Abstract
The COVID-19 pandemic led to an enormous burden on healthcare systems worldwide. Causal therapy is still in its infancy. Contrary to initial views that the use of angiotensin-converting enzyme inhibitors (ACEi)/angiotensin II receptor blockers (ARBs) may increase the risk for a deleterious disease course, it has been shown that these agents may actually be beneficial for patients affected by COVID-19. In this article, we provide an overview of the three most commonly used classes of drugs in cardiovascular disease (ACEi/ARB, statins, beta-blockers) and their potential role in COVID-19 therapy. More results from randomized clinical trials are necessary to identify patients that can benefit most from the use of the respective drugs.
Zusammenfassung
Die COVID-19-Pandemie hat zu einer enormen Belastung der Gesundheitssysteme weltweit geführt. Die kausale Therapie steckt noch in den Kinderschuhen. Entgegen der Auffassung, dass der Einsatz von Angiotensin-Converting-Enzym(ACE)-Hemmern/Angiotensin-II-Rezeptor-Blockern (ARB) das Risiko für einen deletären Verlauf erhöhen könnte, hat sich gezeigt, dass diese Substanzen sogar einen Nutzen in der COVID-19-Therapie haben könnten. Im vorliegenden Artikel geben die Autoren einen Überblick über die 3 am häufigsten verwendeten Medikamentenklassen bei Herz-Kreislauf-Erkrankungen (ACE-Hemmer/ARB, Statine, Betablocker) und diskutieren ihren möglichen Beitrag zur COVID-19-Therapie. Es sind weitere Ergebnisse aus randomisierten klinischen Studien erforderlich, um die Patienten zu identifizieren, die am meisten vom Einsatz der jeweiligen Medikamente profitieren können.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Since the outbreak in 2019, the COVID-19 pandemic has led to more than 750 million infections and more than 6 million cumulative deaths as of 27 January 2023 [1]. Just like SARS-CoV‑1, SARS-CoV‑2 uses the membrane-bound angiotensin-converting enzyme (ACE) 2 as the entrance to cells during the infection process (Fig. 1; [2]). The organ primarily affected by the respiratory virus is the lung, especially alveolar cells type 2, which express ACE2 on their surface. The interaction takes place by binding of the viral spike protein, primed by the viral serine protease TMPRSS2, to the membrane-bound ACE2 [2, 3]. Besides the lung where ACE2 expression is considered rather low, ACE2 is expressed by other organs such as the heart [4], the intestine, or the kidneys [5], which may explain the potential to affect multiple organs and the systemic disease course following an infection. Angiotensin-converting enzyme 2 is part of the renin–angiotensin–aldosterone system (RAAS) and is important in vascular and cardiac physiology and homeostasis. The RAAS is the main contributing system for regulation of blood pressure in a distinct interplay between the kidneys and blood vessels.
The renin–angiotensin–aldosterone (RAAS) system in homeostasis and COVID-19. The protease renin (expressed by the juxtaglomerular cells in the kidneys) converts the preliminary molecule angiotensinogen into angiotensin I. This is cleaved by the angiotensin-converting enzyme (ACE)—mainly located on the endothelial cells of the lung but also in the heart [50]—to angiotensin II (Ang II). This effect can be blunted by ACE-inhibitors (ACEi). Ang II exerts its effects via binding to AT1-receptors and induces vasoconstriction. Ang II also leads to lysosomal internalization of ACE2, resulting in reduced expression. In homeostasis, RAAS is regulated by a feedback mechanism via Ang II inhibiting the expression of renin in the kidney. ACE2 cleaves Ang II into angiotensin 1–7 and Ang I into angiotensin 1–9 thereby having anti-hypertensive action. Angiotensin 1–7 exerts anti-inflammatory and anti-fibrotic actions binding to the Mas receptor, expressed by various cell types. Binding of SARS-CoV‑2 to ACE2 leads to internalization of this complex into the cell and further downregulation of ACE2 on the cell surface. Treatment with ACEi or AT1-receptor blockers (ARBs) increases ACE2 expression on the cell surface by prevention of internalization. (Figure contains modified image material available at Servier Medical Art by Servier licensed under a Creative Commons Attribution 3.0 Unported License; https://smart.servier.com)
The protease renin converts the preliminary molecule angiotensinogen into angiotensin I, which is then cleaved by the ACE—mainly located on the endothelial cells of the lung—to angiotensin II (Ang II, Fig. 1). Ang II exerts its effects via binding to AT1-receptors and induces vasoconstriction. Ang II also induces aldosterone secretion with subsequent sodium and water retention, which additionally impacts blood pressure regulation. In homeostasis, the RAAS is then regulated by a feedback mechanism with Ang II inhibiting the expression of renin in the kidney [6].
Angiotensin-converting enzyme 2 counteracts Ang II by cleavage into angiotensin 1–7, which may have anti-inflammatory and anti-fibrotic action via binding to the Mas receptor (Fig. 1), expressed by various cell types [7]. Additionally, it cleaves Ang I to angiotensin 1–9. Conversely, Ang II leads to lysosomal internalization of ACE2, resulting in reduced surface expression. Binding of SARS-CoV‑2 to ACE2 in the lung—analogous to SARS-CoV-1—also leads to internalization of this complex into the cell and further downregulation of ACE2 on the cell surface [3].
Treatment with ACE inhibitors (ACEi) or angiotensin receptor blockers (ARBs; e.g., for hypertension or heart failure) was shown to increase ACE2 expression in various tissues (Fig. 1, including the heart [8], lung [9], and kidneys [10]) in the majority of animal studies.
Given the crucial role of ACE2 in the pathophysiology of SARS-CoV‑2 infection and its alteration in expression following ACEi/ARB treatment, it was speculated during the beginning of the pandemic that treatment with ACEi or ARB could be harmful due to increased accessibility of the virus to its host cells [11]. The need for clinical studies and clarification of this issue was broadly discussed throughout the public media and the scientific community [12]. The initial hypothesis that ACEi/ARB treatment could be harmful was supported by small observational studies and the fact that patients with comorbidities (e.g., hypertension) treated with ACEi/ARB were particularly at risk for a severe course of the disease [13]. Especially patients with diabetes and vascular diseases on ACEi/ARB treatment were thought to be at higher risk due to increased circulating serum ACE2 activity [14]. However, as no solid evidence could be derived from these observations, several professional societies published recommendations early on not to discontinue ACEi/ARB treatment, as it was unclear whether discontinuation may possibly cause even greater harm [12, 15].
Observations on COVID-19 and RAAS inhibition
The most commonly prescribed drugs worldwide are ACEi and ARB. The range of applications is quite broad (e.g., hypertension, heart failure; [12]). Several observational studies have been published, investigating whether the treatment with ACEi/ARB has an effect on the mortality or disease severity following COVID-19 [16]. An Italian population-based case-control study comprising 6272 case patients and 30,759 control patients showed no association between the use of ACEi or ARB and COVID-19 disease severity [17]. In a retrospective analysis from Denmark in which 4480 COVID-19 patients were included, no association of patients who were on ACEi/ARB prior to the diagnosis (n = 895) with mortality or disease severity was found. In the same study, a nested case-control analysis of COVID-19 susceptibility showed no association of ACEi/ARB treatment and the incidence of COVID-19 when comparing 571 COVID-19 patients with 5710 age- and sex-matched controls [18]. This was confirmed in a study from Cleveland. Here, out of 18,472 patients, 12.5% were on ACEi/ARB treatment and 9.4% had tested positive for COVID-19. Among those who tested positive for COVID-19, only 214 patients were either on ACEi or ARBs, but there was no association between ACEi/ARB treatment and a positive SARS-CoV‑2 test result [19]. In line with this, a study from New York also found no association between the use of ACEi or ARBs and the risk for a positive COVID-19 test result. In addition, in the same study, no association was found between the use of ACEi/ARBs and the likelihood of a severe disease course, defined as intensive care treatment, mechanical ventilation, or death. Interestingly, other drugs, such as calcium-channel blockers or thiazide diuretics, also showed no association with the aforementioned outcomes [20]. Furthermore, in a meta-analysis of 16 studies comprising 24,676 COVID-19 patients, no association between the use of ACEi/ARBs and death or disease severity was found. On the contrary, an effect estimate even showed a protective effect using ACEi or ARB with a 23% reduced risk of death or critical disease course [21]. Another meta-analysis showed that among patients with hypertension, the use of ACEi/ARB was even associated with a lower disease severity and lower mortality [22].
Discontinuation of RAAS inhibition
Due to the initial concern that the continuation of ACEi/ARBs could worsen the course of COVID-19, several studies were initiated to investigate the effect of discontinuation of ACEi/ARBs in COVID-19. None of the trials (BRACE CORONA trial, REPLACE COVID, ACEI-COVID) showed an effect on disease severity, suggesting the decision to continue or discontinue should be made on an individual basis [23,24,25]. A recently published analysis even suggests that variables affecting mortality are age and comorbidities and not the use of ACEi/ARBs [26]. In summary, the concerns about the increased risk for deleterious consequences using ACEi/ARBs were not confirmed by several studies and different cohorts of patients.
RAAS inhibition as treatment for COVID-19
Insights from observational studies and meta-analyses on a potential beneficial effect of ACEi/ARB therapy in COVID-19 patients led to the initiation of studies to investigate the effect of ACEi/ARB therapy for COVID-19. Support for this hypothesis was gathered by animal studies showing that SARS-CoV-induced lung failure could be rescued by AT1 inhibition using losartan, which increases ACE2 expression [3]. A shift toward increased levels of angiotensin 1–7 would thus, due to its anti-inflammatory actions, be in favor (Fig. 2).
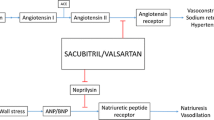
Potential therapeutic implications for cardiovascular drugs in COVID-19. Given the pleiotropic effects of lipid-lowering agents, they may exert anti-inflammatory and immunomodulatory effects. They could also reduce vascular inflammation and thus diminish thrombotic complications. Statins were shown to inhibit factors that are important for viral entry into cells and immune signaling, and have antioxidant effects. Omega‑3 polyunsaturated fatty acids may also have anti-inflammatory action, and fibrates were shown to inhibit the receptor-binding domain of SARS-CoV‑2 that is necessary to bind to ACE2. Beta-blockers may decrease the inflammatory response by direct action on contributing cells (e.g., macrophages). This can potentially ameliorate respiratory function in critically ill patients (e.g., increased PaO2/FiO2 ratio). ARBs act through inhibition of AT1-receptors and thereby increase ACE2 expression, which cleaves Ang II to angiopoietin 1–7. Angiotensin 1–7 exerts anti-inflammatory effects via Mas-receptor activation. Data even indicate that ARBs (i.e., losartan) may affect viral replication of SARS-CoV‑2 in vitro. ACE angiotensin-converting enzyme, Ang II angiotensin II, ARB AT1-receptor blocker. (Figure contains modified image material available at Servier Medical Art by Servier licensed under a Creative Commons Attribution 3.0 Unported License; https://smart.servier.com)
Losartan
Losartan was even shown to prevent the internalization of ACE2 via its action on AT1-receptors (Fig. 1; [27]). Recently, data have been published indicating that losartan may affect viral replication of SARS-CoV‑2 in vitro [28]. Therefore, most published clinical trials were performed using losartan as a treatment for COVID-19. First, the small COVIDMED trial included patients in the early phase of the pandemic and comprised only 14 patients, hospitalized due to COVID-19. In this double-blinded, placebo-controlled trial, losartan, however, did not improve outcome but showed an adverse safety signal [29]. Losartan also did not reduce the risk of hospitalization for outpatients in a small randomized clinical trial (RCT) using 25 mg daily [30] nor did it change the clinical outcome of hospitalized patients with mild hypoxemia in another small RCT including 31 patients [31]. Evaluating the effect of using either losartan or amlodipine for hypertensive patients hospitalized due to COVID-19 showed no difference on 30-day mortality or length of stay in the ICU or hospital in general [32]. In a multicenter, blinded, and placebo-controlled RCT conducted in 13 hospitals in the United States, investigating the effect of 50 mg losartan twice daily for COVID-19 patients with respiratory failure, no improvement in the Horowitz index was observed after 7 days. It also did not improve any other secondary clinical outcome but led to fewer vasopressor-free days compared to placebo [33], which seems plausible given the effect of ARBs on blood pressure.
Telmisartan
Fewer trials are published to date for using telmisartan. In one RCT 80 mg telmisartan was administered twice a day to patients hospitalized for COVID-19. Telmisartan treatment reduced death by day 30 and the composite of ICU, mechanical ventilation, and death was also reduced by day 15 and 30. In addition to this, patients receiving telmisartan had lower C‑reactive protein (CRP) values on day 5 and 8. The authors speculate that an anti-inflammatory effect of telmisartan (e.g., via increased angiotensin 1–7 levels) led to the reduction in mortality and morbidity [34]. The CLARITY trial using 40 mg telmisartan, however, showed no benefit of ARB treatment for hospitalized COVID-19 patients and was stopped due to futility [35].
To overcome potential systemic adverse effects (e.g., hypotension) that may be associated with ARB treatment, novel therapeutic approaches are tested using inhaled forms of telmisartan. The formulation showed an inhibitory effect against replication of SARS-CoV‑2 in vitro and sufficient lung pharmacokinetics in different animal models [36], which seems promising for further application (Fig. 2).
Pleiotropic effects of cardiovascular medications in COVID-19
With respect to the exaggerated immune response and resultant cytokine storm in COVID-19 disease course, drugs that specifically have anti-inflammatory action are central in COVID-19 therapy and anchored in the current guideline-recommended therapies (e.g., cortisone, tocilizumab). Some cardiovascular drugs, including beta-blockers and lipid-lowering agents, were also tested in COVID-19 therapy for their potential pleiotropic effects. Specifically, lipid-lowering agents, such as statins, may exert anti-inflammatory and immunomodulatory effects (Fig. 2; [37]). Indeed, statins were shown to inhibit factors that are important for viral entry into cells [38] and immune signaling, and to have antioxidant effects. Omega‑3 polyunsaturated fatty acids may also have anti-inflammatory action, and fibrates were shown to inhibit the receptor-binding domain of SARS-CoV‑2 that is necessary to bind to ACE2 [39]. For an overview of ongoing RCTs, there reader is referred to the work of Talasaz et al. [40].
In the INSPIRATION‑S trial, 587 patients with COVID-19 admitted to the ICU were randomized to receive atorvastatin 20 mg once daily or placebo for 30 days. No difference was found for the composite endpoint of thrombosis (venous/arterial), need for extracorporeal membrane oxygenation, or all-cause mortality [41]. In a retrospective registry-based analysis, lower odds for in-hospital mortality and development of a severe disease course (defined as admission to the ICU, mechanical ventilation, in-hospital death, or discharge to hospice) were observed. However, a propensity match revealed that only those patients with preexisting cardiovascular comorbidities profit from additional statin therapy [42]. Evidence for a benefit of statin therapy is still lacking and more results from ongoing RCTs are needed to clarify, in particular, which patients might benefit most from statin therapy.
Beta-blockers and COVID-19
COVID-19 is characterized by an immunological dysregulation and overshoot of cytokine production, i.e., a cytokine storm (CS). Beneficial effects of beta-blockers on mortality in critically ill patients with acute respiratory distress syndrome (ARDS) or sepsis (also characterized by a disturbed immunoregulation) were shown before [43, 44]. Contributors to the CS and to the endothelial dysfunction following COVID-19 are leukocytes, especially macrophages and lymphocytes. These cells are known to express beta-adrenergic receptors and thus play a crucial role in therapeutic considerations, since activation of these receptors may increase the release of pro-inflammatory cytokines (e.g., TNF-alpha, IL‑1, IL‑6; [45]).
Neutrophils also contribute to the pathophysiology of ARDS and CS via release of inflammatory mediators and formation of neutrophil extracellular traps (NETs) that further aggravate the inflammatory release [46]. Very recently it was shown that the neutrophil inflammatory activity (including NET formation) was diminished in a lung injury mouse model using i.v. administration of metoprolol [47]. Indeed, in the MADRID COVID trial, i.v. administration of 15 mg metoprolol to 20 patients with COVID-19 and ARDS in need of mechanical ventilation led to a reduction in pulmonary inflammation (Fig. 2) and NET markers and to improved oxygenation 4 days after randomization [48]. In another RCT that additionally aimed to target the sequelae of endothelial dysfunction associated with COVID-19, a mix of nicorandil, L‑arginine folate, nebivolol, and atorvastatin was given to patients. However, the trial stayed neutral and showed no difference in hospitalized COVID-19 patients regarding time to recovery, need for mechanical ventilation, ICU admission, or all-cause mortality [49].
Conclusion
To date, the best available protection for COVID-19 is vaccination, since antiviral therapies still have limited efficacy. Initial considerations that cardiovascular medications (e.g., angiotensin-converting enzyme inhibitors [ACEi]/angiotensin II receptor blockers [ARBs]) may be harmful in the COVID-19 pandemic have not been confirmed to date. On the contrary, intensive research efforts have even found a potential protective effect of using ARBs to treat COVID-19. In addition, it appears that other drugs with primarily different therapeutic objectives (e.g., statins, beta-blockers) may have a small benefit in COVID-19 or other clinical indications (sepsis, acute respiratory distress syndrome) due to their pleiotropic effects. In the future, ongoing preclinical and clinical studies will certainly provide us with more certainty in this regard and, if necessary, enable us to expand our arsenal for the therapy of COVID-19.
References
WHO (2023) Coronavirus disease (COVID-19) pandemic dashboard. https://covid19.who.int/. Accessed: 27.01.2023
Hoffmann M, Kleine-Weber H, Schroeder S et al (2020) SARS-coV‑2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell 181:271–280.e8
Kuba K, Imai Y, Rao S et al (2005) A crucial role of angiotensin converting enzyme 2 (ACE2) in SARS coronavirus-induced lung injury. Nat Med 11:875–879
Chen L, Li X, Chen M et al (2020) The ACE2 expression in human heart indicates new potential mechanism of heart injury among patients infected with SARS-CoV‑2. Cardiovasc Res 116:1097–1100
Danilczyk U, Penninger JM (2006) Angiotensin-converting enzyme II in the heart and the kidney. Circ Res 98:463–471
Naftilan AJ, Oparil S (1978) Inhibition of renin release from rat kidney slices by the angiotensins. Am J Physiol 235:F62–68
South AM, Shaltout HA, Washburn LK et al (2019) Fetal programming and the angiotensin-(1–7) axis: a review of the experimental and clinical data. Clin Sci (Lond) 133:55–74
Ferrario CM, Strawn WB (2006) Role of the renin-angiotensin-aldosterone system and proinflammatory mediators in cardiovascular disease. Am J Cardiol 98:121–128
Han SX, He GM, Wang T et al (2010) Losartan attenuates chronic cigarette smoke exposure-induced pulmonary arterial hypertension in rats: possible involvement of angiotensin-converting enzyme‑2. Toxicol Appl Pharmacol 245:100–107
Hamming I, van Goor H, Turner AJ et al (2008) Differential regulation of renal angiotensin-converting enzyme (ACE) and ACE2 during ACE inhibition and dietary sodium restriction in healthy rats. Exp Physiol 93:631–638
Hanff TC, Harhay MO, Brown TS et al (2020) Is there an association between COVID-19 mortality and the renin-angiotensin system? A call for epidemiologic investigations. Clin Infect Dis 71:870–874
Kessler T, Schunkert H (2020) Inhibitors of the renin-angiotensin system and SARS-CoV‑2 infection. Herz 45:323–324
Zhou F, Yu T, Du R et al (2020) Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet 395:1054–1062
Soro-Paavonen A, Gordin D, Forsblom C et al (2012) Circulating ACE2 activity is increased in patients with type 1 diabetes and vascular complications. J Hypertens 30:375–383
ESC (2020) The European society for cardiology. ESC guidance for the diagnosis and management of CV disease during the COVID-19 pandemic. https://www.escardio.org/Education/COVID-19-and-Cardiology/ESC-COVID-19-Guidance. Accessed 10 June 2020
Pinto-Sietsma SJ, Flossdorf M, Buchholz VR et al (2020) Antihypertensive drugs in COVID-19 infection. Eur Heart J Cardiovasc Pharmacother 6(6):415–416
Mancia G, Rea F, Ludergnani M et al (2020) Renin-angiotensin-aldosterone system blockers and the risk of Covid-19. N Engl J Med 382:2431–2440
Fosbol EL, Butt JH, Ostergaard L et al (2020) Association of angiotensin-converting enzyme inhibitor or angiotensin receptor blocker use with COVID-19 diagnosis and mortality. JAMA 324:168–177
Mehta N, Kalra A, Nowacki AS et al (2020) Association of use of angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers with testing positive for coronavirus disease 2019 (COVID-19). JAMA Cardiol 5:1020–1026
Reynolds HR, Adhikari S, Pulgarin C et al (2020) Renin-angiotensin-aldosterone system inhibitors and risk of Covid-19. N Engl J Med 382:2441–2448
Pirola CJ, Sookoian S (2020) Estimation of renin-angiotensin-aldosterone-system (RAAS)-inhibitor effect on COVID-19 outcome: a meta-analysis. J Infect 81:276–281
Liu X, Long C, Xiong Q et al (2020) Association of angiotensin converting enzyme inhibitors and angiotensin II receptor blockers with risk of COVID-19, inflammation level, severity, and death in patients with COVID-19: A rapid systematic review and meta-analysis. Clin Cardiol. https://doi.org/10.1002/clc.23421
Lopes RD, Macedo AVS, de Barros E Silva PGM et al (2021) Effect of discontinuing vs continuing angiotensin-converting enzyme inhibitors and angiotensin II receptor blockers on days alive and out of the hospital in patients admitted with COVID-19: a randomized clinical trial. JAMA 325:254–264
Cohen JB, Hanff TC, William P et al (2021) Continuation versus discontinuation of renin-angiotensin system inhibitors in patients admitted to hospital with COVID-19: a prospective, randomised, open-label trial. Lancet Respir Med 9:275–284
Bauer A, Schreinlechner M, Sappler N et al (2021) Discontinuation versus continuation of renin-angiotensin-system inhibitors in COVID-19 (ACEI-COVID): a prospective, parallel group, randomised, controlled, open-label trial. Lancet Respir Med 9:863–872
Mazzoni T, Maraia Z, Ruggeri B et al (2022) Sartans and ACE inhibitors: mortality in patients hospitalized with COVID-19. Retrospective study in patients on long-term treatment who died in the Italian hospitals of area Vasta n.5-Marche region. J Clin Med 11(9):2580. https://doi.org/10.3390/jcm11092580
Deshotels MR, Xia H, Sriramula S et al (2014) Angiotensin II mediates angiotensin converting enzyme type 2 internalization and degradation through an angiotensin II type I receptor-dependent mechanism. Hypertension 64:1368–1375
Nejat R, Sadr AS, Freitas B et al (2021) Losartan inhibits SARS-CoV‑2 replication in vitro. J Pharm Pharm Sci 24:390–399
Freilich D, Victory J, Jenkins P et al (2022) COVIDMED—an early pandemic randomized clinical trial of losartan treatment for hospitalized COVID-19 patients. Contemp Clin Trials Commun 29:100968
Puskarich MA, Cummins NW, Ingraham NE et al (2021) A multi-center phase II randomized clinical trial of losartan on symptomatic outpatients with COVID-19. EClinicalMedicine 37:100957
Geriak M, Haddad F, Kullar R et al (2021) Randomized prospective open label study shows no impact on clinical outcome of adding losartan to hospitalized COVID-19 patients with mild hypoxemia. Infect Dis Ther 10:1323–1330
Nouri-Vaskeh M, Kalami N, Zand R et al (2021) Comparison of losartan and amlodipine effects on the outcomes of patient with COVID-19 and primary hypertension: a randomised clinical trial. Int J Clin Pract 75:e14124
Puskarich MA, Ingraham NE, Merck LH et al (2022) Efficacy of losartan in hospitalized patients with COVID-19-induced lung injury: a randomized clinical trial. JAMA Netw Open 5:e222735
Duarte M, Pelorosso F, Nicolosi LN et al (2021) Telmisartan for treatment of Covid-19 patients: an open multicenter randomized clinical trial. EClinicalMedicine 37:100962
Jardine MJ, Kotwal SS, Bassi A et al (2022) Angiotensin receptor blockers for the treatment of covid-19: pragmatic, adaptive, multicentre, phase 3, randomised controlled trial. BMJ 379:e72175
Chen D, Yun X, Lee D et al (2023) Telmisartan nanosuspension for inhaled therapy of COVID-19 lung disease and other respiratory infections. Mol Pharmaceutics 20:750–757
Oesterle A, Laufs U, Liao JK (2017) Pleiotropic effects of statins on the cardiovascular system. Circ Res 120:229–243
Mehrbod P, Omar AR, Hair-Bejo M et al (2014) Mechanisms of action and efficacy of statins against influenza. Biomed Res Int 2014:872370
Davies SP, Mycroft-West CJ, Pagani I et al (2021) The hyperlipidaemic drug fenofibrate significantly reduces infection by SARS-coV‑2 in cell culture models. Front Pharmacol 12:660490
Talasaz AH, Sadeghipour P, Aghakouchakzadeh M et al (2021) Investigating lipid-modulating agents for prevention or treatment of COVID-19: JACC state-of-the-art review. J Am Coll Cardiol 78:1635–1654
Investigators I‑S (2022) Atorvastatin versus placebo in patients with covid-19 in intensive care: randomized controlled trial. BMJ 376:e68407
Daniels LB, Ren J, Kumar K et al (2021) Relation of prior statin and anti-hypertensive use to severity of disease among patients hospitalized with COVID-19: findings from the American heart association’s COVID-19 cardiovascular disease registry. PLoS ONE 16:e254635
Noveanu M, Breidthardt T, Reichlin T et al (2010) Effect of oral beta-blocker on short and long-term mortality in patients with acute respiratory failure: results from the BASEL-II-ICU study. Crit Care 14:R198
Tan K, Harazim M, Tang B et al (2019) The association between premorbid beta blocker exposure and mortality in sepsis—a systematic review. Crit Care 23:298
Al-Kuraishy HM, Al-Gareeb AI, Mostafa-Hedeab G et al (2021) Effects of beta-blockers on the sympathetic and cytokines storms in Covid-19. Front Immunol 12:749291
Middleton EA, He XY, Denorme F et al (2020) Neutrophil extracellular traps contribute to immunothrombosis in COVID-19 acute respiratory distress syndrome. Blood 136:1169–1179
Clemente-Moragon A, Gomez M, Villena-Gutierrez R et al (2020) Metoprolol exerts a non-class effect against ischaemia-reperfusion injury by abrogating exacerbated inflammation. Eur Heart J 41:4425–4440
Clemente-Moragon A, Martinez-Milla J, Oliver E et al (2021) Metoprolol in critically ill patients with COVID-19. J Am Coll Cardiol 78:1001–1011
Matli K, Al Kotob A, Jamaleddine W et al (2022) Managing endothelial dysfunction in COVID-19 with statins, beta blockers, nicorandil, and oral supplements: a pilot, double-blind, placebo-controlled, randomized clinical trial. Clin Transl Sci 15:2323–2330
Schunkert H, Dzau VJ, Tang SS et al (1990) Increased rat cardiac angiotensin converting enzyme activity and mRNA expression in pressure overload left ventricular hypertrophy. Effects on coronary resistance, contractility, and relaxation. J Clin Invest 86:1913–1920
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A. Dutsch and H. Schunkert declare that they have no competing interests.
For this article no studies with human participants or animals were performed by any of the authors. All studies mentioned were in accordance with the ethical standards indicated in each case.
Rights and permissions
About this article
Cite this article
Dutsch, A., Schunkert, H. RAAS inhibition and beyond—cardiovascular medications in patients at risk of or affected by COVID-19. Herz 48, 206–211 (2023). https://doi.org/10.1007/s00059-023-05168-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-023-05168-4