Abstract
Purpose
Acute elbow dislocations are complex injuries that predispose to chronic instability and pain. The ideal treatment strategy is part of controversial discussion and evidence-based recommendations for the treatment could not be concluded from the literature. The purpose of the present study was to assess current epidemiological data, injury pattern, and the changing trend for treatment.
Methods
This study presents a retrospective review of 72 patients ≥ 18 years of age who were treated in our level I trauma centre with acute elbow dislocations from 2014 to 2018. The data were acquired by analysis of the institution’s database, and radiological examinations.
Results
The average age of the patients was 48.5 years (range 18–86). The ratio of male to female patients was 1.9:1. A fall onto the outstretched arm (42%) was the most common injury mechanism. By classification, 42% of the elbow dislocations were simple, and 58% complex. A total of 85% of patients underwent surgery including 73% of the simple elbow dislocations due to remaining instability or non-congruency of the reduced elbow. The indication for surgical treatment correlated merely with the grade of instability and displacement, but not with age.
Conclusion
Acute elbow dislocations need identification of the precise injury pattern and instability after reduction of the elbow joint. To achieve a congruent and stable joint, we recommend primary surgical repair as first-line treatment for patients with unstable simple and complex elbow dislocation independent of age.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The treatment of acute elbow dislocations is a challenge due the complex interaction between the bony articulations of the elbow joint, the capsuloligamentous structures, and dynamic muscle restraints [1]. Comprehension of the elbow anatomy and the relative contribution of the various elements to elbow stability is important in developing an algorithm for diagnosis and treatment [1]. Additionally, early recognition of the precise injury pattern is critical in restoring elbow function and preventing chronic instability and pain [2]. Despite improvement in understanding of these lesions and a recent increasing trend for early surgical ligament repair, evidence-based recommendations for the treatment could not be concluded from literature [3]. This study was performed to better characterise the current epidemiology, injury pattern, and the trend for surgical treatment of these injuries as important step towards definition of a robust treatment algorithm.
Patients and methods
Approval from the institutional review board of the medical faculty (GN19-390) was obtained prior to performing this retrospective study. The study included all patients ≥ 18 years of age with acute elbow dislocations who were treated in our level I trauma centre according our treatment algorithm between 2014 and 2018 (Fig. 1).
The data were collected by analysis of the institution’s database, and radiological examinations. Information obtained included age, gender, injury mechanism, injury pattern, and mode of treatment. Concerning the injury mechanism, low-energy trauma (i.e., fall from standing or seating height), and high-energy trauma (i.e., fall from height greater than standing, motor vehicle accident, sport accident, bicycle accident) were distinguished.
Elbow dislocations were classified into simple and complex. Simple elbow dislocation occurred without significant associated fractures, while complex elbow dislocations were combined with concomitant periarticular fracture(s) [3,4,5,6,7].
Elbows were usually reduced in the emergency department under analgesia and conscious sedation. After reduction, a comprehensive examination of the joint stability was performed under anaesthesia. Radiographs were performed after reduction in all cases. Stable and reducible injuries were treated conservatively. The indication for surgical treatment included: (1) radiological subluxated or non-congruent joint after reduction, (2) elbows that required an extension limitation over 30° to 45° to maintain reduction, (3) detected instability under anaesthesia, and (4) displaced complex elbow dislocations. All operative patients were treated by surgeons specialised in orthopaedic trauma care.
In non-operative patients, early mobilisation occurred using a hinged orthosis within 2 weeks after trauma. After operative treatment, a long arm cast was applied for 2 weeks. Afterwards, a hinged orthosis was recommended for 4 weeks. Extension was limited for 3 weeks and gradually increased. Forced supination and pronation were restricted for 6 weeks. Full weight-bearing was allowed after a total period of 12 weeks.
Statistical evaluation was performed using chi-square test and Fisher’s exact test. Values of p < 0.05 were considered statistically significant.
Results
Age and gender
The average age was 48.5 years (range 18–86) containing 79% (57/72) adult patients (< 65 years), and 21% (15/72) elderly patients (≥ 65 years). The ratio of male to female patients was 1.9:1. The average age of males was 42.6 years (range 20–81), and 59.5 years (range 18–86) for females (Table 1).
Diagnostic procedures
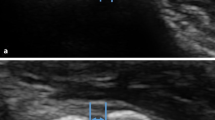
All patients underwent standard of care imaging that included radiographs in 100% (72/72). Computed tomography (CT) was used in 81% (58/72) for the assessment of complex elbow dislocations to delineate fracture type and assist surgical planning as well as on suspicion of a fracture. Magnetic resonance imaging (MRI) was performed in 21% (15/72) providing further information regarding ligament injury. Of these, 20% (3/15) were simple elbow dislocations, 40% (6/15) unstable simple elbow dislocations, and 40% (6/15) complex elbow dislocations.
Injury mechanism
The injury was caused by low-energy trauma in 42% (30/72), and by high-energy trauma in 58% (42/72). The most typical injury mechanism was fall (42%, 30/72) followed by bicycle accident, and fall from height each accounting for 15% (11/72) (Table 1).
Distribution of age versus injury mechanism
Reviewing the relationship between age and injury mechanism, 67% (38/57) of adult patients suffered from high-energy trauma, and 33% (19/57) from low-energy trauma, respectively, 27% (4/15), and 73% (11/15) of elderly patients. The differences were statistically significant (p = 0.008). Hence, elderly patients sustained predominantly low-energy trauma, while high-energy trauma occurred primarily in adult patients.
Injury pattern
The most common direction of displacement was posterior (79%, 38/48), thereof posterolateral accounted for 71% (27/38) of the cases, and posteromedial for 29% (11/38). In 33% (24/72) of the cases, the direction could not be determined as reduction was performed prior to hospital admission (Table 1).
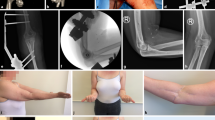
Simple elbow dislocations without significant associated fractures were seen in 42% (30/72), and complex elbow dislocations with relevant associated periarticular fracture(s) in 58% (42/72) (Figs. 2, 3).
Fractures of the radial head and ulnar coronoid process (33%, 14/42) were the most frequent fracture types, thereof 57% (8/14) “terrible triad” injuries with disruption of the medial collateral ligament, followed by fractures of the ulnar coronoid process (19%, 8/42), and fractures of the radial head (17%, 7/42) (Table 2).
Distribution of age versus injury pattern
Evaluating the distribution of age versus injury pattern, 42% (24/57) of adult patients sustained simple elbow dislocations, and 58% (33/57) complex elbow dislocation, versus 40% (6/15), and 60% (9/15) of the elderly patients. The differences were not statistically significant (p = 0.883). This indicates that adult and elderly patients were just as likely to sustain complex elbow dislocations.
Distribution of injury mechanism versus injury pattern
Analysing the distribution of injury mechanism versus injury pattern, 63% (19/30) of the patients with low-energy trauma sustained simple elbow dislocations, and 37% (11/30) complex elbow dislocations, respectively, 26% (11/42), and 74% (31/42) in cases of high-energy trauma. Thereby, the percentage of complex elbow dislocation increased significantly (p = 0.002) with the intensity of the injury mechanism, at the expense of simple elbow dislocations.
Distribution of age versus mode of treatment
A total of 85% (61/72) of patients underwent surgery. Evaluating the relationship between age and mode of treatment, 84% (48/57) of the adult patients were treated operatively versus 87% (13/15) of the elderly patients. The difference was not statistically different (p = 1.000). Therefore, in the present study population, elderly patients were not less likely to get surgical treatment as compared to adult patients.
Distribution of injury pattern versus mode of treatment
Reviewing the relationship between injury pattern and mode of treatment, simple elbow dislocations were treated conservatively in 27% (8/30) and with surgery in 73% (22/30) compared to 7% (3/42), and 93% (39/42) for complex elbow dislocations.
Mode of surgical treatment
For unstable simple elbow dislocations, ligament repair with suture anchor was performed in 45% (10/22) of both the medial and lateral collateral ligament, and isolated medial in 45% (10/22), and lateral in 9% (2/22). Protective fixation was used in 23% (5/22) with a DJD hinged external fixator in 60% (3/5), and a Kirschner wire in 40% (2/5) (Fig. 4, Table 3).
Concerning complex elbow dislocations, radial head fractures were treated surgically in 91% (29/32) of the cases, mainly with screws (41%, 12/29). Fractures of the ulnar coronoid process underwent surgery in 75% (21/28), primarily with transosseous suture (43%, 9/21). Olecranon fractures were managed operatively in 100% (10/10) with locking plates in 90% (9/10). Ligament repair with suture anchor occurred in 74% (29/39), while protective fixation was applied in 28% (11/39) (Fig. 5, Table 4).
Discussion
Age and gender are both important factors for defining risk for sustaining acute elbow dislocations [4, 5, 8]. Previous studies have indicated a male predominance in the occurrence of elbow dislocations and a significantly higher risk for this injury for adult patients [8, 9]. The results of the present study were congruent showing predominantly male patients and a similar age profile.
Most elbow dislocations are the result of falls onto the outstretched arm [3, 6, 8, 10]. Our data were similar in elderly patients with 73% of the elbow dislocations occurring as the result of a fall. However, in the adult population, high-energy trauma was the most common cause of injury (67%).
Posterior dislocations have proven to be the most common direction of displacement by far and can be further subdivided into posterolateral and posteromedial, of which posterolateral accounts for over 80% [3, 11]. The results of the present study were consistent with 79% posterior dislocations, thereof 71% posterolateral.
Concerning injury pattern, the literature indicates that simple elbow dislocations are the most common type of injury, and up to 20% of dislocations are associated with fractures [3, 12]. Our data were different with a higher rate (58%) of complex elbow dislocations. This could be due, in part, to our higher proportion of high-energy trauma in the adult population.
Simple elbow dislocations are mainly treated with conservative management in current literature [3, 7, 13,14,15]. Many authors have reported favorable results after conservative treatment for simple elbow dislocations [10, 13, 16, 17]. Additionally, some studies have reported more satisfactory results after conservative treatment compared to surgical management [11, 18]. However, indication for surgical repair is generally recommended in unstable elbow dislocations, in which primary ligament repair demonstrated satisfactory outcomes [11, 17, 19,20,21]. Therefore, it is standardly indicated to determine the treatment method of simple elbow dislocations according to the stability after reduction of the elbow joint [7, 17]. If the elbow is radiological subluxated or non-congruent after reduction, unstable under anaesthesia, or requires an extension limitation over 30–45° to maintain reduction, unstable simple elbow dislocation has to be diagnosed, recommending early ligament repair [7]. Our data were consistent, but the percentage of patients with unstable simple elbow dislocations was higher compared to current data. In our study cohort, surgery had to be performed in 73% of the simple elbow dislocations due to remaining instability or non-congruency of the reduced elbow. Congruently, disruption of both the medial and lateral collateral ligament was detected in 45% of the cases compared to isolated medial in 45%, and lateral in 9%.
The treatment principles of complex elbow dislocations are mainly reduction of the joint, stabilisation of associated fractures, and early motion [2, 4, 12]. Ligament repair and hinged external fixators are necessary in some cases to restore stability for early motion [11, 12, 22,23,24]. The results of the present study were similar. Screws (41%) predominated the surgical treatment of the radial head compared to transosseous suture (43%) for the ulnar coronoid process, and locking plate (90%) for the olecranon. Ligament repair with suture anchor occurred in most complex elbow dislocations (74%), while protective fixation was applied in 28%.
Age has been shown to be a major determinant of non-operative management [25]. Contrary, in the current study, elderly patients were just as likely to get surgical treatment as adult patients due to a variety of reasons. First, the high percentage of complex elbow dislocations (60%). Second, it was also due to a personal request of the elderly patients who are now more active than ever and often prefer surgical treatments that do not hamper their activities.
Some limitations must be considered for the present study. First, the study design was retrospective. Second, our data provided no information on outcomes. Even though this study contributes to currently available epidemiological data, the definite answer regarding appropriate algorithm for treating acute elbow dislocations requires prospective long-term outcome studies.
Conclusion
In conclusion, the treatment method of acute elbow dislocation has to be determined according precise injury pattern and instability after reduction of the elbow joint. To achieve a congruent and stable joint, we recommend primary surgical repair as first-line treatment for patients with unstable simple and complex elbow dislocation independent of age.
Code availability
Not applicable.
References
Ball CM, Galatz LM, Yamaguchi K. Elbow instability: treatment strategies and emerging concepts. Instr Course Lect. 2002;51:53–61.
Tarassoli P, McCann P, Amirfeyz R. Complex instability of the elbow. Injury. 2017;48:568–77. https://doi.org/10.1016/j.injury.2013.09.032.
Grazette AJ, Aquilina A. The assessment and management of simple elbow dislocations. Open Orthop J. 2017;11:1373–9. https://doi.org/10.2174/1874325001711011373.
DiPaola M, Geissler WB, Osterman AL. Complex elbow instability. Hand Clin. 2008;24:39–52. https://doi.org/10.1016/j.hcl.2007.11.010.
Boretto JG, Rodriguez Sammartino M, Gallucci G, et al. Comparative study of simple and complex open elbow dislocations. Clin Orthop Relat Res. 2014;472:2037–43. https://doi.org/10.1007/s11999-014-3491-3.
Morrey N. Acute and chronic instability of the elbow. J Am Acad Orthop Surg. 1996;4:117–28. https://doi.org/10.5435/00124635-199605000-00001.
Heo YM, Yi JW, Lee JB, et al. Unstable simple elbow dislocation treated with the repair of lateral collateral ligament complex. Clin Orthop Surg. 2015;7:241. https://doi.org/10.4055/cios.2015.7.2.241.
Layson J, Best BJ. Elbow Dislocation. In: StatPearls. Island: StatPearls Publishing Treasure Island (FL); 2019.
Stoneback JW, Owens BD, Sykes J, et al. Incidence of elbow dislocations in the United States population. J Bone Joint Surg Am. 2012;94:240–5. https://doi.org/10.2106/JBJS.J.01663.
Mehlhoff TL, Noble PC, Bennett JB, Tullos HS. Simple dislocation of the elbow in the adult. Results after closed treatment. J Bone Joint Surg Am. 1988;70:244–9.
Hobgood ER, Khan SO, Field LD. Acute dislocations of the adult elbow. Hand Clin. 2008;24:1–7. https://doi.org/10.1016/j.hcl.2007.11.012.
Hildebrand KA, Patterson SD, King GJW. Acute elbow dislocations: simple and complex. Orthop Clin North Am. 1999;30:63–79. https://doi.org/10.1016/S0030-5898(05)70061-4.
Chin TY, Chou H, Peh WCG. The acutely injured elbow. Radiol Clin North Am. 2019;57:911–30. https://doi.org/10.1016/j.rcl.2019.03.006.
Hackl M, Beyer F, Wegmann K, et al. The treatment of simple elbow dislocation in adults. Dtsch Arzteblatt Int. 2015;112:311–9. https://doi.org/10.3238/arztebl.2015.0311.
Taylor F, Sims M, Theis J-C, Herbison GP. Interventions for treating acute elbow dislocations in adults. Cochrane Database Syst Rev. 2012. https://doi.org/10.1002/14651858.CD007908.pub2.
Borris LC, Lassen MR, Christensen CS. Elbow dislocation in children and adults. A long-term follow-up of conservatively treated patients. Acta Orthop Scand. 1987;58:649–51. https://doi.org/10.3109/17453678709146506.
Sheps DM, Hildebrand KA, Boorman RS. Simple dislocations of the elbow: evaluation and treatment. Hand Clin. 2004;20:389–404. https://doi.org/10.1016/j.hcl.2004.07.002.
Josefsson PO, Gentz CF, Johnell O, Wendeberg B. Surgical versus non-surgical treatment of ligamentous injuries following dislocation of the elbow joint. A prospective randomized study. J Bone Joint Surg Am. 1987;69:605–8.
O’Driscoll SW, Jupiter JB, King GJ, et al. The unstable elbow. Instr Course Lect. 2001;50:89–102.
de Haan J, Schep N, Tuinebreijer W, den Hartog D. Complex and unstable simple elbow dislocations: a review and quantitative analysis of individual patient data. Open Orthop J. 2010;4:80–6. https://doi.org/10.2174/1874325001004020080.
Modi CS, Wasserstein D, Mayne IP, et al. The frequency and risk factors for subsequent surgery after a simple elbow dislocation. Injury. 2015;46:1156–60. https://doi.org/10.1016/j.injury.2015.02.009.
Zeiders GJ, Patel MK. Management of unstable elbows following complex fracture-dislocations–the “terrible triad” injury. J Bone Joint Surg Am. 2008;90(Suppl 4):75–84. https://doi.org/10.2106/JBJS.H.00893.
Tan V, Daluiski A, Capo J, Hotchkiss R. Hinged elbow external fixators: indications and uses. J Am Acad Orthop Surg. 2005;13:503–14. https://doi.org/10.5435/00124635-200512000-00003.
Ring D, Jupiter JB, Zilberfarb J. Posterior dislocation of the elbow with fractures of the radial head and coronoid. J Bone Joint Surg Am. 2002;84:547–51. https://doi.org/10.2106/00004623-200204000-00006.
Court-Brown CM, Aitken S, Hamilton TW, et al. Nonoperative fracture treatment in the modern era. J Trauma. 2010;69:699–707. https://doi.org/10.1097/TA.0b013e3181b57ace.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
N. Mühlenfeld, J. Frank, T. Lustenberger, I. Marzi, and A. L. Sander declare that they have no conflict of interest.
Availability of data and material
Not applicable.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mühlenfeld, N., Frank, J., Lustenberger, T. et al. Epidemiology and treatment of acute elbow dislocations: current concept based on primary surgical ligament repair of unstable simple elbow dislocations. Eur J Trauma Emerg Surg 48, 629–636 (2022). https://doi.org/10.1007/s00068-020-01512-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01512-z