Abstract
Purpose:
To compare stereotactic brachytherapy (SBT) with stereotactic radiosurgery (SRS) for treating singular cerebral metastases, regarding feasibility, complications, cerebral disease control, and survival.
Patients and Methods:
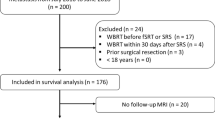
For this retrospective, single-center study, all patients treated for newly diagnosed, untreated singular cerebral metastasis with SBT using 125iodine seeds (cumulative tumor surface dose 50 Gy, applied for 42 days) were compared with patients receiving LINAC-based SRS for the same indication. Survival and actuarial local and distant disease control were evaluated using univariate Kaplan–Meier estimates and Cox regression. Results were compared using Student’s t test and the χ2 test.
Results:
A total of 142 patients treated with SRS were compared with 77 patients undergoing SBT. No significant differences were observed between epidemiological and disease-related features (p > 0.05), except a lower KPS (p < 0.007) and a larger tumor volume (p < 0.001) in the SBT group. Neither median survival (LINAC-SRS vs. SBT = 8.1 vs. 8.0 months, respectively) nor actuarial local/distant cerebral disease control after 12 months showed significant differences (93.6% vs. 96.7% / 42.4% vs. 46.4%). There was no treatment-related mortality and no permanent grade 3 or 4 CNS toxicity (RTOG/EORTC CNS toxicity criteria).
Conclusion:
For the treatment of singular cerebral metastasis, SBT represents a safe, minimally invasive, and effective local treatment option with results comparable to SRS regarding survival and cerebral disease control. Its advantage is that it allows histological (re-)evaluation and treatment within one stereotactic procedure and, compared to microneurosurgery, is almost unrestricted regarding tumor localization. Furthermore, larger metastases can be treated than with SRS. SBT, therefore, represents an alternative local treatment in selected cases.
Zusammenfassung
Ziel:
Vergleich der stereotaktischen Radiochirurgie (SRS) mit stereotaktisch geführter Jod-125-Seedimplantation zur Brachytherapie (SBT) zur Behandlung neu diagnostizierter, unbehandelter singulärer zerebraler Metastasen bezüglich Durchführbarkeit, Komplikationen, zerebraler Tumorkontrolle und Überleben.
Patienten und Methodik:
Für diese retrospektive Studie verglichen wir Behandlungsergebnisse von Patienten mit singulären zerebraler Metastasen, die mittels SBT (Jod-125-Seeds, kumulative Tumoroberflächendosis 50 Gy appliziert über 42 Tage) therapiert wurden, mit solchen, die LINAC-basierte SRS erhielten. Überleben, aktuarische lokale und distante Kontrolle der cerebralen Metastasen nach 12 Monaten wurden mittels Kaplan–Meier ermittelt und Ergebnisse mittels t-Test und Chi-Quadrat Test ausgewertet.
Ergebnisse:
142 SRS-behandelte Patienten wurden mit 77 SBT-therapierten verglichen. Bis auf schlechteren KPS (p < 0.007) und größeres Tumorvolumen (p < 0,001) in der SBT-Gruppe unterschieden sich epidemiologische und krankheitsspezifische Merkmale nicht signifikant (p > 0,05). Weder das mediane Überleben (SRS vs. SBT = 8,1 versus 8,0 Monate) noch die aktuarische lokale/ distante Tumorkontrolle (93,6% vs. 96,7%/42,4% vs. 46,4%) zeigten signifikante Unterschiede. Es gab keine behandlungsassoziierte Mortalität und keine permanenten Grad-3- und -4-Schädigungen (ZNS-Toxizitätskriterien der RTOG/EORTC).
Schlussfolgerung:
SBT stellt eine sichere, minimal-invasive und effektive Methode zur lokalen Behandlung singulärer zerebraler Metastasen dar. Vorteilhaft ist die Kombinationsmöglichkeit von histologischer Diagnostik und Behandlung innerhalb einer Operationssitzung. Die Ergebnisse sind bezüglich Überleben und zerebraler Tumorkontrolle mit denen nach SRS vergleichbar. Im Gegensatz zur Mikro-Neurochirurgie bestehen kaum Restriktionen bezüglich Tumorlokalisation. Im Vergleich zur SRS können auch größere Metastasen behandelt werden. Daher stellt SBT für ausgewählte Fälle eine alternative lokale Behandlungsmethode dar.
Similar content being viewed by others
References
Armstrong JG, Wronski M, Galicich J, et al. Postoperative radiation for lung cancer metastasic to the brain. J Clin Oncol 1994;12:2340–44.
Aoyama H, Shirato H, Tago M, et al. Stereotactic radiosurgery plus wholebrain radiation therapy vs. stereotactic radiosurgery alone for treatment of brain metastases: a randomized controlled trial. JAMA 2006;295:2483–91.
El Majdoub F, Brunn A, et al. Stereotactic interstitial radiosurgery for intracranial Rosai-Dorfman disease. A novel therapeutic approach. Strahlenther Onkol 2009;185:109–12.
Fokas E, Henzel M, Hamm K, et al. Radiotherapy for brain metastases from renal cell cancer: should whole-brain radiotherapy be added to stereotactic radiosurgery? Analysis of 88 patients. Strahlenther Onkol 2010; 186:210–7.
Gaspar L, Scott C, Rotman M, et al. Recursive partitioning analysis (RPA) of prognostic factors in three Radiation Therapy Oncology Group (RTOG) brain metastases trials. Int J Radiat Oncol Biol Phys 1997;37:745–51.
Hagen NA, Cirrincione C, Thaler HT, et al. The role of radiation therapy following resection of single brain metastases from melanoma. Neurology 1990;40:158–60.
Karnofsky DA, Burchenal JH. The clinical evaluation of chemotherapeutic agents in cancer. In: MacLeod CM (ed) Evaluation of chemotherapeutic agents. New York, Columbia University Press 1949;191–205.
Kaulich TW, Bamberg M. Radiation protection of persons living close to patients with radioactive implants. Strahlenther Onkol 2010; 186:107–12.
Kocher M, Maarouf M, Bendel M, et al. Linac radiosurgery versus whole brain radiotherapy for brain metastases. A survival comparison based on the RTOG recursive partitioning analysis. Strahlenther Onkol 2004;180:263–7.
Maarouf M, El Majdoub F, Bührle C, et al. Pineal parenchymal tumors: management with interstitial iodine-125 radiosurgery. Strahlenther Onkol 2010; 496–501.
Macdonald DR, Cascino TL, Schold SC Jr, et al. Response criteria for phase II studies of supratentorial malignant glioma. J Clin Oncol 1990;8:1277–80.
Maldaun MV, Aguiar PH, Lang F, et al. Radiosurgery in the treatment of brain metastases: critical review regarding complications. Neurosurg Rev 2008;3:1–8.
Meisner J, Meyer A, Polivka B, et al. Outcome of moderately dosed radiosurgery for limited brain metastases. Report of a single-center experience. Strahlenther Onkol 2010;186:76–81.
Muacevic A, Kreth FW, Horstmann GA, et al. Surgery and radiotherapy compared with gamma knife radiosurgery in the treatment of solitary cerebral metastases of small diameter. J Neurosurg 1999;91:35–43.
Muacevic A, Wowra B, Siefert A, et al. Microsurgery plus whole brain irradiation versus Gamma Knife surgery alone for treatment of single metastases to the brain: a randomized controlled multicentre phase III trial. J Neurooncol 2008;87:299–307.
Noel G, Medioni J, Valery CA, et al. Three irradiation treatment options including radiosurgery for brain metastases from primary lung cancer. Lung Cancer 2003;41:333–43.
Ostertag CB, Kreth FW. Interstitial iodine-125 radiosurgery for cerebral metastases. Br J Neurosurg 1995;9:593–603.
Patchell RA, Tibbs PA, Regine WF, et al. Postoperative radiotherapy in the treatment of single metastases to the brain: a randomized trial. JAMA 1998;280:1485–9.
Patchell RA, Tibbs PA, Walsh JW, et al. A randomized trial of surgery in the treatment of single metastases to the brain. N Engl J Med 1990;322: 494–500.
Pirzkall A, Debus J, Lohr F, et al. Radiosurgery alone or in combination with wholebrain radiotherapy for brain metastases. J Clin Oncol 1998;16:3563–9.
Prados M, Leibel S, Barnett CM, et al. Interstitial brachytherapy for metastatic brain tumors. Cancer 1989;63:657–60.
Rades D, Pluemer A, Veninga T, et al. Whole-brain radiotherapy versus stereotactic radiosurgery for patients in recursive partitioning analysis classes 1 and 2 with 1 to 3 brain metastases. Cancer 2007;110:2285–92.
Rades D, Pluemer A, Veninga T, et al. Comparison of different treatment approaches for one to two brain metastases in elderly patients. Strahlenther Onkol 2008;184:565–71.
Shaw E, Scott C, Souhami L, et al. Radiosurgery for the treatment of previously irradiated recurrent primary brain tumors and brain metastases: initial report of radiation therapy oncology group protocol (90–05). Int J Radiat Oncol Biol Phys 1996;34:647–54.
Shaw E, Scott C, Souhami L, et al. Single dose radiosurgical treatment of recurrent previously irradiated primary brain tumors and brain metastases: final report of RTOG protocol 90–05. Int J Radiat Oncol Biol Phys 2000;47:291–8.
Skibber JM, Soong SJ, Austin L, et al. Cranial irradiation after surgical excision of brain metastases in melanoma patients. Ann Surg Oncol 1996;3:118–23.
Sneed PK, Lamborn KR, Forstner JM, et al. Radiosurgery for brain metastases: is whole brain radiotherapy necessary? Int J Radiat Oncol Biol Phys 1999;43:549–58.
Sneed PK, Suh JH, Goetsch SJ, et al. A multi-institutional review of radiosurgery alone vs. radiosurgery with whole brain radiotherapy as the initial management of brain metastases. Int J Radiat Oncol Biol Phys 2002; 53:519–26.
Treuer H, Klein D, Maarouf M, et al. Accuracy and conformity of stereotactically guided interstitial brain tumor therapy using I-125 seeds. Radiother Oncol 2005;77:202–9.
Varlotto JM, Flickinger JC, Niranjan A, et al. The impact of whole-brain radiation therapy on the long-term control and morbidity of patients surviving more than one year after gamma knife radiosurgery for brain metastases. Int J Radiat Oncol Biol Phys 2005;62:1125–32.
Voges J, Treuer H, Sturm V, et al. Risk analysis of linear accelerator radiosurgery. Int J Radiat Oncol Biol Phys 1996;36:1055–63.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ruge, M.I., Kocher, M., Maarouf, M. et al. Comparison of Stereotactic Brachytherapy (125Iodine Seeds) with Stereotactic Radiosurgery (LINAC) for the Treatment of Singular Cerebral Metastases. Strahlenther Onkol 187, 7–14 (2011). https://doi.org/10.1007/s00066-010-2168-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-010-2168-4
Key Words
- Stereotaxy
- 125Iodine seeds
- Stereotactic brachytherapy (SBT)
- Singular brain metastases
- Stereotactic radiosurgery (SRS)