Abstract
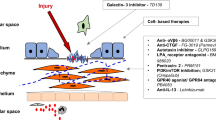
Idiopathic pulmonary fibrosis (IPF) is a chronic irreversible interstitial lung disease characterized by a progressive decline in lung function. The etiology of IPF is unknown, which poses a significant challenge to the treatment of IPF. Recent studies have identified a strong association between lipid metabolism and the development of IPF. Qualitative and quantitative analysis of small molecule metabolites using lipidomics reveals that lipid metabolic reprogramming plays a role in the pathogenesis of IPF. Lipids such as fatty acids, cholesterol, arachidonic acid metabolites, and phospholipids are involved in the onset and progression of IPF by inducing endoplasmic reticulum stress, promoting cell apoptosis, and enhancing the expression of pro-fibrotic biomarkers. Therefore, targeting lipid metabolism can provide a promising therapeutic strategy for pulmonary fibrosis. This review focuses on lipid metabolism in the pathogenesis of pulmonary fibrosis.

Similar content being viewed by others
Data availability
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
References
Ma H, Wu X, Li Y, Xia Y (2022) Research progress in the molecular mechanisms, therapeutic targets, and drug development of idiopathic pulmonary fibrosis. Front Pharmacol 13(963):054. https://doi.org/10.3389/fphar.2022.963054
Maher TM, Bendstrup E, Dron L, Langley J, Smith G, Khalid JM, Patel H, Kreuter M (2021) Global incidence and prevalence of idiopathic pulmonary fibrosis. Respir Res 22(1):197. https://doi.org/10.1186/s12931-021-01791-z
Lederer DJ, Martinez FJ (2018) Idiopathic pulmonary fibrosis. N Engl J Med 378(19):1811–1823. https://doi.org/10.1056/NEJMra1705751
Zheng Q, Cox IA, Campbell JA, Xia Q, Otahal P, de Graaff B, Corte TJ, Teoh AKY, Walters EH, Palmer AJ (2022) Mortality and survival in idiopathic pulmonary fibrosis: A systematic review and meta-analysis. ERJ Open Res 8(1):00591–02021. https://doi.org/10.1183/23120541.00591-2021
Fahy E, Cotter D, Sud M (1811) Subramaniam S (2011) Lipid classification, structures and tools. Biochim Biophys Acta 11:637–47. https://doi.org/10.1016/j.bbalip.2011.06.009
Agudelo CW, Samaha G, Garcia-Arcos I (2020) Alveolar lipids in pulmonary disease. a review. Lipids Health Dis 19(1):122. https://doi.org/10.1186/s12944-020-01278-8
Beike L, Wrede C, Hegermann J, Lopez-Rodriguez E, Kloth C, Gauldie J, Kolb M, Maus UA, Ochs M, Knudsen L (2019) Surfactant dysfunction and alveolar collapse are linked with fibrotic septal wall remodeling in the tgf-beta1-induced mouse model of pulmonary fibrosis. Lab Invest 99(6):830–852. https://doi.org/10.1038/s41374-019-0189-x
Mai C, Verleden SE, McDonough JE, Willems S, De Wever W, Coolen J, Dubbeldam A, Van Raemdonck DE, Verbeken EK, Verleden GM et al (2017) Thin-section ct features of idiopathic pulmonary fibrosis correlated with micro-ct and histologic analysis. Radiology 283(1):252–263. https://doi.org/10.1148/radiol.2016152362
Xu Y, Zhang M, Wang Y, Kadambi P, Dave V, Lu LJ, Whitsett JA (2010) A systems approach to mapping transcriptional networks controlling surfactant homeostasis. BMC Genomics 11:451. https://doi.org/10.1186/1471-2164-11-451
Bujak R, Struck-Lewicka W, Markuszewski MJ, Kaliszan R (2015) Metabolomics for laboratory diagnostics. J Pharm Biomed Anal 113:108–20. https://doi.org/10.1016/j.jpba.2014.12.017
Yan F, Wen Z, Wang R, Luo W, Du Y, Wang W, Chen X (2017) Identification of the lipid biomarkers from plasma in idiopathic pulmonary fibrosis by lipidomics. BMC Pulm Med 17(1):174. https://doi.org/10.1186/s12890-017-0513-4
Fahy E, Subramaniam S, Brown HA, Glass CK, Merrill JAH, Murphy RC, Raetz CR, Russell DW, Seyama Y, Shaw W et al (2005) A comprehensive classification system for lipids. J Lipid Res 46(5):839–61. https://doi.org/10.1194/jlr.E400004-JLR200
Agostoni C, Bruzzese MG (1992) fatty acids: their biochemical and functional classification. La Pediatria Medica E Chirurgica : Medical and Surgical Pediatrics 14(5):473–479
Bach D, Wachtel E (2003) Phospholipid/cholesterol model membranes: formation of cholesterol crystallites. Biochim Biophys Acta 1610(2):187–97. https://doi.org/10.1016/s0005-2736(03)00017-8
Gault CR, Obeid LM, Hannun YA (2010) An overview of sphingolipid metabolism: from synthesis to breakdown. Adv Exp Med Biol 688
Eibl H (1980) Synthesis of glycerophospholipids. Chem Phys Lipids 26(4):405–429
Flowers MT, Ntambi JM (2008) Role of stearoyl-coenzyme a desaturase in regulating lipid metabolism. Curr Opin Lipidol 19(3):248–256. https://doi.org/10.1097/MOL.0b013e3282f9b54d
Wakil SJ (1989) Fatty acid synthase, a proficient multifunctional enzyme. Biochemistry 28(11):4523–4530
Jung MY, Kang JH, Hernandez DM, Yin X, Andrianifahanana M, Wang Y, Gonzalez-Guerrico A, Limper AH, Lupu R, Leof EB (2018) Fatty acid synthase is required for profibrotic tgf-beta signaling. FASEB J 32(7):3803–3815. https://doi.org/10.1096/fj.201701187R
Burman A, Tanjore H, Blackwell TS (2018) Endoplasmic reticulum stress in pulmonary fibrosis. Matrix Biol 68–69:355–365. https://doi.org/10.1016/j.matbio.2018.03.015
Romero F, Hong X, Shah D, Kallen CB, Rosas I, Guo Z, Schriner D, Barta J, Shaghaghi H, Hoek JB et al (2018) Lipid synthesis is required to resolve endoplasmic reticulum stress and limit fibrotic responses in the lung. Am J Respir Cell Mol Biol 59(2):225–236. https://doi.org/10.1165/rcmb.2017-0340OC
Chu SG, Villalba JA, Liang X, Xiong K, Tsoyi K, Ith B, Ayaub EA, Tatituri RV, Byers DE, Hsu FF et al (2019) Palmitic acid-rich high-fat diet exacerbates experimental pulmonary fibrosis by modulating endoplasmic reticulum stress. Am J Respir Cell Mol Biol 61(6):737–746. https://doi.org/10.1165/rcmb.2018-0324OC
Kim HS, Yoo HJ, Lee KM, Song HE, Kim SJ, Lee JO, Hwang JJ, Song JW (2021) Stearic acid attenuates profibrotic signalling in idiopathic pulmonary fibrosis. Respirology 26(3):255–263. https://doi.org/10.1111/resp.13949
Sunaga H, Matsui H, Ueno M, Maeno T, Iso T, Syamsunarno MR, Anjo S, Matsuzaka T, Shimano H, Yokoyama T et al (2013) Deranged fatty acid composition causes pulmonary fibrosis in elovl6-deficient mice. Nat Commun 4:2563. https://doi.org/10.1038/ncomms3563
Abidi A, Kourda N, Feki M, Ben Khamsa S (2020) Protective effect of tunisian flaxseed oil against bleomycin-induced pulmonary fibrosis in rats. Nutr Cancer 72(2):226–238. https://doi.org/10.1080/01635581.2019.1622741
Janssen CI, Kiliaan AJ (2014) Long-chain polyunsaturated fatty acids (lcpufa) from genesis to senescence: the influence of lcpufa on neural development, aging, and neurodegeneration. Prog Lipid Res 53:1–17. https://doi.org/10.1016/j.plipres.2013.10.002
Yamaguchi A, Botta E, Holinstat M (2022) Eicosanoids in inflammation in the blood and the vessel. Front Pharmacol 13(997):403. https://doi.org/10.3389/fphar.2022.997403
Charbeneau RP, Peters-Golden M (2005) Eicosanoids: mediators and therapeutic targets in fibrotic lung disease. Clin Sci (Lond) 108(6):479–491
Cheng H, Huang H, Guo Z, Chang Y, Li Z (2021) Role of prostaglandin e2 in tissue repair and regeneration. Theranostics 11(18):8836–8854. https://doi.org/10.7150/thno.63396
Gabasa M, Royo D, Molina-Molina M, Roca-Ferrer J, Pujols L, Picado C, Xaubet A, Pereda J (2013) Lung myofibroblasts are characterized by down-regulated cyclooxygenase-2 and its main metabolite, prostaglandin e2. PloS One 8(6):e65445. https://doi.org/10.1371/journal.pone.0065445
Dackor RT, Cheng J, Voltz JW, Card JW, Ferguson CD, Garrett RC, Bradbury JA, DeGraff LM, Lih FB, Tomer KB et al (2011) Prostaglandin e2 protects murine lungs from bleomycin-induced pulmonary fibrosis and lung dysfunction. Am J Physiol Lung Cell Mol Physiol 301(5):L645–L655. https://doi.org/10.1152/ajplung.00176.2011
Zhao J, Shu B, Chen L, Tang J, Zhang L, Xie J, Liu X, Xu Y, Qi S (2016) Prostaglandin e2 inhibits collagen synthesis in dermal fibroblasts and prevents hypertrophic scar formation in vivo. Exp Dermatol 25(8):604–10. https://doi.org/10.1111/exd.13014
Mukherjee S, Sheng W, Michkov A, Sriarm K, Sun R, Dvorkin-Gheva A, Insel PA, Janssen LJ (2019) Prostaglandin e inhibits profibrotic function of human pulmonary fibroblasts by disrupting ca signaling. Am J Physiol Lung Cell Mol Physiol 316(5):L810–L821. https://doi.org/10.1152/ajplung.00403.2018
Thomas PE, Peters-Golden M, White ES, Thannickal VJ, Moore BB (2007) Pge(2) inhibition of tgf-beta1-induced myofibroblast differentiation is smad-independent but involves cell shape and adhesion-dependent signaling. Am J Physiol Lung Cell Mol Physiol 293(2):L417-28. https://doi.org/10.1152/ajplung.00489.2006
Bärnthaler T, Theiler A, Zabini D, Trautmann S, Stacher-Priehse E, Lanz I, Klepetko W, Sinn K, Flick H, Scheidl S et al (2020) Inhibiting eicosanoid degradation exerts antifibrotic effects in a pulmonary fibrosis mouse model and human tissue. J Allergy Clin Immunol 145(3):818–833. https://doi.org/10.1016/j.jaci.2019.11.032
Zannikou M, Barbayianni I, Fanidis D, Grigorakaki T, Vlachopoulou E, Konstantopoulos D, Fousteri M, Nikitopoulou I, Kotanidou A, Kaffe E et al (2021) Map3k8 regulates cox-2-mediated prostaglandin e2 production in the lung and suppresses pulmonary inflammation and fibrosis. J Immunol 206(3):607–620. https://doi.org/10.4049/jimmunol.2000862
Li JZ, Li ZH, Kang J, Hou XM, Yu RJ (2004) [change of prostaglandin e2 and interleukin-12, interleukin-13 in the bronchoalveolar lavage fluid and the serum of the patients with idiopathic pulmonary fibrosis]. Zhonghua Jie He He Hu Xi Za Zhi = Zhonghua Jiehe He Huxi Zazhi = Chinese Journal of Tuberculosis and Respiratory Diseases 27(6):378–380
Basu S (2010) Bioactive eicosanoids: role of prostaglandin f(2alpha) and f(2)-isoprostanes in inflammation and oxidative stress related pathology. Mol Cells 30(5):383–91. https://doi.org/10.1007/s10059-010-0157-1
Oga T, Matsuoka T, Yao C, Nonomura K, Kitaoka S, Sakata D, Kita Y, Tanizawa K, Taguchi Y, Chin K et al (2009) Prostaglandin f(2alpha) receptor signaling facilitates bleomycin-induced pulmonary fibrosis independently of transforming growth factor-beta. Nat Med 15(12):1426–1430. https://doi.org/10.1038/nm.2066
Beck H, Thaler T, Meibom D, Meininghaus M, Jorissen H, Dietz L, Terjung C, Bairlein M, von Buhler CJ, Anlauf S et al (2020) Potent and selective human prostaglandin f (fp) receptor antagonist (bay-6672) for the treatment of idiopathic pulmonary fibrosis (ipf). J Med Chem 63(20):11639–11662. https://doi.org/10.1021/acs.jmedchem.0c00834
Aihara K, Handa T, Oga T, Watanabe K, Tanizawa K, Ikezoe K, Taguchi Y, Sato H, Chin K, Nagai S, et al (2013) Clinical relevance of plasma prostaglandin f2alpha metabolite concentrations in patients with idiopathic pulmonary fibrosis. PLoS One 8(6):e66,017. https://doi.org/10.1371/journal.pone.0066017
Del Pozo R, Hernandez Gonzalez I, Escribano-Subias P (2017) The prostacyclin pathway in pulmonary arterial hypertension: a clinical review. Expert Rev Respir Med 11(6):491–503. https://doi.org/10.1080/17476348.2017.1317599
Sandig H, Pease JE, Sabroe I (2007) Contrary prostaglandins: the opposing roles of pgd2 and its metabolites in leukocyte function. J Leukoc Biol 81(2):372–382
Cruz-Gervis R, Stecenko AA, Dworski R, Lane KB, Loyd JE, Pierson R, King G, Brigham KL (2002) Altered prostanoid production by fibroblasts cultured from the lungs of human subjects with idiopathic pulmonary fibrosis. Respir Res 3:17
Murakami S, Nagaya N, Itoh T, Kataoka M, Iwase T, Horio T, Miyahara Y, Sakai Y, Kangawa K, Kimura H (2006) Prostacyclin agonist with thromboxane synthase inhibitory activity (ono-1301) attenuates bleomycin-induced pulmonary fibrosis in mice. Am J Physiol Lung Cell Mol Physiol 290(1):L59–L65
Roberts MJ, May LT, Keen AC, Liu B, Lam T, Charlton SJ, Rosethorne EM, Halls ML (2021) Inhibition of the proliferation of human lung fibroblasts by prostacyclin receptor agonists is linked to a sustained camp signal in the nucleus. Front Pharmacol 12(669):227. https://doi.org/10.3389/fphar.2021.669227
Roberts MJ, Broome RE, Kent TC, Charlton SJ, Rosethorne EM (2018) The inhibition of human lung fibroblast proliferation and differentiation by gs-coupled receptors is not predicted by the magnitude of camp response. Respir Res 19(1):56. https://doi.org/10.1186/s12931-018-0759-2
Kolb M, Orfanos SE, Lambers C, Flaherty K, Masters A, Lancaster L, Silverstein A, Nathan SD (2022) The antifibrotic effects of inhaled treprostinil: An emerging option for ild. Adv Ther 39(9):3881–3895. https://doi.org/10.1007/s12325-022-02229-8
Nathan SD, Waxman A, Rajagopal S, Case A, Johri S, DuBrock H, De La Zerda DJ, Sahay S, King C, Melendres-Groves L et al (2021) Inhaled treprostinil and forced vital capacity in patients with interstitial lung disease and associated pulmonary hypertension: a post-hoc analysis of the increase study. Lancet Respir Med 9(11):1266–1274. https://doi.org/10.1016/S2213-2600(21)00165-X
Ayabe S, Kida T, Hori M, Ozaki H, Murata T (2013) Prostaglandin d2 inhibits collagen secretion from lung fibroblasts by activating the dp receptor. J Pharmacol Sci 121(4):312–317
Wiley CD, Brumwell AN, Davis SS, Jackson JR, Valdovinos A, Calhoun C, Alimirah F, Castellanos CA, Ruan R, Wei Y, et al (2019) Secretion of leukotrienes by senescent lung fibroblasts promotes pulmonary fibrosis. JCI Insight 4(24):e130056. https://doi.org/10.1172/jci.insight.130056
Failla M, Genovese T, Mazzon E, Gili E, Muià C, Sortino M, Crimi N, Caputi AP, Cuzzocrea S, Vancheri C, (2006) Pharmacological inhibition of leukotrienes in an animal model of bleomycin-induced acute lung injury. Respir Res 7:137
Lu W, Yao X, Ouyang P, Dong N, Wu D, Jiang X, Wu Z, Zhang C, Xu Z, Tang Y et al (2017) Drug repurposing of histone deacetylase inhibitors that alleviate neutrophilic inflammation in acute lung injury and idiopathic pulmonary fibrosis via inhibiting leukotriene a4 hydrolase and blocking ltb4 biosynthesis. J Med Chem 60(5):1817–1828. https://doi.org/10.1021/acs.jmedchem.6b01507
Li X, Xie M, Lu C, Mao J, Cao Y, Yang Y, Wei Y, Liu X, Cao S, Song Y et al (2020) Design and synthesis of leukotriene a4 hydrolase inhibitors to alleviate idiopathic pulmonary fibrosis and acute lung injury. Eur J Med Chem 203(112):614. https://doi.org/10.1016/j.ejmech.2020.112614
Izumo T, Kondo M, Nagai A (2009) Effects of a leukotriene b4 receptor antagonist on bleomycin-induced pulmonary fibrosis. Eur Respir J 34(6):1444–1451. https://doi.org/10.1183/09031936.00143708
Wilborn J, Bailie M, Coffey M, Burdick M, Strieter R, Peters-Golden M (1996) Constitutive activation of 5-lipoxygenase in the lungs of patients with idiopathic pulmonary fibrosis. J Clin Invest 97(8):1827–1836
Henderson WR, Tang LO, Chu SJ, Tsao SM, Chiang GKS, Jones F, Jonas M, Pae C, Wang H, Chi EY (2002) A role for cysteinyl leukotrienes in airway remodeling in a mouse asthma model. Am J Respir Crit Care Med 165(1):108–116
Izumo T, Kondo M, Nagai A (2007) Cysteinyl-leukotriene 1 receptor antagonist attenuates bleomycin-induced pulmonary fibrosis in mice. Life Sci 80(20):1882–6. https://doi.org/10.1016/j.lfs.2007.02.038
Shaker OG, Sourour DA (2011) Effect of leukotriene receptor antagonists on lung fibrosis in rats. J Appl Toxicol 31(7):678–84. https://doi.org/10.1002/jat.1625
Yvan-Charvet L, Bonacina F, Guinamard RR, Norata GD (2019) Immunometabolic function of cholesterol in cardiovascular disease and beyond. Cardiovasc Res 115(9):1393–1407. https://doi.org/10.1093/cvr/cvz127
Fireman E, Spitzer S, Grief J, Kivity S, Topilsky M (1996) Cholesterol crystals in bal fluid from patients with idiopathic pulmonary fibrosis. Respir Med 90(6):361–363
Romero F, Shah D, Duong M, Penn RB, Fessler MB, Madenspacher J, Stafstrom W, Kavuru M, Lu B, Kallen CB et al (2015) A pneumocyte-macrophage paracrine lipid axis drives the lung toward fibrosis. Am J Respir Cell Mol Biol 53(1):74–86. https://doi.org/10.1165/rcmb.2014-0343OC
Angelidis I, Simon LM, Fernandez IE, Strunz M, Mayr CH, Greiffo FR, Tsitsiridis G, Ansari M, Graf E, Strom TM et al (2019) An atlas of the aging lung mapped by single cell transcriptomics and deep tissue proteomics. Nat Commun 10(1):963. https://doi.org/10.1038/s41467-019-08831-9
Lund EG, Kerr TA, Sakai J, Li WP, Russell DW (1998) cdna cloning of mouse and human cholesterol 25-hydroxylases, polytopic membrane proteins that synthesize a potent oxysterol regulator of lipid metabolism. J Biol Chem 273(51):34,316–27. https://doi.org/10.1074/jbc.273.51.34316
Ichikawa T, Sugiura H, Koarai A, Kikuchi T, Hiramatsu M, Kawabata H, Akamatsu K, Hirano T, Nakanishi M, Matsunaga K et al (2013) 25-hydroxycholesterol promotes fibroblast-mediated tissue remodeling through nf-kappab dependent pathway. Exp Cell Res 319(8):1176–86. https://doi.org/10.1016/j.yexcr.2013.02.014
Hachisu Y, Murata K, Takei K, Tsuchiya T, Tsurumaki H, Koga Y, Horie T, Takise A, Hisada T (2019) Possible serological markers to predict mortality in acute exacerbation of idiopathic pulmonary fibrosis. Medicina (Kaunas) 55(5):132. https://doi.org/10.3390/medicina55050132
Illingworth DR (1993) Lipoprotein metabolism. Am J Kidney Dis 22(1):90–97
Kovanen PT (1987) Regulation of plasma cholesterol by hepatic low-density lipoprotein receptors. Am Heart J 113(2 Pt 2):464–469
Shi X, Chen Y, Liu Q, Mei X, Liu J, Tang Y, Luo R, Sun D, Ma Y, Wu W et al (2022) Ldlr dysfunction induces ldl accumulation and promotes pulmonary fibrosis. Clin Transl Med 12(1):e711. https://doi.org/10.1002/ctm2.711
Aihara K, Handa T, Nagai S, Tanizawa K, Ikezoe K, Watanabe K, Chihara Y, Harada Y, Yoshimura C, Oga T et al (2013) Impaired endothelium-dependent vasodilator response in patients with pulmonary fibrosis. Respir Med 107(2):269–75. https://doi.org/10.1016/j.rmed.2012.10.005
Lennernäs H, Fager G (1997) Pharmacodynamics and pharmacokinetics of the hmg-coa reductase inhibitors. similarities and differences. Clin Pharmacokinet 32(5):403–425
Barale C, Melchionda E, Morotti A, Russo I (2021) Pcsk9 biology and its role in atherothrombosis. Int J Mol Sci 22(11):5880. https://doi.org/10.3390/ijms22115880
Kreuter M, Bonella F, Maher TM, Costabel U, Spagnolo P, Weycker D, Kirchgaessler KU, Kolb M (2017) Effect of statins on disease-related outcomes in patients with idiopathic pulmonary fibrosis. Thorax 72(2):148–153. https://doi.org/10.1136/thoraxjnl-2016-208819
Kreuter M, Costabel U, Richeldi L, Cottin V, Wijsenbeek M, Bonella F, Bendstrup E, Maher TM, Wachtlin D, Stowasser S et al (2018) Statin therapy and outcomes in trials of nintedanib in idiopathic pulmonary fibrosis. Respiration 95(5):317–326. https://doi.org/10.1159/000486286
Yildirim M, Kayalar O, Atahan E, Oztay F (2022) Atorvastatin attenuates pulmonary fibrosis in mice and human lung fibroblasts, by the regulation of myofibroblast differentiation and apoptosis. J Biochem Mol Toxicol 36(7):e23074. https://doi.org/10.1002/jbt.23074
Santos DM, Pantano L, Pronzati G, Grasberger P, Probst CK, Black KE, Spinney JJ, Hariri LP, Nichols R, Lin Y et al (2020) Screening for yap inhibitors identifies statins as modulators of fibrosis. Am J Respir Cell Mol Biol 62(4):479–492. https://doi.org/10.1165/rcmb.2019-0296OC
Barochia AV, Kaler M, Weir N, Gordon EM, Figueroa DM, Yao X, Lemma WoldeHanna M, Sampson M, Remaley AT, Grant G, et al (2021) Serum levels of small hdl particles are negatively correlated with death or lung transplantation in an observational study of idiopathic pulmonary fibrosis. Eur Respir J 58(6):2004053. https://doi.org/10.1183/13993003.04053-2020
Podolanczuk AJ, Raghu G, Tsai MY, Kawut SM, Peterson E, Sonti R, Rabinowitz D, Johnson C, Barr RG, Hinckley Stukovsky K et al (2017) Cholesterol, lipoproteins and subclinical interstitial lung disease: the mesa study. Thorax 72(5):472–474. https://doi.org/10.1136/thoraxjnl-2016-209568
Kim TH, Lee YH, Kim KH, Lee SH, Cha JY, Shin EK, Jung S, Jang AS, Park SW, Uh ST et al (2010) Role of lung apolipoprotein a-i in idiopathic pulmonary fibrosis: antiinflammatory and antifibrotic effect on experimental lung injury and fibrosis. Am J Respir Crit Care Med 182(5):633–42. https://doi.org/10.1164/rccm.200905-0659OC
Lee E, Lee EJ, Kim H, Jang A, Koh E, Uh ST, Kim Y, Park SW, Park CS (2013) Overexpression of apolipoprotein a1 in the lung abrogates fibrosis in experimental silicosis. PLoS One 8(2):e55827. https://doi.org/10.1371/journal.pone.0055827
Song X, Shi Y, You J, Wang Z, Xie L, Zhang C, Xiong J (2019) D-4f, an apolipoprotein a-i mimetic, suppresses il-4 induced macrophage alternative activation and pro-fibrotic tgf-beta1 expression. Pharm Biol 57(1):470–476. https://doi.org/10.1080/13880209.2019.1640747
Yung YC, Stoddard NC, Chun J (2014) Lpa receptor signaling: pharmacology, physiology, and pathophysiology. J Lipid Res 55(7):1192–1214. https://doi.org/10.1194/jlr.R046458
Tager AM, LaCamera P, Shea BS, Campanella GS, Selman M, Zhao Z, Polosukhin V, Wain J, Karimi-Shah BA, Kim ND et al (2008) The lysophosphatidic acid receptor lpa1 links pulmonary fibrosis to lung injury by mediating fibroblast recruitment and vascular leak. Nat Med 14(1):45–54
Thannickal VJ, Horowitz JC (2006) Evolving concepts of apoptosis in idiopathic pulmonary fibrosis. Proc Am Thorac Soc 3(4):350–6. https://doi.org/10.1513/pats.200601-001TK
Funke M, Zhao Z, Xu Y, Chun J, Tager AM (2012) The lysophosphatidic acid receptor lpa1 promotes epithelial cell apoptosis after lung injury. Am J Respir Cell Mol Biol 46(3):355–64. https://doi.org/10.1165/rcmb.2010-0155OC
Nathan S, Zhang H, Andreoli M, Leopold PL, Crystal RG (2021) Creb-dependent lpa-induced signaling initiates a pro-fibrotic feedback loop between small airway basal cells and fibroblasts. Respir Res 22(1):97. https://doi.org/10.1186/s12931-021-01677-0
Palmer SM, Snyder L, Todd JL, Soule B, Christian R, Anstrom K, Luo Y, Gagnon R, Rosen G (2018) Randomized, double-blind, placebo-controlled, phase 2 trial of bms-986020, a lysophosphatidic acid receptor antagonist for the treatment of idiopathic pulmonary fibrosis. Chest 154(5):1061–1069. https://doi.org/10.1016/j.chest.2018.08.1058
Corte TJ, Lancaster L, Swigris JJ, Maher TM, Goldin JG, Palmer SM, Suda T, Ogura T, Minnich A, Zhan X, et al (2021) Phase 2 trial design of bms-986278, a lysophosphatidic acid receptor 1 (lpa) antagonist, in patients with idiopathic pulmonary fibrosis (ipf) or progressive fibrotic interstitial lung disease (pf-ild). BMJ Open Respir Res 8(1):e001026. https://doi.org/10.1136/bmjresp-2021-001026
Huang LS, Fu P, Patel P, Harijith A, Sun T, Zhao Y, Garcia JGN, Chun J, Natarajan V (2013) Lysophosphatidic acid receptor-2 deficiency confers protection against bleomycin-induced lung injury and fibrosis in mice. Am J Respir Cell Mol Biol 49(6):912–922. https://doi.org/10.1165/rcmb.2013-0070OC
Cartier A, Hla T (2019) Sphingosine 1-phosphate: Lipid signaling in pathology and therapy. Science 366(6463):eaar5551. https://doi.org/10.1126/science.aar5551
Shea BS, Tager AM (2012) Sphingolipid regulation of tissue fibrosis. Open Rheumatol J 6:123–129. https://doi.org/10.2174/1874312901206010123
Huang LS, Sudhadevi T, Fu P, Punathil-Kannan PK, Ebenezer DL, Ramchandran R, Putherickal V, Cheresh P, Zhou G, Ha AW et al (2020) Sphingosine kinase 1/s1p signaling contributes to pulmonary fibrosis by activating hippo/yap pathway and mitochondrial reactive oxygen species in lung fibroblasts. Int J Mol Sci 21(6):2064. https://doi.org/10.3390/ijms21062064
Milara J, Navarro R, Juan G, Peiro T, Serrano A, Ramon M, Morcillo E, Cortijo J (2012) Sphingosine-1-phosphate is increased in patients with idiopathic pulmonary fibrosis and mediates epithelial to mesenchymal transition. Thorax 67(2):147–56. https://doi.org/10.1136/thoraxjnl-2011-200026
Huang LS, Berdyshev E, Mathew B, Fu P, Gorshkova IA, He D, Ma W, Noth I, Ma SF, Pendyala S et al (2013) Targeting sphingosine kinase 1 attenuates bleomycin-induced pulmonary fibrosis. FASEB J 27(4):1749–1760. https://doi.org/10.1096/fj.12-219634
Sobel K, Menyhart K, Killer N, Renault B, Bauer Y, Studer R, Steiner B, Bolli MH, Nayler O, Gatfield J (2013) Sphingosine 1-phosphate (s1p) receptor agonists mediate pro-fibrotic responses in normal human lung fibroblasts via s1p2 and s1p3 receptors and smad-independent signaling. J Biol Chem 288(21):14839–51. https://doi.org/10.1074/jbc.M112.426726
Kono Y, Nishiuma T, Nishimura Y, Kotani Y, Okada T, Nakamura S, Yokoyama M (2007) Sphingosine kinase 1 regulates differentiation of human and mouse lung fibroblasts mediated by tgf-beta1. Am J Respir Cell Mol Biol 37(4):395–404. https://doi.org/10.1165/rcmb.2007-0065OC
Knipe RS, Spinney JJ, Abe EA, Probst CK, Franklin A, Logue A, Giacona F, Drummond M, Griffith J, Brazee PL et al (2022) Endothelial-specific loss of sphingosine-1-phosphate receptor 1 increases vascular permeability and exacerbates bleomycin-induced pulmonary fibrosis. Am J Respir Cell Mol Biol 66(1):38–52. https://doi.org/10.1165/rcmb.2020-0408OC
Shea BS, Brooks SF, Fontaine BA, Chun J, Luster AD, Tager AM (2010) Prolonged exposure to sphingosine 1-phosphate receptor-1 agonists exacerbates vascular leak, fibrosis, and mortality after lung injury. Am J Respir Cell Mol Biol 43(6):662–673. https://doi.org/10.1165/rcmb.2009-0345OC
Oo ML, Thangada S, Wu MT, Liu CH, Macdonald TL, Lynch KR, Lin CY, Hla T (2007) Immunosuppressive and anti-angiogenic sphingosine 1-phosphate receptor-1 agonists induce ubiquitinylation and proteasomal degradation of the receptor. J Biol Chem 282(12):9082–9. https://doi.org/10.1074/jbc.M610318200
Funding
This work was supported by the National Natural Science Foundation of China (No. 82170076).
Author information
Authors and Affiliations
Contributions
Jinghong Dai conceived the study. Ranxun Chen drafted the manuscript and drew the figure. All the authors were involved in revising the paper and approved the submitted version.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, R., Dai, J. Lipid metabolism in idiopathic pulmonary fibrosis: From pathogenesis to therapy. J Mol Med 101, 905–915 (2023). https://doi.org/10.1007/s00109-023-02336-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-023-02336-1