Abstract
Aims/hypothesis
We aimed to determine the longitudinal association of circulating markers of systemic inflammation with subsequent long-term cognitive change in older people with type 2 diabetes.
Methods
The Edinburgh Type 2 Diabetes Study is a prospective cohort study of 1066 adults aged 60 to 75 years with type 2 diabetes. Baseline data included C-reactive protein, IL-6, TNF-α fibrinogen and neuropsychological testing on major cognitive domains. Cognitive testing was repeated after 10 years in 581 participants. A general cognitive ability score was derived from the battery of seven individual cognitive tests using principal component analysis. Linear regression was used to determine longitudinal associations between baseline inflammatory markers and cognitive outcomes at follow-up, with baseline cognitive test results included as covariables to model cognitive change over time.
Results
Following adjustment for age, sex and baseline general cognitive ability, higher baseline fibrinogen and IL-6 were associated with greater decline in general cognitive ability (standardised βs = −0.059, p=0.032 and −0.064, p=0.018, respectively). These associations lost statistical significance after adjustment for baseline vascular and diabetes-related covariables. When assessing associations with individual cognitive tests, higher IL-6 was associated with greater decline in tests of executive function and abstract reasoning (standardised βs = 0.095, p=0.006 and −0.127, p=0.001, respectively). Similarly, raised fibrinogen and C-reactive protein levels were associated with greater decline in processing speed (standardised βs = −0.115, p=0.001 and −0.111, p=0.001, respectively). These associations remained statistically significant after adjustment for the diabetes- and vascular-related risk factors.
Conclusions/interpretation
Higher baseline levels of inflammatory markers, including plasma IL-6, fibrinogen and C-reactive protein, were associated with subsequent cognitive decline in older people with type 2 diabetes. At least some of this association appeared to be specific to certain cognitive domains and to be independent of vascular and diabetes-related risk factors.
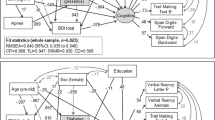
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.

Introduction
Diabetes mellitus, recognised as a major public health challenge [1], is ranked as the fourth leading cause of disability worldwide and is predicted to be the seventh leading cause of death in 2040 [2]. In addition to well-recognised cardiovascular and renal complications of diabetes, people with diabetes have around a 50% increased risk of developing dementia compared with the general population [3]. This includes both Alzheimer’s disease and vascular dementia (relative risks 1.46 and 2.48, respectively) [4]. Worldwide, 826,000 cases of Alzheimer’s disease are attributable to diabetes, resulting in a population attributable risk of 2.4% [5]. Diabetes is also associated with cognitive impairment that falls short of dementia [6], and with accelerated rates of age-related cognitive decline [7], resulting in earlier age of onset of clinically relevant cognitive impairment by 2.5 years [8].
Diabetes-related cognitive change is likely the result of multiple pathophysiological processes including vascular lesions, loss of white matter and general brain atrophy [8]; however, as yet, the underlying mechanism is poorly understood [9]. Rat models have shown that cerebral insulin levels may play a role in Alzheimer-like pathologies [10], while clinical studies have shown that people with diabetes-related dementia are more likely to have vascular dementia pathology [11]. A number of key vascular risk factors have been identified including impaired fasting glucose and insulin [12, 13], hypertension and macrovascular disease [14, 15]. It has also been hypothesised that systemic inflammation may have a role to play as people with diabetes have a proinflammatory state, with generally higher levels of circulating inflammatory mediators than are found in the general population [16]. Moreover, it has been found that low-grade inflammation predicts incident type 2 diabetes, with the inflammatory marker IL-6 driving this association [17].
In the general population, there is increasing evidence that inflammatory markers may predict cognitive change [18], and, in cross-sectional analyses, we showed previously that higher circulating levels of inflammatory mediators were associated with lower cognitive ability in older people with type 2 diabetes [19]. However, to date, little is known about the longitudinal association between systemic inflammation and diabetes-related cognitive change over time. In this 10 year follow-up study from the Edinburgh Type 2 Diabetes Study (ET2DS), we aimed to determine the longitudinal association of specific circulating markers of systemic inflammation measured at baseline with subsequent long-term cognitive change in older people with type 2 diabetes.
Methods
Study population
The ET2DS is a population-based prospective cohort study set up in 2006/2007 of 1066 men and women aged between 60 and 75 years at baseline with type 2 diabetes, living in Edinburgh and the Lothians. Details of recruitment have been published previously [20], but, in brief, participants were recruited at random, selected within sex and 5 year age bands from the Lothian Diabetes Register, a database with information on around 20,000 people diagnosed with diabetes according to WHO criteria. Inclusion criteria included being on oral glucose-lowering medications and/or insulin. If diabetes was managed through diet control alone, an HbA1c measure of >48 mmol/mol (6.5%) at the baseline clinic was required. Medical records were consulted if diabetes status of a potential participant was unclear.
The final study population of 1066 people has been shown previously to be largely representative of the target population of all older people with type 2 diabetes living in Lothian, Scotland, in terms of a range of sociodemographic and clinical characteristics [19]. The baseline population allows for 90% power at the two-sided 5% significance level to detect correlation of ≥0.1 of two continuous variables.
Participants were followed up for 10 years, including three intensive phases of data collection at years 1, 4 and 10 after recruitment. Other than those known to have died, all original participants were invited to re-attend the year 10 follow-up. Participants were invited to attend a research clinic, or, at year 10 follow-up, were visited at home by the research team if unable to attend a clinic. To further maximise attendance rates, participants were offered travel expenses to the clinic and a range of possible dates and times for clinics or home visits, and multiple attempts of contact were made by both post and telephone.
Ethical approval was granted from the Lothian Research Ethics Committee and NHS Lothian Research and Development Office. Written informed consent was obtained from all participants on attendance at each clinical and cognitive examination phase of the study.
Physical examination
Details of the physical and cognitive examination undertaken at baseline, including a fasting venous blood sample and a self-completion questionnaire on past medical history, together with record linkage to hospital discharge data, have been described previously [20]. Data collection took place at the Wellcome Trust Clinical Research Facility at the Western General Hospital, Edinburgh and record linkage was undertaken via the Information and Statistics Division of the National Health Service in Scotland. Baseline data were collected on age; sex; educational attainment levels; duration of diabetes; medications; smoking and alcohol history; past cardiovascular events and diabetic retinopathy; plasma HbA1c and glucose; serum total cholesterol, triacylglycerols and HDL-cholesterol; systolic and diastolic blood pressure; and BMI.
Measurement of inflammatory markers
At baseline, fasting blood samples were processed at the research clinic for immediate measurement of C-reactive protein (CRP), IL-6, TNF-α and fibrinogen. CRP was assayed using a high-sensitivity immunonephelometric assay (Dade Behring, UK) and TNF-α and IL-6 antigen levels were determined using high-sensitivity ELISA kits (R&D Systems, UK), performed in the University Department of Medicine, Glasgow Royal Infirmary. Participants with CRP level above 10 mg/l were removed from analyses, as this is indicative of acute inflammation likely as a result of a temporary infection and not chronic low-level inflammation.
Cognitive assessment
The same cognitive test battery of seven neuropsychological tests was undertaken at baseline and at 10 year follow-up. Verbal and non-verbal memory was measured using the Logical Memory (LM) and Faces subtests of the Wechsler Memory Scale, Third Edition (UK), respectively [21]. Executive function was tested using the Borkowski Verbal Fluency Test (BVFT) and the Trail Making Test B (TMTB). Processing speed, working memory and abstract (non-verbal) reasoning were assessed using the Digit Symbol Test (DST), Letter–Number Sequencing (LNS) and Matrix Reasoning (MR) subtests of the Wechsler Adult Intelligence Scale, Third Edition (UK), respectively [22]. This test battery was selected for the cohort at baseline to capture the major cognitive domains thought to be susceptible to decline in people with diabetes [20]. Following a test of sufficient visual acuity and a blood glucose level of above 4 mmol/l, the participants undertook the cognitive examination, which lasted no more than 1 h. The use of visual and/or hearing aids was encouraged, if required. The Hospital Anxiety and Depression Scale (HADS) [23] was used to measured self-reported symptoms of depression and anxiety on a scale of 0–21.
Statistical analysis
General cognitive function
In order to establish a measure of general cognitive ability for each participant, a principal component analysis (PCA) was performed using age-adjusted cognitive data from the seven cognitive tests at baseline (LM, Faces, TMTB, MR, DST, BVFT and LNS) using an extraction of Eigenvalues of >1.
Based on the approach of Gow et al [24], all cognitive data at both time points were stacked into seven columns and a single component of general cognitive ability was determined. Regression scores of the first component, termed general cognitive ability, ‘g’, were then saved according to time point, allowing baseline ‘g’ values to be centred on zero with an SD of 1 and follow-up ‘g’ values to be relative to baseline scores. Ten year cognitive change was represented by adjustment of year 10 scores for baseline scores. This method is now well established and is preferable to raw change scores as it is less dependent on individual differences in initial cognitive status [25].
PCA is only possible for cases with full cognitive data at baseline and at follow-up. In order to allow as many cases to be included in analyses as possible and to ensure sufficient power of analyses of variable ‘g’, multiple imputation was used for this variable [26]. To impute missing values a number of likely values based on the age, sex and other cognitive test results of the case were generated and a mean was taken. Data were assumed not to be missing at random, as some participants had a physical disability that prevented some cognitive tests being carried out, while others may not have been cognitively able to fully understand the instructions of the task. To ensure test scores were not artificially inflated as a result of imputation, imputations were only carried out on data where there were fewer than three out of seven cognitive tests missing. It should be noted that all other data described and analysed, other than the latent general cognitive function variable ‘g’, are on non-imputed data.
Analysis
Linear multivariable regression analyses were used to determine longitudinal associations between baseline risk factors and cognitive outcomes. A similar approach was used to determine the cross-sectional associations between year 10 risk factors and cognitive abilities. All models adopted a hierarchical approach, whereby blocks of diabetes-related (duration of diabetes, HbA1c and medication status) and cardiovascular risk factors (hypertension, smoking, HDL-cholesterol, serum triacylglycerols, alcohol units, and anxiety and depression scores) were sequentially added to the models to explore the association of each predictor risk factor and cognitive outcome. To determine the association of a risk factor with cognitive change over time, cognitive outcomes at year 10 were adjusted for baseline cognitive performance [24]. Additionally, categorisation of cognitive outcomes allowed for the calculation of ORs for ‘accelerated’ 10 year cognitive decline (lowest vs highest tertile of follow-up ‘g’ adjusted for baseline ‘g’) using logistic regression. All analyses were carried out in SPSS version 21 [27].
Results
The baseline characteristics of the ET2DS cohort and the characteristics of those who re-attended at the year 10 follow-up are described in Table 1. A total of 581 participants returned for cognitive testing after 10 years, which represented 77% of those participants still living (n = 756) at the time of invitation for repeat testing; 25% were tested at a home visit (see Fig. 1). The attrition rate over the full 10 years of the study was 45.5% (n = 485). The most common reason for non-attendance was death of participant (n = 310), accounting for 29.1% of the total baseline study population. The second highest reason given for non-attendance was comorbidities preventing attendance (n = 80), accounting for 7.5% of the total baseline study population (see Table 2). A comparison between baseline characteristics of attenders and non-attenders of the ET2DS at year 10 is presented in electronic supplementary material (ESM) Table 1.
Table 3 describes the baseline and follow-up cognitive test scores of the participants who attended the year 10 follow-up. Average performance on cognitive tests declined over the 10 years, including TMTB (where a higher score is indicative of a poorer performance). Mean ‘g’ at baseline for the ET2DS (N = 1066) was standardised to 0.00 ± 1.00. The population who re-attended at year 10 had a higher baseline general cognition score than the population as a whole had at baseline (0.34 ± 0.85); however, despite this, they showed a marked decline over the course of the study. In terms of effect size, ‘g’ declined by a considerable 0.44 SD (see Fig. 2). At year 10 follow-up, 52 participants scored <24 on the Mini Mental State Exam (MMSE).
The associations between the inflammatory markers and cognitive outcomes as measured by ‘g’ are presented in Table 4 (associations between inflammatory markers and the individual cognitive tests are described in ESM Table 2). Cognitive ability at follow-up was associated, after adjustment for age and sex, with a number of the inflammatory markers. The majority of statistically significant associations between inflammatory markers and either individual cognitive tests or ‘g’ were seen for IL-6, followed by fibrinogen and CRP. The strongest and most numerous associations with individual tests (with βs typically between 0.1 and 0.2) were with DST and TMTB, which assess processing speed, and also with MR, which assesses abstract reasoning. There were few associations with memory-based tests.
The association with cognitive change over time was assessed by adjusting for age, sex and baseline ‘g’. Higher fibrinogen (standardised β −0.059, p=0.032) and IL-6 (standardised β −0.064, p=0.018) were significantly associated with a decline in general cognitive ability. Higher CRP, fibrinogen and IL-6 were significantly associated with the individual cognitive tests, including TMTB (IL-6 standardised β 0.095, p=0.006), MR (IL-6 standardised β −0.127, p=0.001) and DST (CRP standardised β −0.111, p=0.001; fibrinogen standardised β −0.115, p=0.001).
In addition to the adjustments for age, sex and baseline cognition, further adjustment for a range of diabetes- and vascular-related risk factors reduced the strength and statistical significance of the findings. However, after adjustment for specific diabetes-related risk factors (duration of diabetes, HbA1c and medication status as a measure of disease severity), higher IL-6 was still significantly associated with a decline in cognitive ability as measured by DST (standardised β −0.076, p=0.02), MR (standardised β −0.119, p<0.001) and TMTB (standardised β 0.089, p=0.01). Similarly, higher fibrinogen was significantly associated with a decline in cognitive ability as measured by DST (standardised β −0.107, p=0.001) and TMTB (standardised β −0.082, p=0.02), and higher CRP and TNF-α were significantly associated with cognitive decline as measured by DST (standardised βs −0.099, p=0.03; and −0.073, p=0.02, respectively).
When cardiovascular risk factors, including hypertension, smoking, HDL-cholesterol, serum triacylglycerols, alcohol, and anxiety and depression scores, were further adjusted for, higher IL-6 remained associated with TMTB (standardised β −0.076, p=0.04) and MR (standardised β −0.111, p=0.001), and fibrinogen, CRP and TNF-α remained associated with DST (standardised βs −0.086, p=0.008; −0.087, p=0.009; −0.083, p=0.008, respectively). Associations with ‘g’ did not remain statistically significant (data presented in ESM Table 2).
The association between IL-6 and fibrinogen was modelled against 10 year cognitive change, as scoring in the lowest tertile of year 10 ‘g’ adjusted for baseline ‘g’. Cut points for follow-up ‘g’ adjusted for baseline ‘g’: lowest tertile, <−0.16; medium tertile, −0.15 to 0.33; highest tertile, >0.34.
In fully adjusted models for age, sex and all diabetes and cardiovascular risk factors, each increase in IL-6 per SD was associated with 64% increased odds of accelerated 10 year cognitive decline (OR 1.64, p = 0.006), and each increase per SD in fibrinogen was associated with 69% increased odds of accelerated 10 year cognitive decline (OR 1.69, p=0.001).
Discussion
In this 10 year follow-up of a representative cohort of older people with type 2 diabetes, higher baseline levels of systemic inflammatory markers, including plasma IL-6 and fibrinogen, predicted greater cognitive decline. This primary finding of our research involved association with a single test of generalised cognitive ability, derived from multiple individual cognitive tests that are specific to certain cognitive domains. We also found associations between individual cognitive tests and some of the inflammatory markers. In this respect, processing speed and executive function (measured using the TMTB and the DST), and abstract reasoning (measured using the MR), appeared to be particularly associated with altered inflammation. Our results also indicated that severity of diabetes and/or a range of vascular risk factors modified associations to a greater or lesser extent, depending on the inflammatory marker and the cognitive test. This suggests that inflammation may play a differential role across specific cognitive functions, but that at least some effects may be independent of conventional vascular risk factors known to contribute to cognitive dysfunction during ageing. Effect sizes overall were modest, though statistically significant, when the outcome was considered as a continuous outcome. However, we also showed that altered inflammatory marker levels were associated with a moderate increase in odds of being in a more severe tertile of cognitive decline, a potentially more clinically relevant and interpretable measure of age-related cognitive dysfunction.
Previously, in the baseline phase of the ET2DS, we showed associations between raised plasma inflammatory markers (including IL-6 and TNF-α) and lower cognitive ability [19]. Since this time, a number of studies have also found similar cross-sectional associations, mainly in the general population [28], but also in people with type 2 diabetes [18]. However, the important question of whether differences in inflammatory markers might precede the development of cognitive impairment, i.e. that inflammatory markers are associated with subsequent cognitive decline, has remained largely unanswered, especially for high-risk populations such as people with type 2 diabetes. Our current results are consistent with the hypothesis that raised levels of inflammation precede accelerated cognitive decline. This is also in line with emerging evidence presented from studies in the general population [28] and on frank dementia, where a recent systematic review has shown that increased levels of systemic inflammatory markers, namely IL-6, fibrinogen and CRP, increased the risk of developing all-cause dementia, though not with Alzheimer’s disease alone [29]. Our results build on previous work by first exploring cognitive change, as opposed to frank dementia, as this provides a more nuanced exploration of the association with inflammation, taking into account individual differences and more subtle changes in cognition. Second, we explore this association specifically in people with type 2 diabetes who are known to have an increased risk of developing both systemic inflammation and cognitive decline.
There are limitations to consider in our analyses. Over the 10 year follow-up period, there was an inevitable number of drop-outs from the ET2DS; however, the retention rate (55%) was in line with other studies [30] and relatively high when taking into account both participant age [31] and diabetes status [32]. Considerable effort, including the offer of transport or reimbursement of transport costs to and from the clinic, as well as the offer of a home visit, was made by the study team to ensure that as many of the surviving original cohort as possible were seen at year 10. It should also be recognised that any findings reported on associations between predictors and outcomes make no assumption on causality, despite the insights into temporality provided by the prospective study design and which suggest that reverse causation is unlikely to be a major explanation for our findings. We were unable to assess change in inflammatory marker levels over time in relation to the cognitive changes, and this would be relevant to consider in future studies. Fluctuations in levels of circulating inflammatory markers in individual cases may have occurred over time, including in response to lifestyle factors, illness and the use of medication. These latter factors themselves may also be linked both to baseline inflammatory marker levels and with a greater rate of cognitive change during the follow-up period, potentially helping to explain our findings. Despite these limitations, it should be noted that levels of inflammatory markers at baseline did predict subsequent cognitive change, and that this association was independent of a wide range of potentially confounding baseline biological risk factors. The ET2DS population at baseline exclusively consists of people with type 2 diabetes who have survived until the age of 65 years and so can be assumed to be a healthier subgroup of all people with type 2 diabetes. In addition, these analyses represent cognitive data from participants still living at follow-up. Survivor bias therefore plays a role within this research and should be taken into account as estimates will lie closer to the null, with a smaller effect size than likely observed in the true population.
In summary, we provide evidence for an association between increased levels of systemic inflammation as measured at baseline and subsequent 10 year cognitive decline in people with type 2 diabetes. IL-6 and fibrinogen were significantly associated with a decline in general cognition, although in fully adjusted models for a wide range of potential confounding and/or mediating factors, these associations were no longer statistically significant. Conversely, individual cognitive tests (TMTB, DST and MR) remained significantly associated with IL-6 and/or fibrinogen. Although these inflammatory markers are known to be highly correlated, it is possible that specific markers differ in their strength of association with cognitive decline, and also with decline within different domains of cognition. Furthermore, some of the associations may be mediated by vascular and diabetes-related risk factors. Any biological effect of inflammatory markers on cognition can only be surmised from the results of the current study, although the inflammatory marker IL-6 is known to cross the blood–brain barrier and so could have either a direct or indirect intracerebral effect on cognition [33]. Future studies in this area could usefully assess the amount of variance explained by inflammation and consider a wider range of individual and multiple covariables, change in covariables over time and inter-relations between covariables.
Our results go some way to addressing the previous paucity of evidence of a prospective association between markers of systemic inflammation and cognitive decline in people with type 2 diabetes. As this is primarily an exploratory observational study, clinical implications are limited and indirect. For example, while our results would be consistent with a true pathophysiological association, further investigation is required to determine whether associations are causal. If this can be proven, the possibility arises that efforts taken to reduce overall systemic inflammation may be beneficial in preventing the onset and severity of cognitive decline in people with type 2 diabetes. In addition, even if the findings do not translate into direct impact on therapeutic pathways, they could potentially help identify higher-risk groups within the diabetes population and so impact on clinical guidelines and decision making.
Data availability
The data that support the findings of this study are not publicly available due to them containing information that could compromise research participant privacy/consent. Aggregate data may be made available from the corresponding author upon reasonable request.
Abbreviations
- BVFT:
-
Borkowski Verbal Fluency Test
- CRP:
-
C-reactive protein
- DST:
-
Digit Symbol Test
- ET2DS:
-
Edinburgh Type 2 Diabetes Study
- HADS:
-
Hospital Anxiety and Depression Scale
- LM:
-
Logical Memory
- LNS:
-
Letter–Number Sequencing
- MMSE:
-
Mini Mental State Exam
- MR:
-
Matrix Reasoning
- PCA:
-
Principal component analysis
- TMTB:
-
Trail Making Test B
References
Zimmet PZ, Magliano DJ, Herman WH, Shaw JE (2014) Diabetes: a 21st century challenge. Lancet Diabetes Endocrinol 2(1):56–64. https://doi.org/10.1016/S2213-8587(13)70112-8
Institute for Health Metrics and Evaluation (IHME) (2018) Findings from the global burden of disease study 2017. IHME, Seattle, WA
Biessels GJ, Staekenborg S, Brunner E, Brayne C, Scheltens P (2006) Risk of dementia in diabetes mellitus: a systematic review. Lancet Neurol 5(1):64–74. https://doi.org/10.1016/S1474-4422(05)70284-2
Cheng G, Huang C, Deng H, Wang H (2012) Diabetes as a risk factor for dementia and mild cognitive impairment: a meta-analysis of longitudinal studies. Intern Med J 42(5):484. https://doi.org/10.1111/j.1445-5994.2012.02758.x
Barnes DE, Yaffe K (2011) The projected effect of risk factor reduction on Alzheimer’s disease prevalence. Lancet Neurol 10(9):819–828. https://doi.org/10.1016/S1474-4422(11)70072-2
van den Berg E, Kloppenborg RP, Kessels RPC, Kappelle LJ, Biessels GJ (2009) Type 2 diabetes mellitus, hypertension, dyslipidemia and obesity: a systematic comparison of their impact on cognition. Biochim Biophys Acta 1792(5):470–481. https://doi.org/10.1016/j.bbadis.2008.09.004
Yaffe K, Falvey C, Hamilton N et al (2012) Diabetes, glucose control, and 9-year cognitive decline among older adults without dementia. Arch Neurol 69(9):1170–1175. https://doi.org/10.1001/archneurol.2012.1117
Biessels GJ, Strachan MWJ, Visseren FLJ, Kappelle LJ, Whitmer RA (2014) Dementia and cognitive decline in type 2 diabetes and prediabetic stages: towards targeted interventions. Lancet Diabetes Endocrinol 2(3):246–255. https://doi.org/10.1016/S2213-8587(13)70088-3
Schneider JA, Arvanitakis Z, Bang W, Bennett DA (2007) Mixed brain pathologies account for most dementia cases in community-dwelling older persons. Neurology 69(24):2197–2204. https://doi.org/10.1212/01.wnl.0000271090.28148.24
Ho L, Qin W, Pompl PN et al (2004) Diet-induced insulin resistance promotes amyloidosis in a transgenic mouse model of Alzheimer’s disease. FASEB J 18(7):902–904. https://doi.org/10.1096/fj.03-0978fje
Ahtiluoto S, Polvikoski T, Peltonen M et al (2010) Diabetes, Alzheimer disease, and vascular dementia: a population-based neuropathologic study. Neurology 75(13):1195–1202. https://doi.org/10.1212/WNL.0b013e3181f4d7f8
Luchsinger JA (2008) Adiposity, hyperinsulinemia, diabetes and Alzheimer’s disease: an epidemiological perspective. Eur J Pharmacol 585(1):119–129. https://doi.org/10.1016/j.ejphar.2008.02.048
Cooper C, Sommerlad A, Lyketsos CG, Livingston G (2015) Modifiable predictors of dementia in mild cognitive impairment: a systematic review and meta-analysis. Am J Psychiatry 172(4):323–334. https://doi.org/10.1176/appi.ajp.2014.14070878
Xu WL, Qiu CX, Wahlin A, Winblad B, Fratiglioni L (2004) Diabetes mellitus and risk of dementia in the Kungsholmen project: a 6-year follow-up study. Neurology 63(7):1181–1186. https://doi.org/10.1212/01.wnl.0000140291.86406.d1
Cukierman-Yaffe T, Gerstein HC, Williamson JD et al (2009) Relationship between baseline glycemic control and cognitive function in individuals with type 2 diabetes and other cardiovascular risk factors: the action to control cardiovascular risk in diabetes-memory in diabetes (ACCORD-MIND) trial. Diabetes Care 32(2):221–226. https://doi.org/10.2337/dc08-1153
Devaraj S, Dasu MR, Jialal I (2010) Diabetes is a proinflammatory state: a translational perspective. Expert Rev Endocrinol Metab 5(1):19–28. https://doi.org/10.1586/eem.09.44
Duncan BB, Schmidt MI, Pankow JS et al (2003) Low-grade systemic inflammation and the development of type 2 diabetes: the atherosclerosis risk in communities study. Diabetes 52(7):1799–1805. https://doi.org/10.2337/diabetes.52.7.1799
Mittal K, Katare DP (2016) Shared links between type 2 diabetes mellitus and Alzheimer’s disease: a review. Diabetes Metab Syndr 10(2 Suppl 1):S144–S149. https://doi.org/10.1016/j.dsx.2016.01.021
Marioni RE, Strachan MWJ, Reynolds RM et al (2010) Association between raised inflammatory markers and cognitive decline in elderly people with type 2 diabetes the Edinburgh type 2 diabetes study. Diabetes 59(3):710–713. https://doi.org/10.2337/db09-1163
Price JF, Reynolds RM, Mitchell RJ et al (2008) The Edinburgh type 2 diabetes study: study protocol. BMC Endocr Disord 8:18. https://doi.org/10.1186/1472-6823-8-18
Wechsler D (1987) Manual for the Wechsler memory scale-revised. Psychological Corporation, San Antonio, TX
Wechsler D (1997) Wechsler adult intelligence scale—3rd edition (WAIS-3) Harcourt Assessment, San Antonio, TX
Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiatr Scand 67(6):361–370. https://doi.org/10.1111/j.1600-0447.1983.tb09716.x
Gow AJ, Johnson W, Pattie A, Whiteman MC, Starr J, Deary IJ (2008) Mental ability in childhood and cognitive aging. Gerontology 54(3):177–186. https://doi.org/10.1159/000118098
Willett JB (1997) Measuring change: what individual growth modeling buys you. In: Amsel E, Renninger KA (eds) Change and development: issues of theory, method, and application. Lawrence Erlbaum Associates Publishers, pp 213–243
van Beijsterveldt CEM, van Boxtel MPJ, Bosma H, Houx PJ, Buntinx F, Jolles J (2002) Predictors of attrition in a longitudinal cognitive aging study: the Maastricht aging study (MAAS). J Clin Epidemiol 55(3):216–223. https://doi.org/10.1016/S0895-4356(01)00473-5
IBM Corp. Released (2012) IBM SPSS statistics for windows, version 21.0. IBM Corp, Armonk, NY
Singh-Manoux A, Dugravot A, Brunner E et al (2014) Interleukin-6 and C-reactive protein as predictors of cognitive decline in late midlife. Neurology 83(6):486–493. https://doi.org/10.1212/WNL.0000000000000665
Darweesh SKL, Wolters FJ, Ikram MA, de Wolf F, Bos D, Hofman A (2018) Inflammatory markers and the risk of dementia and Alzheimer’s disease: a meta-analysis. Alzheimers Dement 14(11):1450–1459. https://doi.org/10.1016/j.jalz.2018.02.014
Okely JA, Deary IJ (2019) Longitudinal associations between loneliness and cognitive ability in the Lothian birth cohort 1936. J Gerontol Ser B Psychol Sci Soc Sci 74(8):1376–1386. https://doi.org/10.1093/geronb/gby086
Tilvis RS, Kähönen-Väre MH, Jolkkonen J, Valvanne J, Pitkala KH, Strandberg TE (2004) Predictors of cognitive decline and mortality of aged people over a 10-year period. J Gerontol A Biol Sci Med Sci 59(3):268–274. https://doi.org/10.1093/gerona/59.3.m268
Holman RR, Paul SK, Bethel MA, Matthews DR, Neil HAW (2008) 10-year follow-up of intensive glucose control in type 2 diabetes. N Engl J Med 359(15):1577–1589. https://doi.org/10.1056/NEJMoa0806470
Varatharaj A, Galea I (2017) The blood-brain barrier in systemic inflammation. Brain Behav Immun 60:1–12. https://doi.org/10.1016/j.bbi.2016.03.010
Acknowledgements
The authors thank all of the participants and staff involved in the Edinburgh Type 2 Diabetes Study.
Authors’ relationships and activities
Pfizer plc provided a portion of the funding for the ET2DS; however, they had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript. The authors declare that there are no other relationships or activities that might bias, or be perceived to bias, their work.
Funding
The Edinburgh Type 2 Diabetes Study is funded by the Medical Research Council, the Chief Scientist Office of the Scottish Executive and Pfizer plc. The study funders were not involved in the design of the study; the collection, analysis and interpretation of data; writing the report; and did not impose any restrictions regarding the publication of the report.
Author information
Authors and Affiliations
Contributions
AJS contributed to the study design phase, and performed the acquisition of data, data analysis and interpretation of data. AJS also drafted the article. SM and RBF contributed to acquisition of data and interpretation of data and revised the article critically for important intellectual content. JFP, IJD and MWJS conceived and designed the ET2DS and contributed to the analysis and interpretation of data. JFP, IJD and MWJS also revised the article critically for important intellectual content. All authors read and revised the version of the article to be published and have provided final approval of the version to be published. JFP is the guarantor of this work.
Corresponding authors
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM
(PDF 189 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sluiman, A.J., McLachlan, S., Forster, R.B. et al. Higher baseline inflammatory marker levels predict greater cognitive decline in older people with type 2 diabetes: year 10 follow-up of the Edinburgh Type 2 Diabetes Study. Diabetologia 65, 467–476 (2022). https://doi.org/10.1007/s00125-021-05634-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-021-05634-w