Abstract
Background
Left atrial appendage (LAA) obliteration is a proven stroke-preventive measure for patients with nonvalvular atrial fibrillation (AF). However, the efficacy of LAA obliteration for patients with AF after bioprosthetic mitral valve replacement (MVR) remains unclear.
Aim
This study aimed to estimate the efficacy of LAA obliteration in preventing embolism and to investigate the predictors of thromboembolism after bioprosthetic MVR.
Methods
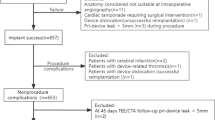
We retrospectively studied 173 AF subjects with bioprosthetic MVR; among them, 81 subjects underwent LAA obliteration using an endocardial running suture method. The main outcome measure was the occurrence of thrombosis events (TEs). The mean follow-up time was 40 ± 17 months.
Results
AF rhythm was observed in 136 patients postoperatively. The incidence rate of TEs was 13.97 % for postoperative AF subjects; a dilated left atrium (LA; > 49.5 mm) was identified as an independent risk factor of TEs (OR = 10.619, 95 % CI = 2.754–40.94, p = 0.001). For postoperative AF patients with or without LAA, the incidence rate of TEs was 15.8 % (9/57) and 12.7 % (10/79; p = 0.603), respectively. The incidence rate of TEs was 2.7 % (1/36) and 4.2 % (2/48) for the subgroup patients with a left atrial diameter of < 49.5 mm, and 38.1 % (8/21) and 25.8 % (8/31) for those with a left atrial diameter of > 49.5 mm (p = 0.346).
Conclusion
Surgical LAA obliteration in patients with valvular AF undergoing bioprosthetic MVR did not reduce TEs, even when the CHA2DS2-VASc score (a score for estimating the risk of stroke in AF) was ≥ 2 points.
Zusammenfassung
Hintergrund
Die Obliteration des linken Herzohrs („left atrial appendage“, LAA) ist nachgewiesenermaßen ein Verfahren zur Prävention des Schlaganfalls bei Patienten mit nichtvalvulärem Vorhofflimmern (VF). Die Wirksamkeit der LAA-Obliteration bei Patienten mit VF nach Mitralklappenersatz („mitral valve replacement“, MVR) mit einer Bioprothese bleibt jedoch unklar.
Ziel
Die vorliegende Studie zielt darauf ab, die Wirksamkeit der LAA-Obliteration bei der Verhütung von Embolien abzuschätzen und Prädiktoren der Thromboembolie nach bioprothetischem MVR zu untersuchen.
Methoden
Retrospektiv wurden 173 Patienten mit VF und bioprothetischem MVR untersucht, in 81 Fällen davon war eine LAA-Obliteration mit fortlaufender Endokardnaht erfolgt. Hauptendpunktparameter war das Auftreten thrombotischer Ereignisse (TE). Die Nachbeobachtungsdauer lag im Durchschnitt bei 40 ± 17 Monaten.
Ergebnisse
Postoperativ bestand bei 136 Patienten ein VF. Die TE-Inzidenzrate betrug 13,97 % bei den Teilnehmern mit postoperativem VF; ein dilatierter linken Vorhof (> 49,5 mm) wurde als unabhängiger Risikofaktor für TE ermittelt (Odds Ratio, OR: 10,619; 95 %-Konfidenzintervall: 2,754–40,94; p = 0,001). Für Patienten mit postoperativem VF mit bzw. ohne LAA lag die Inzidenzrate für TE bei 15,8 % (9/57) bzw. 12,7 % (10/79; p = 0,603), und bei 2,7 % (1/36) bzw. 4,2 % (2/48) für die Untergruppe mit einem linken Vorhof < 49,5 mm; dagegen bei 38,1 % (8/21) bzw. 25,8 % (8/31) für Patienten mit einem linken Vorhof > 49,5 mm (p = 0,346).
Schlussfolgerung
Durch eine chirurgische LAA-Obliteration bei Patienten mit valvulärem VF und bioprothetischem MVR wurden TE nicht vermindert, selbst wenn der CHA2DS2-VASc-Score (Score zur Abschätzung des Schlaganfallrisikos bei VF) bei ≥ 2 Punkten lag.




Similar content being viewed by others
References
Emmert MY, Puippe G, Baumuller S et al (2014) Safe, effective and durable epicardial left atrial appendage clip occlusion in patients with atrial fibrillation undergoing cardiac surgery: first long-term results from a prospective device trial. Eur J Cardiothorac Surg 45(1):126–131
Sick PB, Schuler G, Hauptmann KE et al (2007) Initial worldwide experience with the left atrial appendage system for stroke prevention in atrial fibrillation. J Am Coll Cardiol 49(13):1490–1495
Syed FF, Friedman PA (2014) Left atrial appendage closure for stroke prevention: emerging technologies. Card Electrophysiol Clin 6(1):141–160
Gonzalez-Lavin L, Tandon AP, Chi S et al (1984) The risk of thromboembolism and hemorrhage following mitral valve replacement. A comparative analysis between the porcine xenograft valve and Ionescu-Shiley bovine pericardial valve. J Thorac Cardiovasc Surg 87(3):340–351
Williams JB, Karp RB, Kirklin JW et al (1980) Considerations in selection and management of patients undergoing valve replacement with glutaraldehyde-fixed porcine bioprotheses. Ann Thorac Surg 30(3):247–258
Blackshear JL, Odell JA (1996) Appendage obliteration to reduce stroke in cardiac surgical patients with atrial fibrillation. Ann Thorac Surg 61:755–759
Garcia-Fernandez MA, Perez-David E, Quiles J et al (2003) Role of left atrial appendage obliteration in stroke reduction in patients with mitral valve prosthesis: a transesophageal echocardiographic study. J Am Coll Cardiol 42(7):1253–1258
January CT, Wann LS, Alpert JS et al (2014) 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol 21(64):e1–e76
Katz ES, Tsiamtsiouris T, Applebaum RM, Schwartzbard A, Tunick PA, Kronzon I (2000) Surgical left atrial appendage ligation is frequently incomplete: a transesophageal echocardiograhic study. J Am Coll Cardiol 36(2):468–471
Lynch M, Shanewise JS, Chang GL, Martin RP, Clements SD (1997) Recanalization of the left atrial appendage demonstrated by transesophageal echocardiography. Ann Thorac Surg 63(6):1774–1775
Almahameed ST, Khan M, Zuzek RW et al (2007) Left atrial appendage exclusion and the risk of thromboembolic events following mitral valve surgery. J Cardiovasc Electrophysiol 18(4):364–366
Mahajan R, Brooks AG, Sullivan T et al (2012) Importance of the underlying substrate in determining thrombus location in atrial fibrillation: implications for left atrial appendage closure. Heart 98(15):1120–1126
Habara S, Dote K, Kato M et al (2007) Prediction of left atrial appendage thrombi in non-valvular atrial fibrillation. Eur Heart J 28(18):2217–2222
Burstein B, Nattel S (2008) Atrial fibrosis: mechanisms and clinical relevance in atrial fibrillation. J Am Coll Cardiol 51(8):802–809
Viles-Gonzalez JF, Kar S, Douglas P et al (2012) The clinical impact of incomplete left atrial appendage closure with the Watchman Device in patients with atrial fibrillation: a PROTECT AF (Percutaneous Closure of the Left Atrial Appendage Versus Warfarin Therapy for Prevention of Stroke in Patients With Atrial Fibrillation) substudy. J Am Coll Cardiol 59(10):923–929
Goldberg YH (2008) Relationship between atrial fibrillation and left atrial size. J Am Coll Cardiol 51(7):776 (author reply 776–777)
Chinali M, de Simone G, Roman MJ et al (2005) Left atrial systolic force and cardiovascular outcome. The Strong Heart Study. Am J Hypertens 18(12 Pt 1):1570–1576 (discussion 1577)
Henry WL, Morganroth J, Pearlman AS et al (1976) Relation between echocardiographically determined left atrial size and atrial fibrillation. Circulation 53(2):273–279
Knackstedt C, Gramley F, Schimpf T et al (2008) Association of echocardiographic atrial size and atrial fibrosis in a sequential model of congestive heart failure and atrial fibrillation. Cardiovasc Pathol 17(5):318–324
Gage BF, Waterman AD, Shannon W, Boechler M, Rich MW, Radford MJ (2001) Validation of clinical classification schemes for predicting stroke: results from the National Registry of Atrial Fibrillation. JAMA 285(22):2864–2870
January CT, Wann LS, Alpert JS et al (2014) 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines and the Heart Rhythm Society. Circulation 130(23):2071–2104
Investigators TSPiAF (1992) Predictors of thromboembolism in atrial fibrillation: II. Echocardiographic features of patients at risk. The Stroke Prevention in Atrial Fibrillation Investigators. Ann Intern Med 116(1):6–12
Investigators TSPiAF (1992) Predictors of thromboembolism in atrial fibrillation: I. Clinical features of patients at risk. The Stroke Prevention in Atrial Fibrillation Investigators. Ann Intern Med 116(1):1–5
Whitlock RP, Sun JC, Fremes SE, Rubens FD, Teoh KH (2012) Antithrombotic and thrombolytic therapy for valvular disease: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 141(2 Suppl):e576S–e600S
Daccarett M, Badger TJ, Akoum N et al (2011) Association of left atrial fibrosis detected by delayed-enhancement magnetic resonance imaging and the risk of stroke in patients with atrial fibrillation. J Am Coll Cardiol 57(7):831–838
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
X-P. Min, T-Y. Zhu, J. Han, Y. Li, and X. Meng state that there are no conflicts of interest. All studies on humans described in the present manuscript were carried out with the approval of the responsible ethics committee and in accordance with national law and the Helsinki Declaration of 1975 (in its current, revised form). Informed consent was obtained from all patients included in studies.
Rights and permissions
About this article
Cite this article
Min, X., Zhu, T., Han, J. et al. Left atrial appendage obliteration in atrial fibrillation patients undergoing bioprosthetic mitral valve replacement. Herz 41, 87–94 (2016). https://doi.org/10.1007/s00059-015-4350-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-015-4350-z
Keywords
- Left atrial appendage
- Left atrial dimension
- Thrombosis events
- Atrial fibrillation
- Bioprosthetic mitral valve replacement