Abstract
Purpose
End-of-life (EOL) decisions are not well studied in developing countries. We report EOL decision patterns in two Tunisian intensive care units [ICUs, medical (MICU) and surgical (SICU)] belonging to the same teaching hospital.
Methods
Consecutive deaths that occurred in participating ICUs over 2 years were analysed. End-of-life decisions were prospectively recorded by the senior attending physicians, while subject’s characteristics were retrospectively collected.
Results
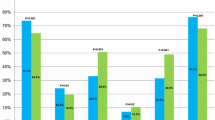
Deaths occurred in 326 of 1,733 ICU-admitted patients (median age: 64 years; median SAPS II at admission = 36). Overall, a decision for full support was taken in 69%, while decisions to withhold or withdraw life support were held in 22.1 and 8.9% of deaths, respectively. The rate of end-of-life decisions was similar in the MICU and the SICU. In no instance was there MV withdrawal during ICU stay. Discharging patients to die at home was observed only in the MICU (10 out of the 20 patients with a withdrawal decision). Two factors were independently associated with WH or WD decisions: a severe and ultimately fatal underlying disease was positively associated with such decisions (OR = 2.4, 95% CI: 1.3–4.36; p = 0.003), while having an independent functional status before the ICU was associated with a decreased rate of physician decisions of WH or WD (OR = 0.32, 95% CI: 0.15–0.67; p = 0.002).
Conclusion
Withholding and withdrawing life support are common in medical and surgical ICUs of a Tunisian hospital. Withholding is more frequent than withdrawing life support. These decisions appear to be effected by functional status and underlying conditions.

Similar content being viewed by others
References
Angus DC, Kelley MA, Schmitz RJ, White A, Popovich J Jr (2000) Caring for the critically ill patient. Current and projected workforce requirements for care of the critically ill and patients with pulmonary disease: can we meet the requirements of an aging population? JAMA 284:2762–2770
Adhikari NK, Fowler RA, Bhagwanjee S, Rubenfeld GD (2010) Critical care and the global burden of critical illness in adults. Lancet 376:1339–1346
Wunsch H, Linde-Zwirble WT, Harrison DA, Barnato AE, Rowan KM, Angus DC (2009) Use of intensive care services during terminal hospitalizations in England and the United States. Am J Respir Crit Care Med 180:875–880
Bertolini G, Boffelli S, Malacarne P, Peta M, Marchesi M, Barbisan C, Tomelleri S, Spada S, Satolli R, Gridelli B, Lizzola I, Mazzon D (2010) End-of-life decision-making and quality of ICU performance: an observational study in 84 Italian units. Intensive Care Med 36(9):1495–1504
Prendergast TJ, Claessens MT, Luce JM (1998) A national survey of end-of-life care for critically ill patients. Am J Respir Crit Care Med 158:1163–1167
Sprung CL, Cohen SL, Sjokvist P, Baras M, Bulow HH, Hovilehto S, Ledoux D, Lippert A, Maia P, Phelan D, Schobersberger W, Wennberg E, Woodcock T (2003) End-of-life practices in European intensive care units: the ethicus study. JAMA 290:790–797
Sprung CL, Woodcock T, Sjokvist P, Ricou B, Bulow HH, Lippert A, Maia P, Cohen S, Baras M, Hovilehto S, Ledoux D, Phelan D, Wennberg E, Schobersberger W (2008) Reasons, considerations, difficulties and documentation of end-of-life decisions in European intensive care units: the ETHICUS Study. Intensive Care Med 34:271–277
Weng L, Joynt GM, Lee A, Du B, Leung P, Peng J, Gomersall CD, Hu X, Yap HY (2011) Attitudes towards ethical problems in critical care medicine: the Chinese perspective. Intensive Care Med 37:655–664
Pochard F, Abroug F (2005) End-of-life decisions in ICU and cultural specificities. Intensive Care Med 31:506–507
Azoulay E, Metnitz B, Sprung CL, Timsit JF, Lemaire F, Bauer P, Schlemmer B, Moreno R, Metnitz P (2009) End-of-life practices in 282 intensive care units: data from the SAPS 3 database. Intensive Care Med 35:623–630
Bulow HH, Sprung CL, Reinhart K, Prayag S, Du B, Armaganidis A, Abroug F, Levy MM (2008) The world’s major religions’ points of view on end-of-life decisions in the intensive care unit. Intensive Care Med 34:423–430
Sachedina A (2005) End-of-life: the Islamic view. Lancet 366:774–779
Gouda A, Al-Jabbary A, Fong L (2010) Compliance with DNR policy in a tertiary care center in Saudi Arabia. Intensive Care Med 36:2149–2153
Iyilikci L, Erbayraktar S, Gokmen N, Ellidokuz H, Kara HC, Gunerli A (2004) Practices of anaesthesiologists with regard to withholding and withdrawal of life support from the critically ill in Turkey. Acta Anaesthesiol Scand 48:457–462
Yazigi A, Riachi M, Dabbar G (2005) Withholding and withdrawal of life-sustaining treatment in a Lebanese intensive care unit: a prospective observational study. Intensive Care Med 31:562–567
Chelli H, Besbes L, BenKhelil J, Thabet H, Bouhaja B, Ghedira S, BenLakhal S, Bchir A, Gahbiche M, Bouaziz M, elAtrous S, Besbes M, Amamou M, BenAmmar, Daoud A, Bouchoucha S, Abroug F (2004) [Mechanical ventilation in intensive care units: indications, modalities and complications. Results of a prospective multicenter survey in Tunisia]. Tunis Med 82:12–18
McCabe WR, Jackson GG (1962) Gram negative bacteremia: etiology and ecology. Arch Intern Med 110:847–855
Soares M, Terzi RG, Piva JP (2007) End-of-life care in Brazil. Intensive Care Med 33:1014–1017
Esteban A, Gordo F, Solsona JF, Alia I, Caballero J, Bouza C, Alcala-Zamora J, Cook DJ, Sanchez JM, Abizanda R, Miro G, FernandezDelCabo MJ, de Miguel E, Santos JA, Balerdi B (2001) Withdrawing and withholding life support in the intensive care unit: a Spanish prospective multi-centre observational study. Intensive Care Med 27:1744–1749
Mani RK, Mandal AK, Bal S, Javeri Y, Kumar R, Nama DK, Pandey P, Rawat T, Singh N, Tewari H, Uttam R (2009) End-of-life decisions in an Indian intensive care unit. Intensive Care Med 35(10):1713–1719
Buckley TA, Joynt GM, Tan PY, Cheng CA, Yap FH (2004) Limitation of life support: frequency and practice in a Hong Kong intensive care unit. Crit Care Med 32:415–420
Wood GG, Martin E (1995) Withholding and withdrawing life-sustaining therapy in a Canadian intensive care unit. Can J Anaesth 42:186–191
Wunsch H, Harrison DA, Harvey S, Rowan K (2005) End-of-life decisions: a cohort study of the withdrawal of all active treatment in intensive care units in the United Kingdom. Intensive Care Med 31:823–831
Turner JS, Michell WL, Morgan CJ, Benatar SR (1996) Limitation of life support: frequency and practice in a London and a Cape Town intensive care unit. Intensive Care Med 22:1020–1025
Hakim RB, Teno JM, Harrell FE Jr, Knaus WA, Wenger N, Phillips RS, Layde P, Califf R, Connors AF Jr, Lynn J (1996) Factors associated with do-not-resuscitate orders: patient’s preferences, prognoses, and physician’s judgments. Support investigators. Study to understand prognoses and preferences for outcomes and risks of treatment. Ann Intern Med 125:284–293
Cohen J, van Delden J, Mortier F, Lofmark R, Norup M, Cartwright C, Faisst K, Canova C, Onwuteaka-Philipsen B, Bilsen J (2008) Influence of physician’s life stances on attitudes to end-of-life decisions and actual end-of-life decision-making in six countries. J Med Ethics 34:247–253
Sprung CL, Maia P, Bulow HH, Ricou B, Armaganidis A, Baras M, Wennberg E, Reinhart K, Cohen SL, Fries DR, Nakos G, Thijs LG (2007) The importance of religious affiliation and culture on end-of-life decisions in European intensive care units. Intensive Care Med 33:1732–1739
Luce JM (1997) Withholding and withdrawal of life support: ethical, legal, and clinical aspects. New Horiz 5:30–37
(1991) Withholding and withdrawing life-sustaining therapy. This Official Statement of the American Thoracic Society was adopted by the ATS Board of Directors, March 1991. Am Rev Respir Dis 144:726–731
Ganz FD, Benbenishty J, Hersch M, Fischer A, Gurman G, Sprung CL (2006) The impact of regional culture on intensive care end of life decision making: an Israeli perspective from the ETHICUS study. J Med Ethics 32:196–199
Beuks BC, Nijhof AC, Meertens JH, Ligtenberg JJ, Tulleken JE, Zijlstra JG (2006) A good death. Intensive Care Med 32:752–753
Kallel H, Dammak H, Bahloul M, BenHamida C, Chelly H, Rekik N, Bouaziz M (2006) A good death: another break in the wall. Intensive Care Med 32:1915–1916
Boussarsar M, Bouchoucha S (2006) Dying at home: cultural and religious preferences. Intensive Care Med 32:1917–1918
Meissner A, Genga KR, Studart FS, Settmacher U, Hofmann G, Reinhart K, Sakr Y (2010) Epidemiology of and factors associated with end-of-life decisions in a surgical intensive care unit. Crit Care Med 38:1060–1068
Huang YC, Huang SJ, Ko WJ (2009) Going home to die from surgical intensive care units. Intensive Care Med 35:810–815
Nathens AB, Rivara FP, Wang J, Mackenzie EJ, Jurkovich GJ (2008) Variation in the rates of do not resuscitate orders after major trauma and the impact of intensive care unit environment. J Trauma 64:81–88 (discussion 88–91)
Azoulay E, Pochard F, Garrouste-Orgeas M, Moreau D, Montesino L, Adrie C, de Lassence A, Cohen Y, Timsit JF (2003) Decisions to forgo life-sustaining therapy in ICU patients independently predict hospital death. Intensive Care Med 29:1895–1901
Keenan SP, Busche KD, Chen LM, McCarthy L, Inman KJ, Sibbald WJ (1997) A retrospective review of a large cohort of patients undergoing the process of withholding or withdrawal of life support. Crit Care Med 25:1324–1331
Ferrand E, Robert R, Ingrand P, Lemaire F (2001) Withholding and withdrawal of life support in intensive-care units in France: a prospective survey. French LATAREA Group. Lancet 357:9–14
Reignier J, Dumont R, Katsahian S, Martin-Lefevre L, Renard B, Fiancette M, Lebert C, Clementi E, Bontemps F (2008) Patient-related factors and circumstances surrounding decisions to forego life-sustaining treatment, including intensive care unit admission refusal. Crit Care Med 36:2076–2083
Acknowledgments
We thank Dr Abdelkarim Waness for his helpful comments and critical review of the article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ouanes, I., Stambouli, N., Dachraoui, F. et al. Pattern of end-of-life decisions in two Tunisian intensive care units: the role of culture and intensivists’ training. Intensive Care Med 38, 710–717 (2012). https://doi.org/10.1007/s00134-012-2500-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-012-2500-9