Abstract
Purpose
Emergency and trauma physicians typically rely on anatomic landmarks to determine the proper intercostal space for emergent tube thoracostomy. However, physicians using this technique select a potentially dangerous insertion site too inferior in nearly one-third of cases, which have the potential to result in subdiaphragmatic puncture. We investigated a point-of-care ultrasound (POCUS) thoracic “Quick Look” procedure as a technique to allow visualization of underlying structures to avoid tube misplacement.
Methods
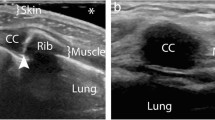
We performed an observational study of adult emergency department patients and their treating physicians. The patient’s emergency physician was asked to rapidly identify and mark a hypothetical tube thoracostomy insertion site on the patient’s chest wall. An ultrasound fellow then performed a POCUS thoracic “Quick Look” exam with a phased-array probe placed directly over the marked site. Over one regular respiratory cycle, the identification of standard lung pattern was considered a negative scan whereas visualization of the diaphragm with underlying liver or spleen was considered a positive scan. Time for completion of the “Quick Look” scan was measured and inter-rater reliability was determined through image review by a single, blinded ultrasound director.
Results
Seventy-six thoracic “Quick Look” scans were performed on patient subjects, of which 17% (13/76, 95%CI 8–26%) were positive. The average time for performing the “Quick Look” exam was 43 s (95%CI 30–57). Inter-rater reliability of the thoracic “Quick Look” was excellent (κ = 0.95).
Conclusion
Thoracic “Quick Look” exams performed at mock chest tube insertion sites demonstrated potentially dangerous insertions in 17% of the cases. POCUS thoracic “Quick Look” may be a rapid and reliable technique that improves safety when placing an emergent chest tube.





Similar content being viewed by others
References
Henry S. ATLS 10th edition offers new insights into managing trauma patients. American College of Surgeons. 2018. www.bulletin.facs.org/2018/06/atls-10th-edition-offers-new-insights-into-managing-trauma-patients/. Accessed March 4, 2022.
Alrahbi R, Easton R, Bendinelli C, Enninghorst N, Sisak K, Balogh ZJ. Intercostal catheter insertion: are we really doing well? ANZ J Surg. 2012;82(6):392–4. https://doi.org/10.1111/j.1445-2197.2012.06093.x.
Ball CG, Lord J, Laupland KB, et al. Chest tube complications: how well are we training our residents? Can J Surg. 2007;50(6):450–8.
Carter P, Conroy S, Blakeney J, Sood B. Identifying the site for intercostal catheter insertion in the emergency department: Is clinical examination reliable? Emerg Med Australas. 2014;26(5):450–4. https://doi.org/10.1111/1742-6723.12276.
Daly RC, Mucha P, Pairolero PC, Fernell MB. The risk of percutaneous chest tube thoracostomy for blunt thoracic trauma. Ann Emerg Med. 1985;14(9):865–70. https://doi.org/10.1016/S0196-0644(85)80635-1.
Harris A, O’Driscoll BR, Turkington PM. Survey of major complications of intercostal chest drain insertion in the UK. Postgraduate Med J. 2010;86(1012):68–72. https://doi.org/10.1136/pgmj.2009.087759.
Kesieme EB, Dongo A, Ezemba N, Irekpita E, Jebbin N, Kesieme C. Tube thoracostomy: complications and its management. Pulmonary Med. 2012. https://doi.org/10.1155/2012/256878.
Osinowo O, Softah AL, Zahrani ME. Ectopic chest tube insertions: diagnosis and strategies for prevention. Afr J Med Med Sci. 2002;31:67–70.
Jayathissa S, Dee S. How safe is the “safe triangle”? N Z Med J. 2011;124(1343):79–83.
Gray EJ, Cranford JA, Betcher JA, et al. Sonogram of safety: ultrasound outperforms the fifth intercostal space landmark for tube thoracostomy site selection. J Clin Ultrasound. 2020;1(48):303–6. https://doi.org/10.1002/jcu.22851.
Diacon AH, Brutsche MH, Solèr M. Accuracy of pleural puncture sites: a prospective comparison of clinical examination with ultrasound. Chest. 2003;123(2):436–41. https://doi.org/10.1378/chest.123.2.436.
Elsayed H, Roberts R, Emadi M, Whittle I, Shackcloth M. Chest drain insertion is not a harmless procedure—are we doing it safely? Interact Cardiovasc Thorac Surg. 2010;11(6):745–9. https://doi.org/10.1510/icvts.2010.243196.
Ferrie EP, Collum N, McGovern S. The right place in the right space? Awareness of site for neddle thoracocentesis. Emerg Med J. 2005;22(11):788–9. https://doi.org/10.1136/emj.2004.015107.
Havelock T, Teoh R, Laws D, Gleeson F. Pleural procedures and thoracic ultrasound: British Thoracic Society pleural disease guideline 2010. Thorax. 2010;65(Suppl 2):ii61–ii76. https://doi.org/10.1136/thx.2010.137026.
Bowness JS, Nicholls K, Kilgour PM, et al. Finding the fifth intercostal space for chest drain insertion: guidelines and ultrasound. Emerg Med J. 2015;32(12):951–4. https://doi.org/10.1136/emermed-2015-205222.
Salamonsen M, Ellis S, Paul E, Steinke K, Fielding D. Thoracic ultrasound demonstrates variable location of the intercostal artery. Respiration. 2012;83(4):323–9. https://doi.org/10.1159/000330920.
Barnes TW, Morgenthaler TI, Olson EJ, Hesley GK, Decker PA, Ryu JH. Sonographically guided thoracentesis and rate of pneumothorax. J Clin Ultrasound 2005;33:442–6. https://doi.org/10.1002/jcu.20163.
Heidecker J, Huggins JT, Sahn SA, Doelken P. Pathophysiology of pneumothorax following ultrasound-guided thoracentesis. Chest. 2006;130(4):1173–84. https://doi.org/10.1378/chest.130.4.1173.
Kiranantawat N, Sungsiri J, Geater SL. Outcome of ultrasound-guided small-bore catheter drainage in exudative pleural effusions. J Med Assoc Thailand. 2014;97(5):548–53.
McGahan JP. Aspiration and drainage procedures in the intensive care unit: percutaneous sonographic guidance. Radiology. 1985;154(2):531–2.
Prina E, Torres A, Roberto C, Carvalho R. Lung ultrasound in the evaluation of pleural effusion. Ultrassom de pulmão na avaliação de derrame pleural. J Bras Pneumol. 2014;40:1–5.
Smargiassi A, Inchingolo R, Soldati G, et al. The role of chest ultrasonography in the management of respiratory diseases: document II. Multidiscip Respir Med. 2013. https://doi.org/10.1186/2049-6958-8-55.
Wrightson JM, Fysh E, Maskell NA, Lee YCG. Risk reduction in pleural procedures: sonography, simulation and supervision. Curr Opin Pulm Med. 2010;16:340–50. https://doi.org/10.1097/MCP.0b013e32833a233b.
Gordon CE, Feller-Kopman D, Balk EM, Smetana GW. Pneumothorax following thoracentesis. A systematic review and meta-analysis. Arch Intern Med. 2010;170(4):332–9.
Dancel R, Schnobrich D, Puri N, et al. Recommendations on the use of ultrasound guidance for adult thoracentesis: a position statement of the society of hospital medicine. J Hosp Med Frontline Med Commun. 2018;13:126–35.
Jenkins JA, Gharahbaghian L, Doniger SJ, et al. Sonographic identification of tube thoracostomy study (SITTS): confirmation of intrathoracic placement. Western J Emerg Med. 2012;13(4):305–11. https://doi.org/10.5811/westjem.2011.10.6680.
Salz TO, Wilson SR, Liebmann O, Price DD. An initial description of a sonographic sign that verifies intrathoracic chest tube placement. Am J Emerg Med. 2010;28(5):626–30. https://doi.org/10.1016/j.ajem.2009.04.010.
Menegozzo CAM, Utiyama EM. Steering the wheel towards the standard of care: proposal of a step-by-step ultrasound-guided emergency chest tube drainage and literature review. Int J Surg. 2018;56:315–9. https://doi.org/10.1016/j.ijsu.2018.07.002.
Alrajhi K, Woo MY, Vaillancourt C. Test characteristics of ultrasonography for the detection of pneumothorax: a systematic review and meta-analysis. Chest. 2012;141(3):703–8. https://doi.org/10.1378/chest.11-0131.
Chan L, Reilly KM, Henderson C, Kahn F, Salluzzo RF. Complication rates of tube thoracostomy. Am J Emerg Med. 1997;15(4):368–70.
Ding W, Shen Y, Yang J, He X, Zhang M. Diagnosis of pneumothorax by radiography and ultrasonography: a meta-analysis. Chest. 2011;140(4):859–66. https://doi.org/10.1378/chest.10-2946.
Kuhajda I, Zarogoulidis K, Kougioumtzi I, et al. Tube thoracostomy; chest tube implantation and follow up. J Thorac Dis. 2014;6(4):470–9. https://doi.org/10.3978/j.issn.2072-1439.2014.09.23.
Maybauer MO, Geisser W, Wolff H, Maybauer DM. Incidence and outcome of tube thoracostomy positioning in trauma patients. Prehosp Emerg Care. 2012;16(2):237–41. https://doi.org/10.3109/10903127.2011.615975.
Saucier S, Motyka C, Killu K. Ultrasonography versus chest radiography after chest tube removal for the detection of pneumothorax. AACN Adv Crit Care. 2010;21(1):34–8.
Peabody CR, Mandavia D. Deep needle procedures: improving safety with ultrasound visualization. 2014 Jun. www.journalpatientsafety.com. Accessed March 5, 2022.
Acknowledgements
We thank the residents and attendings at Allegheny General Hospital’s Emergency Department who participated in mock chest tube insertion site scenarios with enrolled patients. This research was presented in 2017 at the following locations: Society for Academic Emergency Medicine Annual Meeting. Lightening Oral Presentation. Orlando, FL. May 17, 2017. Society for Academic Emergency Medicine Mid-Atlantic Regional Research Conference. Washington, DC. March 11, 2017.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
This study was performed in line with the principles and ethical standards as displayed in the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by Allegheny General Hospital’s Institutional Review Board.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 234 KB)
Supplementary file2 (MP4 370 KB)
Supplementary file3 (MP4 242 KB)
Supplementary file4 (MP4 300 KB)
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lieurance, R., Scheatzle, M., Johnjulio, W.A. et al. Point-of-care ultrasound thoracic “Quick Look” identifies potentially dangerous chest tube insertion sites. Eur J Trauma Emerg Surg 49, 777–783 (2023). https://doi.org/10.1007/s00068-022-02109-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-022-02109-4