Abstract
Purpose
The purpose of this study was to determine outcomes in patients presenting to emergency department (ED) with acute abdominal pain and suspected occult myocardial injury [OMI (high-sensitive cardiac troponin T, hs-cTnT level > 14 ng/L)] without clinical signs of myocardial ischaemia. We hypothesized that OMI is a common entity associated with poor outcomes.
Methods
After institutional research ethics committee approval, a retrospective review was performed on patients subjected to extended use of hs-cTnT measurements during two months period in patients admitted to ED with a chief complaint of abdominal pain, aged 30 years or older and triaged to red, orange, or yellow categories. Primary outcomes were 30-day, six-month, and one-year mortality, respectively. Adjusted mortality rates were compared using the Cox proportional hazard regression model.
Results
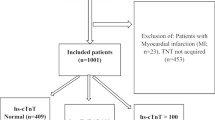
Overall, 1000 consecutive patients were screened. A total of 375 patients were subjected to hs-cTnT measurement and 156 of them (41.6%) experienced OMI. None of the patients had acute myocardial infarction diagnosed in the ED. Patients with OMI had a significantly higher 30-day, six-month and one-year mortality compared to the normal hs-cTnT level group [12.8% (20/156) vs. 3.7% (8/219), p = 0.001, 34.0% (53/156) vs. 6.9% (15/219), p < 0.001 and 39.1% (61/156) vs. 9.1 (20/219), p < 0.001, respectively]. OMI was an independent risk factor for mortality at every time point analyzed.
Conclusion
Our investigation noted OMI in older patients with co-morbidities and in higher triage category presenting with abdominal pain to ED, respectively. OMI is an independent risk factor for poor outcomes that warrants appropriate screening and management strategy. Our results support the use of hs-cTnT as a prognostication tool in this subgroup of ED patients.


Similar content being viewed by others
References
Bhuiya FA, McCaig LF. Emergency department visits for chest pain and abdominal pain: United States, 1999–2008. NCHS Data Brief. 2010;43:1–8.
Moore BJ (IBM Watson Health), Stocks C (AHRQ), Owens PL (AHRQ). Trends in Emergency Department Visits, 2006–2014. HCUP Statistical Brief #227. September 2017. Agency for Healthcare Research and Quality, Rockville MD.
Health & welfare overview [Internet]. Australian Institute of Health and Welfare. [cited 2020 Sep 5]. https://www.aihw.gov.au/reports-data/health-welfare-overview
Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, et al. Executive Group on behalf of the Joint European Society of Cardiology (ESC)/American College of Cardiology (ACC)/American Heart Association (AHA)/World Heart Federation (WHF) Task Force for the Universal Definition of Myocardial Infarction. Fourth Universal Definition of Myocardial Infarction. J Am Coll Cardiol. 2018. https://doi.org/10.1016/j.jacc.2018.08.1038.
Lindner G, Pfortmueller CA, Braun CT, Exadaktylos AK. Non-acute myocardial infarction-related causes of elevated high-sensitive troponin T in the emergency room: a cross-sectional analysis. Internal Emerg Med. 2014. https://doi.org/10.1007/s11739-013-1030-y.
Latini R, Masson S, Anand IS, Missov E, Carlson M, Vago T, et al. Prognostic value of very low plasma concentrations of troponin T in patients with stable chronic heart failure. Circulation. 2007. https://doi.org/10.1161/CIRCULATIONAHA.106.655076.
Omland T, de Lemos JA, Sabatine MS, Christophi CA, Rice MM, Jablonski KA, et al. A sensitive cardiac troponin T assay in stable coronary artery disease. N Engl J Med. 2009. https://doi.org/10.1056/NEJMoa0805299.
Wilhelm J, Hettwer S, Schuermann M, Bagger S, Gerhardt F, Mundt S, et al. Elevated troponin in septic patients in the emergency department: frequency, causes, and prognostic implications. Clin Res Cardiol. 2014. https://doi.org/10.1007/s00392-014-0684-4.
Keskpaik T, Starkopf J, Kirsimägi Ü, Mihnovitš V, Lomp A, Raamat E-M, et al. The role of elevated high-sensitivity cardiac troponin on outcomes following severe blunt chest trauma. Injury. 2020. https://doi.org/10.1016/j.injury.2019.12.037.
Writing Committee for the VISION Study Investigators, Devereaux PJ, Biccard BM, Sigamani A, Xavier D, Chan MTV, et al. Association of postoperative high-sensitivity troponin levels with myocardial injury and 30-day mortality among patients undergoing noncardiac surgery. JAMA. 2017. https://doi.org/10.1001/jama.2017.4360.
Baron JM, Lewandrowski EL, Januzzi JL, Bajwa EK, Thompson BT, Lewandrowski KB. Measurement of high-sensitivity troponin T in noncardiac medical intensive care unit patients. Am J Clin Pathol. 2014. https://doi.org/10.1309/AJCPLVQQY35XTFVN.
DeFilippis AP, Chapman AR, Mills NL, de Lemos JA, Arbab-Zadeh A, Newby LK, et al. Assessment and treatment of patients with type 2 myocardial infarction and acute nonischemic myocardial injury. Circulation. 2019. https://doi.org/10.1161/CIRCULATIONAHA.119.040631.
Kadesjö E, Roos A, Siddiqui A, Desta L, Lundbäck M, Holzmann MJ. Acute versus chronic myocardial injury and long-term outcomes. Heart. 2019. https://doi.org/10.1136/heartjnl-2019-315036.
Widgren BR, Jourak M. Medical emergency triage and treatment system (METTS): a new protocol in primary triage and secondary priority decision in emergency medicine. J Emerg Med. 2011. https://doi.org/10.1016/j.jemermed.
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, et al. The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA. 2016. https://doi.org/10.1001/jama.2016.0287.
Song J-U, Sin CK, Park HK, Shim SR, Lee J. Performance of the quick Sequential (sepsis-related) Organ Failure Assessment score as a prognostic tool in infected patients outside the intensive care unit: a systematic review and meta-analysis. Crit Care. 2018. https://doi.org/10.1186/s13054-018-1952-x.
Müokardiinfarktiregister. [cited 2020 Aug 5]. https://www.kliinikum.ee/leht/e-keskkond/377-mueokardiinfarktiregister
Brieger D, Eagle KA, Goodman SG, Steg PG, Budaj A, White K, et al. Acute coronary syndromes without chest pain, an underdiagnosed and undertreated high-risk group: insights from the Global Registry of Acute Coronary Events. Chest. 2004. https://doi.org/10.1378/chest.126.2.461.
Nakahashi T, Sakata K, Masuda J, Kumagai N, Higuma T, Ogimoto A, et al. Comparison of door-to-balloon time and 30-day mortality according to symptom presentation in patients with acute myocardial infarction. Circ Rep. 2021. https://doi.org/10.1253/circrep.CR-21-0006.
Botto F, Alonso-Coello P, Chan MTV, Villar JC, Xavier D, Srinathan S, et al. Myocardial injury after noncardiac surgery: a large, international, prospective cohort study establishing diagnostic criteria, characteristics, predictors, and 30-day outcomes. Anesthesiology. 2014. https://doi.org/10.1097/ALN.0000000000000113.
Shen J-T, Xu M, Wu Y, Wen S-H, Li X, Zhao B-C, et al. Association of pre-operative troponin levels with major adverse cardiac events and mortality after noncardiac surgery: a systematic review and meta-analysis. Eur J Anaesthesiol. 2018. https://doi.org/10.1097/EJA.0000000000000868.
Haaf P, Drexler B, Reichlin T, Twerenbold R, Reiter M, Meissner J, et al. High-sensitivity cardiac troponin in the distinction of acute myocardial infarction from acute cardiac noncoronary artery disease. Circulation. 2012. https://doi.org/10.1161/CIRCULATIONAHA.112.100867.
Jarolim P. High sensitivity cardiac troponin assays in the clinical laboratories. Clin Chem Lab Med. 2015. https://doi.org/10.1515/cclm-2014-0565.
de Lemos JA, Drazner MH, Omland T, Ayers CR, Khera A, Rohatgi A, et al. Association of troponin T detected with a highly sensitive assay and cardiac structure and mortality risk in the general population. JAMA. 2010. https://doi.org/10.1001/jama.2010.1768.
deFilippi CR, de Lemos JA, Christenson RH, Gottdiener JS, Kop WJ, Zhan M, et al. Association of serial measures of cardiac troponin T using a sensitive assay with incident heart failure and cardiovascular mortality in older adults. JAMA. 2010. https://doi.org/10.1001/jama.2010.1708.
Courtney D, Conway R, Kavanagh J, O’Riordan D, Silke B. High-sensitivity troponin as an outcome predictor in acute medical admissions. Postgr Med J. 2014. https://doi.org/10.1136/postgradmedj-2013-132325.
Devereaux PJ, Beattie WS, Choi PT-L, Badner NH, Guyatt GH, Villar JC, et al. How strong is the evidence for the use of perioperative β blockers in non-cardiac surgery? Systematic review and meta-analysis of randomised controlled trials. BMJ. 2005. https://doi.org/10.1136/bmj.38503.623646.8F.
Foucrier A, Rodseth R, Aissaoui M, Ibanes C, Goarin J-P, Landais P, et al. The long-term impact of early cardiovascular therapy intensification for postoperative troponin elevation after major vascular surgery. Anesth Analg. 2014. https://doi.org/10.1213/ANE.0000000000000302.
POISE Study Group, Devereaux PJ, Yang H, Yusuf S, Guyatt G, Leslie K, et al. Effects of extended-release metoprolol succinate in patients undergoing non-cardiac surgery (POISE trial): a randomised controlled trial. The Lancet. 2008. https://doi.org/10.1016/S0140-6736(08)60601-7.
Funding
Toomas Marandi has been supported by Estonian Research Council [PRG435].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None to declare.
Prior presentations
This work has not been formally presented.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Keskpaik, T., Talving, P., Kirsimägi, Ü. et al. Associations between elevated high-sensitive cardiac troponin t and outcomes in patients with acute abdominal pain. Eur J Trauma Emerg Surg 49, 281–288 (2023). https://doi.org/10.1007/s00068-022-02057-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-022-02057-z