Abstract
Objective
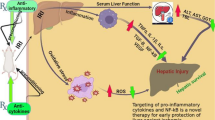
The aim of this study was to investigate the impact of the water-soluble poly-(ADP)-ribose-polymerase (PARP) inhibitor 5-aminoisoquinolinone (5-AIQ) on liver microcirculation and function after haemorrhagic shock and resuscitation.
Design
Controlled, randomized animal study.
Setting
University animal care facility and research laboratory.
Subject
Male Sprague–Dawley rats were subjected to haemorrhagic shock for 1 h, followed by resuscitation with shed blood and crystalloid solution for a total of 5 h.
Interventions
The PARP inhibitor 5-AIQ (3 mg/kg; n = 7) or vehicle (n = 7) was administered 5 min prior to resuscitation. Sham-operated animals without induction of shock served as controls (n = 7).
Measurements and results
Using intravital fluorescence microscopy hepatic microcirculation was assessed at baseline, end of shock phase as well as 1 h and 5 h after resuscitation. Systemic arterial blood pressure and bile flow were continuously monitored. 5-AIQ treatment attenuated shock/resuscitation-induced increase of intrahepatic leukocyte–endothelial cell interaction with a marked reduction of both sinusoidal leukostasis and venular leukocyte adherence. Moreover, nutritive perfusion was found improved, guaranteeing sufficient oxygen supply to tissue, as indicated by low NADH autofluorescence, which was not different to that in controls. Most notably, excretory liver function reached baseline level over 5 h of reperfusion in 5-AIQ-treated animals.
Conclusions
In the present setting of shock/resuscitation in male rats the PARP inhibitor 5-AIQ proved to be very effective in ameliorating compromised liver microcirculation and function. Further research has to confirm that PARP inhibition is a suitable tool in the acute treatment of patients suffering from reduced circulating blood volume and thus microcirculatory organ dysfunction.





Similar content being viewed by others
References
Roesner JP, Vagts DA, Iber T, Vollmar B, Nöldge-Schomburg GFE (2005) Protective effect of the parp-inhibitor 5-AIQ on rat liver microcirculation after hemorraghic shock. In: Abstracts of the 18th European Society of Intensive Care Medicine (ESICM) Annual Congress, Amsterdam, Netherlands, 25–28 September 2005. Intensive Care Med 31 [Suppl 1]:S5–S226
Jarrar D, Wang P, Cioffi WG, Bland KI, Chaudry IH (2000) Critical role of oxygen radicals in the initiation of hepatic depression after trauma hemorrhage. J Trauma 49:879–885
Laplace C, Huet O, Vicaut E, Ract C, Martin L, Benhamou D, Duranteau J (2005) Endothelial oxidative stress induced by serum from patients with severe trauma hemorrhage. Intensive Care Med 31:1174–1180
Jaeschke H (2000) Reactive oxygen and mechanisms of inflammatory liver injury. J Gastroenterol Hepatol 15:718–724
Szabo C, Lim LH, Cuzzocrea S, Getting SJ, Zingarelli B, Flower RJ, Salzman AL, Perretti M (1997) Inhibition of poly (ADP-ribose) synthetase attenuates neutrophil recruitment and exerts antiinflammatory effects. J Exp Med 186:1041–1049
Menger MD, Vollmar B (2000) Role of microcirculation in transplantation. Microcirculation 7:291–306
Jaeschke H (2003) Molecular mechanism of hepatic ischemia-reperfusion injury and preconditioning. Am J Gastrointest Liver Physiol 284:G15--G26
Weiss SJ (1989) Tissue destruction by neutrophils. N Engl J Med 320:367–376
Eipel C, Bordel R, Nickels RM, Menger MD, Vollmar B (2004) Impact of leucocytes and platelets in mediating hepatocyte apoptosis in a rat model of systemic endotoxemia. Am J Physiol Gastrointest Liver Physiol 286:G769–G776
Moore FA, Sauaia A, Moore E, Haenel JB, Burch JM, Lezotte DC (1996) Postinjury multiple organ failure: a bimodal phenomenon. J Trauma 4:501–512
Ikai K, Ueda K (1983) Immunohistochemical demonstration of poly(ADP-ribose)-synthetase in bovine tissues. J Histochem Cytochem 31:261–264
Szabo C (1998) Potential role of the peroxynitrate-poly(ADP-ribose) synthetase pathway in a rat model of severe hemorrhagic shock. Shock 9:341–344
Watts JA, Robert M, Grattan Il RM, Whitlow BS, Kline JA (2001) Activation of poly(ADP-ribose) polymerase in severe hemorrhagic shock and resuscitation. Am J Gastrointest Liver Physiol 281:G498–G506
Ha HC, Snyder SH (1999) Poly (ADP-ribose) polymerase is a mediator of necrotic cell death by ATP depletion. Proc Natl Acad Sci USA 96:13978–13982
Khandoga A, Enders G, Biberthaler P, Krombach F (2002) Poly(ADP-ribose) polymerase triggers the microvascular mechanisms of hepatic ischemia-reperfusion injury. Am J Gastrointest Liver Physiol 283:G553–G560
Zingarelli B, Salzman AL, Szabo C (1998) Genetic disruption of poly (ADP-ribose) synthetase inhibits the expression of P-selectin and intercellular adhesion molecule-1 in myocardial ischemia/reperfusion injury. Circ Res 83:85–94
Thiemermann C (2002) Development of novel, water-soluble inhibitors of poly(adenosine 5'-diphosphate ribose)-synthetase activity for use in shock and ischemia-reperfusion injury. Crit Care Med 30:1163–1165
Jagtap P, Szabo C (2005) Poly(ADP-ribose) polymerase and the therapeutic effects of its inhibitors. Nat Rev Drug Discov 4:421–440
Mota-Filipe H, Sepodes B, McDonald M, Cuzzocrea S, Pinto R, Thiemermann C (2002) The novel PARP inhibitor 5-aminoisoquinolinone reduces the liver injury caused by ischemia and reperfusion in the rat. Med Sci Monit 8:BR444–BR453
Thiemermann C, Bowes J, Myint FP, Vane JR (1997) Inhibition of the activity of poly(ADP ribose) synthetase reduces ischemia-reperfusion injury in the heart and skeletal muscle. Proc Natl Acad Sci USA 94:679–683
McDonald MC, Mota-Filipe H, Wright JA, Abdelrahman M, Threadgill MD, Thompson AS, Thiemermann C (2000) Effects of 5-aminoisoquinolinone, a water-soluble, potent inhibitor of the activity of poly (ADP-ribose) polymerase on the organ injury and dysfunction caused by haemorrhagic shock. Br J Pharmacol 130:843–850
Khandoga A, Biberthaler P, Enders G, Krombach F (2004) 5-Aminoisoquinolinone, a novel inhibitor of poly(adenosine disphosphate-ribose) polymerase, reduces microvascular liver injury but not mortality rate after hepatic ischemia-reperfusion. Crit Care Med 32:472–477
Vollmar B, Glasz J, Leiderer R, Post S, Menger MD (1994) Hepatic microcirculatory perfusion failure is a determinant of liver dysfunction in warm ischemia-reperfusion. Am J Pathol 145:1421–1431
Hoetzel A, Vagts DA, Loop T, Humar M, Bauer M, Pahl HL, Geiger KK, Pannen BH (2001) Effect of nitric oxide on shock-induced hepatic oxygenase-1 expression in the rat. Hepatology 33:925–937
Vollmar B, Menger MD, Glasz J, Leiderer R, Messmer K (1994) Impact of leukocyte-endothelial cell interaction in hepatic ischemia-reperfusion injury. Am J Physiol 267:G786–G793
Vollmar B, Burkhardt M, Minor T, Klauke H Menger MD (1997) High-resolution microscopic determination of hepatic NADH fluorescence for in vivo monitoring of tissue oxygenation during hemorrhagic shock and resuscitation. Microvasc Res 54:164–173
Sumimoto K, Inagaki K, Yamada K, Kawasaki T, Dohi K (1988) Reliable indices for the determination of viability of grafted liver immediately after orthotopic transplantation. Bile flow rate and cellular adenosine triphosphate level. Transplantation 46:506–509
Altman DG, Gardener MJ (1992) Confidence intervals for research findings. Br J Obstet Gyn 99:90–91
Mabley JG, Horvath EM, Murthy KG, Zsengeller Z, Vaslin A, Benko R, Kollai M, Szabo C (2005) Gender differences in the endotoxin-induced inflammatory and vascular responses: potential role of poly(ADP-ribose) polymerase activation. J Pharmacol Exp Ther 315:812–820
McCullough LD, Zeng Z, Blizzard KK, Debchoudhury I, Hurn PD (2005) Ischemic nitric oxide and poly (ADP-ribose) polymerase-1 in cerebral ischemia: male toxicity, female protection. J Cereb Blood Flow Metab 25:502–512
Schmidt R, Baechle T, Hoetzel A, Loop T, Humar M, Roesslein M, Geiger KK, Pannen BH (2006) Dihydralazine treatment limits liver injury after hemorrhagic shock in rats. Crit Care Med 34:815–822
Docherty JC, Kuzio B, Silvester JA, Bowes J, Thiemermann C (1999) An inhibitor of poly(ADP-ribose) synthetase activity reduces contractile dysfunction and preserves high energy phosphate levels during reperfusion of the ischemic rat heart. Br J Pharmacol 127:1518–1524
Szabo A, Hake P, Salzman AL, Szabo C (1998) 3-Aminobenzamide, an inhibitor of poly (ADP-ribose) synthetase, improves hemodynamics and prolongs survival in a porcine model of hemorrhagic shock. Shock 10:347–353
St John J, Barbee RW, Sonin N, Clemens MG, Watts JA (1999) Inhibition of poly(ADP-ribose) synthetase improves vascular contractile responses following trauma-hemorrhage and resuscitation. Shock 12:188–195
Szabo C (1998) Role of poly(ADP-ribose)synthetase in inflammation. Eur J Pharmacol 350:1–19
Genovese T, Mazzon E, Muia C, Patel NS, Threadgill MD, Bramanti P, De Sarro A, Thiemermann C, Cuzzocrea S (2005) Inhibitors of poly(ADP-ribose) polymerase modulate signal transduction pathways and secondary damage in experimental spinal cord trauma. J Pharmacol Exp Ther 312:449–457
Vollmar B, Glasz J, Menger MD, Messmer K (1995) Leukocytes contribute to hepatic ischemia/reperfusion injury via intercellular adhesion molecule-1-mediated venular adherence. Surgery 117:195–200
Braide M, Amundson B, Chien S, Bagge U (1984) Quantitative studies on the influence of leukocytes on the vascular resistance in a skeletal muscle preparation. Microvasc Res 27:331–352
Shatney CH, Read G, Cuevo R, Formeister JF (1981) The natural leukocyte response to hemorrhagic shock. Adv Shock Res 5:79–88
Vollmar B, Lang G, Menger MD, Messmer K (1994) Hypertonic hydroxyethyl starch restores hepatic microvascular perfusion in hemorrhagic shock. Am J Physiol 266:H1927–H1934
Chien S (1985) Role of blood cells in microcirculatory regulation. Microvasc Res 29:129–151
House SD, Lipowsky HH (1987) Leukocyte-endothelium adhesion: microhemodynamics in mesentery of the cat. Microvasc Res 34:363–379
Kamiike W, Nakahara M, Nakao K, Koseki M, Nishida T, Kawashima Y, Watanabe F, Tagawa K (1985) Correlation between cellular ATP level and bile excretion in the rat liver. Transplantation 39:50–55
Acknowledgements
The study was supported by a grant from the University of Rostock (FORUN, 989021). The authors would like to thank B. Blendow, D. Butzlaff, D. Frenz and M. Nerowski, Department of Experimental Surgery, University of Rostock, for their excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
The results of this study were presented as an oral presentation at the 18th Annual Congress of the European Society of Intensive Care Medicine in Amsterdam, September 2005.
This article is discussed in the editorial available at:http://dx.doi.org/10.1007/s00134-006-0336-x
Rights and permissions
About this article
Cite this article
Roesner, J.P., Vagts, D.A., Iber, T. et al. Protective effects of PARP inhibition on liver microcirculation and function after haemorrhagic shock and resuscitation in male rats. Intensive Care Med 32, 1649–1657 (2006). https://doi.org/10.1007/s00134-006-0335-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-006-0335-y