Abstract
Aims/hypothesis
Present guidelines for the treatment of type 2 diabetes recommend HbA1c values of less than 7%. As beta cell function worsens during progress of the disease, insulin therapy is often necessary to achieve this ambitious goal. However, due to peripheral insulin resistance, many patients need rather high insulin dosages. In the light of the extremely high cardiovascular risk of diabetic patients, it is important to determine whether high concentrations of insulin or its frequently used analogues are harmful to the cardiovascular system. We therefore investigated the modulatory effects of regular human insulin and its analogue glargine on proliferation and apoptosis of human coronary artery endothelial cells (HCAECs) and human coronary artery smooth muscle cells (HCASMCs).
Methods
Cells were treated with regular human insulin or insulin glargine. Proliferation was determined by [3H]thymidine incorporation and by flow cytometric analysis of Ki-67 expression. Apoptosis was assessed by flow cytometry (cell cycle analysis and annexin V staining) and determination of caspase-3 activity.
Results
HCAECs and HCASMCs treated with regular human insulin or insulin glargine did not show significant increases in DNA synthesis or Ki-67 expression. Administration of regular human insulin or insulin glargine did not modulate the extent of apoptotic events. No influence of insulin on lipoapoptotic vascular cell death could be detected.
Conclusions/interpretation
Taken together, neither regular human insulin nor insulin glargine influences growth and apoptosis of human coronary artery cells in vitro. Our data do not suggest that regular human insulin or insulin glargine promote atherosclerosis through mechanisms affecting the cellularity of human coronary arteries.
Similar content being viewed by others
Introduction
Current guidelines define HbA1c values of less than 7.0% as the therapeutic goal for type 2 diabetic patients. Due to the natural course of type 2 diabetes with its progressive loss of beta cell function, it often becomes necessary to add insulin to oral therapy to achieve better glycaemic control [1–3]. Recently, Riddle et al. [4] demonstrated that even a simple insulin regimen lowers HbA1c levels to 6.9% in type 2 diabetic patients. However, due to peripheral insulin resistance, most of the patients needed rather high insulin dosages [4, 5]. In this and other trials, the insulin analogue glargine was shown to improve glycaemic control with significantly less nocturnal hypoglycaemia than NPH insulin [2–4, 6]. Therefore, insulin and its analogue glargine are increasingly being used in type 2 diabetic patients to reach the desired HbA1c levels.
As type 2 diabetic patients as a group have extremely high cardiovascular morbidity and mortality, and specifically in the light of the increasing use of insulin glargine with its increased affinity for IGF-I receptors [7], the question of whether high concentrations of insulin may be harmful for the vascular system is again a matter of concern. The role of hyperinsulinaemia as an independent risk factor for cardiovascular disease has been debated for years. An association between increased plasma insulin and the risk of cardiovascular disease has been found in many, but not all, prospective studies (for meta-analysis see [8]). Notably, most of these studies were performed in non-diabetic patients. Currently, evidence is accumulating that insulin therapy in diabetic patients has rather beneficial effects on the cardiovascular system. It has been shown to normalise lipid abnormalities by reducing total plasma triglycerides and increasing plasma HDL-cholesterol, and also to improve endothelial function, determined by measuring forearm blood flow responses to endothelium-dependent vasodilators [5, 6, 9, 10]. Furthermore, insulin exerts anti-inflammatory effects, i.e. insulin therapy reduces levels of pro-inflammatory cytokines and C-reactive protein in critically ill patients [11–13].
The mechanisms of insulin’s actions on vascular cells are still under debate. Human arterial smooth muscle cells express both insulin and IGF-I receptors [14, 15]. Mitogenic effects of insulin in vitro, however, were only detected when insulin was present in sufficient concentrations to interact with the IGF-I receptor [16]. Analogous results were obtained in rat and porcine vascular smooth muscle cells, where low concentrations of insulin showed only little or no mitogenic activity in vitro, while higher concentrations of insulin promoted cell growth in some studies, depending on the vessel type [17–20].
Vascular endothelial cells express insulin receptors as well as IGF-I receptors [21–23]. HUVECs contain approximately 3.5–10 times more IGF-I receptor mRNA than insulin receptor mRNA [24, 25]. This is reflected by significantly more IGF-I receptors than insulin receptors (approximately 400,000/cell and 40,000/cell, respectively) [25]. Furthermore, insulin was shown to prevent HUVECs from apoptosis induced by TNF-α or angiotensin II [26].
The growing necessity to use high doses of insulin or insulin analogues in the therapy of type 2 diabetes provides the rationale to extensively study the effects of insulin and its analogues on the cardiovascular system. Therefore, we studied the effects of regular human insulin and the insulin analogue glargine on proliferation and apoptosis of human coronary artery endothelial cells (HCAECs) and human coronary artery smooth muscle cells (HCASMCs).
Materials and methods
Cell culture
HCAECs and HCASMCs were purchased from Clonetics/BioWhittaker and cultured in endothelial cell growth medium (EGM) or smooth muscle cell growth medium (SMGM) with supplements according to the provider’s instructions. Cells were obtained from healthy donors (16–56 years old), who had given their informed consent. Cells were treated with regular human insulin or insulin glargine (Aventis Pharma, Bad Soden, Germany). In some experiments, cells were incubated with NEFA. NEFA (Sigma-Aldrich, Taufkirchen, Germany) were bound to fatty-acid-free BSA as previously described [27].
Determination of [3H]thymidine incorporation
Cells were seeded in six-well plates (20,000 cells/well). After attachment overnight, cells were starved for 16 h in unsupplemented EGM/SMGM medium containing 0.5% FCS. Then, cells were treated for 20 h as indicated. [3H]Thymidine (55.5 kBq/ml) was added for the final 4 h. The dishes were rinsed twice with ice-cold PBS before 10% trichloroacetic acid was added for 20 min. After dishes were washed once with ice-cold 10% trichloroacetic acid, cells were lysed with 500 μl 0.2 mol/l NaOH/1% SDS, and the lysates were neutralised with 0.2 mol/l HCl. The incorporated radioactivity was determined by liquid scintillation counting.
Flow cytometric analysis of Ki-67 expression
Cells were grown to 50% confluence in 10 cm dishes and starved for 16 h in unsupplemented EGM/SMGM medium containing 0.5% FCS. Cells were treated for 20 h as indicated, harvested by trypsinisation, washed once with wash buffer (PBS/0.1% NaN3/1% heat-inactivated FCS) and fixed in 70% ice-cold ethanol. After at least 24 h incubation at −20°C, cells were washed with wash buffer, resuspended in wash buffer containing 0.25% Triton X-100, and incubated on ice for 5 min. Permeabilised cells were washed again and resuspended in wash buffer containing FITC-conjugated anti-Ki-67 antibody (BD Biosciences Pharmingen, San Diego, CA, USA). Cells were incubated for 30 min at room temperature, washed again and then subjected to flow cytometry using a Becton Dickinson FACScalibur cytometer (BD Biosciences Immunocytometry Systems, San Jose, CA, USA). Percentages of Ki-67-positive cells were calculated by CellQuest software (Becton Dickinson).
Immunoblotting
Cells were serum-starved overnight. After stimulation as indicated, cells were lysed in ice-cold lysis buffer (50 mmol/l HEPES pH7.2, 150 mmol/l NaCl, 1.5 mmol/l MgCl2, 1 mmol/l EGTA, 10% (v/v) glycerol, 1% (v/v) Triton X-100, 100 mmol/l NaF, 10 mmol/l sodium pyrophosphate, 100 μmol/l sodium orthovanadate, 1 mmol/l phenylmethylsulphonylfluoride, 10 μg/ml aprotinin). Cleared crude cell lysates (20 min at 12,000 g) were analysed on a 10% SDS polyacrylamide gel (100 μg protein per lane). Separated proteins were transferred to nitrocellulose membranes by semi-dry electroblotting (transfer buffer: 48 mmol/l Tris–HCl pH7.5, 0.0004% (w/v) SDS, 39 mmol/l glycine, 20% (v/v) methanol). Equal loading was confirmed by Ponceau S staining. After transfer, the membranes were blocked with NET buffer (150 mmol/l NaCl, 5 mmol/l EDTA, 50 mmol/l Tris, 0.05% (v/v) Triton X-100 and 0.25% (w/v) gelatine, pH7.4) for 1 h. Subsequently, filters were incubated with the primary antibody (anti-Phospho-Akt; Cell Signaling, New England Biolabs, Frankfurt/Main, Germany) overnight at 4°C. The membranes were washed four times with NET buffer before incubating with horseradish-peroxidase-conjugated anti-rabbit IgG for 1 h at room temperature. Immunocomplexes were visualised by enhanced chemiluminescence.
Cell cycle analysis
Confluent cells were treated as indicated. Detached cells were harvested from the supernatant by centrifugation and added to the adherent cells harvested by trypsinisation. Cells were washed with PBS, fixed in 70% ice-cold ethanol, centrifuged and washed again with PBS. After staining with propidium iodide (50 μg/ml) diluted in PBS containing RNase A (100 μg/ml), cells were subjected to flow cytometric analysis of DNA content using the FACScalibur cytometer. Percentages of cells in the different cell cycle phases were calculated by CellQuest software.
Propidium iodide–annexin V double staining
Cells were harvested and washed as described above (cell cycle analysis). Cells were double stained with propidium iodide (1 μg/ml) and annexin V-Fluos (Roche Diagnostics) according to the manufacturer’s instructions. Stained cells were subjected to flow cytometry (FACScalibur cytometer). Percentages of necrotic, apoptotic and vital cells were calculated by CellQuest software.
Measurement of DEVD-amc-cleaving caspase activity
Cells were seeded in triplicates in 96-well plates at a density of 104 cells/well. After stimulation as indicated, the cells were incubated in lysis buffer (25 mmol/l Tris–HCl pH 8.0, 60 mmol/l NaCl, 2.5 mmol/l EDTA, 0.25% NP40) for 10 min. Then, the fluorogenic caspase-3 substrate Ac-DEVD-amc (12 μmol; BACHEM, Weil am Rhein, Germany) was added and the fluorescence determined at 15 min intervals using 360 nm excitation and 480 nm emission wavelengths (Mithras Multilabel reader LB940; Berthold Technologies, Bad Wildbad, Germany).
Statistics
Data were analysed by one-way ANOVA with Bonferroni’s post-hoc test. A p value less than 0.05 was considered statistically significant. For these tests, the statistical software SigmaStat for Windows 1.0 (Jandel, San Rafael, CA, USA) was used.
Results
To study the influence of regular human insulin and insulin glargine on proliferation of human coronary artery cells, DNA synthesis was determined by [3H]thymidine incorporation. All cells were serum-starved overnight prior to stimulation. As a positive control, serum-starved cells were incubated with growth medium containing 10% FCS. Under this condition, the [3H]thymidine incorporation rate increased approximately 2.5-fold over basal (unsupplemented basal medium containing 0.5% FCS) in both cell types (Fig. 1a). By contrast, regular human insulin and insulin glargine, at 10 nmol/l each, did not significantly increase [3H]thymidine incorporation. Since HCASMCs showed a tendency towards lower [3H]thymidine incorporation after treatment with insulin glargine, we tested a potential anti-proliferative effect of insulin glargine by dose–response studies. Neither regular human insulin nor insulin glargine significantly altered [3H]thymidine incorporation at physiological (0.1–1 nmol/l) or supraphysiological concentrations (10–100 nmol/l) (Fig. 1b).
No effect of regular human insulin or insulin glargine on [3H]thymidine incorporation. a HCAECs or HCASMCs were serum-starved for 16 h in unsupplemented basal medium containing 0.5% FCS. Cells were then stimulated with growth medium containing 10% FCS (as a positive control), basal medium or basal medium containing 10 nmol/l regular insulin or insulin glargine. [3H]Thymidine incorporation was determined as described in Materials and methods. b HCASMCs were incubated with the indicated concentrations of regular insulin or insulin glargine and [3H]thymidine incorporation was determined as described. Data are means±SE of six independent experiments in triplicate. Open bars, basal medium; hatched bars, growth medium; black bars, regular insulin; grey bars, insulin glargine
To confirm these findings, we independently assessed proliferation by analysis of Ki-67 expression, a nuclear marker of actively cycling cells. Basal and serum-stimulated Ki-67 expression was lower in HCASMCs than in HCAECs (Table 1). Neither regular human insulin, nor insulin glargine, at 10 nmol/l each, significantly altered Ki-67 expression (Table 1).
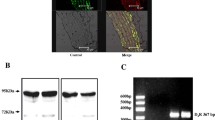
As a positive control for insulin effects in HCASMCs and HCAECs, phosphorylation of protein kinase B, a well-known downstream target of insulin signalling [26], was investigated. As shown in Fig. 2, both regular human insulin and insulin glargine phosphorylated protein kinase B in a time-dependent manner.
Regular human insulin and insulin glargine phosphorylate protein kinase B. HCAECs and HCASMCs were stimulated as indicated. Immunoblotting was performed as described in Materials and methods
Since population growth is controlled by proliferation on the one hand and cell death on the other hand, we also determined apoptosis in insulin-treated cultures and untreated controls. HCAECs and HCASMCs were incubated for 24 h at physiological and supra-physiological concentrations of regular human insulin and insulin glargine ranging from 0.1 to 10 nmol/l. Apoptotic HCAECs were determined by cell cycle analysis (quantification of sub-G1 DNA content). Neither regular human insulin nor insulin glargine significantly affected endothelial cell apoptosis (Fig. 3a).
Viability of a HCAECs or b HCASMCs is not altered by regular insulin or insulin glargine. a HCAECs were cultured for 24 h in growth medium in the absence or presence of regular insulin or insulin glargine at different concentrations. Apoptosis was determined as described in Materials and methods. Data are means±SE of three independent experiments (n=3). Hatched bar, growth medium; black bar, regular insulin; grey bar, insulin glargine. b HCASMCs were incubated with regular insulin or insulin glargine for 24 h at the indicated concentrations and percentages of necrotic and apoptotic cells were determined by propidium iodide–annexin V double staining. Data are means±SE of four independent experiments. Solid shading, apoptosis; no shading, necrosis; grey shading, late apoptosis/necrosis
In HCASMCs, propidium iodide–annexin V double staining was used to determine apoptotic and necrotic cell death. This method was chosen because HCASMCs were found to be essentially more sensitive to agent (e.g. NEFA)-induced necrotic cell death than HCAECs. As shown in Fig. 3b, incubation of HCASMCs for 24 h with different concentrations of regular human insulin and insulin glargine (0.1–10 nmol/l) did not significantly alter cell viability.
To further examine whether insulin affects NEFA-induced cell death, we co-incubated HCAECs and HCASMCs with saturated NEFA (palmitate or stearate, 1 mmol/l) and regular human insulin or insulin glargine for 24 h. Palmitate and stearate significantly induced cell death in both cell types (Fig. 4a,b). Co-incubation with regular human insulin or insulin glargine, at 10 nmol/l each, did not significantly alter NEFA-induced cell death (4a,b).
Lipoapoptosis of a HCAECs or b HCASMCs is not altered by co-incubation with regular insulin or insulin glargine. HCAECs and HCASMCs were co-incubated for 24 h with 1 mmol/l palmitate or stearate and 10 nmol/l regular insulin or insulin glargine. a For HCAECs, apoptosis was measured by determination of cells with sub-G1 DNA content as described in Materials and methods. Data are means±SE of three independent experiments (n=3). Hatched bars, growth medium; black bars, regular insulin; grey bars, insulin glargine. b For HCASMCs, percentages of necrotic and apoptotic cells were determined by propidium iodide–annexin V double staining. Data are means±SE of four independent experiments. Solid shading, apoptosis; no shading, necrosis; grey shading, late apoptosis/necrosis
Furthermore, co-incubation with regular human insulin or insulin glargine had no significant influence on activation of the pro-apoptotic caspase cascade as measured by DEVD-amc cleavage and shown for stearate in Fig. 5a,b.
Co-incubation of a HCAECs and b HCASMCs with regular insulin or insulin glargine does not prevent stearate-induced caspase activation. HCAECs and HCASMCs were co-incubated for 6 h with or without 1 mmol/l stearate and 10 or 100 nmol/l regular insulin or insulin glargine. DEVD-amc-cleaving activity was measured as described in Materials and methods. Data are means±SE of three independent experiments. Open bars, growth medium; shaded bars, stearate
Discussion
In the recent years, it has been recognised that proliferation as well as apoptosis of vascular cells plays a crucial role in the development and stability of atherosclerotic plaques [28]. Proliferation of vascular smooth muscle cells and intima–media thickening are key processes of early atherosclerosis [29], while apoptosis of endothelial or smooth muscle cells promotes coagulation by release of procoagulant microparticles [30, 31] and reduces cellularity of the atherosclerotic plaque, resulting in plaque instability and finally acute vessel occlusion [32].
Using low (0.1 nmol/l) and supraphysiological (100 nmol/l) concentrations of insulin, we mimicked the physiological as well as the extreme hyperinsulinaemic situation, the latter enabling cross-activity of insulin with the IGF-I receptor system. Despite being functionally active in HCAECs and HCASMCs as shown by phosphorylation of protein kinase B, neither regular insulin nor insulin glargine increased DNA synthesis of HCASMCs or HCAECs. This is in accord with other studies showing little or no mitogenic effect of insulin on macrovascular cells [16–20, 22].
Human vascular smooth muscle cells as well as endothelial cells are reported to express both IGF-I receptors and insulin receptors [16, 23–25]. Studies in HUVECs have shown that these endothelial cells predominantly express IGF-I receptors [24, 25]. Since insulin glargine reveals a somewhat higher (i.e. seven- to ten-fold) affinity for the IGF-I receptor than regular human insulin [7, 23], we also tested whether insulin glargine exerts mitogenic effects in HCAECs and HCASMCs. Insulin glargine, even at high concentrations, did not change the thymidine incorporation rate. This suggests that neither insulin nor insulin glargine is able to stimulate DNA synthesis in human coronary artery cells through signalling pathways dependent on insulin receptors or IGF-I-receptors.
Apoptosis of vascular cells is another central factor in the pathogenesis of atherosclerosis. Insulin was shown to prevent TNF-α-induced apoptosis in HUVECs and to protect smooth muscle cells from apoptosis induced by serum starvation or oxidative stress [26, 33, 34]. Especially IGF-I receptor stimulation seems to be important for the viability of smooth muscle cells in human coronary arteries, as smooth muscle cells obtained from coronary atherosclerotic plaques show decreased expression of IGF-I receptors and increased sensitivity to apoptosis [35–37]. We showed here that in human coronary artery cells obtained from donors without coronary artery disease neither regular human insulin nor insulin glargine changes apoptosis and viability.
In insulin-resistant and type 2 diabetic patients, insulin levels as well as plasma concentrations of NEFA are often elevated. Recently, NEFA have been identified as a trigger of apoptosis in vascular endothelial cells [38]. We therefore imitated this pathological situation by co-incubation of HCAECs and HCASMCs with insulin and NEFA. In both cell types, palmitate as well as stearate significantly induced cell death. Regular human insulin or insulin glargine neither protected cells from NEFA-induced cell death nor enhanced NEFA-induced apoptosis or necrosis. Furthermore, no effect of regular insulin or insulin glargine on NEFA-induced activation of the caspase cascade was detectable.
In summary, our data demonstrate that insulin and insulin glargine do not influence cellularity in normal human coronary artery cells. Since the coronary artery cells tested were obtained from individuals without coronary artery disease and, as mentioned above, smooth muscle cells obtained from coronary atherosclerotic plaques reveal altered expression of IGF-I receptors, we cannot rule out the possibility that cells from patients with substantial cardiovascular disease may behave differently.
Abbreviations
- EGM:
-
endothelial cell growth medium
- HCAEC:
-
human coronary artery endothelial cell
- HCASMC:
-
human coronary artery smooth muscle cell
- SMGM:
-
smooth muscle cell growth medium
References
UK Prospective Diabetes Study Group (1998) Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet 352:837–853
Fritsche A, Schweitzer MA, Haring HU (2003) Glimepiride combined with morning insulin glargine, bedtime neutral protamine hagedorn insulin, or bedtime insulin glargine in patients with type 2 diabetes. A randomized, controlled trial. Ann Intern Med 138:952–959
Yki-Jarvinen H, Dressler A, Ziemen M, HOE 901/3002 study group (2000) Less nocturnal hypoglycemia and better post-dinner glucose control with bedtime insulin glargine compared with bedtime NPH insulin during insulin combination therapy in type 2 diabetes. Diabetes Care 23:1130–1136
Riddle MC, Rosenstock J, Gerich J (2003) The treat-to-target trial: randomized addition of glargine or human NPH insulin to oral therapy of type 2 diabetic patients. Diabetes Care 26:3080–3086
Vehkavaara S, Makimattila S, Schlenzka A, Vakkilainen J, Westerbacka J, Yki-Jarvinen H (2000) Insulin therapy improves endothelial function in type 2 diabetes. Arterioscler Thromb Vasc Biol 20:545–550
Vehkavaara S, Yki-Jarvinen H (2004) 3.5 years of insulin therapy with insulin glargine improves in vivo endothelial function in type 2 diabetes. Arterioscler Thromb Vasc Biol 24:325–330
Kurtzhals P, Schaffer L, Sorensen A, Kristensen C, Jonassen I, Schmid C, Trub T (2000) Correlations of receptor binding and metabolic and mitogenic potencies of insulin analogs designed for clinical use. Diabetes 49:999–1005
Diabetologia (2004) Plasma insulin and cardiovascular mortality in non-diabetic European men and women: a meta-analysis of data from eleven prospective studies. Diabetologia 47:1245–1256
Caixas A, Ordonez-Llanos J, de Leiva A, Payes A, Homs R, Perez A (1997) Optimization of glycemic control by insulin therapy decreases the proportion of small dense LDL particles in diabetic patients. Diabetes 46:1207–1213
Taskinen MR, Kuusi T, Helve E, Nikkila EA, Yki-Jarvinen H (1988) Insulin therapy induces antiatherogenic changes of serum lipoproteins in noninsulin-dependent diabetes. Arteriosclerosis 8:168–177
Stentz FB, Umpierrez GE, Cuervo R, Kitabchi AE (2004) Proinflammatory cytokines, markers of cardiovascular risks, oxidative stress, and lipid peroxidation in patients with hyperglycemic crises. Diabetes 53:2079–2086
Dandona P, Aljada A, Mohanty P (2002) The anti-inflammatory and potential anti-atherogenic effect of insulin: a new paradigm. Diabetologia 45:924–930
Hansen TK, Thiel S, Wouters PJ, Christiansen JS, Van den Berghe G (2003) Intensive insulin therapy exerts antiinflammatory effects in critically ill patients and counteracts the adverse effect of low mannose-binding lectin levels. J Clin Endocrinol Metab 88:1082–1088
Banskota NK, Taub R, Zellner K, Olsen P, King GL (1989) Characterization of induction of protooncogene c-myc and cellular growth in human vascular smooth muscle cells by insulin and IGF-I. Diabetes 38:123–129
Pfeifle B, Ditschuneit HH, Ditschuneit H (1982) Binding and biological actions of insulin-like growth factors on human arterial smooth muscle cells. Horm Metab Res 14:409–414
Avena R, Mitchell ME, Carmody B, Arora S, Neville RF, Sidaway AN (1999) Insulin-like growth factor-1 receptors mediate infragenicular vascular smooth muscle cell proliferation in response to glucose and insulin not by insulin receptors. Am J Surg 178:156–161
Yamada H, Tsushima T, Murakami H, Uchigata Y, Iwamoto Y (2002) Potentiation of mitogenic activity of platelet-derived growth factor by physiological concentrations of insulin via the MAP kinase cascade in rat A10 vascular smooth muscle cells. Int J Exp Diabetes Res 3:131–144
Cruzado M, Risler N, Castro C, Ortiz A, Ruttler ME (1998) Proliferative effect of insulin on cultured smooth muscle cells from rat mesenteric resistance vessels. Am J Hypertens 11:54–58
Kamide K, Hori MT, Zhu JH et al (2000) Insulin and insulin-like growth factor-I promotes angiotensinogen production and growth in vascular smooth muscle cells. J Hypertens 18:1051–1056
Agazie YM, Bagot JC, Trickey E, Halenda SP, Wilden PA (2001) Molecular mechanisms of ATP and insulin synergistic stimulation of coronary artery smooth muscle growth. Am J Physiol Heart Circ Physiol 280:H795–H801
King GL, Goodman AD, Buzney S, Moses A, Kahn CR (1985) Receptors and growth-promoting effects of insulin and insulin-like growth factors on cells from bovine retinal capillaries and aorta. J Clin Invest 75:1028–1036
King GL, Buzney SM, Kahn CR et al (1983) Differential responsiveness to insulin of endothelial and support cells from micro- and macrovessels. J Clin Invest 71:974–979
Chisalita SI, Arnqvist HJ (2004) Insulin-like growth factor I receptors are more abundant than insulin receptors in human micro- and macrovascular endothelial cells. Am J Physiol Endocrinol Metab 286:E896–E901
Nitert MD, Chisalita SI, Olsson K, Bornfeldt KE, Arnqvist HJ (2005) IGF-I/insulin hybrid receptors in human endothelial cells. Mol Cell Endocrinol 229:31–37
Zeng G, Quon MJ (1996) Insulin-stimulated production of nitric oxide is inhibited by wortmannin. Direct measurement in vascular endothelial cells. J Clin Invest 98:894–898
Hermann C, Assmus B, Urbich C, Zeiher AM, Dimmeler S (2000) Insulin-mediated stimulation of protein kinase Akt: a potent survival signaling cascade for endothelial cells. Arterioscler Thromb Vasc Biol 20:402–409
Eitel K, Staiger H, Rieger J et al (2003) Protein kinase C delta activation and translocation to the nucleus are required for fatty acid-induced apoptosis of insulin-secreting cells. Diabetes 52:991–997
Geng YJ, Libby P (2002) Progression of atheroma: a struggle between death and procreation. Arterioscler Thromb Vasc Biol 22:1370–1380
Dzau VJ, Braun-Dullaeus RC, Sedding DG (2002) Vascular proliferation and atherosclerosis: new perspectives and therapeutic strategies. Nat Med 8:1249–1256
Bombeli T, Karsan A, Tait JF, Harlan JM (1997) Apoptotic vascular endothelial cells become procoagulant. Blood 89:2429–2442
Mallat Z, Hugel B, Ohan J, Leseche G, Freyssinet JM, Tedgui A (1999) Shed membrane microparticles with procoagulant potential in human atherosclerotic plaques: a role for apoptosis in plaque thrombogenicity. Circulation 99:348–353
Libby P (1995) Molecular bases of the acute coronary syndromes. Circulation 91:2844–2850
Jamali R, Bao M, Arnqvist HJ (2003) IGF-I but not insulin inhibits apoptosis at a low concentration in vascular smooth muscle cells. J Endocrinol 179:267–274
Goetze S, Blaschke F, Stawowy P et al (2001) TNFalpha inhibits insulin’s antiapoptotic signaling in vascular smooth muscle cells. Biochem Biophys Res Commun 287:662–670
Bennett MR, Evan GI, Schwartz SM (1995) Apoptosis of human vascular smooth muscle cells derived from normal vessels and coronary atherosclerotic plaques. J Clin Invest 95:2266–2274
Patel VA, Zhang QJ, Siddle K et al (2001) Defect in insulin-like growth factor-1 survival mechanism in atherosclerotic plaque-derived vascular smooth muscle cells is mediated by reduced surface binding and signaling. Circ Res 88:895–902
Okura Y, Brink M, Zahid AA, Anwar A, Delafontaine P (2001) Decreased expression of insulin-like growth factor-1 and apoptosis of vascular smooth muscle cells in human atherosclerotic plaque. J Mol Cell Cardiol 33:1777–1789
Artwohl M, Roden M, Waldhausl W, Freudenthaler A, Baumgartner-Parzer SM (2004) Free fatty acids trigger apoptosis and inhibit cell cycle progression in human vascular endothelial cells. FASEB J 18:146–148
Acknowledgements
We thank C. Haas for excellent technical assistance. This work was supported by DFG-KF0114, Kennedy-Allee 40, Bonn, Germany.
Duality of Interest
H.-U. Häring received consulting fees for participating on scientific boards of Aventis Pharma Deutschland, and has received grant support. M. Kellerer has received honoraria for speaking engagements from Aventis Pharma Deutschland, and was supported by a grant from Aventis Pharma. M.A. Schweitzer was employed by Aventis Pharma Germany until February 2005. He has still stock options in the company but no shares.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Staiger, K., Staiger, H., Schweitzer, M.A. et al. Insulin and its analogue glargine do not affect viability and proliferation of human coronary artery endothelial and smooth muscle cells. Diabetologia 48, 1898–1905 (2005). https://doi.org/10.1007/s00125-005-1874-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-005-1874-4