Abstract
Developmental dysplasia of the hip (DDH) is characterized by the pathomorphology of inadequate acetabular coverage of the femoral head leading to increased loading of the articular surface and acetabular rim. If left untreated, this ultimately leads to osteoarthritis. Germany introduced a nationwide universal ultrasound screening program for all newborn infants in 1996. Subsequently, the incidence of undiagnosed hip dislocation was significantly reduced. In this consecutive series of patients who underwent periacetabular osteotomy for the treatment of symptomatic dysplasia of the hip between October 2014 and October 2022 data regarding the U3 screening examination were analyzed. The data included whether the examination was performed, whether the findings were positive or negative, whether the patients underwent any form of treatment in the case of a positive finding and whether a control X‑ray was performed. This study provides evidence that acetabular undercoverage cannot be ruled out based on a normal finding in ultrasonography screening. Furthermore, the study also shows that residual dysplasia may persist despite attempts of conservative treatment.
Graphic abstract

Zusammenfassung
Das Krankheitsbild der entwicklungsbedingten Hüftdysplasie („developmental dysplasia of the hip“, DDH) ist pathomorphologisch charakterisiert durch eine unzureichende Überdachung des Hüftkopfes durch das Acetabulum. Diese Inkongruenz der Artikulation führt zu einer erhöhten Belastung der Gelenkflächen sowie des Pfannenrandes und unbehandelt letztendlich zu einer Arthrose des Hüftgelenks. In Deutschland wurde 1996 ein flächendeckendes Ultraschallscreening der Hüftgelenke für alle Neugeborenen eingeführt. Daraufhin sank die Zahl der nicht diagnostizierten Hüftluxationen signifikant. In dieser konsekutiven Serie von Patienten, bei denen zwischen Oktober 2014 und Oktober 2022 eine periacetabuläre Osteotomie zur Behandlung einer symptomatischen Hüftdysplasie durchgeführt worden war, wurden die Daten zur U3-Vorsorgeuntersuchung analysiert. Unter anderem wurde erfasst, ob die Untersuchung durchgeführt wurde, ob der Befund regelhaft oder pathologisch war, ob die Patienten im Falle eines pathologischen Befundes in irgendeiner Form behandelt wurden und ob ein Kontrollröntgenbild angefertigt wurde. Diese Studie erbringt die Evidenz dafür, dass ein Defizit der acetabulären Überdachung des Hüftgelenks aufgrund eines regelhaften Befundes im Rahmen des Ultraschallscreenings nicht ausgeschlossen werden kann. Darüber hinaus verdeutlicht die Studie auch, dass trotz konservativer Behandlungsversuche eine Restdysplasie bestehen bleiben kann.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
A universal nationwide ultrasound screening program was introduced in Germany in 1996 to reduce the incidence of developmental dysplasia of the hip (DDH). Despite the introduction of this program, a rise in young adults with symptomatic acetabular undercoverage seeking treatment in hip preservation centers is being seen. This study shows that acetabular undercoverage cannot be ruled out based on a normal ultrasound finding at neonatal screening.
Introduction
Developmental dysplasia of the hip (DDH) is characterized by the pathomorphology of insufficient acetabular coverage of the femoral head, resulting in instability and increased loading of the articular surface and acetabular rim. These pathological loads on the articular cartilage, if left undetected or untreated, lead to intra-articular structural damage and subsequently to the development of secondary osteoarthritis of the hip joint. It is estimated that approximately 20–40% of all cases of adult hip osteoarthritis are due to unrecognized or untreated DDH [1]. The prevalence of DDH in the population can range from 1% to 40% depending on a multitude of factors including ethnicity, gender, pregnancy-related aspects and radiographic thresholds of definition [2,3,4,5]. In general, a lateral central edge angle (LCEA) of < 20°, an acetabular index (AI) > 15°, and a femoral head extrusion index (EI) > 25% on a mature anteroposterior (AP) pelvic radiograph are signs of undercoverage in terms of DDH [6, 7]. If insufficient acetabular roofing is detected in early childhood, it can be often addressed with non-surgical methods of splinting [8]. In skeletally mature patients, reorientation osteotomy represents the gold standard for treatment of the underlying pathomorphology. The two most prominent types of osteotomy that are commonly performed in adults include the triple Tönnis osteotomy and the periacetabular Ganz osteotomy (PAO) [9, 10].
It has been well described that DDH is frequently abundant despite the absence of common risk factors, making selective screening difficult [11]. Therefore, Germany introduced a nationwide ultrasound screening program in 1996 for all newborn infants using the Graf method. This procedure is commonly referred to as the U3 check-up examination [12, 13].
The effectiveness of ultrasonography as a preventive measure is determined by the subsequent need for a treatment intervention on detection of DDH. Several studies underline the potential of universal ultrasound screening as a successful and cost-efficient preventive tool [14, 15]. Von Kries et al. demonstrated that introduction of sonography as part of the screening examination in Germany significantly reduced the need for surgical interventions in children up to 5 years of age [16]. The examiner evaluates the bony and cartilaginous roof of the acetabulum by measuring the alpha and beta angles and describes the position of the femoral head within the acetabulum.
Despite the introduction of screening programs, there has been a rise in young adults with symptomatic acetabular undercoverage seeking treatment in hip preservation centers. This is accompanying increased awareness and the recent emergence of the field of hip preservation surgery.
It was the aim of this study to focus on a consecutive cohort of patients undergoing PAO surgery for symptomatic hip dysplasia. It was hypothesized that patients undergoing PAO surgery showed positive ultrasonography findings as infants.
Methods
A consecutive series of patients who underwent periacetabular osteotomy for the treatment of symptomatic dysplasia of the hip between October 2014 and October 2022 were considered for inclusion in the study. Inclusion criteria were symptomatic hip dysplasia that was diagnosed based on an anteroposterior (AP) pelvic radiograph. All radiographs were obtained in a standardized manner as previously described by Tannast et al. [7] and three radiographic findings were necessary for the diagnosis of dysplasia, a lateral center edge angle (LCEA) of ≤ 20°, anterior wall coverage (AC) of < 15° and an acetabular extrusion index (EI) of > 25%. Patients fulfilling these criteria and undergoing PAO were considered eligible for inclusion in the study. Patients who underwent PAO for acetabular retroversion, posterior dysplasia, or for deformities in association with neuromuscular diseases, were excluded to ensure the homogeneity of the cohort.
After obtaining formal consent for anonymous analysis of data, patients were contacted for retrieval of a simple set of data regarding the U3 screening examination including whether the examination was performed, whether the findings were positive or negative, whether the patients underwent any form of treatment in the case of a positive finding and whether a control X‑ray was performed.
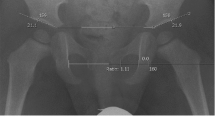
Demographic data of all patients were tabulated. In addition to the abovementioned radiographic measures that were used for surgical indications, the acetabular index and posterior wall coverage were also measured to enable a global depiction of acetabular coverage (Fig. 1).
Anteroposterior (AP) pelvic radiographs of the radiological measurement in native pelvic X‑ray obtained in a standardized manner as previously described by Tannast et al. a Lateral center edge angle, b acetabular index, c extrusion index (x /y ×100), d anterior coverage (A /B ×100) and e posterior coverage (A /B ×100). Red dot femoral head center, white line axis of the femoral neck, pink line rim of the anterior or posterior acetabulum
Due to the retrospective nature and inhomogeneity of reporting, the results were documented based on a binary scale of either Graf I normal finding or Graf II–IV abnormal finding requiring a Pavlic harness, splinting or surgery.
Comparison between groups was performed using an unpaired t test. A normal distribution was assumed. Values were expressed as mean and standard deviation. Positive predictive values were calculated. P-values of < 0.05 were considered significant. Statistical analysis was performed using IBM® SPSS® Statistics software version 28.0.1.1 (14) (64 bit version, IBM, Chicago, IL, USA) and Microsoft® Excel version 16.43 (Microsoft, Redmond, WA, USA).
Results
From a total of 134 patients, 92 individual patients managed to provide a conclusive result of their infant screening. Of these, 82 (89.1%) patients were females and 10 (10.9%) males. The mean age at time of surgery was 27.4 years (standard deviation, SD±7.3 years, range 14.6–41.5 years). The mean acetabular morphometric measures prior to PAO were: LCEA 13.5° (SD±6.1°, range −6.2–24.5°), AI 16.3° (SD±6.3°, range 6.3–42.1°), EI 27.7% (SD±7.4%, range 12.0–56.0%), AC 36.2% (SD±15.5%, range 0.0–71.0%) and PC 79.3% (±21.0%, range 0.0–124.0%) (Fig. 2). All patients underwent U3 ultrasonography screening of the hip as infants. In 47 cases (51.1%) ultrasonography revealed a positive finding (Graf > 1) and 45 (48.9%) hips were reported to be normal (Graf 1) at U3 and needed to undergo pelvic osteotomy in adulthood due to hip dysplasia. The true positive rate (sensitivity) of ultrasonography was calculated to be 51.0%. Both patient groups with DDH detection and without DDH detection in the U3 examination, did not differ regarding gender distribution, time point of surgery and radiographic acetabular measurements (Table 1, Fig. 1, p > 0.05). Figure 3 shows the rate and distribution of treatment in patients with positive findings and depicts whether a pelvic X‑ray was performed after skeletal maturity.
Comparison of radiological parameters in the mature pelvis in AP projection showed no significant difference between patients presenting with sonographic hip development Graf 1 or Graf > 1 in U3 examination. LCEA lateral center edge angle, AI acetabular index, EI extrusion index, PC posterior coverage, AC anterior coverage
Discussion
The most important finding of this study was that 50% of young adults undergoing periacetabular osteotomy for DDH in a German institution reported a nonpathological neonatal hip sonography scan result. The low sensitivity of 50% underlines a high likelihood of misdiagnosing a hip that is likely to develop symptoms due to acetabular coverage.
Reports of this type are lacking in the literature. This is due to the concept of this study that was intended to put the focus on the morphology of acetabular undercoverage after skeletal maturity.
There have been reports looking into the diagnostic and screening value of sonography in preventing treatment in infants and toddlers. Ihme et al. found that on average 0.26 of 1000 infants received treatment for DDH at the age of 10 months to 5 years despite unremarkable sonographic screening of the hip [12]. A slightly higher incidence rate of 0.74 per 1000 births was described by Clarke et al. for selective DDH sonography screening [17].
The problematic issue of technical mistakes and misinterpretation of anatomic structures during hip sonography have previously been outlined [18]. The German Association of Statutory Health Insurance Physicians reported that 32% of consultants who applied for initial certification in infant hip sonography did not undertake adequate training [19]. Bucher et al. reported that the initial diagnosis at neonatal sonography screening of 132 neonates was confirmed by a certified pediatrician in only 75 cases [20].
It has been shown that the successful implementation of newborn screening was accompanied by a subsequent reduction in the rate of open surgery. This is likely due to the reduced incidence of neglected hip dislocation; however, the prevalence of acetabular undercoverage in the adult population remains high with late onset of symptoms at various stages of life depending on the severity of disease [12, 21, 22]. This form of DDH is also known as adolescent-onset acetabular dysplasia and is commonly associated with a greatly reduced hip and acetabular undercoverage. The causes of late-onset acetabular dysplasia are not fully understood. A possible explanation was described by Tönnis and Remus in a case series, demonstrating irregular calcification and structural irregularities of the triradiate cartilages in the acetabular roof and superior acetabular rim in patients with adolescent-onset acetabular dysplasia [23]. The extent to which further radiological screening is necessary after skeletal maturity should be assessed in the presence of symptoms or risk factors. The high prevalence and consequences of late-onset acetabular dysplasia have been underlined in arthroplasty registries. It was shown that one third of arthritic hips undergoing hip replacement surgery before the age of 60 years showed signs of acetabular undercoverage [24].
Based on the results of the current study, half of all patients undergoing pelvic osteotomy had some form of conservative treatment due to a positive sonography finding; however, only a minority of these patients received further imaging after skeletal maturity to evaluate the morphology of the developed acetabulum.
Delayed growth rate of the acetabular roof with subsequent lower shape differentiation of the roof also seems to be associated with splinting and cast treatment and might be responsible for later forms of dysplasia [12, 25].
A study by Sarkissian et al. [26] emphasized the usefulness of a follow-up X‑ray examination in the case of unremarkable hip sonography or after successful conservative therapy. The study examined 115 children over a period of 4 years who had abnormal findings on infant hip sonography at the time of birth. All these 115 patients showed clinical as well as sonographic normalization of findings after conservative therapy. An additional pelvic X‑ray of these children was performed at 6 and 12 months after birth, which showed evidence of residual DDH in 17% of these patients, despite the normal clinical and sonographic findings.
Conclusion
Hip dysplasia is a complex, divergent and multifactorial disease that may present in different stages of life based on the severity of the underlying pathomorphology. The U3 ultrasonography examination that was introduced in Germany for universal DDH screening in 1996 has effectively reduced surgical interventions in the early years and nearly eliminated the entity of neglected hip dislocation. With increasing awareness in the area of hip preservation in young adults, it is becoming clear that milder forms of dysplasia are a frequent cause of hip pain in young adults. This study underlines that acetabular undercoverage cannot be ruled out based on a normal finding of ultrasonography screening. Furthermore, the study also showed that residual dysplasia may persist despite conservative treatment. It is therefore encouraged to perform a follow-up pelvic X‑ray after skeletal maturity for hips that had undergone conservative treatment. Furthermore, every symptomatic hip in young adulthood must be considered at risk of being dysplastic until proven otherwise and referred for further evaluation by an adult hip specialist.
Abbreviations
- AC:
-
Anterior coverage
- AI:
-
Acetabular index
- AP:
-
Anteroposterior
- DDH:
-
Developmental dysplasia of the hip
- EI:
-
Femoral head extrusion index
- LCEA:
-
Lateral central edge angle
- PAO:
-
Periacetabular osteotomy
- PC:
-
Posterior coverage
- U3:
-
Postnatal infant examination at 3–8 weeks
References
Gala L, Clohisy JC, Beauĺe PE (2016) Current concepts review hip dysplasia in the young adult. J Bone Joint Surg Am. https://doi.org/10.2106/JBJS.O.00109
Wilkin GP, Ibrahim MM, Smit KM, Beaulé PE (2017) A contemporary definition of hip dysplasia and structural instability: toward a comprehensive classification for acetabular dysplasia. J Arthroplasty. https://doi.org/10.1016/j.arth.2017.02.067
Pun S (2016) Hip dysplasia in the young adult caused by residual childhood and adolescent-onset dysplasia. Curr Rev Musculoskelet Med. https://doi.org/10.1007/s12178-016-9369-0
Jacobsen S, Sonne-Holm S (2005) Hip dysplasia: A significant risk factor for the development of hip osteoarthritis. A cross-sectional survey. Rheumatology. https://doi.org/10.1093/rheumtology/keh436
Loder RT, Skopelja EN (2011) The epidemiology and demographics of hip dysplasia. isrn Orthop. https://doi.org/10.5402/2011/238607
Ahmad SS, Haertlé M, Konrads C, Derksen A, Windhagen HNW (2022) The scientific evolution of periacetabular osteotomy: a global review. J Clin Med. https://doi.org/10.3390/jcm11206099
Tannast M, Hanke MS, Zheng G, Steppacher SD, Siebenrock KA (2015) What are the radiographic reference values for acetabular under- and overcoverage? Clin Orthop Relat Res. https://doi.org/10.1007/s11999-014-4038-3
Gather KS, Mavrev I, Gantz S, Dreher T et al (2022) Outcome prognostic factors in MRI during spica cast therapy treating developmental hip dysplasia with midterm follow-up follow-Uptle. Children 9(7):1010. https://doi.org/10.3390/children9071010
Ahmad SS, Haertlé M, Konrads C, Derksen A, Windhagen H, Wirries N (2022) The scientific evolution of Periacetabular osteotomy: a global review. J Clin Med. https://doi.org/10.3390/jcm11206099
Selberg CM, Chidsey B, Skelton A, Mayer S (2020) Pelvic osteotomies in the child and young adult hip: indications and surgical technique. J Am Acad Orthop Surg. https://doi.org/10.5435/JAAOS-D-19-00223
Chan A, Cundy PJ, Foster BK, Keane RJ, Byron-Scott R (1999) Late diagnosis of congenital dislocation of the hip and presence of a screening programme: South Australian population-based study. Lancet. https://doi.org/10.1016/S0140-6736(98)12469-8
Ihme N, Altenhofen L, von Kries R et al (2008) Sonographisches Hüftscreening in Deutschland. Orthopade. https://doi.org/10.1007/s00132-008-1237-1
Biedermann R, Eastwood DM (2018) Universal or selective ultrasound screening for developmental dysplasia of the hip? A discussion of the key issues. J Child Orthop. https://doi.org/10.1302/1863-2548.12.180063
Thaler M, Biedermann R, Lair J, Krismer M, Landauer F (2011) Cost-effectiveness of universal ultrasound screening compared with clinical examination alone in the diagnosis and treatment of neonatal hip dysplasia in Austria. J Bone Joint Surg Br. https://doi.org/10.1302/0301-620X.93B8.25935
Graf R (2007) Hip sonography: 20 years experience and results. hip Int. https://doi.org/10.1177/112070000701705s02
Von Kries R, Ihme N, Altenhofen L, Niethard FU, Krauspe R, Rückinger S (2012) General ultrasound screening reduces the rate of first operative procedures for developmental dysplasia of the hip: a case-control study. J Pediatr. https://doi.org/10.1016/j.jpeds.2011.08.037
Clarke NMP, Reading IC, Corbin C, Taylor CC, Bochmann T (2012) Twenty years experience of selective secondary ultrasound screening for congenital dislocation of the hip. Arch Dis Child. https://doi.org/10.1136/archdischild-2011-301085
Graf R (2017) Hip sonography: background; technique and common mistakes; results; debate and politics; challenges. hip Int. https://doi.org/10.5301/hipint.5000514
Kassenärztliche-Bundesvereinigung (2019) Qualitätsbericht Kassenärztliche-Bundesvereinigung 2018. https://www.kbv.de/media/sp/KBV_Qualitaetsbericht_2018.pdf
Bucher F, Görg C, Weber S, Peterlein CD (2021) Paediatric hip ultrasound: Uncertainties in examination and choice of treatment. J Child Orthop. https://doi.org/10.1302/1863-2548.15.200084
Sink EL, Ricciardi BF, Torre K, Price CT (2014) Selective ultrasound screening is inadequate to identify patients who present with symptomatic adult acetabular dysplasia. J Child Orthop. https://doi.org/10.1007/s11832-014-0620-1
Schams M, Labruyère R, Zuse A, Walensi M (2017) Diagnosing developmental dysplasia of the hip using the Graf ultrasound method: risk and protective factor analysis in 11,820 universally screened newborns. Eur J Pediatr. https://doi.org/10.1007/s00431-017-2959-z
Tönnis D, Remus W (2004) Development of hip dysplasia in puberty due to delayed ossification of femoral nucleus, growth plate and triradiate cartilage. J Pediatr Orthop Part B. https://doi.org/10.1097/01202412-200409000-00001
Furnes O, Lie SA, Espehaug B, Vollset SE, Engesaeter LB, Havelin LI (2001) Hip disease and the prognosis of total hip replacements. A review of 53,698 primary total hip replacements reported to the Norwegian Arthroplasty Register 1987–99. J Bone Joint Surg Br 83(4):579
Kraus T, Novak M (2018) Kindliche Hüftreifungsstörungen. Paediatr Paedolog Austria. https://doi.org/10.1007/s00608-018-0611-4
Sarkissian EJ, Sankar WN, Zhu X, Wu CH, Flynn JM (2015) Radiographic follow-up of DDH in infants: are X‑rays necessary after a normalized ultrasound? J Pediatr Orthop. https://doi.org/10.1097/BPO.0000000000000326
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M. Haertlé, H. Hawi, H. Windhagen, N. Becker and S.S. Ahmad declare that they have no competing interests.
All procedures performed in studies involving human participants or on human tissue were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Declaration of Helsinki and its later amendments or comparable ethical standards. The study was approved by the local ethics committee of the Hannover Medical School (code: 10405_BO_K_2022). Informed consent was obtained from all individual participants included in the study.
Additional information

Scan QR code & read article online
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Haertlé, M., Hawi, H., Windhagen, H. et al. Fifty percent of patients undergoing periacetabular osteotomy for hip dysplasia showed normal findings upon neonatal ultrasound screening. Orthopädie 52, 313–319 (2023). https://doi.org/10.1007/s00132-023-04357-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00132-023-04357-7
Keywords
- Infant hip sonography
- Acetabulum
- Reorientation osteotomy
- Developmental hip dysplasia
- Secondary hip osteoarthritis