Abstract
Purpose
To examine the nature of positive and negative environmental change on clinical outcome in 210 patients presenting with anxiety and depression and followed up over 30 years.
Methods
In addition to clinical assessments, major environmental changes, particularly after 12 and 30 years, were recorded in all patients by a combination of self-report and taped interviews. Environmental changes were separated into two major groups, positive or negative, determined by patient opinion.
Results
In all analyses positive changes were found to be associated with better outcome at 12 years with respect to accommodation (P = 0.009), relationships (P = 007), and substance misuse (P = 0.003), with fewer psychiatric admissions (P = 0.011) and fewer social work contacts at 30 years (P = 0.043). Using a consolidated outcome measure positive changes were more likely than negative ones to be associated with a good outcome at 12 and 30 years (39% v 3.6% and 30.2% v 9.1%, respectively). Those with personality disorder at baseline had fewer positive changes (P = 0.018) than others at 12 years and fewer positive occupational changes at 30 years (P = 0.041). Service use was greatly reduced in those with positive events with 50–80% more time free of all psychotropic drug treatment (P < 0.001). Instrumental positive change had greater effects than imposed changes.
Conclusions
Positive environmental change has a favourable impact on clinical outcome in common mental disorders. Although studied naturalistically in this study the findings suggest that if harnessed as a therapeutic intervention, as in nidotherapy and social prescribing, it would yield therapeutic dividends.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Although it is widely appreciated that environmental factors have a major role in the outcome of mental illness most of the evidence is retrospective. Principally, the influence of deprivation, abuse and neglect early in life has been shown to be responsible for, or at least heavily implicated in, the later manifestation of mental disorder, both in adolescence and adult life [1,2,3,4]. The study of life events has also reinforced awareness that the environment is a trigger for many illness episodes [5,6,7,8,9], but not necessarily a reason for greater psychiatric consultations [10].
Prospective studies of environmental change sometimes have the advantage of agency; they can be manipulated and otherwise altered to influence mental illness. The evidence that investment in occupational interventions [11, 12], ‘green care’ and other activities linked to the natural world [13, 14], and drama [15] can all have benefits for mental health is strong but still needs more vigorous evaluation.
But in evaluating the positive effects of environmental change in mental disorders there are few studies that evaluate the relative effects of environment and standard treatments, especially over the longer term. The opportunity to compare the relationship between clinical interventions and environmental factors came about in a long-term follow-up study of common mental illness, the Nottingham Study of Neurotic Disorder.
In this study, carried out between 1983 and 2019, 210 patients presenting at general practice psychiatric clinics with the most common mental disorders, anxiety and depression, were first involved in a 10 week randomised trial of treatments [16] and then followed up over a 30 year period. The most detailed data were obtained at the 12 year and 30 year follow-up points in the study.
Method
The Nottingham Study of Neurotic Disorder recruited patients from general practice psychiatric clinics in Nottingham between 1983 and 1987. These clinics were set up primarily to improve liaison with general practitioners and were commonly used in the latter years of the twentieth century to extend community care [17, 18] and reduce psychiatric admissions [19]. As patients were seen at an early stage they could be regarded as more representative of mental illness in the community than those seen in standard out-patient clinics.
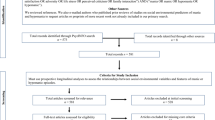
In the first phase of the study 210 patients were randomised to drug treatment (n = 84) (separated into the antidepressant, dothiepin [n = 28], the anti-anxiety drug, diazepam [n = 28], and placebo [n = 28]), cognitive behaviour therapy (n = 84), and self-help (n = 42). Each of these were given for 6 weeks and then tapered so that at 10 weeks-the patients were on no therapy [16]. Normal clinical care was then followed but if patients had improved on their randomised treatment they were given the option of continuing in the same mode (i.e. drugs, psychological treatment or self-help) subsequently and most did so in the first 2 years after randomisation, with the one exception being the prescription of benzodiazepines, which were prescribed similarly in all groups [20]. After 2 years, follow-up care continued as necessary and the study became a cohort one.
The inclusion criteria for the original trial were (i) no active psychiatric treatment at entry, (ii) informed consent, (iii) a diagnosis of either GAD, panic disorder or dysthymic disorder (or any mixture of these), using the Structured Clinical Interview for DSM-III [21] and (iv) no history of other presumed independent psychiatric illness (schizophrenia, bipolar disorder or alcohol or drug addiction).
Follow-up
Patients were followed up and had clinical assessments 16, 32, 52 and 104 weeks after randomisation and at 5 years had their service contacts recorded by examination of notes but without being interviewed [22]. Full clinical and environmental assessments were carried out at 12 and 30 years.
The primary outcome at 30 years was the absence of a DSM diagnosis of any affective (including anxiety) disorder [23]. As long-term outcome includes many elements beyond clinical symptoms a combined symptomatic, social, and service outcome was generated in advance of any analysis to allow good, intermediate, and poor outcomes to be generated.
The 30-year follow-up also allowed a better assessment of long-term outcomes. One of the difficulties in comparing the impact of environmental changes, particularly in the context of standard therapeutic interventions, is that of time. Standard drug and psychological treatments tend to have their main effects within a matter of weeks or days, whereas the effects of environmental changes, unless they are specifically formulated as short term (e.g. as in randomised trials of interventions such as singing [24] are usually delayed. As in the Nottingham Study of Neurotic Disorder major data were collected at 12 and 30 years the option of testing together both clinical and environmental outcomes was taken up (Table 1).
Outcomes recorded over the 30 year follow-up
There were four key points at which a range of clinical and environmental outcomes were assessed over the time course of the study (Table 1).
Many of the outcome measures were closely related and so their specific data are not recorded here. These include the MADRS scale for depression [25], the Brief Anxiety Scale [26], both subdivisions of the Comprehensive Psychopathological Rating Scale (CPRS) [27], and the Hospital Anxiety and Depression Scale [28]. The general neurotic syndrome, a Galenic syndrome [29] recorded in the study [23], also correlates highly with other measures, particularly personality status. For this reason, only one symptomatic outcome, the scores on the CPRS, was included in a putative combined outcome scale. Other broader items included were social function and scores on the Neurotic Disorder Outcome Scale (NDOS) [30], a 10 point measure of longitudinal outcome.
Before analysis the subjects were separated into good, intermediate and poor outcome groups. The criteria for each element of the scale are indicated in Table 2.
The environmental hypothesis at the start of the study in 1983 was a general one, that ‘environmental factors would have at least an equivalent influence on long-term outcome than clinical ones’. A subsidiary hypothesis was that personality disorder would be more susceptible to negative environmental factors than clinical symptoms, as this had been found in previous studies [35, 36].
Personality status
Personality assessment was made at baseline by previously trained independent researchers (all psychiatrists) using the Personality Assessment Schedule (PAS) [37,38,39]. The basic principle behind the PAS is that personality disturbance is best viewed as a spectrum between normal personality function and severe personality dysfunction and this has now been adopted as the new ICD-11 classification of personality disorder [40]. A previous study examined the baseline PAS scores and the criteria for the ICD-11 classification were adjusted to be concordant with ICD-11 [41].
Environmental outcomes and service costs
Assessments of environmental changes recorded over the 30 year study period are summarised in Table 1.
Preferred treatment
After the assessments made at 12 and 30 years each patient was asked to rate which treatment in the past 12- or 18-year-period, respectively had helped them most. The options given were (a) drug treatment, (b) psychological treatment (of any sort), (c) self-help (including self-help groups, books or other media, (d) no treatment was superior to any other, and (e) nothing helped. Patients were also asked follow-up questions to amplify their responses and the answers noted down. These helped to decide on the impact of each environmental change.
Major life changes
A life chart was constructed for each patient at 12 and 30 years and all relevant events noted together with their date of onset. A previous study covering the first 2 years of the Nottingham study had shown that those with some personality disorders had more, mainly negative, life events than others [36]. The event choices were made from the Paykel Life Events scale [42].
Perceived positive events
Perceived positive events were recorded from a combination of answers to questions at interview, the information from the life charts and events scales and the comments about preferred treatment. In almost all cases these responses were congruent and there was no need for another independent assessment.
Perceived negative events
This followed the same principle as for positive events and also used the same three sources of data.
As a separate component to the study the environmental changes were classified as either (i) spontaneous or unavoidable (e.g., death of close relative, serious illness, standard date of retirement), (ii) created by decisions made by the patient, (iii) created by individuals on behalf of the patient, and (iv) created by others independently of the patient, were separated into positive instrumental changes, those carried out for the intended benefit of the patient, or positive imposed changes, those instigated by others with no patient involvement. A similar distinction was made for negative changes.
Differentiation of environmental changes and relationship to life events
The environmental changes chosen in the methodology were a combination of both independent and contextual life events and decision making that led to important change that could not easily be defined as a life event (e.g., a personal decision to end alcohol abuse). For this reason the assessments made went beyond the methodology of life event literature, which generally has been focused on threats [43] rather than positive change. But if one uses the broadest definition of a life event as any life change that has an impact on psychological well-being [44] then all changes are life events. A small proportion of the changes also came about as a consequence of therapeutic intervention by a mental health professional and so were not typical life events. Planned environmental change to improve mental health is formalised as nidotherapy [45, 46] and examination of the data by all the authors confirmed that some of the interventions could be classed as nidotherapy. In examining the elements of change, an attempted consensus was made after examining all the data, including short voice recordings of the interviews after they had been completed.
Social function
Social function was measured using the Social Functioning Questionnaire (SFQ) [32], an 8 item scale with scores between 0 and 3 for each item, with a maximum score of 24. High scores indicate poor social function.
The primary clinical outcome, a simple one recommended at the beginning of the study by Sir Richard Doll [23] was the absence or presence of a significant DSM-III diagnosis (excluding adjustment and simple stress reactions and simple phobias). The principal secondary outcome was the score on the Social Functioning Questionnaire (SFQ), a measure which is correlated strongly with personality status [33, 47].
At 12 years all service costs were recorded using a combination of questions at interview and examination of the general practice notes (approved in advance as part of the ethical submission). At 30 years notes were not examined so exact details of out-patient appointments could not be determined, but admissions to hospital, suicide episodes, social work and day centre contacts, and details of drug treatments were obtained at interview [48].
Statistical analysis
The analysis was carried out for the periods of 0–12 years and 13–30 years separately, to examine the impact of environmental changes and nidotherapy during the first 12 years and the remaining 18 years on the combined outcome scales, personality status and use of services at the end of the two periods respectively. Due to missing data on different outcomes, the first 12-year period had available data points in the analysis between 175 and 182, and between 75 and 89 in the second 18-year period. Previous analysis of the cohort data suggested many of the missing data could be regarded as occurring at random [23]. Considering only small number of missing data at each period, list-wise deletion approach was used for all analyses in this study.
For continuous outcomes, geometric means and standard deviations by environment change level (no change, positive change and negative change) were presented. One-way analysis of variance was performed to test differences in the geometric means among change levels due to heterogeneity in variances among change levels, with 95% confidence intervals by change levels presented. For discrete outcomes, percentage by environment change level was presented and differences between change levels tested using Fisher’s exact test. Since descriptive analysis showed no significant difference in patients’ age and gender proportion by environment change levels, no adjustment for age and sex was made for comparison of all outcomes. However, in examining the impact of environmental changes on the combined outcome scale, we adjusted for personality status using multinomial models.
We used IBM SPSS v19 for most of the analysis, with MLwiN v3.03 for multinomial models.
Results
These are separated into five sections.
Environment and overall outcome
At 12 years, 176 subjects provided data, with 49 (27.8%) having a good outcome and 33 (18.8%) a poor one. Those with positive environmental changes were significantly more likely to have a good outcome (39.1%) and less likely a poor outcome (2.2%), compared with 3.6% good outcome and 39.3% poor outcome in those who had negative environmental change (P < 0.007 after adjustment) (Table 2). At 30 years, following attrition through death and failure to follow-up, only 85 subjects had data and although the results were similar with 16 (30.2%) having a good outcome after positive instrumental change compared with 1 (9.1%) after negative change this was not a significant difference (adjusted P = 0.3) (Table 2).
Type of environmental change and outcome
A much larger proportion of the cohort had positive environmental changes that could not be clearly identified as instrumental or imposed. In the first 12 years positive changes of accommodation (P = 0.009), relationships (P = 0.007), and substance use (P = 0.003) were all significantly associated with more good outcomes and less poor outcomes than no change group; at 30 years these differences did not reach significance (Table 3).
Impact of personality disorder
Patients diagnosed with personality disorder at 12 years had fewer positive events (26.1%) that those with no personality disorder (73.9%) (P = 0.018) (Table 4), mirroring the findings after 2 years [36], with occupational changes showing the largest differences between personality disorder and no disorder (P = 0.041) (Table 4).
Environmental change and service costs
The data showed that psychiatric admissions (P = 0.011) and social work contacts (P = 0.013) were significantly greater in those with negative environmental changes. The most marked difference was in the number of months without any psychotropic drugs being taken, with those having positive events had nearly twice the period being drug free compared with the other two groups at 12 years (Table 5).
Effects of therapeutically induced environmental change
The joint assessments of all the positive instrumental environmental changes also revealed that at least 6 of the 46 interventions in the first 12 years and 22 of the 45 interventions in the second 18 years were initiated by a mental health professional or a person with mental health skills. This type of intervention is now part of the interventions described as social prescribing and nidotherapy. The interventions with these numbers were too small to analyse but they do indicate that mental health staff have a potential role in initiating positive change.
Many of these changes and their major consequences were difficult to classify easily. Examples are given below.
Example 1: positive instrumental change
A housing advisor with persistent anxiety symptoms treated with medication became increasingly unhappy with the bureaucracy of her job and, after discussing options with her husband, decided to retire early and move to a seaside county 250 miles away. She and her husband settled in a village and quickly integrated into the local community. At 30-year follow-up she had lost all her original symptoms, had no psychiatric contact, was a valued member of a volunteer group helping older people in the village, and both she and her husband hosted village events in supporting a local charity.
Example 2: negative instrumental change
A patient living in an inner city ward gradually accumulated additional members of her family when they needed accommodation and so asked her housing association to be moved off so she could live in a flat on her own. But when this was arranged she was placed in a retirement complex on the edge of Nottingham where she became completely isolated and because transport was poor in the area she was very seldom visited. When assessed at follow-up, she took a very long time to answer the door as ‘I never have a visit nowadays’. Initially she had viewed the move as a positive one but it was clearly classed as negative at 30 years, after she had been living in the flat for 5 years, and regretted bitterly that she had made the housing request.
Example 3: positive imposed change
A man who had worked for an engineering company for most of his working life became increasingly stressed. He had frequent depressive episodes and became fearful of many of the tasks that were demanded of him. These became more complex and involved more travelling time than previously, especially when the company was put under economic pressure and laid off staff. Eventually he was made redundant. In retrospect, he thought this was the best thing that had ever happened to him. He got his life into balance, developed very good relationships with his grandchildren and moved to a smaller house needing little maintenance. At follow-up, he described himself as fully recovered with no contact with mental health services.
Example 4: negative imposed change
A highly anxious secretary with no friends maintained a level of stability by support from colleagues at work and her family. The support of her colleagues became even more important when her father died. Shortly after this she was made redundant when the company reorganised. At the time of follow up she was severely agoraphobic and virtually housebound, had self-harmed twice, was drinking to excess and taking benzodiazepines and two antidepressants continuously.
These examples indicate a mixture of occupational, accommodation and relationship changes. Some of the instrumental changes even had a spontaneous element to them.
Example 5: a fortuitous mixture of positive and negative events
A very anxious and depressed woman with frequent attacks of panic was never able to maintain regular employment and had a series of failed relationships. She was frequently suicidal and many of her self-harm episodes led to general hospital admission because they were so severe. On one of these occasions, she was looked after by a male nurse and they developed a cordial relationship. She continued to remain emotionally unstable and 2 years later took another large overdose and was readmitted to the same general hospital. By coincidence she was looked after by the same nurse who had seen her on the previous episode. Their relationship continued to grow and they remained in contact after her discharge. Shortly afterwards he proposed and they married. Their relationship continued to prosper but eight years later her husband died. But her mental stability remained reinforced and at follow-up, she was only taking benzodiazepines for anxiety, and broke off the follow-up interview at 6 pm to drink a toast to her husband, a ritual that had been carried out regularly since he died.
These descriptions indicate that a lot more needs to be done to describe these events systematically and comprehensively and new terminology may be needed.
Discussion
Main findings
In a well-known pioneering study Eysenck used national insurance data (Equitable Life Society) to show that the outcome of ‘neurosis’, as defined at that time, was the same as that achieved by formal psychotherapy. In both groups, about third of the people in each group improved and the rest either remained the same or became worse [49]. The results of the Nottingham Study were very similar to those of Eysenck after 30 years despite apparent advances in treatment. Close to a half still had a significant DSM diagnosis at assessment, with those with personality pathology having worse outcomes [23]. There was also little evidence that treatments given over the course of the study had major impact on outcome [48].
In interpreting the data the impact of environmental change features strongly. Those with positive environmental events had most of their pathology halved compared with those who had negative environmental events at 12 years and although the differences were less significant at 30 years account has to be taken of the smaller numbers in the 30-year follow up (Table 3). Those with common mental disorders who recognise environmental change and life events as positive have been shown in other studies to have better outcomes [50, 51].
The results give a strong indication that positive environmental factors, including a wide admixture of life events, are at least as effective, if not greater, than specific treatment interventions in common mental disorders. The clinical status of the patients overall was no better after 30 years than at baseline and yet there was clear evidence that some environmental changes had significant effects on outcome. Although it could be claimed that all the positive changes were standard life events some were much more complex as the case examples above indicate. When patients regarded the advice about smoking and drug behaviour, usually given in the first or second assessment, as critical in their improvement at 30 years, that cannot be regarded as a simple life event. The fact that this particular memory was so important after this long period indicates the potential power of the first psychiatric interview, when a comprehensive assessment is followed by a formulation of the problem in all its aspects.
The smaller number of positive environmental changes in those with personality disorder could have contributed to the generally worse outcome in this group, a finding that is now very well-known but not fully understood [52]. These patients also incurred greater costs than others at 12 years [53]. It is reasonable to suppose that if more positive events can generated in those with a tendency to negative interactions, as in personality disorder, these consequences could be reversed, particularly if environmental changes can reinforce personality strengths [54] that are protective in the longer term.
Strengths and limitations
Although there are many studies on the impact of the environment on health, with a growing number promoting access to nature and green spaces, these are focused mainly on general well-being rather than direct management of significant mental illness. They also focus on one type of environmental change instead of the full range available. Our study is unusual in three respects; (a) examining all types of environmental change, (b) having simultaneous records of changes in environment and clinical status, and (c) following the trajectories of patients for 30 years. There is one distant comparison. In a systematic review of health promotion in schools, the effects of interventions focused on environmental change, nutrition, exercise, safety, substance use and family life were compared. Those promoting mental health rather than trying to prevent ill-health, and those focusing on environmental change were the most effective [55]. This accords with our findings but the studies are not strictly comparable.
There are several important limitations to this study. The systematic examination of types of environmental change, particularly the separation of instrumental and imposed change, was not part of the original study and necessarily much of the data have been obtained retrospectively. It could therefore be influenced by bias, but we have tried to keep this to a minimum by allowing patients to drive the separation of positive from negative changes from their own reports and not by inference. By taking a longer time frame, interventions that might first be perceived as negative or neutral may be understood to be positive in the long-term, and vice-versa. This is the main advantage of a longer follow-up period.
Role of therapeutic intervention in positive instrumental change
Positive instrumental environmental change can be assisted by health practitioners in many ways. At its simplest level simple advice may be sufficient, such as explaining the advantages of giving up smoking or reducing hazardous drinking. At the other extreme someone with social disadvantage with very limited resources has very few options available and successful ones have to be worked for assiduously. Some of the interventions which led to environmental change in the Nottingham study were clearly therapist engendered. Although the benefits of these were too small to be significant they do suggest that if formal environmental interventions such as nidotherapy had been given during the course of the 30 years greater improvement might have been possible. Often the benefits of nidotherapy are delayed [56] and so it is preferable to use a long time course in their evaluation.
In this study there was no attempt to manipulate the environment deliberately to improve significant mental illness. It is becoming clear that this type of intervention could be of great value but at present has not been well studied. The two most common forms of environmental intervention are social prescribing and nidotherapy. In social prescribing patients can be referred to a link worker with knowledge of environmental options in the immediate locality. Such interventions may often be of value to the patient but research is this area has not yielded strong results because of barriers to implementation and concern over training needs [57,58,59] and one recent meta-analysis suggested it was both clinically ineffective and cost-ineffective [60]. Nidotherapy overlaps with social prescribing but is more complex [61], and has been shown to be of promise in several studies, including two randomised trials [56, 62,63,64] and also to improve social function in severe mental illness [65] but more larger scale studies are needed. The development of instrumental interventions more generally needs attention and will assist in this work. As personality function is likely to be closely linked to environmental change the measurement of personality status is also important in these enquiries [66, 67]. More attention needs to be paid to the potential cost-savings of such interventions, as they are generally cheap and when they offer equivalent outcome to more expensive alternatives they are to be fostered [63, 68].
Conclusion
The finding that, despite sometimes continuous and varied treatments and repeated care appointments, the effects of positive environmental change were greater than standard management in terms of clinical outcome, must call for a re-evaluation of the therapeutic strategies for treating common mental illness, particularly in the presence of personality disorder [29]. Only a small proportion of the positive changes in our study were created by therapists in services, but those that did take place, including many that were spontaneous, led to even more improvement than those receiving formal psychiatric treatment. There are, therefore, good reasons to believe that if the focus of management shifted from personal intervention for symptoms to an evaluation of environmental needs and their interaction [61], and consequent attention to those needs, the aim of fuller recovery can be achieved. This will not be easy, as chronic environmental deprivation is itself resistant to improvement but in treatments such as nidotherapy there is growing evidence that change engineered by a different attitude both to care and in society can yield long-term gains [62, 69]. But such changes have to made after careful planning, and other linked approaches such as social prescribing need to have a more rigorous structure linked to systematic assessment if they are to succeed.
Data availability
Data supporting the study findings are available from the corresponding author and Professor Yang upon reasonable request.
References
Kessler RC (1997) The effects of stressful life events on depression. Ann Rev Psychol 48:191–214. https://doi.org/10.1146/annurev.psych.48.1.191
Kessler RC, McLaughlin KA, Gree JG, Gruber MJ, Sampson NA, Zaslavsky AM et al (2010) Childhood adversities and adult psychopathology in the WHO World Mental Surveys. Br J Psychiatry 197:378–385. https://doi.org/10.1192/bjp.bp.110.080499
Hughes K, Bellis MA, Hardcastle KA, Sethi D, Butchart A, Mikton C et al (2017) The effect of multiple adverse childhood experiences on health: a systematic review and meta-analysis. Lancet Public Health 2:e356-366. https://doi.org/10.1016/S2468-2667(17)30118-4
Sonuga-Barke E, Kennedy M, Kumsta R, Knights N, Golm D, Rutter M et al (2017) Child-to- adult neurodevelopmental and mental health trajectories after early life deprivation: the young adult follow-up of the longitudinal English and Romanian Adoptees study. Lancet 389:1539–1548. https://doi.org/10.1016/S0140-6736(17)30045-4
Brown GW, Harris T (1978) Social origins of depression: a study of psychiatric disorders in women. Tavistock, London. https://doi.org/10.4324/9780203714911
Larsson S, Andreassen OA, Aas M, Rossberg JI, Mork E, Steen NE et al (2013) High prevalence of childhood trauma in patients with schizophrenia spectrum and affective disorder. Compr Psychiatry 54:123–127. https://doi.org/10.1016/j.comppsych.2012.06.009
Surtees PG, Ingham JG (1980) Life stress and depressive outcome: application of a dissipation model to life events. Soc Psychiatry 15:21–31
Surtees PG, Miller PM, Ingham JG, Kreitman NB, Rennie D, Sashidharan SP (1986) Life events and the onset of affective disorder: a longitudinal general population study. J Affect Disord 10:37–50. https://doi.org/10.1016/0165-0327(86)90047-9
Low NCP, Dugas E, O’Loughlin E, Rodriguez D, Contreras G, Chalton M, O’Loughlin J (2012) Common stressful life events and difficulties are associated with mental health symptoms and substance use in young adolescents. BMC Psychiatry. https://doi.org/10.1186/1471-244X-12-116
Lundin A, Forsell Y, Dalman C (2018) Mental health service use, depression, panic disorder and life events among Swedish young adults in 2000 and 2010: a repeated cross-sectional population study in Stockholm County, Sweden. Epidemiol Psychiatr Sci 27:510–518
Knight C, Patterson M, Dawson J (2017) Building work engagement: a systematic review and meta-analysis investigating the effectiveness of work engagement interventions. J Organ Behav 38:792–812
Janssen M, Heerkens Y, Kuijer W, van der Heijden B, Engels J (2018) Effects of mindfulness-based stress reduction on employees’ mental health: a systematic review. PLoS ONE 13:e0191332
Stigsdotter UK, Corazon SS, Sidenius U, Nyed PK, Larsen HB, Fjorback L (2018) Efficacy of nature-based therapy for individuals with stress-related illnesses: randomised controlled trial. Br J Psychiatry 213:404–411
Pijpker R, Veen EJ, Vaandrager L, Koelen M, Bauer GF (2022) Developing an intervention and evaluation model of outdoor therapy for employee burnout: unraveling the interplay between context, processes, and outcomes. Front Psychol. https://doi.org/10.3389/fpsyg.2022.785697
Gómez-Restrepo C, Casasbuenas NG, Ortiz-Hernández N, Bird VJ, Acosta MPJ, Restrepo JMU et al (2022) Role of the arts in the life and mental health of young people that participate in artistic organizations in Colombia: a qualitative study. BMC Psychiatry 22:757
Tyrer P, Seivewright N, Murphy S, Ferguson B, Kingdon D, Brothwell J et al (1988) The Nottingham study of neurotic disorder: comparison of drug and psychological treatments. Lancet 332:235–240
Tyrer P (1984) Psychiatric clinics in general practice - an extension of community care. Br J Psychiatry 145:9–14
Tyrer P, Ferguson B, Wadsworth J (1990) Liaison psychiatry in general practice: the comprehensive collaborative model. Acta Psychiat Scand 81:359–363
Williams P, Balestrieri M (1989) Psychiatric clinics in general practice: do they reduce admissions? Br J Psychiatry 154:67–71
Tyrer P, Seivewright N, Ferguson B, Murphy S, Johnson AL (1993) The Nottingham study of neurotic disorder: impact of personality status on response to drug treatment, cognitive therapy and self-help over two years. Br J Psychiatry 162:219–226
Spitzer R, Williams JB (1983) Structured clinical interview for DSM-III (1983 version). New York State Psychiatric Institute, New York
Seivewright H, Tyrer P, Johnson T (1998) Prediction of outcome in neurotic disorder: a five year prospective study. Psychol Med 28:1149–1157
Tyrer P, Tyrer H, Johnson T, Yang M (2022) Thirty year outcome of anxiety and depressive disorders and personality status: comprehensive evaluation of mixed symptoms and the general neurotic syndrome in the follow-up of a randomised controlled trial. Psychol Med 52:3999–4008
Coulton S, Clift S, Skingley A, Rodriguez J (2015) Effectiveness and cost-effectiveness of community singing on mental health-related quality of life of older people: randomised controlled trial. Br J Psychiatry 207:250–255
Montgomery SA, Åsberg M (1979) A new depression scale designed to be sensitive to change. Br J Psychiatry 134:382–389
Tyrer P, Owen RT, Cicchetti D (1984) The Brief Scale for Anxiety: a subdivision of the Comprehensive Psychopathological Rating Scale. J Neurol Neurosurg Psychiatry 47:970–975
Åsberg M, Montgomery SA, Perris C, Schalling D, Sedvall G (1978) A comprehensive psychopathological rating scale. Acta Psychiat Scand 57(Suppl 271):5–27
Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiat Scand 67:361–370
Tyrer P, Mulder R, Newton-Howes G, Duggan C (2022) Galenic syndromes: combinations of mental state and personality disorders too closely entwined to be separated. Br J Psychiatry 220:309–310
Tyrer P, Seivewright H, Johnson T (2004) The Nottingham Study of Neurotic Disorder: predictors of 12 year outcome of dysthymic, panic and generalised anxiety disorder. Psychol Med 34:1385–1394
Merson S, Tyrer P, Onyett S, Lynch S, Lack S, Johnson AL (1992) Early intervention in psychiatric emergencies: a controlled clinical trial. Lancet 339:1311–1314
Tyrer P, Nur U, Crawford M, Karlsen S, McLean C et al (2005) The Social Functioning Questionnaire: a rapid and robust measure of perceived functioning. Int J Soc Psychiatry 51:265–275
Tyrer P, Yang M, Tyrer H, Crawford M (2021) Is social function a good proxy measure of personality disorder? Pers Ment Health 15:261–272
Hanlon C, Medhin G, Alem A, Araya A, Abdullahi A, Tesfaye M et al (2008) Measuring common mental disorders in women in Ethiopia: reliability and construct validity of the comprehensive psychopathological rating scale. Soc Psychiatry Psychiatr Epidemiol 43:653–659
Yen S, Pagano ME, Shea MT, Grilo CM, Gunderson JG, Skodol AE et al (2005) Recent life events preceding suicide attempts in a personality disorder sample: findings from the collaborative longitudinal personality disorders study. J Consult Clin Psychol 73:99–105
Seivewright N, Tyrer P, Ferguson B, Murphy S, North B, Johnson T (2000) Longitudinal study of the influence of life events and personality status on diagnostic change in three neurotic disorders. Depress Anxiety 11:105–113
Tyrer P, Alexander J (1979) Classification of personality disorder. Br J Psychiatry 135:163–167
Tyrer P, Alexander MS, Cicchetti D, Cohen MS, Remington M (1979) Reliability of a schedule for rating personality disorders. Br J Psychiatry 135:168–174
Tyrer P (2022) Neurosis: understanding common mental disorders. Cambridge University Press, Cambridge
Mulder R (2021) ICD-11 Personality disorders: utility and implications of the new model. Front Psychiatry 12:655548
Tyrer P, Crawford M, Sanatinia R, Tyrer H, Cooper S, Muller-Pollard C et al (2014) Preliminary studies of the ICD 11 classification of personality disorder in practice. Pers Ment Health 8:254–263
Paykel ES, Prusoff BA, Uhlenhuth EH (1971) Scaling of life events. Arch Gen Psychiatry 25:340–347
Tennant C, Smith A, Bebbington P, Hurry J (1979) The contextual threat of life events: the concept and its reliability. Psychol Med 9:525–528
Goodyer I (1991) Life events, development and childhood psychopathology. Wiley, Chichester
Tyrer P (2002) Nidotherapy: a new approach to the treatment of personality disorder. Acta Psychiat Scand 105:469–471
Tyrer P, Sensky T, Mitchard S (2003) The principles of nidotherapy in the treatment of persistent mental and personality disorders. Psychother Psychosom 72:350–356
Carp FM (1985) Relevance of personality traits to adjustment in group living situations. J Gerontol 40:544–551
Tyrer P, Tyrer H, Yang M (2022) Relationships between treatments received in the Nottingham Study of Neurotic Disorder over 30 years and personality status. Pers Ment Health 16:99–110
Eysenck HJ (1952) The effects of psychotherapy: an evaluation. J Consult Clin Psychol 16:319–324
Yarringon JS, Metts JV, Craske M et al (2023) The role of positive and negative aspects of life events in depressive and anxiety symptoms. Clin Psychol Sci. https://doi.org/10.1177/21677026221141654
Blonski SC, Conradi HJ, Oldehinkel AJ, Bos EH, de Jonge P (2016) Associations between negative and positive life events and the course of depression: a detailed repeated-assessments study. J Nerv Ment Dis 204:175–180
Newton-Howes G, Tyrer P, Johnson T, Mulder R, Kool S, Dekker J et al (2014) Influence of personality on the outcome of treatment in depression: systematic review and meta-analysis. J Pers Disord 28:577–593
Knerer G, Byford S, Johnson T, Seivewright H, Tyrer P (2005) The Nottingham Study of Neurotic Disorder: predictors of 12 years costs. Acta Psychiat Scand 112:224–232
Yang M, Tyrer P, Tyrer H (2022) The recording of personality strengths: an analysis of the impact of positive personality features on the long-term outcome of common mental disorders. Pers Ment Health 16:120–129
Lister-Sharpe D, Chapman S, Stewart-Brown S, Sowden A (1999) Health promotion schools and health promotion in schools: two systematic reviews. Health Technol Ass 3(22):1–193
Tyrer P, Tarabi SA, Bassett P, Liedtka N, Hall R, Nagar J et al (2017) Nidotherapy compared with enhanced care programme approach training for adults with aggressive challenging behaviour and intellectual disability (NIDABID): cluster-randomised controlled trial. J Intellect Disabil Res 61:521–531
Auchterson H, Baxter L, Fancourt D (2020) Social prescribing for individuals with mental health problems: a qualitative study of barriers and enablers experienced by general practitioners. BMC Fam Pract 21:194
Bickerdike L, Booth A, Wilson PM et al (2017) Social prescribing: less rhetoric and more reality. A systematic review of the evidence. BMJ Open 7:e013384. https://doi.org/10.1136/bmjopen-2016-013384
Tyrer P, Boardman J (2020) Refining social prescribing in the UK. Lancet Psychiatry 7:831–832
Kiely B, Croker AO, Shea M, Boland FO, Shea E, Connolly D et al (2022) Effect of social prescribing link workers on health outcomes and costs for adults in primary care and community settings: a systematic review. BMJ Open 12:e062951. https://doi.org/10.1136/bmjopen-2022-062951
Tyrer P (2019) Nidotherapy: a cost-effective systematic environmental treatment. World J Psychiatry 18:144–145
Tyrer P, Bajaj P (2005) Nidotherapy: making the environment do the therapeutic work. BJPsychAdvances 11:232–238
Ranger M, Tyrer P, Milošeska K, Fourie H, Khaleel I, North B, Barrett B (2009) Cost-effectiveness of nidotherapy for comorbid personality disorder and severe mental illness: randomized controlled trial. Epidemiol Psychiatr Sci 18:128–136
Spears B, Tyrer H, Tyrer P (2017) Nidotherapy in the successful management of comorbid depressive and personality disorder. Pers Ment Health 11:344–350
Tyrer P, Miloseska K, Whittington C, Ranger M, Khaleel I, Crawford M et al (2011) Nidotherapy in the treatment of substance misuse, psychosis and personality disorder: secondary analysis of a controlled trial. BJPsychBull 35:9–14
Van Os J, Park B, Jones P (2001) Neuroticism, life events and mental health: evidence for person-environment correlation. Br J Psychiatry supplement 40:s72–s77
Jha M, Barrett B, Brewin C, Bowker G, Harwood N, Jalil I, Crawford M, Phull J, Allen K, Duggan C, Yang M, Tyrer P (2022) Matching ICD-11 personality status to clinical management in a community team—the Boston (UK) Personality Project: study protocol. Pers Ment Health 16:139–137
Ward Thompson C, Silveirinha de Oliveira E, Tilley S et al (2019) Health impacts of environmental and social interventions designed to increase deprived communities’ access to urban woodlands: a mixed-methods study. NIHR Journals Library, Southampton
Pearce J, Cherrie M, Shortt N, Deary I, Ward Thompson C (2018) Life course of place: a longitudinal study of mental health and place. Trans Inst Br Geogr 43:555–572. https://doi.org/10.1111/tran.12246
Acknowledgements
We thank the patients for their assistance in taking part in a long interview and the late Tony Johnson of the MRC Biostatistics Unit, Cambridge, who gave statistical help throughout the 30 year study for his valuable advice.
Funding
This follow-up study was supported by grants from the Mental Health Research Foundation (UK), Jessie Spencer Trust, Greater Manchester NHS Trust, Trent Regional Health Authority, MRC Co-operative Group for the Evaluation of Mental Health Interventions and Services (MENCOG), and the Nicola Pigott Memorial Fund. It was an NIHR Clinical Research Network (CRN) Portfolio Study.
Author information
Authors and Affiliations
Contributions
PT wrote the initial draft and CD, MY and HT added comments and changes MY analysed the data and created the Tables PT, CD and HT analysed the follow-up data and determined the nature of the environmental changes All authors agreed the final manuscript
Corresponding author
Ethics declarations
Conflict of interest
PT is the Chair of a registered charity, NIDUS-UK, that promotes the development of nidotherapy and the environmental interventions to improve mental illness.
Ethical standards
Ethical approval for this follow-up study was granted by the Northampton Research Ethics Committee (12/EM/0331).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tyrer, P., Duggan, C., Yang, M. et al. The effect of environmental change, planned and unplanned life events on the long-term outcome of common mental disorders. Soc Psychiatry Psychiatr Epidemiol 59, 1587–1598 (2024). https://doi.org/10.1007/s00127-023-02520-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-023-02520-1