation Trust: Phil Donnison, FFICM, Maggie Johns, RGN, Ruth Casey, BSc, Lehentha Mattocks, Dip, Sarah Salisbury; Salford Royal NHS Foundation Trust: Paul Dark, PhD, Alice Harvey, BSc, Reece, Doonan, BSc, Liam McMorrow, BA (Hons), Karen Knowles, BA (Hons);Sandwell and West Birmingham NHS Trust: Jonathan Hulme, FFICM, Santhana Kannan, FFICM, Sibet Joseph, BSc, Fiona Kinney, RGN, Ho Jan Senya, BPharm; Sherwood Forest Hospitals NHS Foundation Trust: Valli Ratnam, MD, Mandy Gill, Jill Kirk, Sarah Shelton. South Tyneside District Hospital: Christian Frey, MD, Riccardo Scano, MD, Madeleine McKee, BSc, Peter Murphy, BSc; Southmead Hospital: Matt Thomas, FFICM, Ruth Worner, RGN, Beverley Faulkner, RGN, Emma Gendall, BSc, Kati Hayes, BSc, Hayley Blakemore, BSc, Borislava Borislavova, MSc; St. Bartholomew’s Hospital: Colin Hamilton-Davies, MBBS, Carmen Chan, BSc, Celina Mfuko, BSc, Hakam Abbass, MSc, Vineela Mandadapu, MSc; St. George’s Hospital: Susannah Leaver, MRCP, Kamal Patel, MRCP, Sarah Farnell-Ward, MSc, Romina Pepermans Saluzzio, BSc, John Rawlins, MBBS; St. Mary’s Hospital: Anthony Gordon, MD; Dorota Banach, BSc, Ziortza Fernández de Pinedo Artaraz, BN, Leilani Cabreros, BSN; St. Peter’s Hospital, Chertsey: Ian White, FFICM, Maria Croft, BSc(Hons), Nicky Holland, BN(Hons), Rita Pereira, MPharm; Stepping Hill Hospital, Stockport: Ahmed Zaki, PhD, David Johnson, MPhil, Matthew Jackson, MBChB, Hywel Garrard, BMBS, Vera Juhaz, MD, Louise Brown BSc (Hons); Sunderland Royal Hospital: Alistair Roy, MBChB, Anthony Rostron, PhD, Lindsey Woods, BSc, Sarah Cornell, BSc; Swansea Bay University Health Board: Suresh Pillai, FFCIM, Rachel Harford, RN, Helen Ivatt, FRCA, Debra Evans, BN, Suzanne Richards, BN, Eilir Roberts, MBBCh, James Bowen, MBBCh James Ainsworth, MBBS; Torbay and South Devon NHS Foundation Trust: Thomas Clark, MBChB, FRCA, FFICM, Angela Foulds, BSc, Stacey Atkins, Dip RN; United Lincolnshire NHS Trust: Kelvin Lee, PhD, Russell Barber, FRCA, Anette Hilldrith, RGN, Claire Hewitt, RGN, Gunjan Phalod, MPharm; University Hospitals Coventry & Warwickshire NHS Trust: Pamela Bremmer, BSc, Geraldine Ward, MA, Christopher Bassford, PhD; University Hospital of North Tees: Farooq Brohi, FFARCSI, Vijay Jagannathan, FRCA, Michele Clark, MA, Sarah Purvis, Dip, Bill Wetherill, MSc; University Hospital Southampton NHS Foundation Trust: Ahilanandan Dushianthan, PhD, Rebecca Cusack, MD, Kim de Courcy-Golder, PGDip, Karen Salmon, MSc, Rachel Burnish, Simon Smith, BN, Susan Jackson, BSc, Winningtom Ruiz, BSc (Hons), Zoe Duke BSc (Hons) Magaret Johns, BA, Michelle Male, Dip, Kirsty Gladas, BSc (Hons), Satwinder Virdee, MPharm, Jacqueline Swabe, MPharm, Helen Tomlinson; Warwick Hospital: Ben Attwood, MBBCh, Penny Parsons, BSc, Bridget Campbell, BSc, Alex Smith, BSc; Watford General Hospital: Valerie J Page, MBBCh, Xiao Bei Zhao, BSc (Hons), Deepali Oza, BPharm, Gail Abrahamson, DPhil, Ben Sheath, BSc (Hons), Chiara Ellis, BSc (Hons); Western General Hospital, Edinburgh: Jonathan Rhodes, PhD, Thomas Anderson, MBChB, Sheila Morris; Whipps Cross Hospital: Charlotte Xia Le Tai, MBChB, Amy Thomas, MSc, Alexandra Keen, MSc; Whiston Hospital: Dr Ascanio, Tridente, Karen Shuker, Jeanette Anders, Sandra Greer, Paula Scott, Amy Millington, Philip Buchanan, Jodie Kirk. Wirral University Teaching Hospital NHSFT: Craig Denmade, MBChB, Girendra Sadera, MBBS, Reni Jacob, BSc, Cathy Jones, BSc, Debbie Hughes; Worcester Royal Hospital: Stephen Digby, MBBS, Nicholas Cowley, MD, Laura Wild, BSc(Hons), Jessica Thrush, RGN, Hannah Wood, BSc(Hons), Karen Austin, RGN; Wrexham Maelor Betsi Cadwaladr University Hospital: David Southern, FFICM, Harsha Reddy, FFICM, Sarah Hulse, BSc, Andy Campbell, FFICM, Mark Garton, Claire Watkins, PGDip, Sara Smuts, BN; Wrightington, Wigan and Leigh Teaching Hospitals NHS Foundation Trust: Alison Quinn, MD, Benjamin Simpson, MD, Catherine McMillan, MD, Cheryl Finch, BSc, Claire Hill BSc, Josh Cooper; Wye Valley NHS Trust: Joanna Budd, MBBS, Charlotte Small, PhD, Ryan O’Leary, MBBS, Janine Birch, RN, Emma Collins, BSc (Hons); Wythenshawe Hospital: Peter D G Alexander, FFICM, Tim Felton, FFICM, Susan Ferguson, BSc, Katharine Sellers, BSc, Joanne Bradley-Potts, BSc; York Teaching Hospital: David Yates, FCRA, Isobel Birkinshaw, BSc(Hons), Kay Kell, BSc(Hons), Zoe Scott, BN, Harriet Pearson, BSc; United States of America: UPMC Health System (enrolling hospitals – UPMC Altoona, UPMC East, UPMC Hamot, UPMC Horizon, UPMC McKeesport, UPMC Mercy, UPMC Passavant, UPMC Presbyterian, UPMC Shadyside, UPMC St. Margaret, UPMC Williamsport, UPMC Montefiore, UPMC Magee, UPMC Bedford, UPMC Northwest, UPMC Jameson): Peter Adams, William Bain, MD, Ian Barbash, MD, Emily Brant, MD, Meghan Fitzpatrick, MD, Christopher A Franz, MD, Timothy D Girard, MD, David T Huang, MD, MPH, Kim Basile, BS, Ghady Haidar, MD, Mahwish Hussain MD, Georgios Kitsios, MD, Kelsey Linstrum, MD, Florian B Mayr, MD, MPH, Brian Malley, MD, Erin McCreary, PharmD, Bryan J McVerry, MD, Kaveh Moghbeli, MD, Brian Rosborough, MD, PhD, Faraaz Shah, MD, Andrew Schoenling, MD, Varun U Shetty, MD, Tina Vita, Alexandra Weissman, MD; The Clinical Research, Investigation, and Systems Modeling of Acute Illness (CRISMA) Center coordinators and Multidisciplinary Acute Care Research Organization (MACRO) coordinators.
Funding
Supported by the European Union—through FP7-HEALTH-2013-INNOVATION: the Platform for European Preparedness Against emerging Epidemics (PREPARE) consortium (602525), and Horizon 2020 research and innovation program: the Rapid European Covid-19 Emergency Research response (RECOVER) consortium (101003589)—and by the Australian National Health and Medical Research Council (APP1101719 and APP1116530), the Health Research Council of New Zealand (16/631), a Canadian Institutes of Health Research Strategy for Patient-Oriented Research Innovative Clinical Trials Program Grant (158584), the U.K. NIHR and the NIHR Imperial Biomedical Research Centre, the Health Research Board of Ireland (CTN 2014-012), the UPMC Learning While Doing Program, the Breast Cancer Research Foundation, the French Ministry of Health (PHRC-20-0147), the Minderoo Foundation, Amgen, Eisai, the Global Coalition for Adaptive Research, and the Wellcome Trust Innovations Project (215522). Dr. Gordon is funded by an NIHR Research Professorship (RP-2015-06-18), and Dr. Shankar-Hari by an NIHR Clinician Scientist Fellowship (CS-2016-16-011).
Author information
Authors and Affiliations
Consortia
Contributions
For conceptualization: YMA, ACG, LPGD, ADN, SM, FAB, DA, LAS, AB, RB, ZB, MJMB, CAB, FMB, MB, AC, ADJ, EJD, LJE, RF, TDG, HG, RH, TEH, CMH, DTH, AJK, FL, PRL, KL, E Litton, DFM, AM, SMC, BJM, SKM, SCM, PRM, KO, RP, JCP, AEP, KMR, MSS, SWS, MSH, SYCT, AFT, AMT, FVV, RZ, CG, SB, JCM, CM, DA, SAW. Data curation: AB, AMH, CMH, KL, SSM, PRM, JCP, AMT, CG, CM. Formal analysis: LRB, MAD, MF, RJL, E Lorenzi, AM, CTS, SB, DA, SAW. Funding acquisition: ACG, LPGD, ADN, SM, MJMB, MB, KMR, JCM, CM, DA, SAW. Investigation and methodology: YMA, ACG, LPGD, ADN, SM, FAB, DA, LAS, AB, RB, ZB, MJMB, CAB, FMB, MB, AC, ADJ, EJD, LJE, RF, TDG, ECG, HG, RH, AMH, TEH, CMH, DTH, AJK, FL, PRL, KL, E Litton, SSM, DFM, AM, SMC, BJM, SKM, SCM, PRM, KO, RP, JCP, AEP, KMR, MSS, SWS, MSH, SYCT, AFT, AMT, FVV, RZ, CG, SB, JCM, CM, DA, SAW. Project administration: YMA, ACG, LPGD, ADN, SM, FAB, ZB, ECG, HG, DTH, AJK, KL, SSM, SKM, PRM, JCP, KMR, MSS, CG, SB, JCM, CM, DA, SAW. Resources: ACG, LPGD, ADN, SM, RB, MJMB, FMB, MB, KMR, JCM, CM, DA, SAW. Software: LRB, AB, MF, AMH, CMH, DTH, RJL, E Lorenzi, SSM, AM, SKM, PRM, JCP, KMR, CTS, CG, SB, CM, SAW. Supervision: YMA, ACG, LPGD, ADN, SM, MJMB, FMB, HG, BJM, KMR, SB, JCM, CM, DA, SAW. Validation: FAB, AB, TDG, AMH, CMH, DTH, KL, BJM, SKM, PRM, JCP, CTS, AMT, CG, CM. Visualization: LRB, MAD, MF, RJL, E Lorenzi, AM, CTS, SB. Writing—draft: YMA, ACG, LPGD, ADN, SM, SB, JCM, CM, DA, SAW. Writing—review & editing: YMA, ACG, LPGD, ADN, SM, FAB, DA, LAS, AB, RB, LRB, ZB, MJMB, CAB, FMB, MB, AB, AC, ADJ, MAD, EJD, LJE, MF, RF, TDG, ECG, HG, RH, AMH, TEH, CMH, DTH, AJK, FL, PRL, RJL, KL, E Litton, E Lorenzi, SSM, DFM, AM, SMC, BJM, SKM, SCM, PRM, KO, RP, JCP, AEP, KMR, MSS, CTS, SWS, MSH, SYCT, AFT, AMT, FVV, RZ, CG, SB, JCM, CM, DA, SAW.
Corresponding author
Ethics declarations
Conflicts of interest
ACG reports grants from NIHR, grants from NIHR Research Professorship (RP-2015-06-18), non-financial support from NIHR Clinical Research Network, during the conduct of the study; personal fees from GlaxoSmithKline, personal fees from Bristol Myers Squibb, personal fees from 30 Respiratory, outside the submitted work; LPGD is a member of the COVID-19 guideline committee SCCM/ESICM/SSC, member of the ESICM COVID-19 taskforce, and chair of the Dutch intensivists (NVIC) taskforce acute infectious threats; AND reports grants from Health Research Board of Ireland, during the conduct of the study; AB reports grants from Minderoo, grants from Wellcome, during the conduct of the study; LRB reports grants from EU PREPARE consortium, grants from Australian National Health and Medical Research Council, grants from Health Research Council of New Zealand, grants from UPMC, during the conduct of the study; CAB reports personal fees from BMS pfizer, non-financial support from Bayer, personal fees from Novartis, personal fees from Janssen, non-financial support from Amgen, personal fees from Lilly, personal fees from Portola, personal fees from Ablynx, outside the submitted work; MB reports other from Breast Cancer Research Foundation, during the conduct of the study; other from Eisai Inc, other from Amgen Inc, outside the submitted work; MDJ reports receiving fees for being on the Advisory Board for Roche and Cidara. He also reports receiving fee for being on IDSMB for Janssen and GSK; MAD reports grants from EU PREPARE, grants from Australian National Health and Medical Research Council, grants from Health Research Council of New Zealand, grants from UPMC, during the conduct of the study; MF reports grants from EU PREPARE, grants from Australian National Health and Medical Research Council, grants from Health Research Council of New Zealand, grants from UPMC, during the conduct of the study; RH reports grants from Wellcome Trust, during the conduct of the study; grants from National Institute of Health Research, outside the submitted work; AMH.reports grants from National Health and Medical Research Council and from the Minderoo Foundation during the conduct of the study; TEH. reports grants from Health Research Council of New Zealand, during the conduct of the study; CMH. reports grants from NICHD, during the conduct of the study; DTH.reports grants from The Breast Cancer Research Foundation in collaboration with the Translational Breast Cancer Research Consortium, during the conduct of the study; PRL. reports personal fees from Novartis, personal fees from Brigham and Women's Hospital, personal fees from Corona LLC, personal fees from McGraw Hill Publishing, outside the submitted work; RJL reports that Berry Consultants, LLC, a statistical consulting firm that specializes in the design, conduct, oversight, and analysis of adaptive and platform clinical trials, received support for its role in the design, conduct, and analysis of REMAP-CAP. Dr. Lewis is the Senior Medical Scientist at Berry Consultants, LLC; EL reports grants from EU, grants from Australian National Health and Medical Research Council, grants from Health Research Council of New Zealand, grants from UPMC, during the conduct of the study; DFM reports personal fees from consultancy for GlaxoSmithKline, Boehringer Ingelheim, Bayer, Novartis and Eli Lilly, and from sitting on a DMEC for a trial undertaken by Vir Biotechnology. In addition his institution has received funds from grants from several funders for studies in patients with ARDS and COVID-19. In addition, DFM has a patent (US8962032) issued to his institution for a treatment for inflammatory disease. He is a Director of Research for the Intensive Care Society and NIHR EME Programme Director; AM reports grants from EU-PREPARE, grants from Australian National Health and Medical Research Council, grants from Health Research Council of New Zealand, grants from UPMC, during the conduct of the study; B JM reports grants from Translational Breast Cancer Research Consortium, grants from UPMC Learning While Doing Program, during the conduct of the study; grants from NIH/NHLBI, grants from Bayer Pharmaceuticals, Inc, outside the submitted work; SCM reports grants from Health Research Council of New Zealand, during the conduct of the study; PRM reports grants from National Institute for Health Research, grants from European Union FP7 (PREPARE), during the conduct of the study; RP reports grants from Fisher and Paykel Healthcare NZ Ltd, outside the submitted work; KMR reports grants from European Union, grants from UK National Institute for Health Research, during the conduct of the study; CTS. reports grants from EU PREPARE, grants from Australian National Health and Medical Research Council, grants from Health Research Council of New Zealand, grants from UPMC, during the conduct of the study; CWS. reports grants from NIH, personal fees from Beckman Coulter, outside the submitted work; MSH reports other from National Institute For Health Research, outside the submitted work; AMT reports grants from Health Research Council of New Zealand, during the conduct of the study; FVV reports personal fees from Gilead, personal fees from Sobi, outside the submitted work; SB reports personal fees from Berry Consultants, during the conduct of the study; JCM. reports grants from Canadian Institutes of Health Research, during the conduct of the study; personal fees from Gilead Pharmaceuticals, outside the submitted work; CM reports grants from Health Research Council of New Zealand, non-financial support from Abbvie, during the conduct of the study; DCA reports non-financial support from European Union FP7 PREPARE, grants from Breast Cancer Research Foundation, Amgen, Inc., and Eisai, Inc, during the conduct of the study; SAW reports grants from National Health and Medical Research Council, grants from Minderoo Foundation, grants from Health Research Council, during the conduct of the study. *All other authors had no conflict of interest to disclose.
Ethics approval
The trial was approved by the relevant ethics committees in all regions.
Consent to participate
Written or verbal informed consent, in accordance with regional legislation, was obtained from all patients or from their surrogates.
Consent for publication
All authors approved the manuscript for submission.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The members of “The REMAP-CAP Investigators” are listed in Acknowledgements section.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Arabi, Y.M., Gordon, A.C., Derde, L.P.G. et al. Lopinavir-ritonavir and hydroxychloroquine for critically ill patients with COVID-19: REMAP-CAP randomized controlled trial. Intensive Care Med 47, 867–886 (2021). https://doi.org/10.1007/s00134-021-06448-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-021-06448-5