Abstract
Purpose
Mobility patterns of western societies have been changing due to ongoing demographic change. Therefore, continuously updated epidemiological data on fracture morphology and treatment strategies are needed.
Methods
This retrospective single-center study included all tibial plateau fractures (TPF) between January 2011 and December 2020 in a level-I trauma center in Central Europe. Epidemiology, trauma mechanism and fracture morphology were analyzed. Age- and sex-specific differences regarding fracture classification (Schatzker, AO/OTA, Moore) and changes during the study period are highlighted.
Results
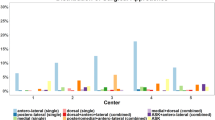
A total of 607 patients (55.2% women, 44.8% men, mean age 52.9 years (± 17.9)) were included in the study, 462 (76.1%) thereof having undergone surgical treatment. Over the decade, an increase in mean age (+ 7.4 years; p = 0.10), incidence (+ 68%; p < 0.05) and low-energy trauma was observed, with the highest peak in elderly women. Within classifications, AO/OTA 41-B3 (24.9%), Schatzker II (26.8%) and Moore V (46.6%) fractures were the most common.
Conclusion
Incidence (+ 68%), mean age and fractures with signs of knee dislocation of tibial plateau fracture increased over the last decade and low-energy trauma mechanism are more frequent. As the increase in incidence is mainly seen in older women, the comorbidities and need for immediate postoperative full weight-bearing have to be considered in treatment strategies.





Similar content being viewed by others
References
Rapp K, Büchele G, Dreinhöfer K, Bücking B, Becker C, Benzinger P. Epidemiology of hip fractures : systematic literature review of german data and an overview of the international literature. Z Gerontol Geriatr. 2019;52:10–6.
Hagen G, Magnussen J, Tell G, Omsland T. Estimating the future burden of hip fractures in Norway. NOREPOS Study Bone. 2020;131:115156.
Rundgren J, Bojan A, Mellstrand Navarro C, Enocson A. Epidemiology, classification, treatment and mortality of distal radius fractures in adults: an observational study of 23,394 fractures from the national swedish fracture register. BMC Musculoskelet Disord. 2020;21:88.
Hernandez RK, Do TP, Critchlow CW, Dent RE, Jick SS. Patient-related risk factors for fracture-healing complications in the United Kingdom general practice research database. Acta Orthop. 2012;83:653–60.
Pfeufer D, Grabmann C, Mehaffey S, Keppler A, Böcker W, Kammerlander C, et al. Weight bearing in patients with femoral neck fractures compared to pertrochanteric fractures: a postoperative gait analysis. Injury. 2019;50:1324–8.
Sabatini L, Aprato A, Camazzola D, Bistolfi A, Capella M, Massè A. Primary total knee arthroplasty in tibial plateau fractures: literature review and our institutional experience. Injury. 2021;S0020–1383(21):00104–12.
Elsoe R, Larsen P, Nielsen NPH, Swenne J, Rasmussen S, Ostgaard SE. Population-based epidemiology of tibial plateau fractures. Orthopedics. 2015;38:e780–6.
Oladeji LO, Worley JR, Crist BD. Age-related variances in patients with tibial plateau fractures. J Knee Surg. 2020;33:611–5.
Wennergren D, Bergdahl C, Ekelund J, Juto H, Sundfeldt M, Möller M. Epidemiology and incidence of tibia fractures in the swedish fracture register. Injury. 2018;49:2068–74.
Rupp M, Walter N, Pfeifer C, Lang S, Kerschbaum M, Krutsch W, et al. The incidence of fractures among the adult population of germany–an analysis from 2009 through 2019. Dtsch Arztebl Int. 2021;118:665–9.
Krause M, Preiss A, Müller G, Madert J, Fehske K, Neumann MV, et al. Intra-articular tibial plateau fracture characteristics according to the “ten segment classification.” Injury. 2016;47:2551–7.
Borgström F, Karlsson L, Ortsäter G, Norton N, Halbout P, Cooper C, et al. Fragility fractures in Europe: burden, management and opportunities. Arch Osteoporos. 2020;15:59.
Decruz J, Antony Rex RP, Khan SA. Epidemiology of inpatient tibia fractures in Singapore—a single centre experience. Chin J Traumatol. 2019;22:99–102.
Hua K, Jiang X, Zha Y, Chen C, Zhang B, Mao Y. Retrospective analysis of 514 cases of tibial plateau fractures based on morphology and injury mechanism. J Orthop Surg Res. 2019;14:267.
Yao X, Xu Y, Yuan J, Lv B, Fu X, Wang L, et al. Classification of tibia plateau fracture according to the “four-column and nine-segment.” Injury. 2018;49:2275–83.
Hissnauer T-N, Krause M, Frings J, Frosch K-H. Chirurgische Zugänge zum Tibiakopf. OP-JOURNAL Georg Thieme Verlag KG. 2019;34:107–16.
Schatzker J, Mcbroom R, Bruce D. The tibial plateau fracture: the toronto experience 1968–1975. Clin Orthop Rel Res. 1979;138:94–104.
Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, DeCoster TA, et al. Fracture and dislocation classification compendium - 2007: Orthopaedic Trauma Association classification, database and outcomes committee. J Orthop Trauma. 2007;21:S1-133.
Moore TM. Fracture dislocation of the knee. Clin Orthop Relat Res. 1981;156:128–40.
Alvi F, Charalambous CP, Tryfonidis M, Samarji R, Hirst P. Inter- and intra-observer variation of the Schatzker and AO/OTA classifications of tibial plateau fractures and a proposal of a new classification system. Injury Extra. 2008;5:178.
Luo C-F, Sun H, Zhang B, Zeng B-F. Three-column fixation for complex tibial plateau fractures. J Orthop Trauma. 2010;24:683–92.
Wang Y, Luo C, Zhu Y, Zhai Q, Zhan Y, Qiu W, et al. Updated three-column concept in surgical treatment for tibial plateau fractures—a prospective cohort study of 287 patients. Injury. 2016;47:1488–96.
Walton NP, Harish S, Roberts C, Blundell C. AO or Schatzker? How reliable is classification of tibial plateau fractures? Arch Orthop Trauma Surg. 2003;123:396–8.
Mthethwa J, Chikate A. A review of the management of tibial plateau fractures. Musculoskelet Surg. 2018;102:119–27.
Statistisches Amt München—ZIMAS 2021.
Herteleer M, Van Brandt C, Vandoren C, Nijs S, Hoekstra H. Tibial plateau fractures in Belgium: epidemiology, financial burden and costs curbing strategies. Eur J Trauma Emerg Surg. 2020. https://doi.org/10.1007/s00068-020-01525-8.
Hopewell S. Multifactorial and multiple component interventions for preventing falls in older people living in the community. Cochrane Library. 2018. https://doi.org/10.1002/14651858.CD012221.pub2/full.
Ali M, Eiriksdottir A, Murtadha M, Åkesson A, Atroshi I. Incidence of distal radius fracture in a general population in southern Sweden in 2016 compared with 2001. Osteoporos Int. 2020;31:715–20.
Wilcke MKT, Hammarberg H, Adolphson PY. Epidemiology and changed surgical treatment methods for fractures of the distal radius: a registry analysis of 42,583 patients in Stockholm County, Sweden, 2004–2010. Acta Orthop. 2013;84:292–6.
McLellan AR, Gallacher SJ, Fraser M, McQuillian C. The fracture liaison service: success of a program for the evaluation and management of patients with osteoporotic fracture. Osteoporos Int. 2003;14:1028–34.
Nakayama A, Major G, Holliday E, Attia J, Bogduk N. Evidence of effectiveness of a fracture liaison service to reduce the re-fracture rate. Osteoporos Int. 2016;27:873–9.
Hadji P, Klein S, Gothe H, Häussler B, Kless T, Schmidt T, et al. The epidemiology of osteoporosis–bone evaluation study (BEST): an analysis of routine health insurance data. Dtsch Arztebl Int. 2013;110:52–7.
Court-Brown CM, Caesar B. Epidemiology of adult fractures: a review. Injury. 2006;37:691–7.
Blain H, Masud T, Dargent-Molina P, Martin FC, Rosendahl E, van der Velde N, et al. A comprehensive fracture prevention strategy in older adults: the European Union geriatric medicine society (EUGMS) statement. Aging Clin Exp Res. 2016;28:797–803.
Gosch M, Kammerlander C, Neuerburg C. Osteoporose—epidemiologie und versorgungsqualität. Z Gerontol Geriat. 2019;52:408–13.
Johnell O, Kanis JA. An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int. 2006;17:1726–33.
Mustonen AOT, Koskinen SK, Kiuru MJ. Acute knee trauma: analysis of multidetector computed tomography findings and comparison with conventional radiography. Acta Radiol. 2005;46:866–74.
Kfuri M, Schatzker J. Revisiting the schatzker classification of tibial plateau fractures. Injury Elsevier. 2018;49:2252–63.
Yacoubian SV, Nevins RT, Sallis JG, Potter HG, Lorich DG. Impact of MRI on treatment plan and fracture classification of tibial plateau fractures. J Orthop Trauma. 2002;16:632–7.
Millar SC, Arnold JB, Thewlis D, Fraysse F, Solomon LB. A systematic literature review of tibial plateau fractures: what classifications are used and how reliable and useful are they? Injury. 2018;49:473–90.
Jensen DB, Rude C, Duus B, Bjerg-Nielsen A. Tibial plateau fractures a comparison of conservative and surgical treatment. J Bone Joint Surg Br. 1990;72(4):9–52.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest. All authors certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
The study was approved by the local Ethical Committee. (21–0559).
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bormann, M., Neidlein, C., Gassner, C. et al. Changing patterns in the epidemiology of tibial plateau fractures: a 10-year review at a level-I trauma center. Eur J Trauma Emerg Surg 49, 401–409 (2023). https://doi.org/10.1007/s00068-022-02076-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-022-02076-w