Abstract
Purpose
Thoracic endovascular aortic repair (TEVAR) is increasingly utilized to treat blunt thoracic aortic injury (BTAI), but post-discharge outcomes remain underexplored. We examined 90-day readmission in patients treated with TEVAR following BTAI.
Methods
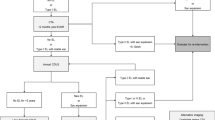
Adult patients discharged alive after TEVAR for BTAI in the Nationwide Readmissions Database between 2016 and 2019 were included. Outcomes examined were 90-day non-elective readmission, primary readmission reasons, and 90-day mortality. As a complementary analysis, 90-day outcomes following TEVAR for BTAI were compared with those following TEVAR for acute type B aortic dissection (TBAD).
Results
We identified 2085 patients who underwent TEVAR for BTAI. The median age was 43 years (IQR, 29–58), 65% of all patients had an ISS ≥ 25, and 13% were readmitted within 90 days. The main primary causes for readmission were sepsis (8.8%), wound complications (6.7%), and neurological complications (6.5%). Two patients developed graft thrombosis as primary readmission reasons. Compared with acute TBAD patients, BTAI patients had a significantly lower rate of readmission within 90 days (BTAI vs. TBAD; 13% vs. 29%; p < .001).
Conclusion
We found a significant proportion of readmission in patients treated with TEVAR for BTAI. However, the 90-day readmission rate after TEVAR for BTAI was significantly lower compared with acute TBAD, and the common cause for readmission was not related to residual aortic disease or vascular devices. This represents an important distinction from other patient populations treated with TEVAR for acute vascular conditions. Elucidating differences between trauma-related TEVAR readmissions and non-traumatic indications better informs both the clinician and patients of expected post-discharge course.
Level of evidence/study type: IV, Therapeutic/care management.

Similar content being viewed by others
Data Availability
The datasets generated and analyzed for this study are not publicly available except for those who purchased the data and signed the HCUP Data Use agreement training. Researchers should readily be able to publicly purchase the same databases we did to conduct research.
References
Akhmerov A, DuBose J, Azizzadeh A. Blunt thoracic aortic injury: current therapies, outcomes, and challenges. Ann Vasc Dis. 2019;12:1–5.
Mouawad NJ, Paulisin J, Hofmeister S, Thomas MB. Blunt thoracic aortic injury – concepts and management. J Cardiothorac Surg. 2020;15:62.
Kan Y, Huang L, Shi Z, Guo D, Si Y, Fu W. Aortic-related readmission after thoracic endovascular aortic repair for type B aortic dissection patients: a single-center retrospective study. Ann Vasc Surg. 2021; https://doi.org/10.1016/j.avsg.2021.10.072
Moore L, Stelfox HT, Turgeon AF, Nathens AB, le Sage N, Émond M, et al. Rates, patterns, and determinants of unplanned readmission after traumatic injury. Ann Surg. 2014;259:374–80.
Kalesan B, Cheng TW, Farber A, Zuo Y, Kalish JA, Jones DW, et al. Readmissions after thoracic endovascular aortic repair. J Vasc Surg. 2018;68:372-382.e3.
Chen SL, Kuo IJ, Kabutey N-K, Gabra F, Fujitani RM. Perioperative risk factors for hospital readmission after elective endovascular aortic aneurysm repair. J Vasc Surg. 2018;68:731-738.e1.
Wiseman JT, Guzman AM, Fernandes-Taylor S, Engelbert TL, Saunders SR, Kent CK. General and vascular surgery readmissions: a systematic review. J Am Coll Surg. 2014;219:552-569e2. https://doi.org/10.1016/j.jamcollsurg.2014.05.007.
Siracuse JJ, Shah NK, Peacock MR, Tahhan G, Kalish JA, Rybin D, et al. Thirty-day and 90-day hospital readmission after outpatient upper extremity hemodialysis access creation. J Vasc Surg. 2017;65:1376–82.
Tahhan G, Farber A, Shah NK, Krafcik BM, Sachs TE, Kalish JA, et al. Characterization of planned and unplanned 30-day readmissions following vascular surgical procedures. Vasc Endovascular Surg. 2017;51:17–22.
Krafcik BM, Komshian S, Lu K, Roberts L, Farber A, Kalish JA, et al. Short- and long-term readmission rates after infrainguinal bypass in a safety net hospital are higher than expected. J Vasc Surg. 2017;66:1786–91.
Fox N, Schwartz D, Salazar JH, Haut ER, Dahm P, Black JH, et al. Evaluation and management of blunt traumatic aortic injury. J Trauma Acute Care Surg. 2015;78:136–46.
Lee WA, Matsumura JS, Mitchell RS, Farber MA, Greenberg RK, Azizzadeh A, et al. Endovascular repair of traumatic thoracic aortic injury: clinical practice guidelines of the Society for Vascular Surgery. J Vasc Surg. 2011;53:187–92.
Williamson AJ, Sankary S, Kuchta KM, Gaines S, Morcos O, Lind B, et al. Contemporary unplanned readmission trends following management of type B aortic dissection. Vasc Specialist Int. 2022;38:16.
Iyengar A, Goel NJ, Kelly JJ, Han J, Brown CR, Khurshan F, et al. Predictors of 30-day readmission and resource utilization after thoracic endovascular aortic repair. Eur J Cardiothorac Surg. 2020;58:574–82.
Weiss S, Rojas RL, Habermann EB, Moriarty JP, Borah BJ, DeMartino RR. Impact of patient factors and procedure on readmission after aortic dissection admission in the states of Florida and New York. J Vasc Surg. 2020;72:1277–87.
Carroll BJ, Schermerhorn M, Kennedy KF, Swerdlow N, Soriano KM, Yeh RW, et al. Readmissions after acute type B aortic dissection. J Vasc Surg. 2020;72:73-83.e2.
Introduction to the HCUP Nationwide Readmissions Database (NRD) 2019 [Internet]. 2019 [cited 2022 Aug 13]. Available from: https://www.hcup-us.ahrq.gov/db/nation/nrd/Introduction_NRD_2019.pdf. Accessed 13 Aug 2022
Cuschieri S. The STROBE guidelines. Saudi J Anaesth. 2019;13:31. https://doi.org/10.4103/sja.SJA_543_18.
Lombardi JV, Hughes GC, Appoo JJ, Bavaria JE, Beck AW, Cambria RP, et al. Society for Vascular Surgery (SVS) and Society of Thoracic Surgeons (STS) reporting standards for type B aortic dissections. J Vasc Surg. 2020;71:723–47.
Elixhauser A, Steiner C, Harris DR, Coffey RM. Comorbidity measures for use with administrative data. Med Care. 1998;36:8–27.
Townsend JCM, Beauchamp RD, Evers BM, Mattox KL. (2016). Sabiston textbook of surgery. (21st ed.) Elsevier - Health Sciences Division
Treffalls JA, Sylvester CB, Parikh U, Zea-Vera R, Ryan CT, Zhang Q, et al. Nationwide database analysis of one-year readmission rates after open surgical or thoracic endovascular repair of Stanford type B aortic dissection. JTCVS Open. 2022;11:1–13.
Starnes BW, Dwivedi A, Giglia J, Woo K, Yeh C. Updated outcomes from the TRANSFIX study to evaluate endovascular repair of blunt thoracic aortic injuries with the Zenith Alpha thoracic device. J Vasc Surg. 2020;71:1851–7.
Olufajo OA, Cooper Z, Yorkgitis BK, Najjar PA, Metcalfe D, Havens JM, et al. The truth about trauma readmissions. The Am J Surg. 2016;211:649–55.
Parreco J, Buicko J, Cortolillo N, Namias N, Rattan R. Risk factors and costs associated with nationwide nonelective readmission after trauma. J Trauma Acute Care Surg. 2017;83:126–34.
Greenblatt DY, Greenberg CC, Kind AJH, Havlena JA, Mell MW, Nelson MT, et al. Causes and implications of readmission after abdominal aortic aneurysm repair. Ann Surg. 2012;256:595–605.
Liu V, Lei X, Prescott HC, Kipnis P, Iwashyna TJ, Escobar GJ. Hospital readmission and healthcare utilization following sepsis in community settings. J Hosp Med. 2014;9:502–7.
Chang DW, Tseng C-H, Shapiro MF. Rehospitalizations following sepsis. Crit Care Med. 2015;43:2085–93.
Prescott HC, Langa KM, Liu V, Escobar GJ, Iwashyna TJ. Increased 1-year healthcare use in survivors of severe sepsis. Am J Respir Crit Care Med. 2014;190:62–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The Mass General Brigham Institutional Review Board approved this study, and informed consent was waived.
Conflict of interest
The authors declare no competing interests.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Romijn, AS.C., Proaño-Zamudio, J.A., Rastogi, V. et al. Readmission after thoracic endovascular aortic repair following blunt thoracic aortic injury. Eur J Trauma Emerg Surg 50, 551–559 (2024). https://doi.org/10.1007/s00068-023-02432-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-023-02432-4