Abstract
Purpose
Urban violence is a major problem in Brazil and may contribute to mental disorders among victims. The aim of this study was to assess the association between robbery victimisation and mental health disorders in late adolescence.
Methods
At age 18 years, 4106 participants in the 1993 Pelotas Birth Cohort Study were assessed. A questionnaire about history of robbery victimisation was administered, the Self-Report Questionnaire was used to screen for common mental disorders, and the Mini International Neuropsychiatric Interview was used to assess major depressive disorder and generalised anxiety disorder. Cross-sectional prevalence ratios between lifetime robbery victimisation and mental disorders were estimated using Poisson regression with robust standard errors, adjusting for socioeconomic variables measured at birth and violence in the home and maltreatment measured at age 15.
Results
There was a dose–response relationship between frequency of lifetime robberies and risk of mental disorders. Adolescents who had been robbed three or more times had twice the risk (PR 2.04; 95% CI 1.64–2.56) for common mental disorders, over four times the risk for depression (PR 4.59; 95% CI 2.60–8.12), and twice the risk for anxiety (PR 1.93; 95% CI 1.06–3.50), compared with non-victims, adjusting for covariates. Experiencing frequent robberies had greater impact on common mental disorders than experiencing an armed robbery. Population attributable fractions with regard to robbery were 9% for common mental disorders, 13% for depression, and 8% for anxiety.
Conclusions
Robberies are associated with common mental disorders in late adolescence, independently of violence between family members. Reducing urban violence could significantly help in preventing common mental illnesses.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In 1996, the World Health Organization declared that violence was a major and growing public health problem, accounting for more than 1 million deaths worldwide per year [1]. Violence is defined as the use of physical strength, power or any threat that can result in physical and psychological harm [2]. The highest rates of serious violence, as indicated by homicide rates, are found in sub-Saharan Africa and in Latin America and the Caribbean, where interpersonal violence was the leading cause of death among 15–49 year olds in 2013 [3]. As well as physical injuries, exposure to non-lethal violence has been linked to mental health problems and poorer quality of life, including impaired personal and professional relationships [4,5,6,7].
The mental health consequences of community violence, between individuals outside of the family context [8], has been less studied than other forms of violence, such as intimate partner violence [9] and child maltreatment [10, 11]; however, strong effects of community violence on posttraumatic stress disorder and externalising behaviour have been reported [12]. Most studies of community violence that have considered other mental heath outcomes have examined internalising problems in a broad fashion [7], with mixed results [12], and few have examined its effects while also considering violence experienced in the home [13]. Although one meta-analysis on the effects of community violence on internalising problems found a weak association [12], co-occurring violence in the home was not taken into account, which might have biased the results [13].
Brazil has experienced an enormous rise in serious urban violence over the past three decades [14]. According to a national victimisation survey in 2011/2012, 4% of adults had been victims of robbery in a 12-month period, 2% had been threatened with a gun or knife, and 1% had been victim of a sexual offence [14]. Late adolescence (ages 16–24) is when individuals are at highest risk for robbery or theft in Brazil [15]. In the city of Pelotas in Southern Brazil, where the current study was conducted, one-fifth of individuals born in 1993 had been officially registered as a victim of crime by age 18 years, with physical injury and robbery/blackmail being the most common types of victimisation [16]. The aim of the the current study was to assess the association between lifetime robbery victimisation and common mental disorders, depression and anxiety, among 18-year-old adolescents in the 1993 Pelotas Birth Cohort Study, in southern Brazil. Additionally, we examine the population attributable fraction associated with victimisation to consider the potential benefits for mental health if robberies could be reduced in this context.
Methods
We conducted cross-sectional analyses of data from the 1993 Pelotas Birth Cohort Study. Pelotas is a city in Southern Brazil with a population of 328,275 inhabitants and a Human Development Index of 0.739 [17]. In 1993, all hospital live births from the urban area of Pelotas (N = 5265) were eligible to participate in the birth cohort study. After 16 refusals, 5249 were included in the study. Follow-ups were conducted during childhood and adolescence. Details on the study’s methodology can be found elsewhere [18, 19].
This current study is based on data collected during the 18-year follow-up (N = 4106; 81.3% of the original cohort), which was carried out by a trained team of interviewers between September 2011 and April 2012. All participants in the cohort were invited to attend the clinic at the Postgraduate Program in Epidemiology, at the Federal University of Pelotas. This study was approved by the Research Ethics Committee of the Faculty of Medicine at the Federal University of Pelotas, and participants and/or parents/guardians received relevant information about the study and signed an informed consent form.
Measures
Information about robbery victimisation was obtained from the following questions in personal interviews: “Considering your entire life, have you ever been robbed?” “[If yes] How many times?” and “In this robbery (or any of these robberies), was a weapon used?” We examined both the frequency of robbery victimisation and the severity of victimisation (indicated by weapon use) as the main exposure variables for this study. In the original interviews in Portuguese, participants were asked about incidents of “assalto” which can be translated as “robbery” [20]; however, it is also possible some participants interpreted “assalto” more widely, and might have included assaults, or perhaps some non-violent thefts. Thus, not all events were necessarily robberies, although according to follow-up questions, most involved the use of a weapon.
The Brazilian version of the Self-Report Questionnaire (SRQ-20) was used to assess common mental disorders, which is a screening tool to investigate non-psychotic symptoms in the last month, especially depression and anxiety. The WHO suggests the SRQ-20 is suitable for studies with community samples in developing countries. The instrument includes four questions about physical symptoms and 16 questions about emotional symptoms, with dichotomous (yes or no) answers. Following a validation study in Brazil, male participants were classified as positive for common mental disorders if they answered positively to six or more questions (sensitivity 89% and specificity 81%), and women were classified positive for common mental disorders if they answered positively to eight or more questions (sensitivity 86% and specificity 77%) [21].
The Mini International Neuropsychiatric Interview instrument (MINI) was used to diagnose major depressive disorder and generalised anxiety disorder according to DSM-IV criteria [22], and has been validated previously for the Brazilian population [23]. It is a short standardized interview (15–30 min) designed to be used both for outcome-tracking in clinical practice and in epidemiological studies.
A priori, we included exposure to violence and maltreatment in the home as control variables. Violence and maltreatment in the home were measured in the age 15 follow-up of the cohort, based on five questions in a confidential questionnaire that were previously found to associate with depression at age 18 [24].
In addition, the following variables measured in the perinatal assessment were considered as possible additional confounding variables for inclusion in the final model: sex, maternal age at birth (complete years categorized as 13–19, 20–29, 30–39, and 40 or more), maternal education at birth (complete years of study, categorized as 0–8 and 9 or more), family income at birth (categorized in quintiles), mother living with a partner at birth (yes or no). Maternal common mental disorder (yes or no) measured in the 11-year follow-up was also considered as a possible confounding variable, as well as the adolescent’s skin colour (self-reported at age 15 years and subsequently categorized as white/black/brown/other).
Analyses
Statistical analyses were performed in STATA version 14.0. Bivariate analyses were used to examine the associations between sociodemographic characteristics, robbery victimisation, and mental health using the heterogeneity Chi square test and the Chi square test for linear trend in the case of ordinal variables. Possible confounding variables were identified as those associated (p < 0.20) with both the exposure and at least one outcome variable, and were included in the final multivariate analysis models. Poisson regression with robust standard errors was used to obtain adjusted effect estimates (including confounding factors) [25]. The p value for statistical significance was < 0.05 in the final model. The main analyses were focused on the number of robbery victimisations, but we also stratified additional analyses of the effects of robbery on common mental disorders according to whether or not a weapon had been used. There was no interaction between sex and robbery exposure in predicting the mental health outcomes (all p ≥ 0.05), which is why analyses were not stratified by sex. Population attributable fractions (PAF) were calculated using the following equation: \({\text{PAF}}=\frac{{p({\text{PR}} - 1)}}{{p({\text{PR}} - 1)+1}}\), where p is the proportion of the sample exposed to robbery, and PR is the fully adjusted prevalence ratio representing the increased risk of a mental health outcome caused by exposure to at least one robbery.
Results
At the 18-year-old follow up, 4106 adolescents participated in the study, corresponding to a follow-up rate of 81.3% (including in the denominator participants at age 18 and 164 deaths that had occurred mostly in early infancy). Among the 4106 interviewed participants, 50.9% were females, and the majority (64.2%) were white. At age 18 years, 27.4% of the participants reported they had been robbed at least once in their lifetime, and 18.5% reported having been victim of at least one armed robbery. In terms of frequency, 17.8% of youth had been robbed once, 6.2% twice and 3.4% reported three or more lifetime robberies. With respect to common mental disorders, 27.3% screened positive, and 4.0 and 7.5% of the adolescents presented with major depressive disorder and generalised anxiety disorder, respectively (Table 1).
The lifetime prevalence of robbery victimisation according to maternal and youth characteristics is shown in Table 2. Higher frequencies of robbery victimisation were reported by males, adolescents who self-reported white or other skin colour, participants with higher maternal education, and those in the higher quintiles of family income.
Examining mental health outcomes according to socioeconomic and demographic characteristics (Table 3), a higher prevalence of common mental disorders, depression and anxiety was found among female adolescents, those in poorer families, and among participants whose mothers had common mental disorders. Common mental disorders were also more common among adolescents with self-reported black/brown skin colour, and those whose mothers were younger, had lower education, and were not living with a partner. Adolescents who experienced more frequent robberies had particularly increased rates of common mental disorders, depression, and anxiety. Experiencing an armed robbery was associated with higher risk for common mental disorders than non-armed robbery.
The associations between robbery victimisation and mental health outcomes are shown in Table 4, both before and after adjusting for socioeconomic and demographic variables (sex, skin colour, maternal education, and family income at birth), violence in the home, and maltreatment (see the Methods section for how were selected). Even adjusting for confounders, a dose–response effect was found between the number of times participants were victims of robbery and their risk for mental health problems. For example, in adjusted analyses, the risk for common mental disorders was 19% higher among individuals who had been robbed once in their lifetime (compared to those who were never robbed), but this increased to 63% and 104% higher risk among those who had suffered two, and three or more robberies, respectively. Comparing participants who experienced three or more robberies to the no robbery group, diagnoses of depression and anxiety were 359% and 93% more likely, respectively. Comparing youth who had suffered armed robbery to the no robbery group, risk for common mental disorder, depressive disorder, and generalized anxiety disorder was 49% higher, 78% higher, and 48% higher, respectively.
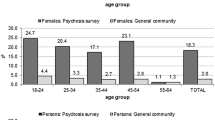
As one would expect, adolescents who had experienced more frequent robberies were also more likely to have experienced an armed robbery. Among youth who had experienced three or more robberies, 88% had experienced an armed robbery, compared to 74% among youth who had experienced two robberies and 61% among victims of a single robbery (χ2 = 43.15 (2); p < 0.001). To disentangle the effects on mental health of robbery frequency and robbery severity (weapon use), we examined the risk for common mental disorders associated with robbery frequency, stratifying by whether or not the youth had ever experienced armed robbery (in these stratified analyses with smaller numbers, only common mental disorders were analysed). Figure 1 shows adjusted prevalence ratios from these stratified analyses. The prevalence of common mental disorders increased with more frequent victimisations, even among youth who had never experienced an armed robbery; moreover, there was no evidence that this dose–response pattern was modified by the experience of an armed robbery. Hence, it appears that the frequency of robbery victimisation was more important in determining common mental disorders than whether or not adolescents had ever experienced an armed robbery, although confidence intervals are quite wide for these results.
Prevalence ratio (PR) for common mental disorder at 18 years according to number of robbery victimisations, stratified according to whether or not the person had ever experienced an armed robbery. * Adjusted for sex, skin colour, maternal education and family income at birth, and domestic violence/maltreatment up to age 15. CI confidence interval
Finally, we calculated the population attributable fraction of mental health outcomes associated with any lifetime robbery victimisation, using adjusted prevalence ratios. According to these calculations, if the adjusted prevalence ratios represent causal effects, reducing robberies in this population could, theoretically, prevent up to 9% of common mental disorders, 13% of major depressive disorders and 8% of generalized anxiety disorders.
Discussion
The key finding in this Brazilian population-based study was that multiple robbery victimisation was associated with increased risk for common mental health disorders, anxiety and depression, even adjusting for several possible confounding variables. We discuss findings about the sociodemographic characteristics of robbery victims, possible mechanisms accounting for the effects of robbery on mental disorder, and implications for policy and practice.
Three out of ten adolescents in the current study experienced robbery by age 18 years, reflecting the high prevalence of urban violence in Brazil [14, 26, 27]. Male, white, and richer adolescents had elevated rates of robbery victimisation, as in other Brazilian studies [15, 28, 29]. The fact that males were at greater risk of robbery than females is consistent with international studies showing that, although females suffer higher rates of domestic violence and sexual crimes, males are more involved in urban violence including robbery, assault, and homicide [7, 30]. Considering that white and richer adolescents were at elevated risk of robbery, racial and socioeconomic victimisation patterns clearly depend on the type of violence being examined, given that black people and people in more disadvantaged socioeconomic groups are at much higher risk of homicide in Brazil [31, 32]. In the United States, black people are also among the main victims of homicide, accounting for more than half of all cases [33].
In the current study, robbery victimization was associated with higher rates of common mental disorders, major depressive disorder, and generalized anxiety disorder, especially when adolescents had suffered multiple events of robbery victimisation. Recent robbery, assault or other physical aggression was also associated with common mental disorders among university employees in a study in Rio de Janeiro [34], and strong associations between assaultive violence and generalised anxiety disorder and major depression were found in another study in both Rio de Janeiro and São Paulo [35]. In São Paulo, a particularly large effect of exposure to multiple types of crimes was reported in a third survey [36]. Hence, the findings of the current study, specific to robbery, are consistent with other Brazilian studies that have examined exposure to additional forms of urban violence.
Armed robbery is likely to be particularly traumatic for victims. The presence of physical violence, and experiences of terror or hopelessness during a robbery, have been associated with post-traumatic stress disorder [37]. In the current study, armed robbery also carried greater risk for common mental disorders compared to non-armed robbery. However, considering all events to age 18, it appeared that frequency of robbery was even more important in determining common mental disorders than whether or not armed robbery had ever occurred, corresponding to a cumulative risk model of trauma and psychological distress [38,39,40].
It was notable that the effects of robbery on mental disorders in the current study persisted even after adjusting for indicators of child maltreatment and domestic violence, as well as sociodemographic variables measured early in life. In fact, adjusted associations were actually stronger than in unadjusted analyses—a form of negative confounding [41]. Negative confounding arose because sociodemographic factors, such as family income, were positively associated with robbery, but were inversely associated with mental health disorders. Few prior studies have examined the effects of community violence on mental health while accounting for the influence of violence in the home. In one British study, Cecil et al. [13] found that exposure to community violence did not predict internalising problems after adjusting for maltreatment. The difference in findings between this and our Brazilian study might reflect lower rates of community violence in Britain, given that only multiple events of robbery victimisation were associated with mental disorders in the current study, or different measures of mental health used between the studies; also, in Britain, community violence was measured as a composite variable referring to witnessing and hearing about violence, in addition to victimisation, which was the sole focus of our Brazilian study.
Theories about the effects of community violence on mental health have largely been based on the more consolidated body of research on the effects of maltreatment on children [7, 10]. Tolan [7] discusses three main theories linking community violence and mental disorders. Trauma theories suggest that the frightening nature of violent victimisation may give rise to overactive fear conditioning and stress on the hypothalamic–pituitary–adrenal system, leading to hypervigilance and related anxiety and depression; see also Moffitt [42] on the stress-biology of these effects. By contrast, attachment theories emphasise the disruption to social relationships that can be caused by violent victimisation, rather than effects on neurobiological systems. According to an attachment perspective, victimisation in the community may highlight the inability of carers to guarantee safety and a sense of belonging in the outside world, “which acts as a trauma to undercut relationship engagement, trust, and communication” [7]. In disadvantaged neighbourhoods, violence in the form of assault and homicide exposure might also cause psychopathology as part of “an overall ecology of exceptional stress and unpredictability” [7]; however, this seems less likely with respect to robbery victimisation in the current study, which was more common among socially advantaged groups. In contrast with these theories about victimisation causing mental disorder, reverse causality is also possible. For example, mental disorders could cause victimisation if mental illness leads to increased involvement in high-risk environments, or if it causes behaviour that elicits grievances in others [43,44,45]. Although eliciting grievances could occur in ongoing, interpersonal relationships, or in assaults between known parties, this seems less plausible with respect to robbery, normally a quick incident conducted by strangers in an urban environment.
By calculating population attributable fractions, we estimated that up to 9% of common mental disorders, 13% of major depressive disorders, and 8% of generalized anxiety disorders among adolescents could potentially be avoided by reducing robberies. This assumes that the observed associations are causal, i.e. that reverse causality did not occur and that there is no residual confounding. Although residual confounding would reduce these estimates, even small effects on depression and anxiety may have important practical implications, given the significance of these disorders for public health. Worldwide, mental and substance use disorders are the leading cause of years lived with disability [46], and depression and anxiety are the two most important contributors. Prevention of urban violence in Brazil is an enormous challenge for justice, health, and educational systems, and may not be achieved substantially for many years. The effects of robberies and other forms of violence on mental health need addressing in this context. Police who respond to violent victimisation in the community should be aware of possible effects on mental disorders, especially for people who have experienced multiple victimisations; police training should highlight the need to relay high-risk cases for evaluation by mental health professionals. In mental health treatment settings, clinicians should consider community violence victimisation as a possible source of common mental disorders such as depression and anxiety, and not only as a source of post-traumatic stress disorder, with which urban violence has been primarily associated. Hence, screening for a history of urban violence should be routine practice in high-violence social contexts such as Brazil.
Strengths and limitations
Our findings should be interpreted in view of the following limitations. We lacked more detailed information about the context, type and timing of the robberies reported on in this study. It would have been desirable to test whether robbery victimisation at different ages had different effects on mental disorders, but we were limited to data on lifetime robbery occurrence. For some participants, it is possible that victimisation referred to other types of crime, such as theft; however, among participants who answered positively about victimisation, two-thirds reported that a weapon was used, implying that a violent crime had definitely taken place. The self-reported lifetime robbery questions were also retrospective in nature, and although one would expect this type of traumatic event to be well remembered, prospective measures would have been preferable. Finally, we did not assess other forms of violent victimisation in the community, such as assault, or sexual offences, which might have confounded the association between robbery and the study outcomes, although the sociodemographic factors associated with robbery (male sex, higher socioeconomic position) are not likely to be positively associated with all these other types of urban violence.
Strengths of this study include the large sample and a low percentage of attrition and refusals by age 18 years. Also, there were only very small differences between individuals who had complete mental health and robbery data at age 18 compared to individuals without complete data (Online Supplementary Table). In addition, mental health outcomes were assessed with both screening and diagnostic instruments. Finally, given that this study was nested in a birth cohort, we were able to use prospectively measured variables to adjust for confounding factors from early in life.
Conclusions
The findings of the present study suggest that robbery victimisation contributes to common mental disorders, depression and anxiety in late adolescence, and more frequent robberies carry particular risk. Greater investment in preventive interventions that decrease urban violence may help reduce mental health problems among adolescents, which represent a major public health burden. Given the elevated prevalence of violent victimisation in low- and middle-income countries such as Brazil, practitioners working with victims and clinicians in mental health services need to be attentive to the consequences of urban violence for common mental disorders such as depression and generalised anxiety, in addition to post-traumatic stress disorder, which is often associated with such events.
References
World Health Organization (1996) Violence: a public health priority. Global Consultation on Violence and Health. World Health Organization, Geneva
Krug EG, Mercy JA, Dahlberg LL, Zwi AB (2002) The world report on violence and health. Lancet 360(9339):1083–1088
Global Burden of Disease 2013 Data (2016) Institute for Health Metrics and Evaluation. http://www.healthdata.org/gbd/data. Accessed Aug 2016
World Health Organization (2010) Mental Health and development: targeting people with mental health conditions as a vulnerable group. World Health Organization, Geneva
Gawryszewski VP, Rodrigues EM (2006) The burden of injury in Brazil. 2003. São Paulo Med J 124(4):208–213
Kessler RC, Aguilar-Gaxiola S, Alonso J, Chatterji S, Lee S, Ormel J, Ustun TB, Wang PS (2009) The global burden of mental disorders: an update from the WHO World Mental Health (WMH) surveys. Epidemiol Psichiatr Soc 18(1):23–33
Tolan PH (2016) Community violence exposure and developmental psychopathology. In: Cicchetti D (ed) Developmental psychopathology, vol 4, 3th edn. Wiley, Hoboken, pp 43–85. https://doi.org/10.1002/9781119125556.devpsy402
Foege WH, Rosenberg ML, Mercy JA (1995) Public health and violence prevention. Curr Issues Public Health 1:2–9
World Health Organization (2013) Global and regional estimates of violence against women: prevalence and health effects of intimate partner violence and non-partner sexual violence. World Health Organization, Geneva
Cicchetti D, Lynch M (1993) Toward an ecological/transactional model of community violence and child maltreatment: consequences for children’s development. Psychiatry 56(1):96–118
Norman RE, Byambaa M, De R, Butchart A, Scott J, Vos T (2012) The long-term health consequences of child physical abuse, emotional abuse, and neglect: a systematic review and meta-analysis. PLoS Med 9(11):e1001349
Fowler PJ, Tompsett CJ, Braciszewski JM, Jacques-Tiura AJ, Baltes BB (2009) Community violence: a meta-analysis on the effect of exposure and mental health outcomes of children and adolescents. Dev Psychopathol 21(01):227–259
Cecil CAM, Viding E, Barker ED, Guiney J, McCrory EJ (2014) Double disadvantage: the influence of childhood maltreatment and community violence exposure on adolescent mental health. J Child Psychol Psychiatry 55(7):839–848
Pesquisa Nacional de Vitimização [National Victimisation Survey]. Belo Horizonte, Brazil. (2013). http://www.crisp.ufmg.br/wp-content/uploads/2013/10/Sumario_SENASP_final.pdf. Accessed Aug 2016
Instituto Brasileiro de Geografia e Estatística (2010) Pesquisa Nacional por Amostra de Domicílios: Características da vitimização e do acesso à justiça no Brasil 2009 [Brazilian National Household Survey: Characteristics of victims and access to justice in Brazil 2009]. Instituto Brasileiro de Geografia e Estatística, Rio de Janeiro, Brazil
Gallo EAG, Menezes AMB, Murray J, Silva LAD da, Wehrmeister FC, Gonçalves H, Barros F (2016) Criminal victimization in childhood and adolescence according to official records: the Pelotas (Brazil) birth cohort study. Cad Saude Publica 32(8):e00072915
Atlas do Desenvolvimento Humano no Brasil. Pelotas, RS. http://www.atlasbrasil.org.br/2013/pt/perfil_m/pelotas_rs. Accessed May 2016
Victora CG, Araujo CL, Menezes AM, Hallal PC, Vieira Mde F, Neutzling MB, Goncalves H, Valle NC, Lima RC, Anselmi L, Behague D, Gigante DP, Barros FC (2006) Methodological aspects of the 1993 Pelotas (Brazil) Birth Cohort Study. Rev Saude Publica 40(1):39–46
Goncalves H, Assuncao MC, Wehrmeister FC, Oliveira IO, Barros FC, Victora CG, Hallal PC, Menezes AM (2014) Cohort profile update: the 1993 Pelotas (Brazil) birth cohort follow-up visits in adolescence. Int J Epidemiol 43(4):1082–1088
https://www.collinsdictionary.com/translator (2017). Accessed 1 Dec 2017
Mari JJ, Williams P (1986) A validity study of a psychiatric screening questionnaire (SRQ-20) in primary care in the city of Sao Paulo. Br J Psychiatry 148:23–26
Sheehan DV, Lecrubier Y, Sheehan KH, Amorim P, Janavs J, Weiller E, Hergueta T, Baker R, Dunbar GC (1998) The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry 59(Suppl 20):22–33
de Azevedo Marques JM, Zuardi AW (2008) Validity and applicability of the Mini International Neuropsychiatric Interview administered by family medicine residents in primary health care in Brazil. Gen Hosp Psychiatry 30(4):303–310
Gallo EAG, De Mola CL, Wehrmeister F, Gonçalves H, Kieling C, Murray J (2017) Childhood maltreatment preceding depressive disorder at age 18 years: a prospective Brazilian birth cohort study. J Affect Disord 217:218–224
Barros AJ, Hirakata VN (2003) Alternatives for logistic regression in cross-sectional studies: an empirical comparison of models that directly estimate the prevalence ratio. BMC Med Res Methodol 3:21
Waiselfisz JJ (2013) Mapa da Violência 2013: Homicídios e Juventude no Brasil [Map of Violence in 2013: Homicides and youth in Brazil]. Secretaria-Geral da Presidência da República e Secretaria Nacional de Juventude, Brasilia
Murray J, Cerqueira DRdC, Kahn T (2013) Crime and violence in Brazil: Systematic review of time trends, prevalence rates and risk factors. Aggress Violent Beh 18(5):471–483
Cruz SH, Azevedo MR, Gonçalves H (2011) Urban violence victimization in a medium size town in south Brazil. Rev Bras Epidemiol 14(1):15–26
Beato CF, Peixoto BT, Andrade MV (2004) Crime, opportunity, and victimization. Revista Brasileira de Ciências Sociais 19(55):73–89
Rand M (2009) National Victimization Survey, 2008 (BJS Bulletin). Bureau of Justice Statistics. U.S. Department of Justice, Washington, DC
Filho AMS, de Souza MFM, Gazal-Carvalho C, Malta DC, Alencar AP, da Silva MMA, Neto OLM (2007) Analysis of homicide mortality in Brazil. Epidemiol Serv Saúde 16(1):7–18
Waiselfisz JJ (2010) Mapa da violência 2010: Anatomia dos homícidios no Brasil [Map of violence 2010: Anatomy of homicides in Brazil]. Instituto Sangari, São Paulo
Black victms of violent crime: special report. Washington DC: U.S. Department of Justice (2007) http://bjs.ojp.usdoj.gov/content/pub/pdf/bvvc.pdf. Accessed Mar 2017
Lopes CS, Faerstein E, Chor D (2003) [Stressful life events and common mental disorders: results of the Pro-Saude Study]. Cad Saude Publica 19(6):1713–1720
Ribeiro WS, Mari JdJ, Quintana MI, Dewey ME, Evans-Lacko S, Vilete LMP, Figueira I, Bressan RA, de Mello MF, Prince M, Ferri CP, Coutinho ESF, Andreoli SB (2013) The impact of epidemic violence on the prevalence of psychiatric disorders in Sao Paulo and Rio de Janeiro, Brazil. PLoS One 8(5):e63545
Andrade LH, Wang YP, Andreoni S, Silveira CM, Alexandrino-Silva C, Siu ER, Nishimura R, Anthony JC, Gattaz WF, Kessler RC, Viana MC (2012) Mental disorders in megacities: findings from the São Paulo megacity mental health survey, Brazil. PLoS One 7(2):e31879
Fichera GP, Fattori A, Neri L, Musti M, Coggiola M, Costa G (2015) Post-traumatic stress disorder among bank employee victims of robbery. Occup Med 65(4):283–289
Williams SL, Williams DR, Stein DJ, Seedat S, Jackson PB, Moomal H (2007) Multiple traumatic events and psychological distress: the South Africa stress and health study. J Trauma Stress 20(5):845–855
Green BL, Goodman LA, Krupnick JL, Corcoran CB, Petty RM, Stockton P, Stern NM (2000) Outcomes of single versus multiple trauma exposure in a screening sample. J Trauma Stress 13(2):271–286
Suliman S, Mkabile SG, Fincham DS, Ahmed R, Stein DJ, Seedat S (2009) Cumulative effect of multiple trauma on symptoms of posttraumatic stress disorder, anxiety, and depression in adolescents. Compr Psychiatry 50(2):121–127
Mehio-Sibai A, Feinleib M, Sibai TA, Armenian HK (2005) A Positive or a negative confounding variable? A simple teaching aid for clinicians and students. Ann Epidemiol 15(6):421–423
Moffitt TE (2013) Childhood exposure to violence and lifelong health: clinical intervention science and stress-biology research join forces. Dev Psychopathol 25:1619–1634
Silver E, Arseneault L, Langley J, Caspi A, Moffitt TE (2005) Mental disorder and violent victimization in a total birth cohort. Am J Public Health 95(11):2015–2021
Silver E (2002) Mental disorder and violent victimization: the mediating role of involvement in conflicted social relationships. Criminology 40(1):191–212
Fazel S, Wolf A, Chang Z, Larsson H, Goodwin GM, Lichtenstein P (2015) Depression and violence: a Swedish Population Study. Lancet Psychiatry 2(3):224–232
Whiteford HA, Degenhardt L, Rehm J, Baxter AJ, Ferrari AJ, Erskine HE, Charlson FJ, Norman RE, Flaxman AD, Johns N, Burstein R, Murray CJL, Vos T (2013) Global burden of disease attributable to mental and substance use disorders: findings from the Global Burden of Disease Study 2010. Lancet 382(9904):1575–1586
Acknowledgements
This article is based on data from the 1993 Pelotas Birth Cohort Study conducted by Postgraduate Program in Epidemiology at Universidade Federal de Pelotas with the collaboration of the Brazilian Public Health Association (ABRASCO). From 2004 to 2013, the 1993 birth cohort was funded by Wellcome Trust through the program Major Awards for Latin America on Health Consequences of Population Change (Grant: 086974/Z08/Z). SF is funded by the Wellcome Trust. Previous phases of the study were funded by the European Union, Program of Support to Nuclei of Excellence (PRONEX), National Council of Scientific and Technological Development (CNPq) and the Brazilian Ministry of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The study protocol was approved by the Ethics and Research Committee of the Faculty of Medicine of the Federal University of Pelotas-RS under registration 05/11.
Informed consent
All research participants received the information pertinent to the study and signed an informed consent form.
Conflict of interest
The authors declare no conflicts of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Murray, J., Lima, N.P., Ruivo, A.C.O. et al. Lifelong robbery victimisation and mental disorders at age 18 years: Brazilian population-based study. Soc Psychiatry Psychiatr Epidemiol 53, 487–496 (2018). https://doi.org/10.1007/s00127-018-1488-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-018-1488-z