Abstract
Background
Advanced airway management (AAM) is part of the standard treatment during advanced cardiac life support (ACLS). Current studies underline the importance of a first-pass intubation success (FPS) during in-hospital ACLS. It was shown that a failed initial intubation attempt in out-of-hospital cardiac arrest (OHCA) patients in the emergency department is an independent risk factor for the decreased effectiveness of ACLS measured by the return of spontaneous circulation (ROSC).
Objective
This study first examines the association between prehospital FPS and ROSC in adults with OHCA and second identifies factors associated with FPS and ROSC. The initial hypothesis was that FPS would increase the probability of ROSC as well as decrease the time to ROSC.
Material and methods
A retrospective multicenter analysis of 180 adult non-traumatic OHCA patients on whom advanced airway management (AAM) was performed between July 2017 and December 2018 in five different German physician-staffed ambulance stations. For information on FPS the Intubation Registry, and for information on ROSC the German Resuscitation Registry were used. In addition to yes/no questions, multiple answers and free text answers are possible in those questionnaires. The main outcome variables were ‘FPS’, ‘ROSC’ and ‘time to ROSC’. Mann-Whitney tests, χ2-tests, Fisher’s exact tests and multivariate binary logistic regressions were used for the statistical evaluation. Demographic factors, characteristics of the performer, selected equipment, laryngoscopy type, intubation method, medications, verification of tube position, respiratory evaluation, complications and time to ROSC were examined with respect to the influence on FPS. Concerning ROSC, the following factors were examined: demographic factors, initial heart rhythm, initial breathing, medications, defibrillation and AAM.
Results
An FPS was recorded in 150 patients (83.3%), and ROSC was achieved in 82 patients (45.5%) after an average time of 22.16 min. There was a positive association between FPS and ROSC (p = 0.027). In patients with FPS, a trend for shorter time to ROSC was observed (p = 0.059; FPS 18 min; no FPS 28 min). The use of capnography (odds ratio, OR = 7.384, 95% confidence interval, CI 1.886–28.917) and complications during AAM (OR = 0.033, 95% CI: 0.007–0.153) were independently associated with FPS. The independent factor associated with ROSC was FPS (OR = 5.281, 95% CI: 1.800–15.494).
Conclusion
In prehospitally resuscitated adult OHCA patients with AAM, FPS is associated with a higher chance of ROSC.
Zusammenfassung
Hintergrund
Das erweiterte Atemwegsmanagement (AAM) ist Teil der Standardbehandlung bei erweiterten Reanimationsmaßnahmen (ACLS). Aktuelle Studien betonen die Relevanz eines erfolgreichen ersten Intubationsversuches (FPS) während ACLS. Bei Patienten mit außerklinischem Herz-Kreislauf-Stillstand (OHCA) erwies sich ein fehlgeschlagener erster Intubationsversuch als unabhängiger Risikofaktor für die verminderte Wirksamkeit des ACLS – gemessen am Wiedereinsetzen des Spontankreislaufs (ROSC).
Ziel der Arbeit
Diese Studie untersucht den präklinischen Zusammenhang zwischen dem FPS und ROSC bei Erwachsenen mit OHCA. Die initiale Hypothese war, dass bei erzieltem FPS die Wahrscheinlichkeit des ROSC steigt und sich die Zeit bis zum ROSC verringert.
Material und Methoden
Eine retrospektive multizentrische Analyse von 180 erwachsenen Patienten mit nichttraumatischem OHCA, bei denen zwischen Juli 2017 und Dezember 2018 in fünf verschiedenen deutschen ärztlich besetzten Rettungswachen ein AAM durchgeführt wurde. Für Informationen zum FPS wurde das Intubationsregister und für Informationen zum ROSC das Deutsche Reanimationsregister verwendet. Neben Ja/Nein-Fragen sind in diesen Fragebögen auch Mehrfachantworten und Freitextantworten möglich. Die wichtigsten Ergebnisvariablen waren „FPS“, „ROSC“ und „Zeit bis zum ROSC“. Für die statistische Auswertung wurden Mann-Whitney-Tests, χ2-Tests, Fisher-Exakt-Test und multivariate binäre logistische Regressionen verwendet. Demografische Faktoren, Charakteristika des Ausführenden, gewählte Ausrüstung, Art der Laryngoskopie, Intubationsmethode, Medikamente, Überprüfung der Tubusposition, respiratorische Bewertung, Komplikationen und Zeit bis zum ROSC wurden im Hinblick auf den Einfluss auf das FPS untersucht. In Bezug auf ROSC wurden folgende Faktoren untersucht: demografische Faktoren, anfänglicher Herzrhythmus, anfängliche Atmung, Medikamente, Defibrillation und AAM.
Ergebnisse
Bei 150 Patienten (83,3 %) wurde ein FPS, bei 82 Patienten (45,5 %) ein ROSC beobachtet. Beide Variablen standen korrelierten positiv miteinander (p = 0,027). Bei erzieltem FPS verringerte sich die Zeit bis zum ROSC (p = 0,059; FPS 18 min; kein FPS 28 min). Der FPS wurde als unabhängige Variable für den ROSC (OR = 5,281; 95 % KI 1,800–15,494) identifiziert.
Schlussfolgerung
Bei präklinisch wiederbelebten OHCA-Patienten mit AAM ist der FPS mit einer höheren ROSC-Wahrscheinlichkeit assoziiert.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction and background
Cardiac arrest is one of the most common causes of death. Cardiac arrest is treated by cardiopulmonary resuscitation (CPR): in the case of out-of-hospital cardiac arrest (OHCA), the basic life support, consisting of ventilation and chest compression, should be carried out by medical laypersons immediately after the need for CPR has been established. The medical team arriving usually later continues the CPR with measures of advanced cardiac life support (ACLS). Advanced airway management (AAM) is part of the standard treatment during ACLS [1].
If the first attempt at intubation is successful during AAM, it is called first-pass intubation success (FPS). Current studies underline the importance of FPS during in-hospital ACLS regarding further resuscitation measures [2]. A failed initial intubation attempt during OHCA is an independent risk factor for decreased effectiveness of the whole ACLS [3]. This might be explained by reduced hands-on chest time, which is known to reduce chances for return of spontaneous circulation (ROSC) [1].
The primary aim of this study was to investigate the association between prehospital FPS and ROSC and the occurrence of ROSC and time to ROSC in OHCA patients. The secondary aim was to identify factors associated with FPS and ROSC.
Methods
Study design and setting
This was a retrospective multicenter registry study in five different physician-staffed ambulance stations in Germany where AAM is provided by physicians trained in emergency medicine. In this setting, all steps of CPR are performed according to the guidelines of the European Resuscitation Council [4]. This study was approved by the ethics committees of the University Hospitals of Jena (No. 2019-1318-Daten) and Tübingen (No. 116/2019BO2).
Participants
The inclusion criteria for the patients in the study were non-traumatic OHCA patients aged ≥ 18 years, on whom AAM was provided by prehospital emergency physicians in the German physician-staffed ambulance stations Jena, Meiningen, Tübingen, Wittlich and Wolfenbüttel.
Data collection and processing
Data were collected during an 18-month period from 1 July 2017 until 31 December 2018, utilizing the local intubation registry, the German Resuscitation Registry, and the emergency medical protocols. All registry data were gathered by online questionnaires.
The intubation registry includes information on AAM (performer, equipment, laryngoscopy, intubation method, medications, verification of tube position, respiratory evaluation, complications) and FPS. The German Resuscitation Registry includes information on CPR (initial heart rhythm, initial breathing, medications, defibrillation) and ROSC.
Result measurements
The main outcome variables were FPS, ROSC and time to ROSC. Because time to ROSC is not included as variable in the registry, it was calculated by taking the time difference between starting point of CPR and time of ROSC.
Statistical methods
Continuous variables were presented as mean ± standard deviation (SD) or median and interquartile ranges (IQR), categorical variables as number and percent.
To compare nominal variables with more than 2 categories in univariate analysis we used the χ2-test, for continuous variables the Mann-Whitney U test and for binary variables the Fisher’s exact test. Only significant variables were included in the multivariate binary logistic regression and odds ratios (OR) with 95% confidence interval (CI) of the model are reported. All statistical analyses were conducted using the IBM SPSS Statistics software (IBM Corp., Armonk, NY, USA; version 25), the significance level was set at 0.05 for each test.
Results
Patient characteristics
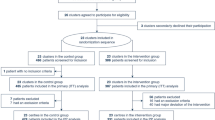
During the 18-month study period, 213 patients were recorded in the intubation registry, of which 180 patients were included in the study and analyzed, with most of the exclusions caused by incomplete questionnaires. The study population showed the following demographics: average age of 69.7 years (SD 12.9 years), mean age of 70 years (IQR 60–79.75 years), median body weight of 82.5 kg (IQR 75–95kg) and 71.7% male patients.
An FPS was recorded in 150 patients (83.3%), and ROSC was achieved in 82 patients (45.5%).
Association between FPS and ROSC and time to ROSC
There was a positive association between FPS and ROSC (p = 0.027, Table 1). In multivariate analysis, FPS was the only factor independently associated with ROSC, with an OR of 5.281 (p = 0.002, 95% CI 1.800–15.494) (Table 2). In patients with FPS, a statistically non-significant trend for shorter time to ROSC was observed: median 18min (IQR 7–27 min) vs. median 28 min (IQR 21–35 min) (p = 0.059, Table 3).
Factors associated with FPS
Patients were divided into two groups based on the presence of prehospital FPS (FPS, n = 150, 83.3%; No FPS, n = 30, 16.7%, Table 3).
In univariate analysis (Table 1), the following factors were associated with FPS: body weight (p = 0.044), throat suction (p = 0.001), verification of tube position (p < 0.001), airway assessment according to Cormack and Lehane (p < 0.001) and complications during intubation (p < 0.001). The following factors were not associated with FPS: age (p = 0.186), sex (p = 0.182), level of education of performer (p = 0.180), specialization of performer (p = 0.335), selected intubation equipment (p = 0.197), type of laryngoscopy (p = 0.062), intubation method (p = 0.901), specific medications (analgesics, p = 0.130; sedative, p = 0.692; muscle relaxants, p = 0.585) and time to ROSC (p = 0.059).
In multivariate analysis (Table 2), the use of capnography (OR = 7.384, 95% CI: 1.886–28.917) and complications during AAM (OR = 0.033, 95% CI: 0.007–0.153) were independently associated with FPS.
Factors associated with ROSC
Patients were divided into two groups based on the presence of prehospital ROSC (ROSC, n = 82, 45.6%; No ROSC, n = 98, 54.4%; Table 1). The average time to ROSC was 22.16 min (SD 12.7 min), the mean time was 20 min (IQR 14.5–28.5 min).
In univariate analysis (Table 1), the following factors were associated with ROSC: initial hearth rhythm (p = 0.001), initial breathing (p = 0.001), amiodarone (p = 0.037) and FPS (p = 0.027). The following factors were not associated with ROSC: age (p = 0.148), sex (p = 0.246), body weight (p = 0.057) and number of defibrillations (p = 0.227).
In multivariate analysis (Table 2), only FPS was independently associated with ROSC (OR = 5.281, 95% CI: 1.800–15.494).
Discussion
This study showed that in adult OHCA patients with AAM prehospital FPS was associated with a higher chance of ROSC. Factors associated with FPS positively were the use of capnography for confirmation of tube position, and no complications during AAM. Only FPS was a factor associated with ROSC.
In recent studies, FPS has been in the spotlight, e.g. a systematic review examined the emergency AAM in general and concluded that preclinical physicians achieved an FPS rate of 71.2–87.5% [2]. The FPS rate in this study (83.3%) during prehospital CPR is in line with these results. Since there was no connection between the FPS and the level of education of performer and specialization of performer in this study, one can assume good intubation expertise on the part of the emergency physicians for the data examined. Compared to pan-European data (32.7%) [9] the rate of prehospital ROSC (45.6%) was higher. This might be explained by the fact that in this study AAM was mostly provided by emergency physicians and not by paramedics.
Regarding FPS, the negative association of body weight to FPS can be explained by AAM itself becoming more difficult [10]. Using capnography for confirmation of correct tube position is required in the current resuscitation guidelines as the treatment standard [1]. The results of this study support this fact, because using capnography was independently associated with higher chance of FPS. The available data also show that the application rate of capnography was not 100%. This is probably due to the fact that the questionnaire differentiates between capnography and capnometry and is marginally misleading when it is filled out. This fuzziness should be examined more profoundly in the future.
Over the past few years, many studies have been carried out researching the best equipment for AAM [5,6,7,8]. This study cannot draw any sound conclusions about the best equipment, because ETI is overpresented (85.3% of all intubations).
Regarding complications during AAM (complication rate 14.2%), the most common documented was failed intubation followed by aspiration. Statistically, in this study complications during AAM were independently associated with FPS. Here, future studies should clarify the connection, because it is not clear whether the FPS failed due to complications during the AAM or whether an FPS was present before the emergency physicians noticed those complications (e.g. later aspiration). Further improvement of the questionnaires to depict the chronological sequence of event should occur.
The findings of this study show that a shockable rhythm and present gasping have a positive effect on probability of ROSC by intervening in the circulatory arrest in an earlier more favorable phase, which is consistent with other studies [3, 11, 12]. Compared to other studies, time to ROSC is slightly longer, which can be justified by methodological differences on calculating time to ROSC [11, 13]. Therefore, it would be desirable to integrate the variable time to ROSC into the resuscitation registers in order to ensure clear comparability.
The results confirm the significant positive association between prehospital FPS and ROSC [3, 14], with the distinctiveness that this study found this association in a setting with physician-staffed ambulance stations. If FPS was achieved, time to ROSC was lowered by an average of 10 min [3].
As prolonged intubation attempts usually occur while stopping chest compressions, an extended no-flow time might reduce the chance to achieve a ROSC and therefore affirm the importance of a fast FPS. Other reasons for the lower rate of ROSC might be a delay of other necessary interventions such as defibrillation or detecting and treating reversible causes of the cardiac arrest.
In future this study design should be repeated with larger power to see whether there is a statistically significant difference in time to ROSC depending on prehospital FPS.
Additionally, the length of the interruptions for intubating (if present) while performing chest compressions and subsequent disturbances if the ACLS algorithm should be further queried in the questionnaires. To this end, the questionnaires could be modified so that the medical staff could assess the effectiveness of their chest compressions and the amount of time they spent on resuscitation on a scale.
Limitations
This study has several limitations. First, the results are based on a retrospective analysis of 2 registries with the possible bias by the intrinsic design itself.
Second, the full treatment time was not always documented (start and end), therefore valid statements about survival times could not be made.
Third, this study only looked at appearance of preclinical ROSC. It is not possible to draw any conclusions as to whether the patients achieved a ROSC later in the hospital and no evaluation of neurological outcome.
Fourth, the informative value is limited in that the group sizes “FPS” and “No FPS” differ greatly from one another in quantitative terms. Attention should be paid to greater power in future investigations and possibly more locations to be included.
Conclusion
These results indicate that in adult OHCA patients with AAM, prehospital FPS is associated with a higher chance of ROSC. Additionally, the use of capnography and no complications during AAM were positive associated with the successful first-pass attempt.
References
Soar J, Nolan JP, Bottiger BW, Perkins GD, Lott C, Carli P et al (2015) European Resuscitation Council Guidelines for Resuscitation 2015: Section 3. Adult advanced life support. Resuscitation 95:100–147. https://doi.org/10.1016/j.resuscitation.2015.07.016
Bernhard M, Becker TK, Gries A, Knapp J, Wenzel V (2015) The first shot is often the best shot: first-pass intubation success in emergency airway management. Anesth Analg 121(5):1389–1393. https://doi.org/10.1213/ane.0000000000000891
Kim J, Kim K, Kim T, Rhee JE, Jo YH, Lee JH et al (2014) The clinical significance of a failed initial intubation attempt during emergency department resuscitation of out-of-hospital cardiac arrest patients. Resuscitation 85(5):623–627. https://doi.org/10.1016/j.resuscitation.2014.01.017
Monsieurs KG, Nolan JP, Bossaert LL, Greif R, Maconochie IK, Nikolaou NI et al (2015) European Resuscitation Council Guidelines for Resuscitation 2015: Section 1. Executive summary. Resuscitation 95:1–80. https://doi.org/10.1016/j.resuscitation.2015.07.038
Benoit JL, Gerecht RB, Steuerwald MT, McMullan JT (2015) Endotracheal intubation versus supraglottic airway placement in out-of-hospital cardiac arrest: a meta-analysis. Resuscitation 93:20–26. https://doi.org/10.1016/j.resuscitation.2015.05.007
White L, Melhuish T, Holyoak R, Ryan T, Kempton H, Vlok R (2018) Advanced airway management in out of hospital cardiac arrest: a systematic review and meta-analysis. Am J Emerg Med. https://doi.org/10.1016/j.ajem.2018.09.045
Bernhard M, Benger JR (2015) Airway management during cardiopulmonary resuscitation. Curr Opin Crit Care 21(3):183–187. https://doi.org/10.1097/mcc.0000000000000201
Okamoto H, Goto T, Wong ZSY, Hagiwara Y, Watase H, Hasegawa K et al (2019) Comparison of video laryngoscopy versus direct laryngoscopy for intubation in emergency department patients with cardiac arrest: a multicentre study. Resuscitation 136:70–77. https://doi.org/10.1016/j.resuscitation.2018.10.005
Grasner JT, Wnent J, Herlitz J, Perkins GD, Lefering R, Tjelmeland I et al (2020) Survival after out-of-hospital cardiac arrest in Europe—Results of the EuReCa TWO study. Resuscitation 148:218–226. https://doi.org/10.1016/j.resuscitation.2019.12.042
Wilson ME, Spiegelhalter D, Robertson JA, Lesser P (1988) Predicting difficult intubation. Br J Anaesth 61(2):211–216. https://doi.org/10.1093/bja/61.2.211
Navab E, Esmaeili M, Poorkhorshidi N, Salimi R, Khazaei A, Moghimbeigi A (2019) Predictors of out of hospital cardiac arrest outcomes in pre-hospital settings; a retrospective cross-sectional study. Arch Acad Emerg Med 7(1):36
Bobrow BJ, Zuercher M, Ewy GA, Clark L, Chikani V, Donahue D et al (2008) Gasping during cardiac arrest in humans is frequent and associated with improved survival. Circulation 118(24):2550–2554. https://doi.org/10.1161/circulationaha.108.799940
Gregers E, Kjaergaard J, Lippert F, Thomsen JH, Kober L, Wanscher M et al (2018) Refractory out-of-hospital cardiac arrest with ongoing cardiopulmonary resuscitation at hospital arrival—survival and neurological outcome without extracorporeal cardiopulmonary resuscitation. Crit Care 22(1):242. https://doi.org/10.1186/s13054-018-2176-9
Lesnick J, Zhang Y, Moore JX, Daya MR, Jarvis JW, Nichol G et al (2019) Abstract 02: effect of airway insertion first-pass success upon patient outcomes in the pragmatic airway resuscitation trial. Circulation 140(Suppl_2):A2‑A. https://doi.org/10.1161/circ.140.suppl_2.02
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
S. Montag, S. Herdtle, S. John, T. Lehmann, W. Behringer and C. Hohenstein declare that they have no competing interests.
This retrospective study was performed after consultation with the ethics committee of the university clinics in Jena and Tübingen and in accordance with national legal requirements.
Additional information

Scan QR code & read article online
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Montag, S., Herdtle, S., John, S. et al. Association between prehospital FPS and ROSC in adults with OHCA. Anaesthesiologie 71 (Suppl 2), 198–203 (2022). https://doi.org/10.1007/s00101-022-01193-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00101-022-01193-w
Keywords
- First-pass intubation success
- Airway management
- Out-of-hospital cardiac arrest
- Resuscitation
- Return of spontaneous circulation