Abstract
Aims/hypothesis
In a recent study using a standard additive genetic model, we identified a TBC1D4 loss-of-function variant with a large recessive impact on risk of type 2 diabetes in Greenlanders. The aim of the current study was to identify additional genetic variation underlying type 2 diabetes using a recessive genetic model, thereby increasing the power to detect variants with recessive effects.
Methods
We investigated three cohorts of Greenlanders (B99, n = 1401; IHIT, n = 3115; and BBH, n = 547), which were genotyped using Illumina MetaboChip. Of the 4674 genotyped individuals passing quality control, 4648 had phenotype data available, and type 2 diabetes association analyses were performed for 317 individuals with type 2 diabetes and 2631 participants with normal glucose tolerance. Statistical association analyses were performed using a linear mixed model.
Results
Using a recessive genetic model, we identified two novel loci associated with type 2 diabetes in Greenlanders, namely rs870992 in ITGA1 on chromosome 5 (OR 2.79, p = 1.8 × 10−8), and rs16993330 upstream of LARGE1 on chromosome 22 (OR 3.52, p = 1.3 × 10−7). The LARGE1 variant did not reach the conventional threshold for genome-wide significance (p < 5 × 10−8) but did withstand a study-wide Bonferroni-corrected significance threshold. Both variants were common in Greenlanders, with minor allele frequencies of 23% and 16%, respectively, and were estimated to have large recessive effects on risk of type 2 diabetes in Greenlanders, compared with additively inherited variants previously observed in European populations.
Conclusions/interpretation
We demonstrate the value of using a recessive genetic model in a historically small and isolated population to identify genetic risk variants. Our findings give new insights into the genetic architecture of type 2 diabetes, and further support the existence of high-effect genetic risk factors of potential clinical relevance, particularly in isolated populations.
Data availability
The Greenlandic MetaboChip-genotype data are available at European Genome-Phenome Archive (EGA; https://ega-archive.org/) under the accession EGAS00001002641.
Similar content being viewed by others
Avoid common mistakes on your manuscript.

Introduction
Numerous genome-wide association studies (GWAS) have been performed to identify genetic factors predisposing to type 2 diabetes. These studies, mainly performed in European and Asian populations, have identified around 120 genetic variants associated with risk of type 2 diabetes [1,2,3,4,5,6,7,8].
Until now, GWAS of type 2 diabetes and glycaemic traits have almost exclusively been performed using an additive genetic model [1,2,3,4,5]. This model, however, has limited statistical power to detect associations with variants displaying recessive effects [9, 10], unless the effect is very large. Recently, a GWAS of type 2 diabetes in up to 4040 individuals with type 2 diabetes and 116,246 participants without diabetes from the UK Biobank applied a dominance deviation model to identify non-additive association signals [11]. Although no novel signals were identified, the paper reported a recessive effect on risk of type 2 diabetes at the previously identified CDKAL1 locus [11], which is in concordance with the findings from the original discovery [12]. Importantly, given the effective sample size of around 15,300, this study lacked statistical power to exclude the possibility that additional alleles with recessive effects predispose to type 2 diabetes in European populations.
We previously demonstrated the existence of a high-impact type 2 diabetes risk allele with predominately recessive effect in the Greenlandic population, despite using an additive genetic model in the discovery analysis [13]. Notably, however, this TBC1D4 loss-of-function variant was discovered via analyses of a type 2 diabetes-related trait, 2 h plasma glucose, on which it had an extremely large effect, and not via analyses of type 2 diabetes. Indeed, the study in which that variant was discovered had very limited statistical power to detect variants with recessive effects on type 2 diabetes unless they were very frequent and had very large effects. Here, we aimed to identify additional variants with recessive effects on risk of type 2 diabetes in the Greenlandic population by applying a recessive genetic model to an increased number of Greenlandic samples with type 2 diabetes information.
Methods
Study populations
The Greenlandic study sample comprised individuals from two cohorts selected as part of a general population health survey of the Greenlandic population during the periods 1999–2001 (B99, n = 1401) and 2005–2010 (Inuit Health in Transition (IHIT), n = 3115) and from a cohort of Greenlanders living in Denmark on whom information was collected during 1998–1999 (BBH, n = 547) [14, 15]. There was an overlap of individuals (n = 295) between the IHIT and B99 cohorts, and these were assigned to B99. Of the 4674 genotyped individuals who passed quality control, 4648 had phenotype data available. The characteristics of the three cohorts are shown in electronic supplementary material (ESM) Table 1. All participants gave informed consent, and the study was approved by the Commission for Scientific Research in Greenland (project 2011-13, ref. no. 2011-056978; and project 2013-13, ref. no. 2013-090702), and conducted in accordance with the ethical standards of the Declaration of Helsinki, second revision.
Yup’ik samples for quantitative trait replication came from the Center for Alaska Native Health Research (CANHR), which performs studies related to genetic, behavioural, and nutritional risk factors for obesity and cardiometabolic diseases among Yup’ik people in a community-based setting [16]. Recruitment of Yup’ik families was initiated in 2003 and continues in 11 Southwest Alaska communities, where all residents are invited to participate, resulting in a convenience sample. The present study sample comprised 1059 non-pregnant Yup’ik individuals aged 14 years or above at the time of enrolment. All participants signed informed consent documents, and the study protocols were approved by the Institutional Review Boards of the University of Alaska and the National and Alaska Area Indian Health Service Institutional Review Boards, as well as the Yukon Kuskokwim Health Corporation Human Studies Committee.
Additional replication analyses were performed on up to 23,776 Danish samples from the Inter99 study (n = 4947) (CT00289237, ClinicalTrials.gov) [17], from Health2006–Health2010 studies (n = 4776) [18], from the Danish study of Functional Disorders (DanFunD; n = 6004) [19], from the Vejle Diabetes Biobank (n = 6266) [20], and from the Steno Diabetes Center Copenhagen (n = 1783). Characteristics of the cohorts have previously been published [6]. The studies were approved by the appropriate Regional Ethical Committees and were performed in accordance with the scientific principles of the Helsinki Declaration, second revision.
Measurements and assays
The Greenlandic participants underwent an OGTT in which blood samples were drawn after an overnight fast and after 2 h during a 75 g OGTT. Plasma glucose levels were analysed using a Hitachi 912 system (Roche Diagnostics, Indianapolis, IN, USA), serum insulin with an immunoassay excluding des-31,32 split products and intact proinsulin (AutoDELFIA; PerkinElmer, Waltham, MA, USA), and HbA1c by ion-exchange HPLC (G7 [Tosoh Bioscience, Tokyo, Japan] for IHIT samples; VARIANT [Bio-Rad, Hercules, CA, USA] for B99 samples). The thickness of visceral and subcutaneous adipose tissue was measured according to a validated protocol using a portable ultrasound scanner (Pie Medical, Maastricht, the Netherlands) with a 3.5 MHz transducer [21]. Serum cholesterol, HDL-cholesterol and triacylglycerol concentrations were measured using enzymatic calorimetric techniques (Hitachi 917, Roche Molecular Biochemicals, Indianapolis, IN, USA). LDL-cholesterol concentration was calculated according to Friedewald’s formula. Insulin resistance was estimated by either: (1) HOMA-IR [22], calculated as [fasting glucose level (mmol/l) × fasting insulin (pmol/l)/6.945]/22.5; or (2) the insulin sensitivity index, ISI(0,120) [23], calculated as [(75,000 + [fasting glucose (mmol/l) × (18 − 2 h glucose [mmol/l]) × 18] × 0.19 × weight [kg])/120] / ([fasting glucose (mmol/l) + 2 h glucose (mmol/l)]/2) / log([fasting insulin (pmol/l)/6.945] + [2 h insulin (pmol/l)/6.945]/2), where log is the natural logarithm.
In the CANHR Yup’ik study population, blood samples were collected after an overnight fast. Insulin was measured with a radioimmunoassay applying an 125I-iodinated insulin tracer, anti-human insulin-specific antibody and human insulin standards from Linco Research (Winchester, VA, USA). The Poly-Chem System Chemistry Analyzer (Polymedco, Courtlandt Manor, NY, USA) was applied to measure HDL-cholesterol, total cholesterol and triacylglycerols. Fasting blood glucose was measured on a Cholestech LDX analyser (Cholestech, Hayward, CA, USA), and glycosylated haemoglobin was measured on a Bayer HbA1c DCA 2000+ analyser (Bayer, Leverkusen, Germany).
In the Danish samples, plasma glucose was measured by the glucose oxidase method (Granutest; Merck, Darmstadt, Germany).
In the Greenlandic and Danish cohorts, type 2 diabetes was defined based on self-reported type 2 diabetes, fasting plasma glucose level >7 mmol/l, or 2 h plasma glucose during an OGTT >11.1 mmol/l. Control individuals were normal glucose tolerant with a fasting plasma glucose <6.1 mmol/l and 2 h plasma glucose during an OGTT <7.8 mmol/l.
Genotyping
The Greenlandic samples were genotyped using Illumina MetaboChip (Illumina, San Diego, CA, USA), which contains 196,725 SNPs potentially related to metabolic, cardiovascular or anthropometric traits [24]. Details about the genotyping procedure and quality control have previously been described [25]. In total, 4674 individuals (IHIT, 2791; B99, 1336; BBH, 547) and 115,182 SNPs passed the quality control.
Detailed descriptions of the genotyping procedures and data cleaning of CANHR Yup’ik samples have also previously been published [26]. Briefly, we used the Illumina Linkage IV panel to genotype 6090 SNPs spanning the entire genome, with an average genetic distance of 0.58 cM. A total of 5632 autosomal SNPs from this Linkage IV panel passed the quality control. These SNPs were used to obtain ancestry information for the statistical analysis. Additionally, genotyping of SNPs for replication was performed by the KASPar Genotyping assay (LGC Genomics, Hoddesdon, UK).
The Danish samples were genotyped by the Illumina Infinium OmniExpress-24 v1.1 array. Genotypes were called by the Illumina GenCall algorithm, and variants with a call rate <98% and Hardy–Weinberg equilibrium p < 1 × 10−5 were removed. Samples were excluded if they were ethnic outliers, had a mismatch between genetic and phenotypic sex or had a call rate <95%. Genotype data were imputed using the Haplotype Reference Consortium (HRC) reference panel v1.1 [27] at the Michigan imputation server using MiniMac3 v2.0.1 (https://genome.sph.umich.edu/wiki/Minimac3) after phasing with Eagle2 v2.4 (https://data.broadinstitute.org/alkesgroup/Eagle/) [28]. Post-imputation filtering of SNPs excluded variants with a minor allele frequency (MAF) <0.01 and info score <0.70.
Statistical power simulations
To assess the statistical power of an additive and a recessive model-based test to detect association to a variant with recessive effect, we performed a range of simulations of data from a locus with a type 2 diabetes effect allele. For each of 540 combinations of effect allele frequencies (EAFs; EAF values 0.05, 0.1, 0.15, 0.2, 0.25 and 0.3) and effect sizes (ORs ranging from 1.1 to 10 with a step size of 0.1), we simulated first genotypes for n individuals and then their diabetes status based on these genotypes. For the simulation of type 2 diabetes status, we assumed a baseline risk of type 2 diabetes of 0.1, which we used to randomly simulate diabetes status for all individuals who were not homozygous carriers of the effect allele. For homozygous carriers of the effect allele, we simulated the diabetes status while taking both the baseline risk and the effect size into account. For each combination of EAF and OR, we performed 20,000 simulations, and finally, to estimate the power for the additive and the recessive model-based tests, we tested for association using logistic regression assuming each of these models, and estimated power as the proportion of tests that gave a p value <4.3 × 10−7 (the Bonferroni-corrected significance threshold of this study; see below for details). We performed the power simulations for 2948 individuals to reflect the number of individuals with type 2 diabetes information available in this study.
Statistical association analysis
For analyses of association in the Greenlanders, we used a linear mixed model, implemented in GEMMA software v0.96 (http://www.xzlab.org/) [29]. This model controls for admixture and relatedness between individuals as random effects via a genetic similarity matrix, which we estimated using GEMMA. This control is needed because the Greenlandic population is admixed with ancestry from both Inuit and Europeans [30]. With this model, we achieved an acceptable genomic inflation factor (λ = 1.009; ESM Fig. 1). In the discovery analyses, we used a recessive genetic model and applied a study-wide significance threshold of p = 4.3 × 10−7 corresponding to a Bonferroni correction for analysing 115,182 SNPs. In all the association analyses, we analysed data combined from the three cohorts and included sex, age and cohort as covariates. Prior to performing the association tests, quantitative traits were quantile-transformed to a standard normal distribution within each sex and each cohort. Therefore, for quantitative traits, effect sizes are reported as β in SD units (95% CI) in the text, and additionally as trait units in tables, obtained from association analyses on raw trait values. Effect sizes for association with type 2 diabetes are reported as ORs in the text, and were obtained from logistic regression analyses adjusted for age, sex and ten principal components. We estimated the effect sizes for the Inuit and European ancestry components using logistic regression also adjusted for age, sex and ten principal components with asaMap (https://github.com/ANGSD/asaMap, accessed 1 August 2017) [31] based on the estimated admixture proportions.
The Yup’ik cohort was also analysed using GEMMA software [29]. Here, however, the genetic similarity matrix required for the association analysis was not estimated using GEMMA, as we did in our analyses of the Greenlanders, but was instead calculated using the genotype data from the linkage panel merged with the additional genotypes of the SNPs genotyped for this study.
In the Danish data, association analyses of type 2 diabetes were carried out by logistic regression adjusting for age, sex and the first ten principal components. These analyses were performed on imputed genotype data, taking genotype uncertainty into account, applying the expected count test in SNPTEST v2.5.2 (https://mathgen.stats.ox.ac.uk/genetics_software/snptest/snptest.html).
Allele frequency estimation
For the SNPs of interest, we estimated allele frequencies for each of the Inuit and European ancestry components of the Greenlandic population using a two-step approach. In step 1, we estimated ancestry proportions for the Greenlandic study individuals as well as 50 Danish individuals. To do this, we applied ADMIXTURE v1.3.0 (https://www.genetics.ucla.edu/software/admixture/) [32] to all the SNP data from these individuals, assuming two ancestral populations—Inuit and Europeans. In step 2, we estimated ancestral allele frequencies with CIs for each SNP separately using bootstrap with replacement. We used 1000 bootstrap samples of individuals and, based on each, we performed maximum likelihood estimation of the allele frequencies, using the likelihood from ADMIXTURE with the ancestry proportions fixed to the estimates obtained in step 1. The CIs were based on the quantiles of these bootstrap estimates.
In CANHR Yup’ik samples, allele frequencies for the SNPs of interest were estimated using the Mendel program v16 (https://www.genetics.ucla.edu/software/mendel) [33, 34].
Querying results from previous large GWAS of type 2 diabetes and metabolic traits
Additive genetic model GWAS results were queried online: type 2 diabetes results from the DIAGRAM Consortium (DIAbetes Genetics Replication And Meta-analysis; http://diagram-consortium.org) [8], glycaemic trait results from MAGIC (the Meta-Analyses of Glucose and Insulin-related traits; www.magicinvestigators.org) [35], anthropometric trait results from the GIANT Consortium (Genetic Investigation of Anthropometric Traits; http://portals.broadinstitute.org/collaboration/giant/index.php/GIANT_consortium) [36,37,38], and lipid results from GLGC (Global Lipids Genetics Consortium; http://lipidgenetics.org) [39].
Assessment of functional effects and expression quantitative trait loci
To investigate whether the associated variants were causal, RegulomeDB (http://www.regulomedb.org/, accessed 10 January 2018) and HaploReg v4.1 (http://archive.broadinstitute.org/mammals/haploreg/haploreg.php) were applied to assess possible co-localisation of the genetic variants with regulatory elements, such as transcription factor binding sites, promoter regions and regions of DNAase hypersensitivity. We also used data from the GTEx Consortium available online to investigate associations between genetic variants and RNA expression (www.gtexportal.org; accessed 27 January 2018). All 48 tissues with more than 70 samples were queried. Sample sizes ranged from 80 to 388. Results were only available for an additive genetic model.
Results
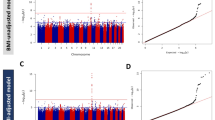
We analysed association with type 2 diabetes for 317 individuals with type 2 diabetes and 2631 participants with normal glucose tolerance. Using a recessive genetic model on these Greenlandic data, we identified three loci associated with type 2 diabetes below the study-wide Bonferroni-corrected significance threshold (p < 4.3 × 10−7) (ESM Fig. 1). Besides the previously described TBC1D4 locus [13], these comprised two novel loci, namely the common intron variant rs870992 in ITGA1 on chromosome 5 (MAF 23%, OR 2.79, p = 1.8 × 10−8) and the common intergenic variant rs16993330 approximately 25 kb upstream of LARGE1 on chromosome 22 (MAF 16%, OR 3.52, p = 1.3 × 10−7) (Fig. 1, Table 1). However, the LARGE1 variant did not reach the conventional threshold for genome-wide significance (p < 5 × 10−8). Similar associations with type 2 diabetes were observed when adjusting for BMI (data not shown).
Association results with type 2 diabetes for those SNPs on the MetaboChip that are located in a 2 Mb region around the lead SNPs: (a) rs870992 in ITGA1, and (b) rs16993330 near LARGE1. Each SNP in the region is represented by a circle whose colour indicates the extent of correlation (r2) between the SNP and the lead SNP, which is shown in red. The position of the circle along the x-axis shows the genomic position of the SNP. The position of the circle along the left y-axis shows the −log10 (p) value of the SNP when testing for association with type 2 diabetes as determined using a recessive model. The solid blue line illustrates the recombination rate from the Chinese HapMap Phase III panel (www.sanger.ac.uk/resources/downloads/human/hapmap3.html). The protein-coding genes in the genetic region are shown below the plot
The Greenlandic population is admixed with ancestry from both Inuit and Europeans [30]. Interestingly, the estimated EAF were considerably higher in the Inuit ancestry component for ITGA1 rs870992 (31%) and for LARGE1 rs16993330 (19%), than in the European ancestry component among Greenlanders (3% and 7%, respectively) and in European populations (Table 1, ESM Table 2). The allele frequencies found in Europeans were so low that homozygous carriers were almost absent. The novel variants in ITGA1 and LARGE1 had a high impact on risk of type 2 diabetes in Greenlanders, evident by the estimated effect sizes (Table 1) and by the higher frequency of type 2 diabetes among homozygous carriers compared with non-carriers (24.9% and 28.9% vs 10%; Fig. 2). To gain further insights into the effect of the identified loci, we also performed type 2 diabetes association analyses of these assuming an additive model (Table 1). This led to low p values as well, although none of them was low enough to pass the Bonferroni-corrected significance threshold (p < 4.3 × 10−7). Based on genetic data and functional annotation analyses facilitated by in silico tools, we were unable to determine whether the identified variants were causal.
Frequency of type 2 diabetes among Greenlanders stratified by the genotypes of (a) ITGA1 rs870992 and (b) LARGE1 rs16993330. The superimposed hatched areas represent effect sizes and the error bars represent SE. The effect sizes and SEs were estimated using a linear mixed model with no assumptions of inheritance mode. Frequencies were calculated in the subset of individuals included in the type 2 diabetes case–control study
Next, to elucidate the diabetes-related mechanisms underlying the association of the novel variants, we analysed diabetes-related traits in individuals without diabetes from the Greenlandic cohorts with a recessive genetic model. Homozygous carriers of ITGA1 rs870992 had nominally increased HbA1c levels (β = 0.13 SD [95% CI 0.027, 0.23], p = 0.012) (Table 2). For LARGE1 rs16993330, the underlying physiological mechanism seems to be linked to increased fat accumulation, indicated by higher levels of visceral adipose tissue (0.29 SD [95% CI 0.076, 0.50], p = 0.0078), larger hip circumference (0.22 SD [95% CI 0.048, 0.40], p = 0.013) and waist circumference (0.21 SD [95% CI 0.041, 0.38], p = 0.015) and higher BMI (0.18 SD [95% CI 0.0046, 0.35], p = 0.045) (Table 2). Furthermore, homozygous LARGE1 rs16993330 carriers had increased insulin resistance, indicated by higher levels of fasting serum insulin (0.22 SD [95% CI 0.027, 0.41], p = 0.026) and HOMA-IR (0.24 SD [95% CI 0.048, 0.44], p = 0.014), and lower levels of the ISI (−0.21 SD [95% CI −0.016, −0.41], p = 0.034) (Table 2). We then performed the analyses of the same quantitative diabetes-related traits with an additive model and obtained similar results (ESM Table 3).
We subsequently attempted to validate our findings in another Arctic indigenous population by genotyping the ITGA1 and LARGE1 variants in 1059 Alaska Native Yup’ik. However, none of the potential associations with diabetes-related quantitative traits were replicated in this smaller sample (ESM Table 4), and analysis of type 2 diabetes was precluded due to the low number of participants with diabetes. A second line of replication was attempted in a Danish sample of 5220 individuals with type 2 diabetes and 18,556 control participants. However, we did not observe an association with type 2 diabetes using a recessive model (ESM Table 2). In addition, the results of a dominance deviance model GWAS of European UK Biobank samples [11] showed no significant rejection of the additive model for either ITGA1 rs870992 or LARGE1 rs16993330 (p = 0.54 and p = 0.36, respectively) based on 117,775 individuals. We also queried the two variants from the available summary data from a recent additive genetic model GWAS of type 2 diabetes [8] and found that the ITGA1 rs870992 G allele was nominally associated with increased risk of type 2 diabetes, whereas no effect was observed for LARGE1 rs16993330 (ESM Table 5). Additionally, queries of results from GWAS of other traits revealed associations of the ITGA1 rs870992 G allele with increased total cholesterol and LDL-cholesterol levels, and nominal associations of the LARGE1 rs16993330 A allele with increased total cholesterol and triacylglycerol levels (ESM Table 5). Owing to the possible inflation of the test statistics, we also included the quantile of p values for the significant tests in ESM Table 5.
Finally, we queried RNA expression data available online as part of the GTEx project (www.gtexportal.org/) under the hypothesis that the newly identified variants in ITGA1 and LARGE1 could change the expression of regional genes. Here we observed that the type 2 diabetes-associated ITGA1 rs870992 G allele was associated with increased ITGA1 RNA expression in nerve, pancreas and smooth muscle tissue in up to 361 samples, albeit with modest p values (p < 0.0001). No expression quantitative trait loci (eQTL) associations were found for LARGE1 rs16993330.
Discussion
Using a recessive genetic model, we investigated the association between markers on MetaboChip and type 2 diabetes in a Greenlandic study population. Besides the established TBC1D4 locus [13], we identified a novel genome-wide significant variant for risk of type 2 diabetes in ITGA1, and a variant near LARGE1 showing a suggestive association. Additional analyses of diabetes-related quantitative traits indicated that the LARGE1 variant might increase the risk of type 2 diabetes through accumulation of visceral fat and increased insulin resistance, whereas these analyses provided no clues to the mechanistic link underlying the ITGA1 association. This study demonstrates the value of using the correct genetic model for identification of disease-associated variants, which is also supported by simulations showing that, for example, for a recessive effect allele with a frequency of 0.25 and an OR of 3 (similar to the ITGA1 variant), the power under an additive model is less than 20% whereas the power under a recessive model is around 80% (ESM Fig. 2). Moreover, under a wide range of EAF and ORs, the recessive model has markedly higher statistical power to detect variants with recessive effects associated with type 2 diabetes.
A possible link between the ITGA1 locus and altered glucose regulation is supported by studies of type 2 diabetes-related traits. Recently, rs6450057 mapping to PELO, a gene embedded in intron 1 of ITGA1, was found to be associated with fasting serum insulin levels in a transethnic GWAS meta-analysis of 70,000 individuals [40]. Interestingly, this study found an opposite direction of effect in European and African-American samples, indicating that rs6450057 is not the causal variant at this locus. Moreover, another ITGA1 intron variant, rs6867040, has been associated with fasting plasma glucose concentrations in 46,262 European individuals [41], and a recent prepublished GWAS of more than 800,000 samples showed an independent association between three variants at the ITGA1 locus and type 2 diabetes using an additive genetic model [42]. These studies support our findings of a link between variation in ITGA1 and type 2 diabetes. However, it is unclear whether it is the same signal, as the identified variants in the European study do not include rs870992, nor are the identified variants in high linkage disequilibrium with rs870992 in Europeans (r2 < 0.1).
Biologically, ITGA1 is an attractive candidate gene, encoding the α1-integrin subunit, which heterodimerises with the β1 subunit to form cell surface receptors that bind collagen and laminin. Interestingly, α1β1-integrin is the primary collagen receptor used by cultured beta cells, and this interaction regulates beta cell adhesion, motility and insulin secretion [43, 44]. Moreover, specific interactions between α1β1-integrin and extracellular matrix have been shown to be critical for beta cell survival and function [45], and therefore are possibly also important for glucose homeostasis and risk of type 2 diabetes. Besides the possible effects on beta cell function, ITGA1 seems to be linked to liver function. Thus, ITGA1 variants have been associated with plasma levels of the liver enzyme γ-glutamyl transferase [46], and modestly with ITGA1 protein expression levels in the liver [41]. In mice, knocking out Itga1 leads to severe hepatic insulin resistance [47] and altered fatty acid metabolism when they are fed a high-fat diet [48]. In line with this, we observed a borderline significant association between ITGA1 rs870992 and increased levels of fasting plasma glucose, which might indicate altered hepatic glucose regulation in the fasted state. Thus, studies of phenotypes reflecting liver function in Greenlanders would be of great interest to elucidate the biological mechanisms underlying the association between variation in ITGA1 and type 2 diabetes. In eQTL analyses, no effect of the type 2 diabetes-associated rs870992 variant on mRNA expression in liver tissue was observed. Instead, the variant was associated with increased ITGA1 expression in three other tissues; however, this was in the opposite direction to what was expected from the Itga1 knockout mice. This difference might rely on the fact that rs870992 is unlikely to be the causal variant and therefore we cannot conclude that the causal variant acts through RNA regulation even if our top SNP is significantly associated with ITGA1 expression.
No previous studies have indicated a link between LARGE1 and type 2 diabetes in additive model GWAS [8], nor did we replicate our findings in recessive analysis in a Danish sample of 5220 individuals with diabetes and 18,556 control participants. This lack of association in European samples may rely on low statistical power for recessive effects, due to the low frequency of risk alleles (EAF<10%) in Europeans (ESM Fig. 2) or due to population-specific differences in linkage disequilibrium between the identified variant and the causal variant. It is also possible that the causal variant behind the observed type 2 diabetes association is Inuit-specific, similar to the risk variant in TBC1D4 [13]. However, we were unable to pinpoint such a causal variant. Moreover, the lack of replication of the diabetes-related quantitative traits associations in a small sample of Alaska Native Yup’ik illustrates one of the main challenges with studies of isolated populations, namely the difficulty of finding appropriate replication cohorts in terms of both genetic composition and sample size. It is, however, also possible that the LARGE1 association represents a false-positive discovery.
LARGE1 encodes the LARGE xylosyl- and glucuronyltransferase 1 protein. This protein interacts with α-dystroglycan and functions as a glycosyltransferase stimulating glycosylation of α-dystroglycan, which in skeletal muscles connects the cytoplasm with the extracellular matrix as part of the dystrophin–glycoprotein complex [49, 50]. How this relates to the observed association with visceral fat accumulation and insulin resistance is unclear; therefore studies including a more comprehensive coverage of the genome and a larger sample size are warranted to verify the suggested associations, and possibly identify the causal variant in the locus.
In this study, we observed three loci, TBC1D4, ITGA1 and LARGE1, harbouring variants with large recessive effects on the risk of type 2 diabetes in Greenlanders, the latter, however, having weaker statistical support. In addition to these loci, based on a loss-of-function screening of the same population, we recently identified a variant in ADCY3 recessively associated with obesity and type 2 diabetes [51]. Variants in all four loci have effect sizes that are much greater than what has been reported for TCF7L2, which is the greatest genetic risk factor for type 2 diabetes among Europeans [1]. Even though the estimated effects are likely to be inflated by the ‘winner’s curse’, these variants have the potential to be of clinical relevance by facilitating the prediction of diabetes development in Greenlandic population. More research is needed to identify the causal variants, to elucidate the biological mechanisms underlying the association with type 2 diabetes, and to clarify whether these novel variants distinguish type 2 diabetes subtypes with specific aetiology, as demonstrated for TBC1D4 [13]. This additional knowledge could have the potential to guide choice of treatment for subtypes of type 2 diabetes.
In conclusion, we demonstrate that common alleles with recessive effects play a role in the genetic architecture of type 2 diabetes in the small and historically isolated Greenlandic population. These findings reiterate the importance of considering non-additive genetic models when performing GWAS.
Data availability
The Greenlandic MetaboChip-genotype data are available at European Genome-Phenome Archive (EGA; https://ega-archive.org/) under the accession EGAS00001002641.
Abbreviations
- CANHR:
-
Center for Alaska Native Health Research
- EAF:
-
Effect allele frequency
- eQTL:
-
Expression quantitative trait loci
- IHIT:
-
Inuit Health in Transition
- GWAS:
-
Genome-wide association study/studies
- ISI:
-
Insulin sensitivity index
- MAF:
-
Minor allele frequency
References
Morris AP, Voight BF, Teslovich TM et al (2012) Large-scale association analysis provides insights into the genetic architecture and pathophysiology of type 2 diabetes. Nat Genet 44:981–990
Mahajan A, Go MJ, Zhang W et al (2014) Genome-wide trans-ancestry meta-analysis provides insight into the genetic architecture of type 2 diabetes susceptibility. Nat Genet 46:234–244
Yamauchi T, Hara K, Maeda S et al (2010) A genome-wide association study in the Japanese population identifies susceptibility loci for type 2 diabetes at UBE2E2 and C2CD4A-C2CD4B. Nat Genet 42:864–868
Steinthorsdottir V, Thorleifsson G, Sulem P et al (2014) Identification of low-frequency and rare sequence variants associated with elevated or reduced risk of type 2 diabetes. Nat Genet 46:294–298
Grarup N, Sandholt CH, Hansen T, Pedersen O (2014) Genetic susceptibility to type 2 diabetes and obesity: from genome-wide association studies to rare variants and beyond. Diabetologia 57:1528–1541
Albrechtsen A, Grarup N, Li Y et al (2013) Exome sequencing-driven discovery of coding polymorphisms associated with common metabolic phenotypes. Diabetologia 56:298–310
Fuchsberger C, Flannick J, Teslovich TM et al (2016) The genetic architecture of type 2 diabetes. Nature 536:41–47
Scott RA, Scott LJ, Magi R et al (2017) An expanded genome-wide association study of type 2 diabetes in Europeans. Diabetes 66:2888–2902
Lettre G, Lange C, Hirschhorn JN (2007) Genetic model testing and statistical power in population-based association studies of quantitative traits. Genet Epidemiol 31:358–362
Hemminki K, Försti A, Bermejo JL (2010) Re: “Underlying Genetic Models of Inheritance in established type 2 diabetes loci”. Am J Epidemiol 171:1153–1154
Wood AR, Tyrrell J, Beaumont R et al (2016) Variants in the FTO and CDKAL1 loci have recessive effects on risk of obesity and type 2 diabetes, respectively. Diabetologia 59:1214–1221
Steinthorsdottir V, Thorleifsson G, Reynisdottir I et al (2007) A variant in CDKAL1 influences insulin response and risk of type 2 diabetes. Nat Genet 39:770–775
Moltke I, Grarup N, Jorgensen ME et al (2014) A common Greenlandic TBC1D4 variant confers muscle insulin resistance and type 2 diabetes. Nature 512:190–193
Bjerregaard P, Curtis T, Borch-Johnsen K et al (2003) Inuit health in Greenland: a population survey of life style and disease in Greenland and among Inuit living in Denmark. Int J Circumpolar Health 62(Suppl 1):3–79
Bjerregaard P (2011) Inuit health in transition – Greenland survey 2005-2010: population sample and survey methods, 2nd revised edition. Available from http://si-folkesundhed.dk/upload/inuit_health_in_transition_greenland_methods_5_2nd_revision.pdf. Accessed 10 Jan 2018
Mohatt GV, Plaetke R, Klejka J et al (2007) The Center for Alaska Native Health Research Study: a community-based participatory research study of obesity and chronic disease-related protective and risk factors. Int J Circumpolar Health 66:8–18
Jørgensen T, Borch-Johnsen K, Thomsen TF, Ibsen H, Glumer C, Pisinger C (2003) A randomized non-pharmacological intervention study for prevention of ischaemic heart disease: baseline results Inter99 (1). Eur J Cardiovasc Prev Rehabil 10:377–386
Thuesen BH, Cerqueira C, Aadahl M et al (2014) Cohort profile: the Health2006 cohort, Research Centre for Prevention and Health. Int J Epidemiol 43:568–575
Dantoft TM, Ebstrup JF, Linneberg A et al (2017) Cohort description: the Danish study of Functional Disorders. Clin Epidemiol 9:127–139
Petersen ER, Nielsen AA, Christensen H et al (2016) Vejle Diabetes Biobank - a resource for studies of the etiologies of diabetes and its comorbidities. Clin Epidemiol 8:393–413
Ronn PF, Andersen GS, Lauritzen T et al (2017) Ethnic differences in anthropometric measures and abdominal fat distribution: a cross-sectional pooled study in Inuit, Africans and Europeans. J Epidemiol Community Health 71:536–543
Matthews DR, Hosker JP, Rudenski AS et al (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419
Gutt M, Davis CL, Spitzer SB et al (2000) Validation of the insulin sensitivity index (ISI0,120): comparison with other measures. Diabetes Res Clin Pract 47:177–184
Voight BF, Kang HM, Ding J et al (2012) The metabochip, a custom genotyping array for genetic studies of metabolic, cardiovascular, and anthropometric traits. PLoS Genet 8:e1002793
Andersen MK, Jorsboe E, Sandholt CH et al (2016) Identification of novel genetic determinants of erythrocyte membrane fatty acid composition among Greenlanders. PLoS Genet 12:e1006119
Aslibekyan S, Vaughan LK, Wiener HW et al (2013) Evidence for novel genetic loci associated with metabolic traits in Yup'ik people. Am J Hum Biol 25:673–680
McCarthy S, Das S, Kretzschmar W et al (2016) A reference panel of 64,976 haplotypes for genotype imputation. Nat Genet 48:1279–1283
Das S, Forer L, Schonherr S et al (2016) Next-generation genotype imputation service and methods. Nat Genet 48:1284–1287
Zhou X, Stephens M (2012) Genome-wide efficient mixed-model analysis for association studies. Nat Genet 44:821–824
Moltke I, Fumagalli M, Korneliussen TS et al (2015) Uncovering the genetic history of the present-day Greenlandic population. Am J Hum Genet 96:54–69
Skotte L, Korneliussen TSS, Moltke I, Albrechtsen A (2015) Ancestry specific association mapping in admixed populations. bioRxiv 014001. https://doi.org/10.1101/014001
Alexander DH, Novembre J, Lange K (2009) Fast model-based estimation of ancestry in unrelated individuals. Genome Res 19:1655–1664
Lange K, Sinsheimer JS, Sobel E (2005) Association testing with Mendel. Genet Epidemiol 29:36–50
Lange K, Papp JC, Sinsheimer JS, Sripracha R, Zhou H, Sobel EM (2013) Mendel: the Swiss army knife of genetic analysis programs. Bioinformatics 29:1568–1570
Scott RA, Lagou V, Welch RP et al (2012) Large-scale association analyses identify new loci influencing glycemic traits and provide insight into the underlying biological pathways. Nat Genet 44:991–1005
Locke AE, Kahali B, Berndt SI et al (2015) Genetic studies of body mass index yield new insights for obesity biology. Nature 518:197–206
Shungin D, Winkler TW, Croteau-Chonka DC et al (2015) New genetic loci link adipose and insulin biology to body fat distribution. Nature 518:187–196
Wood AR, Esko T, Yang J et al (2014) Defining the role of common variation in the genomic and biological architecture of adult human height. Nat Genet 46:1173–1186
Willer CJ, Schmidt EM, Sengupta S et al (2013) Discovery and refinement of loci associated with lipid levels. Nat Genet 45:1274–1283
Liu CT, Raghavan S, Maruthur N et al (2016) Trans-ethnic meta-analysis and functional annotation illuminates the genetic architecture of fasting glucose and insulin. Am J Hum Genet 99:56–75
Billings LK, Hsu Y-H, Ackerman RJ et al (2012) Impact of common variation in bone-related genes on type 2 diabetes and related traits. Diabetes 61:2176–2186
Mahajan A, Taliun D, Thurner M et al. (2018) Fine-mapping of an expanded set of type 2 diabetes loci to single-variant resolution using high-density imputation and islet-specific epigenome maps. bioRxiv 245506. https://doi.org/10.1101/245506
Kaido T, Yebra M, Cirulli V, Montgomery AM (2004) Regulation of human beta-cell adhesion, motility, and insulin secretion by collagen IV and its receptor alpha1beta1. J Biol Chem 279:53762–53769
Kaido TJ, Yebra M, Kaneto H, Cirulli V, Hayek A, Montgomery AM (2010) Impact of integrin-matrix interaction and signaling on insulin gene expression and the mesenchymal transition of human beta-cells. J Cell Physiol 224:101–111
Krishnamurthy M, Li J, Al-Masri M, Wang R (2008) Expression and function of alphabeta1 integrins in pancretic beta (INS-1) cells. J Cell Commun Signal 2:67–79
Chambers JC, Zhang W, Sehmi J et al (2011) Genome-wide association study identifies loci influencing concentrations of liver enzymes in plasma. Nat Genet 43:1131–1138
Williams AS, Kang L, Zheng J et al (2015) Integrin α1-null mice exhibit improved fatty liver when fed a high fat diet despite severe hepatic insulin resistance. J Biol Chem 290:6546–6557
Kang L, Ayala JE, Lee-Young RS et al (2011) Diet-induced muscle insulin resistance is associated with extracellular matrix remodeling and interaction with integrin α2β1 in mice. Diabetes 60:416–426
Michele DE, Campbell KP (2003) Dystrophin-glycoprotein complex: post-translational processing and dystroglycan function. J Biol Chem 278:15457–15460
Barresi R, Michele DE, Kanagawa M et al (2004) LARGE can functionally bypass alpha-dystroglycan glycosylation defects in distinct congenital muscular dystrophies. Nat Med 10:696–703
Grarup N, Moltke I, Andersen MK et al (2018) Loss-of-function variants in ADCY3 increase risk of obesity and type 2 diabetes. Nat Genet 50:172–174
Acknowledgements
We gratefully acknowledge the participants in the Greenlandic health surveys. From Novo Nordisk Foundation Center for Basic Metabolic Research, University of Copenhagen, Denmark, we wish to thank A. Forman, T. H. Lorentzen and G. J. Klavsen for laboratory assistance, P. Sandbeck for data management, G. Lademann for secretarial support, and T. F. Toldsted for grant management.
Funding
The Novo Nordisk Foundation Center for Basic Metabolic Research is an independent Research Center at the University of Copenhagen partially funded by an unrestricted donation from the Novo Nordisk Foundation (www.metabol.ku.dk). This project was also funded by the Danish Council for Independent Research (DFF-4090-00244, Sapere Aude grant DFF-11-120909 and DFF-4181-00383), the Steno Diabetes Center Copenhagen (www.steno.dk), the Lundbeck Foundation (R215–2015-4174) and the Novo Nordisk Foundation (NNF15OC0017918, NNF16OC0019986 and NNF15CC0018486). The Greenlandic health surveys (IHIT and B99) were supported by Karen Elise Jensen’s Foundation, the Department of Health in Greenland, NunaFonden, Medical Research Council of Denmark, Medical Research Council of Greenland and Commission for Scientific Research in Greenland. The CANHR studies involving Alaska Native Yup’ik people were funded by the following National Institutes of Health grants: P30 GM103325, R01 DK104347 and R01 DK074842.
Author information
Authors and Affiliations
Contributions
TH and AA conceived and headed the project. IM and AA designed the statistical set-up, while TH, NG, MKA and OP designed the experimental set-up for the extraction, genotyping and sequencing of the DNA. MEJ and PB were principal investigators of the population studies in Greenland, and together with CVLL and IKD-P, they provided the Greenlandic samples, collected and defined the phenotypes and provided context of these samples. AL planned, recruited and acquired the Danish samples for replication. BBB and SEH led the initial study design for the Yup’ik studies and data collection. HKT and HWW led the statistical analyses for the Yup’ik studies. BB was the principal investigator of the population studies in Alaska and, together with SEH, provided the Yup’ik samples, collected and defined the phenotypes and provided the context of these samples. IM, NG, EJ, and AA performed the association analyses. NG, IM, MKA, AA and TH wrote the majority of the manuscript with input from all authors. All authors approved the final version of the manuscript. NG and TH are the guarantors of this work.
Corresponding authors
Ethics declarations
The authors declare that there is no duality of interest associated with this manuscript.
Electronic supplementary material
ESM
(PDF 510 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Grarup, N., Moltke, I., Andersen, M.K. et al. Identification of novel high-impact recessively inherited type 2 diabetes risk variants in the Greenlandic population. Diabetologia 61, 2005–2015 (2018). https://doi.org/10.1007/s00125-018-4659-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-018-4659-2