Abstract
Aims/hypothesis
Impaired awareness of hypoglycaemia (IAH) in type 1 diabetes increases the risk of severe hypoglycaemia sixfold and can be resistant to intervention. We explored the impact of IAH on central responses to hypoglycaemia to investigate the mechanisms underlying barriers to therapeutic intervention.
Methods
We conducted [15O]water positron emission tomography studies of regional brain perfusion during euglycaemia (target 5 mmol/l), hypoglycaemia (achieved level, 2.4 mmol/l) and recovery (target 5 mmol/l) in 17 men with type 1 diabetes: eight with IAH, and nine with intact hypoglycaemia awareness (HA).
Results
Hypoglycaemia with HA was associated with increased activation in brain regions including the thalamus, insula, globus pallidus (GP), anterior cingulate cortex (ACC), orbital cortex, dorsolateral frontal (DLF) cortex, angular gyrus and amygdala; deactivation occurred in the temporal and parahippocampal regions. IAH was associated with reduced catecholamine and symptom responses to hypoglycaemia vs HA (incremental AUC: autonomic scores, 26.2 ± 35.5 vs 422.7 ± 237.1; neuroglycopenic scores, 34.8 ± 88.8 vs 478.9 ± 311.1; both p < 0.002). There were subtle differences (p < 0.005, k ≥ 50 voxels) in brain activation at hypoglycaemia, including early differences in the right central operculum, bilateral medial orbital (MO) cortex, and left posterior DLF cortex, with additional differences in the ACC, right GP and post- and pre-central gyri in established hypoglycaemia, and lack of deactivation in temporal regions in established hypoglycaemia.
Conclusions/interpretation
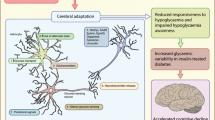
Differences in activation in the post- and pre-central gyri may be expected in people with reduced subjective responses to hypoglycaemia. Alterations in the activity of regions involved in the drive to eat (operculum), emotional salience (MO cortex), aversion (GP) and recall (temporal) suggest differences in the perceived importance and urgency of responses to hypoglycaemia in IAH compared with HA, which may be key to the persistence of the condition.
Similar content being viewed by others
Avoid common mistakes on your manuscript.

Introduction
For people with diabetes, the main defence against severe hypoglycaemia, in which blood glucose falls too low to sustain cognitive function [1], is subjective awareness of minor episodes. Impaired awareness of hypoglycaemia (IAH) is associated with delayed and diminished counterregulatory responses to hypoglycaemia [2]. It is reported in 25–40% of people with longstanding type 1 diabetes mellitus [3, 4], and 10% with insulin-treated type 2 diabetes [5], increasing risk of severe hypoglycaemia 6- and 17-fold respectively [3–5].
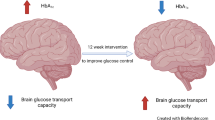
The brain triggers counterregulatory neuroendocrine responses to hypoglycaemia, symptom perception, and coordination of endogenous and behavioural protective responses. Animal studies [6] have hypothesised that IAH, which is inducible by exposure to plasma glucose below 3 mmol/l [7, 8], is associated with increased brain capacity for glucose uptake. However, early studies of enhanced global brain glucose uptake in humans [9] are not compatible with the clinical picture of IAH, where deterioration of cognitive function precedes the onset of diminished and asymptomatic counterregulatory responses [10]. Early neuroimaging studies failed to confirm a global increase in glucose uptake in IAH [11].
Functional neuroimaging investigates the brain’s response to a challenge by measuring regional changes in glucose uptake and metabolism or perfusion as markers of neuronal activation. Activation of the hypothalamus, important in glucose sensing, has been described with modest decrements of blood glucose (to 4.3 mmol/l) in healthy volunteers [12]. More extensive activation, including the dorsal-medial thalamus, globus pallidus (GP) and anterior cingulate cortex (ACC), has been described in healthy people at 3 mmol/l and considered to be associated with autonomic stress responses [13]. Using [15O]water positron emission tomography (PET) scans repeated during induction of, maintenance of and recovery from hypoglycaemia at 2.8 mmol/l, we described activation of the thalamus and ACC, with progressive involvement of pathways involved in feeding behaviour and reward, symptom perception and aversion [14].
Less is known about the impact of diabetes and hypoglycaemia awareness (HA) status. Hormone responses to hypoglycaemia are diminished in type 1 diabetes [15], but the importance for symptoms experienced is unclear [16]. Thalamic activation has been described as enhanced in a model of IAH [17] but reduced in IAH itself [18]. A recent study compared a single measurement of global and regional cerebral blood flow (rCBF) after 45 min at 2.8 mmol/l in people with type 1 diabetes with and without IAH using arterial spin-labelling MRI. This reported a global increase in cerebral blood flow only in IAH, and failure of an enhanced regional thalamic response [19], but there are no reports of IAH-specific differences in other regional responses.
Understanding the central pathophysiology of IAH is key to its management. Although IAH can be restored by avoiding hypoglycaemia [2, 20], this can be difficult to achieve, with 8% of adults with type 1 diabetes showing low concern about hypoglycaemia despite being at high risk [21]. Cognitions around hypoglycaemia may create barriers to its avoidance [22]. We therefore extended the use of repeated [15O]water PET scans to measure changes in regional brain perfusion during sequential euglycaemia, hypoglycaemia and recovery in men with type 1 diabetes with and without IAH.
Methods
Participants
Right-handed men with type 1 diabetes aged between 20 and 50 years, with HbA1c levels less than 86 mmol/mol (<10%), were recruited into two groups, based on their awareness of hypoglycaemia as defined by history and 8-item Clarke score [23]. HA was defined as good awareness of occasional hypoglycaemia, no severe hypoglycaemia in the past year and a Clarke score ≤3. IAH was defined by history, including experience of severe hypoglycaemia, and Clarke score ≥4.
The protocol was approved by the Ethics Committee of King’s College Hospital London and the Administration of Radioactive Substances Committee (ARSCAC, Health Protection Agency, Didcot, Oxfordshire, UK). All participants gave written informed consent.
Protocol
Scans were performed at the PET Imaging Centre, St Thomas’ Hospital, London, using a GE Discovery ST PET/computerised tomography (CT) scanner (GE Medical Systems, Milwaukee, WI, USA) with a 15.8 cm axial field of view. Participants were admitted the evening before the study. Two intravenous cannulae were inserted for infusion of soluble insulin (Actrapid; NovoNordisk, Copenhagen, Denmark) in a 4% (vol./vol.) saline (154 mmol/l NaCl) solution of autologous blood; blood was sampled hourly. Participants fasted after their evening meal, sips of water being allowed, and omitted their evening background insulin dose. To achieve normoglycaemia without hypoglycaemia, plasma glucose was maintained between 4 and 7 mmol/l overnight by adjusting the insulin infusion.
In the morning, the left radial artery was cannulated. After at least 20 min, each participant rested supine on the scanner trolley, in a headrest with a forehead positioning strap. Once in the scanner, the head position was checked using gantry lasers. A new primed-continuous infusion of soluble insulin was started, at a maintenance rate 1.5 mU kg−1 min−1. Four minutes later, an infusion of 10% (wt/vol.) glucose (Baxter Healthcare, Thetford, Norfolk, UK) was started and was adjusted using 5 min arterial plasma glucose readings (YSI 2300 Stat Plus; Yellow Springs Instruments, Yellow Springs, OH, USA). The target plasma glucose level was 5 mmol/l for 40 min, with a reduction over 20 min to 2.6 mmol/l, maintenance at 2.6 mmol/l for 45 min, and restoration to 5 mmol/l (over 15–20 min) for 30 min. The insulin was then stopped, and the participant withdrawn from the scanner. He was then given lunch, with his usual subcutaneous fast-acting insulin pre-meal dose and, if a morning dose of basal insulin had been omitted, a reduced basal insulin dose to provide cover until the evening dose. The glucose infusion was reduced and plasma glucose monitored until concentrations were spontaneously maintained. The cannulae were then removed. Participants were advised about monitoring and dosing to minimise risk of hypoglycaemia over the next 24 h.
Scanning protocol
This was as previously reported [14]. In brief, the brain was localised in the PET view field using a planar CT scout. A low-dose CT scan was acquired to correct attenuation in subsequent PET scans. Head position was checked, and 3 min [15O]water PET scans were made at 10 min intervals. For each scan, 350 MBq [15O]water in 10 ml sterile water was manually injected intravenously over 10 s. Three scans were acquired during euglycaemia: one during the fall in glucose, five during the hypoglycaemic phase and three during recovery. Scans were acquired in 3D mode, reconstructed to a single static frame using the 3D FORE algorithm [24], and 2D-filtered back-projection with scatter correction and CT-based correction of attenuation. To minimise movement artefacts, each participant’s CT scan was realigned to each PET scan using the rigid-body registration algorithm in the Statistical Parametric Mapping 2 program (SPM2; www.fil.ion.ucl.ac.uk/spm, accessed 15 March 2013). The realigned CT was used to correct the attenuation in the PET reconstruction.
Assessment of physiological responses
After scanning, arterial blood was taken to measure counterregulatory hormones. The participant was asked verbally to rate (from 1 to 7) 13 hypoglycaemia-associated symptoms (see below) [25].
Biochemical analyses
Blood was kept on ice, spun, separated and flash-frozen on dry ice until storage. A volume of 1 ml was added to 30% (wt/vol.) polyethylene glycol for free insulin radioimmunoassay (Diagnostic Systems Laboratories, London, UK). Blood (3 ml) for catecholamines was taken into heparinised tubes containing 15 μl sodium metabisulphite; plasma was separated at the time of study, stored at −80°C and analysed by radioimmunoassay [14].
Symptom scores
Scores for sweating, shakiness, anxiety, warmth, palpitation and tingling were summed as autonomic. Scores for dizziness, irritability, difficulty in speaking, confusion, lack of energy, drowsiness and poor concentration were totalled as neuroglycopenic.
Statistical analyses of non-imaging data
Age, BMI, HbA1c and duration of diabetes were compared between groups using independent sample t tests, and Clarke scores by Mann–Whitney U testing. Hormonal and symptom responses to hypoglycaemia and impact of awareness status were examined by calculating the main and interaction effects of scan and group on each variable using a repeated measures linear mixed model (first-order autoregressive covariance structure). To assess the effect of hypoglycaemia, baseline values for each variable were calculated by averaging data from scans 1–3. A summary statistic of response to the total hypoglycaemic period was calculated as the incremental AUC (iAUC) of the response in scans 4–9. The effect of hypoglycaemia was tested using a one-sample t test of the iAUC if the mixed model revealed significant scan or interaction effects. To assess differences between the two groups, the baseline and iAUC measures were used in two-sample t tests if the mixed model revealed significant group or interaction effects. Analyses were performed using SPSS software version 24 (www-01.ibm.com/software/uk/analytics/spss/).
Neuroimaging analysis
The analytic program was chosen to allow interrogation of the data without preconceptions of the brain regions that might respond to hypoglycaemia in people with type 1 diabetes or respond differently between HA and IAH. SPM2 was used to preprocess and analyse the PET data. Image processing and analysis of regional perfusion were performed automatically and identically in each participant or group, removing the need for blinding. PET images were transformed into standard anatomical space conforming to the standard Montreal Neurological Institute (MNI) space using the [15O]water PET template supplied with SPM2, masked to exclude the scalp and smoothed using a Gaussian kernel (full width at half maximum [FWHM] = 6 mm).
Within SPM2, each image was spatially normalised to its whole-brain mean using SPM2, which performs an initial affine registration followed by a basis function method non-linear registration [26] and calculates regional perfusion relative to the whole-brain mean. SPM2 calculates the mean image intensity across the whole brain, without segmentation, using its default threshold method (mean of the overall mean × 0.8), and uses integrated activity over time (here 3 min), which is proportional to rCBF [27].
For analysis, scans were grouped as: euglycaemia/baseline (scans 1–3), early hypoglycaemia (scans 4–6), established hypoglycaemia (scans 7–9) and recovery (scans 10–12). Two-way repeated measures ANOVA was used to investigate the main effects of stage of hypoglycaemia (early, late or recovery vs baseline), group and interactions [28].
Regions of significant effects were calculated using a voxel-level p value <0.001 and cluster sizes (k) ≥100 voxels; these were recalculated at p < 0.005, k ≥ 50 voxels to examine for smaller differences where more significant differences had been excluded. t values <2 (or <−2) indicate significance with >95% confidence. Clusters were localised using the Tziortzi atlas [29].
Results
Participants
Of the 17 men with type 1 diabetes recruited, nine had intact HA. These nine individuals were aged 37.6 ± 9.3 years and had a diabetes duration of 14.3 ± 12.3 years, BMI, 23.4 ± 3.4 kg/m2 and HbA1c, 58.5 ± 12.4 mmol/mol (7.5 ± 1.3%) (all means ± SD). They reported good awareness of hypoglycaemia, with a median Clarke score of 2 (range 1–3) and no severe hypoglycaemia in the past year. The other eight men (means ± SD: age, 36.4 ± 7.8 years; diabetes duration, 27.1 ± 11.9 years; BMI, 26.6 ± 1.4 kg/m2; HbA1c, 57.7 ± 9.3 mmol/mol [7.3 ± 0.8%]) had IAH, with a median Clarke score of 5.5 (range 4–6); all had a history of severe hypoglycaemia. The IAH and HA groups did not differ in terms of age (p = 0.79), duration of diabetes (p = 0.07) or HbA1c (p = 0.89) but had slightly a greater BMI (p = 0.02). By design, Clarke scores were significantly different between groups (p < 0.001).
Plasma insulin, glucose, symptoms and counterregulatory hormones
During the studies, steady-state free plasma insulin was (mean ± SD) 476.4 ± 138.48 and 487.9 ± 225.3 pmol/l for the HA and IAH group, respectively (p = 0.89). The hypoglycaemia achieved (Fig. 1a) did not differ between groups (2.4 ± 0.1 and 2.4 ± 0.1 mmol/l, respectively; p = 0.7); there were no significant differences in starting glucose level, or glucose concentration during recovery. Mean glucose levels were: scan 4, 3.4 ± 0.2 vs 3.5 ± 0.4; scan 5, 2.7 ± 0.2 vs 2.7 ± 0.3; and scan 6 2.2 ± 0.3 vs 2.3 ± 0.2 (all p > 0.05). Hormone concentrations did not differ between the groups during euglycaemia. Adrenaline (epinephrine) and noradrenaline (norepinephrine) (Fig. 1b, c) showed significant main effects of scan number (see also electronic supplementary material [ESM] Table 1), with a significant interaction effect of scan and group for adrenaline levels. Post hoc tests of effect of hypoglycaemia using iAUC revealed significant responses in HA for adrenaline (p < 0.001) and noradrenaline (p = 0.009). The adrenaline response with IAH was significant (p = 0.003) but significantly lower than for HA (p for comparison = 0.007). There was a significant noradrenaline response only in the HA group (p = 0.009). The iAUC for cortisol did not reach significance in either group, with a trend towards significance for HA (p = 0.075; see ESM Table 1). The iAUC for growth hormone was significant in both groups (HA, p = 0.035; IAH, p = 0.006; see ESM Table 1).
Plasma glucose, catecholamine and symptom responses. Blue lines, HA; red lines, IAH. (a) Plasma glucose levels (mean ± SD). Grey bars represent scan time points. iAUC was not significantly different between groups. (b, c) Mean ± SD at each scan for (b) plasma adrenaline (iAUC, p = 0.007 between groups) and (c) plasma noradrenaline (significant response to hypoglycaemia in HA only (p < 0.009); no significant difference in iAUC between groups. (d, e) Box plots showing median (circles), upper and lower quartiles (box), range (vertical lines) and outliers (crosses) for (d) autonomic symptom scores and (e) neuroglycopenic symptom scores. For both (d) and (e), difference between groups, p = 0.002
Symptom responses
Significant main effects for scan, group and interaction were revealed in autonomic and neuroglycopenic total scores (Fig. 1d, e; ESM Table 1). The HA group showed significant responses (iAUC) for both scores (422.7 ± 237.1, p = 0.001 and 478.9 ± 311.1, p = 0.002, respectively). The IAH group showed a small response for autonomic scores (26.2 ± 35.5; p = 0.038), significantly lower than the response with HA (p = 0.002), and no significant neuroglycopenic symptom response (34.8 ± 88.8, p = 0.15 from baseline, p = 0.002 vs HA group). Baseline autonomic scores were slightly higher for HA than IAH (p = 0.024), with a mean difference in score of 1.5, which was small in comparison with the mean increase of 10.5 seen during hypoglycaemia.
Neuroimaging data
Regional brain responses to acute hypoglycaemia in type 1 diabetes with preserved HA
The response to early hypoglycaemia across HA participants (Fig. 2a, ESM Table 2) included a regional increase in perfusion (compared with baseline) in the thalamic pulvinar bilaterally, bilateral dorsolateral frontal (DLF) cortices, right insular cortex and ACC; a decrease in perfusion was seen in the left inferior temporal gyrus. As hypoglycaemia progressed (Fig. 2b, ESM Table 3), the activation area became more extensive, with additional activation (vs baseline) in the following: posterior, middle and anterior thalamus and GP; bilateral insula and frontal opercula; frontal cortex including the DLF cortex bilaterally and lateral orbital cortex; ACC; and precuneus and right angular gyrus/supramarginal gyrus/superior temporal gyrus. Perfusion was reduced in established hypoglycaemia bilaterally in the parahippocampal and posterior parietal cortex, inferior temporal gyri and parts of the cerebellum including the vermis. During recovery (Fig. 2c, ESM Table 4), regions including the ACC, GP, right insula and left precuneus showed activation; there was persisting deactivation in the inferior temporal and posterior parietal gyri, and new activation of the amygdala.
SPM2 results showing significant (voxel level p < 0.001, k ≥ 100 voxels) regional changes in brain perfusion compared with baseline euglycaemia during (a) early hypoglycaemia, (b) established hypoglycaemia and (c) recovery from hypoglycaemia measured with repeated [15O]water PET scans in men with IAH and without (HA). For analysis, scans were grouped as euglycaemia (scans 1–3), early hypoglycaemia (scans 4–6), established hypoglycaemia (scans 7–9) and recovery (scans 10–12). Significant increases in rCBF are shown in red-yellow, and decreases are shown in blue-white. t values are shown in the right-hand scale. Scans were overlaid onto an MRI scan in Montreal Neurological Institute standard space (greyscale)
Impact of awareness of hypoglycaemia on regional brain responses to hypoglycaemia
Regional brain responses to hypoglycaemia in IAH involved various regions similar to those showing responses in the HA group (Fig. 2, ESM Tables 5–7), with some differences that were explored in a formal comparison. Directly comparing responses between groups identified clusters showing significantly different hypoglycaemia responses between the IAH and HA groups at the second statistical threshold voxel level (p < 0.005, k ≥ 50 voxels) (Fig. 3; Table 1). In early hypoglycaemia (Fig. 3a–c), five clusters were identified. One in the left lingual gyrus showed deactivation for IAH and activation for HA, and four—the right central operculum, medial orbital (MO) cortex bilaterally and left posterior DLF cortex (two clusters)—showed activation in IAH vs deactivation in HA.
SPM2 results for comparisons of HA and IAH responses to hypoglycaemia (see Table 1). (a, d, g) Images showing regions with significantly different responses between HA and IAH to early (a), established (d) and recovered (g) hypoglycaemia (change from baseline). Changes were detected using SPM2 statistical thresholds set at voxelwise p < 0.005 and k ≥ 50 voxels. No clusters were seen with stricter thresholds (k ≥ 100 voxels, p < 0.001). Yellow clusters show regions where response is significantly more positive for HA than IAH; blue clusters show regions where response is more negative in HA than IAH. t values are shown in the right-hand scale. Associated bar charts show the mean and SE of group responses for whole clusters; all between-group differences were significant, as defined above. (b, e, h) Data for clusters where response is more positive for HA than IAH in early (b), established (e) and recovered (h) hypoglycaemia. (c, f, i) Data for clusters where response is more negative for HA than IAH in early (c), established (f) and recovered (i) hypoglycaemia. Black bars, HA; white bars, IAH. a, anterior; AG, angular gyrus; CC, cingulate cortex; CO, central operculum; d, dorsal; i, inferior; L, left; LG, lingual gyrus; m, medial; MF, medial frontal cortex; MidB, midbrain; p, posterior; Par, parahippocampal gyrus; PoCG, postcentral gyrus; PrCG, precentral gyrus; R, right; s, superior; SMG, supramarginal gyrus; TG, temporal gyrus; TOF, temporal occipital fusiform gyrus; TP, temporal gyrus. Where no laterality is noted (L or R), the cluster was represented bilaterally. Where there are two data sets for one brain region, there were two clusters in that region
As hypoglycaemia continued (Fig. 3d–f), eight clusters showed significantly different changes in activation between groups. Five showed limited or absent responses for IAH but activation for HA: the right GP, ACC, dorsal cingulate cortex, right pre- and bilateral post-central gyri, and left precuneus. Two further clusters, in the right MO and left parietal cortices (parietal lobule and angular gyrus), showed activation in IAH but no change or deactivation in HA. A cluster including the left posterior middle temporal gyrus, angular gyrus and occipital pole showed no change in IAH but deactivation in HA. Fourteen clusters showed significantly different activation between groups during the recovery period (Fig. 3g–i). IAH showed deactivation or minimal response compared with activation in the HA group in the following: right fusiform cortex; a midbrain cluster, extending to the right amygdala; right superior temporal gyrus/insula; left pre- and post-central gyri; and a cluster including right white matter, anterior temporal pole and amygdala. The IAH group failed to show the deactivation seen with HA in the bilateral middle and left inferior temporal gyri. However, there was activation in IAH compared with deactivation in HA in the left posterior medial frontal cortex, left posterior DLF cortex extending to pre-central gyrus, and left angular gyrus/occipital pole/parietal lobule/supramarginal gyrus/left posterior superior temporal gyrus.
Discussion
In this neuroimaging study of men with type 1 diabetes, differences in symptomatic and hormonal responses to hypoglycaemia between participants with preserved (HA) or impaired (IAH) awareness of hypoglycaemia were accompanied by subtle differences in brain responses. These occurred not only in regions associated with the generation and subjective awareness of stress responses, but also in regions associated with executive control, reward, memory and emotional salience.
Defective hormonal responses to hypoglycaemia in IAH are well recognised [2, 8, 16]. They are inducible by exposure to hypoglycaemia [7, 8] and restored by avoiding it [2, 20]. The IAH group showed the expected diminution of symptomatic and catecholamine responses to our hypoglycaemic challenge.
Responses in men with type 1 diabetes and intact awareness
Our neuroimaging data in HA participants are largely consistent with studies in people without diabetes and extend earlier observations, particularly by describing the evolution of responses during development of and recovery from hypoglycaemia. Our ‘early’ scans were made as arterialised plasma glucose level was falling, and include data collected at glucose values between 3.5 and 2.2 mmol/l; the ‘established’ data were collected at 2.4 mmol/l. Thalamic activation seen in both early and established hypoglycaemia is consistent with data from individuals without diabetes, and with the role of the thalamus in relaying sensory signals to cortical areas [30]. Novel findings include insula activation, seen in all three phases of hypoglycaemia and not previously described in diabetes. Using similar techniques, we previously described insular activation in established hypoglycaemia only in people without diabetes [14]; we speculate that earlier and more persistent activation in type 1 diabetes relates to heightened sensitivity to changes in plasma glucose or prior experience of more fluctuating glucose concentrations. Wiegers et al did not find insular activation in people without diabetes and described reduced insular perfusion using functional MRI (fMRI) in seven HA individuals with type 1 diabetes [19]. Comparing direction of signal change across studies using different technologies is complex; however, [15O]water PET is less susceptible to low signal to noise ratios and movement than fMRI. It also allows more quantitative measurement of regional responses and may be better at detecting differences between groups in studies of similar size [31].
Activation of the GP in established hypoglycaemia and recovery, and the ACC in all three phases, is consistent with some reports involving individuals without diabetes at similar glucose concentrations [13, 14] but has not been described in type 1 diabetes. The GP and ACC, involved in reward, might be reacting to the hypoglycaemic stress responses. Activation of orbital cortex is likewise consistent with non-diabetic responses to comparable hypoglycaemia [13, 14, 18] but not previously observed in type 1 diabetes [19]. The orbital cortex encodes stimulus value or salience [32], and the lateral orbital cortex forms a ‘salience’ network with the ACC [33]. Activation of the DLF cortex in response to hypoglycaemia has not previously been described [12,13,14, 18, 19]. It has a role in working memory—the short-term recall and processing of information necessary for complex task performance, including learning and reasoning [34]—and is involved in inhibitory control [35, 36]. Changing activity during hypoglycaemia is consistent with clinically observed changes in cognition and behavioural disinhibition during hypoglycaemia, and recall after it. The report of activation of the precuneus and angular gyrus during established hypoglycaemia and recovery is also novel [12,13,14, 19]. The precuneus is part of the ‘default mode network’, showing reduced activity compared with the resting state when undertaking tasks [33]; activation may reflect lesser ability to perform tasks during hypoglycaemia. The angular gyrus, linked to the DLF cortex [37] and showing parallel responses, plays a role in regulating shift of attention to more salient stimuli [38]. The amygdala encodes the predicted biological relevance of a stimulus [39]; its activation in recovery may be a key determinant of responses to subsequent hypoglycaemic events.
Deactivation of the inferior temporal gyri in all three phases, of parietal regions during established hypoglycaemia and recovery, and of parahippocampal regions during established hypoglycaemia, described in some studies of individuals without diabetes but not previously in type 1 diabetes, provide a neurological correlate of failure to form memory during hypoglycaemia: temporal gyri for semantic or conceptual memory [40], and parahippocampal gyrus and lateral parietal cortex for episodic memory [41].
Impact of IAH
The subtle differences in hypoglycaemia responses in IAH are potentially important. In early hypoglycaemia, deactivation seen in parts of the central operculum, MO cortex and posterior and lateral DLF cortex in HA was replaced by activation. Operculum activation changes in response to food cues, modulated by feeding state and degree of liking the food [32]: differences between IAH and HA may relate to differences in the drive to eat to treat. These were paralleled by different responses in the MO cortex, encoding stimulus value and salience [32], in early and established hypoglycaemia; this may underlie differences in perceived importance of hypoglycaemia, including lack of aversion. Lack of activation of the GP, with its role in memory of unpleasant experiences or aversion [42], is also consistent with not finding hypoglycaemia unpleasant. These are key findings, as IAH is clinically associated with reduced motivation to avoid hypoglycaemia [21, 22], with reduced incentive to treat hypoglycaemia as important [43].
Parts of the dorsal and posterior DLF cortex responded from early hypoglycaemia through to recovery with activation responses in IAH compared with deactivation in HA. Hypoglycaemia is associated with impaired inhibitory control; perhaps the deactivation in HA represents conscious attempts to maintain inhibitory control of behaviour during hypoglycaemia.
The ACC is involved in decision-making and conflict resolution between options, and is key in monitoring performance, evaluating actions and detecting events that require behavioural modification and re-evaluation [44]. Lack of ACC activation only in IAH fits with views of IAH as a habituation response. A similar lack of activation in IAH in the somatosensory post-central (somatosensory) and pre-central (motor) gyri, persisting in recovery, may reflect reduced somatic sensations (e.g. warmth, shakiness) and motor responses (e.g. tremor) experienced by the IAH group in hypoglycaemia.
Minimal responses in IAH, vs deactivation in HA, in the left posterior middle temporal gyrus during established hypoglycaemia, and the bilateral posterior middle and left inferior temporal gyri in recovery, are also consistent with different memory formation during hypoglycaemia and recovery [40, 41]. The same is true of differences in the left parietal lobule/angular gyrus in established hypoglycaemia, with activation in IAH but minimal response in HA, and in recovery in the left angular gyrus and supramarginal gyrus, with activation in IAH and deactivation in HA. The lateral parietal cortex shows functional connectivity with the hippocampal formation and is associated with recollection of experiences [41, 45].
In recovery, in addition to persisting differential responses in somatosensory and memory networks, we found activation in IAH and deactivation in HA in part of the medial frontal cortex; this was in a cluster corresponding to regions of the dorsal-medial prefrontal cortex identified as having a role in self-referential mental activity, such as making judgements about unpleasantness/pleasantness [46]. It may also have a role in episodic or experiential memory [41]. This may provide a correlate for individuals with type 1 diabetes with IAH and HA forming differently valenced memories of the experience of hypoglycaemia. However, the medial frontal cortex, along with the lateral parietal regions discussed above, is also a component of the default mode network [33], and these differences may represent hypoglycaemia being a different ‘task’ for the brain in IAH than HA.
Our participants were matched well for age, diabetes duration and diabetes control but imperfectly for BMI. Obesity alters brain responses to food and food cues, including the responses of some frontal regions described as different in their response to hypoglycaemia here [47]. However, none of our participants was obese, so it is unlikely our observed differences in response to hypoglycaemia were related to this. The recruitment of only men facilitates research involving radio-isotopes and importantly reduces variability of responses due to sex differences in counterregulation [48]. The clinical picture of IAH is not sex-specific so our data interpretation probably also applies to women; however, adaptation to antecedent hypoglycaemia may vary by sex, at least in individuals without diabetes [49], and studies in women would be of interest. Right-handedness was chosen as many brain functions are lateralised.
The strengths of our study include pre-study determination of awareness status on clinical grounds, so individuals defined as having IAH were representative of those with clinically problematic hypoglycaemia. In addition, the analysis did not require a preconception of brain regions that might respond differently to hypoglycaemia by awareness status. Although less powerful than a region of interest analysis, in which data are compared between groups only in prespecified brain regions, this enabled us to identify areas not traditionally associated with stress responses. That differences between the two groups (the effect of awareness status on rCBF responses) were identified at lower thresholds than those used to find differences within groups (the effect of hypoglycaemia) is statistically explicable: within-group comparison is always more powerful than between-group comparison, where differences between participants come into play. It is also biologically plausible as hypoglycaemia is a large stress stimulus whereas differences between HA and IAH are probably an order of magnitude less. It is, however, possible that other brain regions responding differently were missed.
Conclusion
In conclusion, we used [15O]water PET to describe the evolution of the brain’s responses to hypoglycaemia over time in men with type 1 diabetes and found differences related to HA status. These differences provide a mechanism explaining the resilience of IAH as a clinical entity highly resistant to treatment strategies that are usually capable of restoring awareness through hypoglycaemia avoidance. The neuroimaging differences are compatible with a different behavioural response, with regard to the drive to eat, different emotional salience of the experience and differences in its recall; all may contribute in IAH to the reduced drive to treat hypoglycaemia in timely fashion and avoid future episodes. It remains to be determined whether these IAH-specific central responses are induced by hypoglycaemia exposure or are an inherent way of responding to stress that results in a proportion of people susceptible to persistent IAH. If the latter, it may be possible to detect high risk for IAH and recurrent severe hypoglycaemia through cognitive or neuroimaging studies before the syndrome has fully developed. Meanwhile, the differential responses described are likely to correlate with cognitions and behaviours unhelpful to future hypoglycaemia avoidance; further research is required into how best to address these in clinical practice.
Data availability
The primary data are medical imaging data for which there are no publicly available repositories. The authors are able to provide data in response to email requests.
Abbreviations
- ACC:
-
Anterior cingulate cortex
- CT:
-
Computerised tomography
- DLF:
-
Dorsolateral frontal
- fMRI:
-
Functional MRI
- GP:
-
Globus pallidus
- HA:
-
Hypoglycaemia awareness
- IAH:
-
Impaired awareness of hypoglycaemia
- iAUC:
-
Incremental AUC
- k :
-
Cluster size
- MO:
-
Medial orbital
- PET:
-
Positron emission tomography
- rCBF:
-
Regional cerebral blood flow
- SPM:
-
Statistical Parametric Mapping 2
References
International Hypoglycaemia Study Group (2017) Glucose concentrations of less than 3.0 mmol/l (54 mg/dl) should be reported in clinical trials: a joint position statement of the American Diabetes Association and the European Association for the Study of diabetes. Diabetologia 60:3–6
Cranston I, Lomas J, Maran A, Macdonald I, Amiel SA (1994) Restoration of hypoglycaemia awareness in patients with long-duration insulin-dependent diabetes. Lancet 344:283–287
Geddes J, Schopman JE, Zammitt NN, Frier BM (2008) Prevalence of impaired awareness of hypoglycaemia in adults with type 1 diabetes. Diabet Med 25:501–504
Hopkins D, Lawrence I, Mansell P et al (2012) Improved biomedical and psychological outcomes 1 year after structured education in flexible insulin therapy for people with type 1 diabetes: the U.K. DAFNE experience. Diabetes Care 35:1638–1642
Schopman JE, Geddes J, Frier BM (2010) Prevalence of impaired awareness of hypoglycaemia and frequency of hypoglycaemia in insulin-treated type 2 diabetes. Diabetes Res Clin Pract 87:64–68
Simpson I, Appel N, Hokari M et al (1999) Blood-brain barrier glucose transporter: effects of hypo- and hyperglycemia revisited. J Neurochem 72:238–247
Heller SR, Cryer PE (1991) Reduced neuroendocrine and symptomatic responses to subsequent hypoglycemia after 1 episode of hypoglycemia in nondiabetic humans. Diabetes 40:223–226
Dagogo-Jack SE, Craft S, Cryer PE (1993) Hypoglycemia-associated autonomic failure in insulin-dependent diabetes mellitus. Recent antecedent hypoglycemia reduces. Clin Invest 91:819–828
Boyle PJ, Kempers SF, O'Connor AM, Nagy RJ (1995) Brain glucose uptake and unawareness of hypoglycemia in patients with insulin-dependent diabetes mellitus. N Engl J Med 333:1726–1731
Maran A, Lomas J, Macdonald IA, Amiel SA (1995) Lack of preservation of higher brain function during hypoglycaemia in patients with intensively-treated IDDM. Diabetologia 38:1412–1148
Segel SA, Fanelli CG, Dence CS et al (2001) Blood-to-brain glucose transport, cerebral glucose metabolism, and cerebral blood flow are not increased after hypoglycemia. Diabetes 50:1911–1917
Page KA, Arora J, Qiu M, Relwani R, Constable RT, Sherwin RS (2009) Small decrements in systemic glucose provoke increases in hypothalamic blood flow prior to the release of counterregulatory hormones. Diabetes 58:448–452
Teves D, Videen TO, Cryer PE, Powers WJ (2004) Activation of human medial prefrontal cortex during autonomic responses to hypoglycaemia. Proc Natl Acad Sci U S A 101:6217–6221
Teh MM, Dunn JT, Choudhary P et al (2010) Evolution and resolution of human brain perfusion responses to the stress of induced hypoglycaemia. NeuroImage 53:584–592
Bolli G, de Feo P, Compagnucci P et al (1983) Abnormal glucose counterregulation in insulin-dependent diabetes mellitus. Interaction of anti-insulin antibodies and impaired glucagon and epinephrine secretion. Diabetes 32:134–141
Dagogo-Jack S, Rattarasarn C, Cryer PE (1994) Reversal of hypoglycaemia unawareness, but not defective glucose counterregulation, in IDDM. Diabetes 43:1426–1434
Arbelaez AM, Powers WJ, Videen TO, Price JL, Cryer PE (2008) Attenuation of counterregulatory responses to recurrent hypoglycaemia by active thalamic inhibition: a mechanism for hypoglycaemia-associated autonomic failure. Diabetes 57:470–475
Mangia S, Tesfaye N, De Martino F et al (2012) Hypoglycaemia-induced increases in thalamic cerebral blood flow are blunted in subjects with type 1 diabetes and hypoglycaemia unawareness. J Cereb Blood Flow Metab 32:2084–2090
Wiegers EC, Becker KM, Rooijackers HM et al (2017) Cerebral blood flow response to hypoglycemia is altered in patients with type 1 diabetes and impaired awareness of hypoglycemia. J Cereb Blood Flow Metab 37:1994–2001
Fanelli CG, Epifano L, Rambotti AM et al (1993) Meticulous prevention of hypoglycaemia normalizes the glycaemic thresholds and magnitude of most of neuroendocrine responses to, symptoms of, and cognitive function during hypoglycaemia in intensively treated patients with short-term IDDM. Diabetes 42:1683–1689
Anderbro T, Gonder-Frederick L, Bolinder J et al (2015) Fear of hypoglycaemia: relationship to hypoglycaemic risk and psychological factors. Acta Diabetol 52:581–589
Rogers HA, de Zoysa N, Amiel SA (2012) Patient experience of hypoglycaemia unawareness in type 1 diabetes: are patients appropriately concerned? Diabet Med 29:321–327
Clarke WL, Cox DJ, Gonder-Frederick LA, Julian D, Schlundt D, Polonsky W (1995) Reduced awareness of hypoglycaemia in adults with IDDM. A prospective study of hypoglycaemic frequency and associated symptoms. Diabetes Care 18:517–522
Defrise M, Kinahan PE, Townsend DW, Michel C, Sibomana M, Newport DF (1997) Exact and approximate rebinning algorithms for 3-D PET data. IEEE Trans Med Imaging 16:145–158
Deary IJ, Hepburn DA, KM ML, Frier BM (1993) Partitioning the symptoms of hypoglycaemia using multi-sample confirmatory factor analysis. Diabetologia 36:771–777
Ashburner J, Friston KJ (1999) Nonlinear spatial normalization using basis functions. Hum Brain Mapp 7:254–266
Herscovitch P, Markham J, Raichle ME (1983) Brain blood flow measured with intravenous H2(15)O. I. Theory and error analysis. J Nucl Med 24:782–789
Friston KJ, Holmes AP, Price CJ, Büchel C, Worsley KJ (1999) Multisubject fMRI studies and conjunction analyses. NeuroImage 10:385–396
Tziortzi AC, Searle GE, Tzimopoulou S et al (2011) Imaging dopamine receptors in humans with [11C]-(+)-PHNO: dissection of D3 signal and anatomy. NeuroImage 54:264–277
Sherman SM (2016) Thalamus plays a central role in ongoing cortical functioning. Nat Neurosci 19:533–541
Kameyama M, Murakami K, Jinzaki M (2016) Comparison of [(15)O] H2O positron emission tomography and functional magnetic resonance imaging in activation studies. World J Nucl Med 15:3–6
Kringelbach ML, O’Doherty J, Rolls ET, Andrews C (2003) Activation of the human orbitofrontal cortex to a liquid food stimulus is correlated with its subjective pleasantness. Cereb Cortex 13:1064–1071
Raichle ME (2015) The brain’s default mode network. Annu Rev Neurosci 38:433–447
Hautzel H, Mottaghy FM, Schmidt D et al (2002) Topographic segregation and convergence of verbal, object, shape and spatial working memory in humans. Neurosci Lett 323:156–160
Miller BT, D’Esposito M (2005) Searching for ‘the top’ in top-down control. Neuron 48:535–538
Tanji J, Hoshi E (2008) Role of the lateral prefrontal cortex in executive behavioral control. Physiol Rev 88:37–57
Sakurai Y (2017) Brodmann areas 39 and 40: human parietal association area and higher cortical function. Brain Nerve 69:461–469
Gottlieb J (2007) From thought to action: the parietal cortex as a bridge between perception, action, and cognition. Neuron 53:9–16
Staniloiu A, Markowitsch HJ (2012) A rapprochement between emotion and cognition: amygdala, emotion, and self-relevance in episodic-autobiographical memory. Behav Brain Sci 35:164–166
Bonner MF, Price AR (2013) Where is the anterior temporal lobe and what does it do? J Neurosci 33:4213–4215
Rugg MD, Vilberg KL (2013) Brain networks underlying episodic memory retrieval. Curr Opin Neurobiol 23:255–260
Skirzewski M, López W, Mosquera E et al (1993) Enhanced GABAergic tone in the ventral pallidum: memory of unpleasant experiences? Brain Res 624:1–10
Smith CB, Choudhary P, Pernet A, Hopkins D, Amiel SA (2009) Hypoglycaemia unawareness is associated with reduced adherence to therapeutic decisions in patients with type 1 diabetes: evidence from a clinical audit. Diabetes Care 32:1196–1198
Kolling N, Behrens TEJ, Wittmann MK, Rushworth MFS (2016) Multiple signals in anterior cingulate cortex. Curr Opin Neurobiol 37:36–43
Vincent JL, Snyder AZ, Fox MD et al (2006) Coherent spontaneous activity identifies a hippocampal-parietal memory network. J Neurophysiol 96:3517–3531
Gusnard DA, Akbudak E, Shulman GE, Raichle ME (2001) Medial prefrontal cortex and self-referential mental activity: relation to a default mode of brain function. Proc Natl Acad Sci 98:4259–4264
Cheah YS, Lee S, Ashoor G et al (2014) Ageing diminishes the modulation of human brain responses to visual food cues by meal ingestion. Int J Obes 38:1186–1192
Amiel SA, Maran A, Powrie JK, Umpleby AM, Macdonald IA (1993) Gender differences in counterregulation to hypoglycaemia. Diabetologia 36:460–464
Davis SN, Shavers C, Costa F (2000) Gender-related differences in counterregulatory responses to antecedent hypoglycemia in normal humans. J Clin Endocrinol Metab 85:2148–2157
Acknowledgements
We are grateful to the following: research nurses A. Pernet and B. Wilson (King’s College London and King’s College Hospital NHS Foundation Trust), who assisted in the care of the participants and supported the clinical studies and sample-handling; M. O’Doherty and the radiologists, radiographers and chemists of the King’s College London PET Imaging Centre for their support; L. Reed, then of the Institute of Psychiatry, King’s College London, for significant intellectual input into the interpretation of our neuroimaging data; D. Forster, Nottingham, and J. Jones London, for the biochemical analyses; and finally our volunteers.
Contribution statement
SAA, JTD and PKM conceived and designed the study. MMT and PC acquired the data; JTD, PKM, SAA, KFH, IM and PC analysed and/or interpreted the data. SAA, JTD and KFH drafted the article. All authors revised it critically for important intellectual content and gave final approval of the version to be published. SAA is the guarantor of this work.
Funding
This work was funded by a research grant from the JDRF International.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that there is no duality of interest associated with this manuscript.
Electronic supplementary material
ESM
(PDF 1.45 mb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Dunn, J.T., Choudhary, P., Teh, M.M. et al. The impact of hypoglycaemia awareness status on regional brain responses to acute hypoglycaemia in men with type 1 diabetes. Diabetologia 61, 1676–1687 (2018). https://doi.org/10.1007/s00125-018-4622-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-018-4622-2