Abstract
Objective
Shock induces oxidative stress by ischemia-reperfusion phenomenon. Endothelial cells are involved in the inflammatory response and oxidative stress responsible for microcirculation impairment and organ failure. We examined the potential of serum from patients to induce in vitro reactive oxygen species production by cultured human umbilical vein endothelial cells (HUVECs).
Patients
Three groups were compared: hemorrhagic shock trauma patients, isolated brain injured patients, and healthy volunteers.
Methods
In the hemorrhagic shock group we sought a correlation between reactive oxygen species production and severity of shock. Serum was separated and perfused in an in vitro model of perfused HUVECs. Ex vivo reactive oxygen species production was assessed by fluorescence microscopy using dichlorodihydrofluorescein, an intracellular dye oxidized by H2O2. Results are expressed in proportional change from baseline and normalized by protidemia to control for variation related to hemodilution.
Results
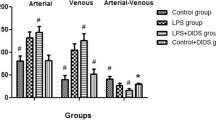
Reactive oxygen species production by endothelial cells exposed to serum from hemorrhagic shock patients (46.2±24.9%) was significantly greater than in those with brain injury (3.9±35.1%) and in healthy volunteers (−6.8±5.8%). In the hemorrhagic shock group dichlorodihydrofluorescein fluorescence was strongly correlated positively to Simplified Acute Physiology Score II and lactatemia and negatively to [HCO3−].
Conclusions
Serum from trauma patients with hemorrhagic shock induces reactive oxygen species formation in naive endothelial cells which is correlated to shock severity.




Similar content being viewed by others
References
Zulueta JJ, Sawhney R, Yu FS, Cote CC, Hassoun PM (1997) Intracellular generation of reactive oxygen species in endothelial cells exposed to anoxia-reoxygenation. Am J Physiol 272:L897–902
Goossens V, Grooten J, De Vos K, Fiers W (1995) Direct evidence for tumor necrosis factor-induced mitochondrial reactive oxygen intermediates and their involvement in cytotoxicity. Proc Natl Acad Sci U S A 92:8115–8119
Zhang Z, Blake DR, Stevens CR, Kanczler JM, Winyard PG, Symons MC, Benboubetra M, Harrison R (1998) A reappraisal of xanthine dehydrogenase and oxidase in hypoxic reperfusion injury: the role of NADH as an electron donor. Free Radic Res 28:151–164
Childs EW, Udobi KF, Wood JG, Hunter FA, Smalley DM, Cheung LY (2002) In vivo visualization of reactive oxidants and leukocyte-endothelial adherence following hemorrhagic shock. Shock 18:423–427
Al-Mehdi AB, Zhao G, Dodia C, Tozawa K, Costa K, Muzykantov V, Ross C, Blecha F, Dinauer M, Fisher AB (1998) Endothelial NADPH oxidase as the source of oxidants in lungs exposed to ischemia or high K+. Circ Res 83:730–737
Chandel NS, Maltepe E, Goldwasser E, Mathieu CE, Simon MC, Schumacker PT (1998) Mitochondrial reactive oxygen species trigger hypoxia-induced transcription. Proc Natl Acad Sci U S A 95:11715–11720
Pearlstein DP, Ali MH, Mungai PT, Hynes KL, Gewertz BL, Schumacker PT (2002) Role of mitochondrial oxidant generation in endothelial cell responses to hypoxia. Arterioscler Thromb Vasc Biol 22:566–573
Takahashi M, Nagao T, Imazeki Y, Matsuzaki K, Minamitani H (2002) Roles of reactive oxygen species in monocyte activation induced by photochemical reactions during photodynamic therapy. Front Med Biol Eng 11:279–294
Lasnier E, Blanc MC, Housset C, Rey C, Roch-Arveiller M, Vaubourdolle M (2002) Cytotoxic response of sinusoidal endothelial cells to polymorphonuclear leukocytes and its potential implication in hypoxia-reoxygenation injury. Liver 22:495–500
Cooper D, Stokes KY, Tailor A, Granger DN (2002) Oxidative stress promotes blood cell-endothelial cell interactions in the microcirculation. Cardiovasc Toxicol 2:165–180
Nishida M, Futami S, Morita I, Maekawa K, Murota SI (2000) Hypoxia-reoxygenation inhibits gap junctional communication in cultured human umbilical vein endothelial cells. Endothelium 7:279–286
Grisham MB, Granger DN, Lefer DJ (1998) Modulation of leukocyte-endothelial interactions by reactive metabolites of oxygen and nitrogen: relevance to ischemic heart disease. Free Radic Biol Med 25:404–433
Botha AJ, Moore FA, Moore EE, Sauaia A, Banerjee A, Peterson VM (1995) Early neutrophil sequestration after injury: a pathogenic mechanism for multiple organ failure. J Trauma 39:411–417
Ng CK, Deshpande SS, Irani K, Alevriadou BR (2002) Adhesion of flowing monocytes to hypoxia-reoxygenation-exposed endothelial cells: role of Rac1, ROS, and VCAM-1. Am J Physiol Cell Physiol 283:C93–102
Kaminski KA, Bonda TA, Korecki J, Musial WJ (2002) Oxidative stress and neutrophil activation-the two keystones of ischemia/reperfusion injury. Int J Cardiol 86:41–59
Lakshminarayanan V, Lewallen M, Frangogiannis NG, Evans AJ, Wedin KE, Michael LH, Entman ML (2001) Reactive oxygen intermediates induce monocyte chemotactic protein-1 in vascular endothelium after brief ischemia. Am J Pathol 159:1301–1311
Forde RC, Fitzgerald DJ (1997) Reactive oxygen species and platelet activation in reperfusion injury. Circulation 95:787–789
Flaring UB, Rooyackers OE, Wernerman J, Hammarqvist F (2003) Temporal changes in muscle glutathione in ICU patients. Intensive Care Med 29:2193–2198
Laplace C, Huet O, Vicaut E, Benhamou D, Duranteau J (2003) Endothelial oxidative stress is correlated with haemorrhagic shock severity in trauma patients. Intensive Care Med 29 [Suppl 1]:S123–S145
Corda S, Laplace C, Vicaut E, Duranteau J (2001) Rapid reactive oxygen species production by mitochondria in endothelial cells exposed to tumor necrosis factor-alpha is mediated by ceramide. Am J Respir Cell Mol Biol 24:762–768
Sawada GA, Raub TJ, Decker DE, Buxser SE (1996) Analytical and numerical techniques for the evaluation of free radical damage in cultured cells using scanning laser microscopy. Cytometry 25:254–262
Rothe G, Valet G (1990) Flow cytometric analysis of respiratory burst activity in phagocytes with hydroethidine and 2′,7′-dichlorofluorescin. J Leukoc Biol 47:440–448
Vanden Hoek TL, Becker LB, Shao Z, Li C, Schumacker PT (1998) Reactive oxygen species released from mitochondria during brief hypoxia induce preconditioning in cardiomyocytes. J Biol Chem 273:18092–18098
Duranteau J, Chandel NS, Kulisz A, Shao Z, Schumacker PT (1998) Intracellular signaling by reactive oxygen species during hypoxia in cardiomyocytes. J Biol Chem 273:11619–11624
Wiles ME, Hechtman HB, Morel NM, Shepro D (1993) Hypoxia reoxygenation-induced injury of cultured pulmonary microvessel endothelial cells. J Leukoc Biol 53:490–497
Zweier JL, Kuppusamy P, Lutty GA (1988) Measurement of endothelial cell free radical generation: evidence for a central mechanism of free radical injury in postischemic tissues. Proc Natl Acad Sci U S A 85:4046–4050
Li C, Jackson RM (2002) Reactive species mechanisms of cellular hypoxia-reoxygenation injury. Am J Physiol Cell Physiol 282:C227–C241
Eichelbronner O, Sibbald WJ, Chin-Yee IH (2003) Intermittent flow increases endotoxin-induced adhesion of human erythrocytes to vascular endothelial cells. Intensive Care Med 29:709–714
Botha AJ, Moore FA, Moore EE, Peterson VM, Goode AW (1997) Base deficit after major trauma directly relates to neutrophil CD11b expression: a proposed mechanism of shock-induced organ injury. Intensive Care Med 23:504–509
Seekamp A, Jochum M, Ziegler M, van Griensven M, Martin M, Regel G (1998) Cytokines and adhesion molecules in elective and accidental trauma-related ischemia/reperfusion. J Trauma 44:874–882
Solomkin JS (2001) Focus on “Essential role for IL-6 in postresuscitation inflammation in hemorrhagic shock.” Am J Physiol Cell Physiol 280:C237–C238
Tamion F, Richard V, Lyoumi S, Daveau M, Bonmarchand G, Leroy J, Thuillez C, Lebreton JP (1997) Gut ischemia and mesenteric synthesis of inflammatory cytokines after hemorrhagic or endotoxic shock. Am J Physiol 273:G314–G321
Yao YM, Redl H, Bahrami S, Schlag G (1998) The inflammatory basis of trauma/shock-associated multiple organ failure. Inflamm Res 47:201–210
Yokoyama Y, Kitchens WC, Toth B, Schwacha MG, Rue LW 3rd, Bland KI, Chaudry IH (2004) Role of IL-10 in regulating proinflammatory cytokine release by Kupffer cells following trauma-hemorrhage. Am J Physiol Gastrointest Liver Physiol 286:G942–G946
Mueller A, Kreuzfelder E, Nyadu B, Lindemann M, Rebmannn V, Majetschak M, Obertacke U, Schade UF, Nast-Kolb D, Grosse-Wilde H (2003) Human leukocyte antigen-DR expression in peripheral blood mononuclear cells from healthy donors influenced by the sera of injured patients prone to severe sepsis. Intensive Care Med 29:2285–2290
Botha AJ, Moore FA, Moore EE, Peterson VM, Silliman CC, Goode AW (1996) Sequential systemic platelet-activating factor and interleukin 8 primes neutrophils in patients with trauma at risk of multiple organ failure. Br J Surg 83:1407–1412
Zallen G, Moore EE, Johnson JL, Tamura DY, Aiboshi J, Biffl WL, Silliman CC (1999) Circulating postinjury neutrophils are primed for the release of proinflammatory cytokines. J Trauma 46:42–48
Rhee P, Wang D, Ruff P, Austin B, DeBraux S, Wolcott K, Burris D, Ling G, Sun L (2000) Human neutrophil activation and increased adhesion by various resuscitation fluids. Crit Care Med 28:74–78
Remondino A, Kwon SH, Communal C, Pimentel DR, Sawyer DB, Singh K, Colucci WS (2003) Beta-adrenergic receptor-stimulated apoptosis in cardiac myocytes is mediated by reactive oxygen species/c-Jun NH2-terminal kinase-dependent activation of the mitochondrial pathway. Circ Res 92:136–138
Troadec JD, Marien M, Darios F, Hartmann A, Ruberg M, Colpaert F, Michel PP (2001) Noradrenaline provides long-term protection to dopaminergic neurons by reducing oxidative stress. J Neurochem 79:200–210
Bleeke T, Zhang H, Madamanchi N, Patterson C, Faber JE (2004) Catecholamine-induced vascular wall growth is dependent on generation of reactive oxygen species. Circ Res 94:37–45
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Laplace, C., Huet, O., Vicaut, E. et al. Endothelial oxidative stress induced by serum from patients with severe trauma hemorrhage. Intensive Care Med 31, 1174–1180 (2005). https://doi.org/10.1007/s00134-005-2737-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-005-2737-7